Quick Summary: Yes, it is possible to get pregnant from precum, though the risk is lower than from ejaculate. Research shows that some healthy males have motile sperm in their pre-ejaculate fluid, with studies finding varying results, and the withdrawal method has been reported to have failure rates around 22% in typical use annually. Using reliable contraception is essential for pregnancy prevention.
The question “can you get pregnant from precum?” ranks among the most searched reproductive health topics. It’s a legitimate concern that deserves a straightforward, science-based answer.
Here’s the reality: pregnancy from precum is absolutely possible. While the likelihood differs from full ejaculation, the risk is real enough that withdrawal shouldn’t be considered reliable birth control.
Understanding how precum works, what it contains, and why it poses pregnancy risks helps make informed decisions about contraception and sexual health.
What Is Precum?
Precum, medically known as pre-ejaculate or pre-ejaculatory fluid, is a clear, viscous liquid released from the penis during sexual arousal—well before ejaculation occurs.
This fluid originates primarily from the Cowper’s glands (bulbourethral glands) and the Littre glands. These small structures produce and release precum to serve several physiological functions.
The primary purposes of pre-ejaculate include:
- Neutralizing acidity in the urethra from residual urine
- Creating a more favorable pH environment for sperm survival
- Providing lubrication for intercourse
- Preparing the urethral passage for ejaculation
Most people produce between a few drops to about 5 milliliters of precum. The amount varies significantly between individuals, and some may not notice any at all.
The release of precum is involuntary—there’s no conscious control over when or how much gets produced. This matters tremendously when considering withdrawal as a contraceptive strategy.
Does Precum Contain Sperm?
This is where the science gets interesting. The fluid produced by Cowper’s glands doesn’t naturally contain sperm—that’s not its biological function.
But here’s the catch.
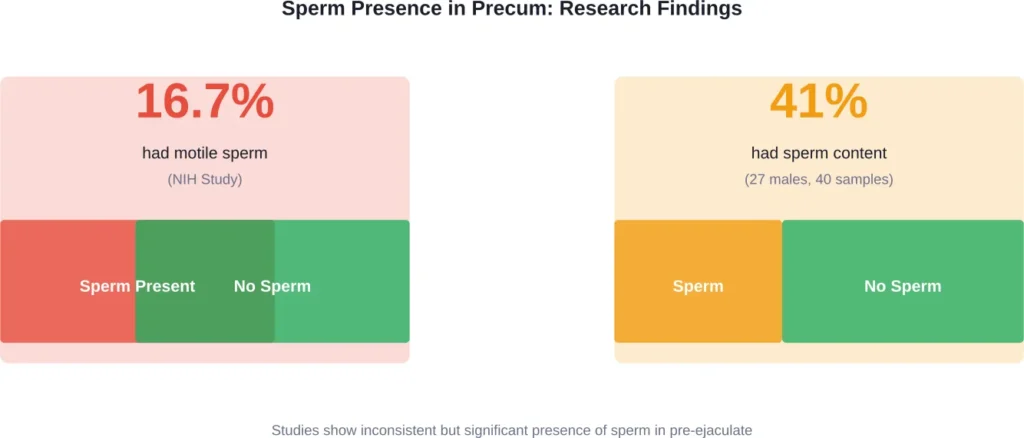
Research shows that some healthy males have motile sperm in their pre-ejaculate fluid, with studies finding varying results. Research has found varying prevalence of sperm in pre-ejaculate samples across different studies.
How does sperm end up in precum if it doesn’t originate there?
The most accepted explanation involves residual sperm. After ejaculation, live sperm can remain in the urethra. When precum passes through the same channel during subsequent arousal, it can pick up these leftover sperm cells and transport them out of the penis.
This means that precum from a sexual encounter following a recent ejaculation carries higher pregnancy risk than precum when no previous ejaculation occurred.
Some research suggests urination between ejaculations might flush out residual sperm, potentially reducing this risk. However, no definitive studies confirm this protective effect reliably enough to count on it.
Can You Actually Get Pregnant From Precum?
Yes. If sperm is present in precum, and that precum enters the vagina, pregnancy can occur.
The chances depend on several factors:
Timing in the Menstrual Cycle
Pregnancy risk peaks during the fertile window—roughly five days before ovulation through the day of ovulation itself. According to the American College of Obstetricians and Gynecologists, sperm can survive inside a woman’s body for about three days, sometimes up to five days.
An egg survives approximately 24 hours after ovulation. This creates a critical window where even small amounts of sperm from precum could potentially result in conception.
Outside this fertile window, pregnancy risk drops significantly but doesn’t disappear entirely. Ovulation timing varies between cycles, making it difficult to pinpoint safe periods with certainty.
Sperm Concentration
Medical research indicates that motile sperm concentrations greater than 1 million per milliliter are usually absent or inconsistently present in pre-ejaculate. When sperm is present, it’s typically in lower concentrations than ejaculate.
Lower concentration means lower probability—but not zero probability. It only takes one sperm cell to fertilize an egg.
Previous Ejaculation
As mentioned earlier, precum released after a recent ejaculation carries higher risk due to residual sperm in the urethra. This matters for couples having multiple sexual encounters in succession.
Understanding the Withdrawal Method
The withdrawal method (also called pulling out or coitus interruptus) involves removing the penis from the vagina before ejaculation occurs. Some couples rely on this as their primary contraceptive method.
The appeal is obvious: it’s free, requires no devices, has no hormonal side effects, and is always available. But effectiveness tells a different story.
Withdrawal Method Failure Rates
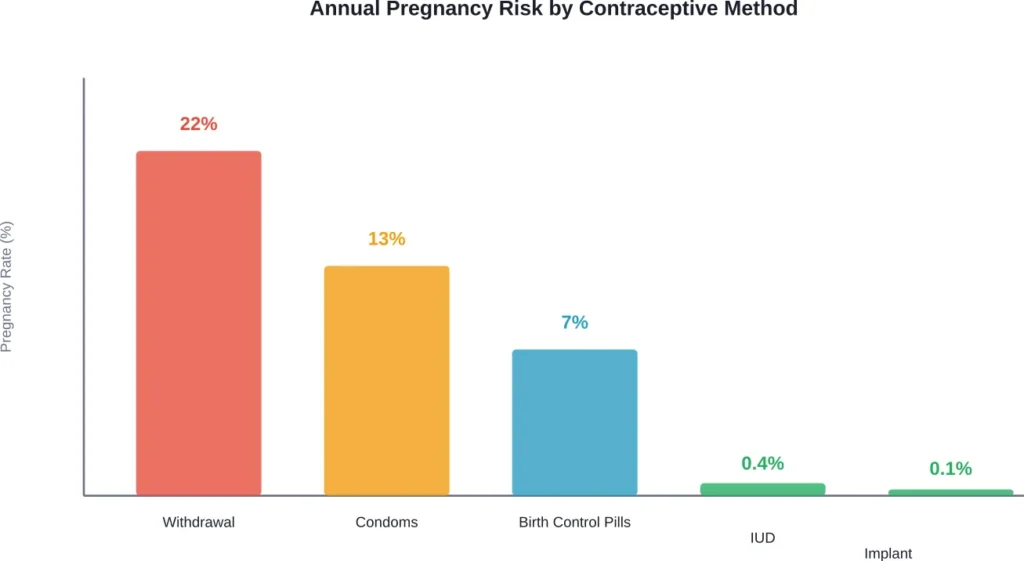
With typical use, the withdrawal method has been reported to have failure rates around 22% in typical use annually. That’s more than one in five—a significant failure rate compared to other contraceptive methods.
With perfect use consistently maintained, failure rates are reported to be lower. This is comparable to condoms when used correctly, but achieving perfect use consistently is challenging.
Why does withdrawal fail so often?
- Precum released before withdrawal contains sperm in some cases
- Timing the withdrawal correctly requires significant control and awareness
- The moment before ejaculation can be difficult to predict accurately
- In the heat of the moment, pulling out may not happen as planned
- Even partial penetration during re-entry after withdrawal can introduce sperm
| Birth Control Method | Typical Use Failure Rate | Perfect Use Failure Rate |
|---|---|---|
| Withdrawal Method | 22% | 4% |
| Male Condoms | 13% | 2% |
| Birth Control Pills | 7% | 0.3% |
| IUD (hormonal) | 0.1-0.4% | 0.1-0.4% |
| Implant | 0.1% | 0.1% |
The CDC’s contraceptive guidance highlights that unintended pregnancy rates remain high in the United States, with a substantial proportion of all pregnancies being unintended. Reliance on less effective methods like withdrawal contributes to these statistics.
Real Pregnancy Risk: What the Numbers Tell Us
Combining the research on sperm in precum with withdrawal method failure rates paints a clear picture.
If roughly 16-41% of males have sperm in their precum at any given time, and the withdrawal method fails for 22% of couples annually even when accounting for other factors, the pregnancy risk from precum is substantial.
Consider this scenario: A couple uses withdrawal as their only contraception over one year. Even if the male partner has sperm in his precum only occasionally (not consistently), multiple exposures throughout the year create cumulative risk.
During the fertile window specifically, even minimal sperm exposure carries meaningful pregnancy potential. The WHO’s research on contraceptive discontinuation found that 85% of women who stopped using contraception became pregnant within the first year.
What If You’re Using Birth Control?
The pregnancy risk from precum drops dramatically when using effective contraception.
Birth Control Pills
When taken correctly and consistently, combination birth control pills are highly effective at preventing pregnancy—with failure rates around 0.3% with perfect use. The pill works by preventing ovulation, so even if sperm from precum or ejaculate enters the vagina, there’s no egg to fertilize.
The key phrase is “taken correctly and consistently.” Missing pills, taking them at irregular times, or interactions with certain medications can reduce effectiveness.
Condoms
Condoms provide a physical barrier that prevents sperm from entering the vagina at all. Used correctly, they’re about 98% effective, with typical use effectiveness around 87%.
Condoms also offer protection against sexually transmitted infections—something hormonal methods and withdrawal don’t address.
Long-Acting Reversible Contraception (LARC)
According to CDC data, IUDs have typical use failure rates of 0.1-0.4%, staying effective for 3-8 years depending on the device. Implants show even better numbers at 0.1% failure rate.
These methods don’t depend on daily action or in-the-moment decisions, which explains their superior real-world effectiveness.
What to Do If You’re Concerned About Pregnancy
Worried about potential pregnancy from precum exposure? Here’s what to know.
Emergency Contraception
Emergency contraception (EC) can prevent pregnancy after unprotected sex or contraceptive failure. Options include:
- Levonorgestrel pills (Plan B, generics): Most effective within 72 hours, but can work up to 120 hours after intercourse
- Ulipristal acetate (ella): Effective up to 120 hours after sex
- Copper IUD: Can be inserted up to 5 days after unprotected sex and is the most effective emergency contraception option
Emergency contraception is more effective the sooner it’s taken after intercourse.
Pregnancy Testing
Home pregnancy tests detect the hormone hCG (human chorionic gonadotropin) in urine. Most tests become accurate around the time of the missed period—roughly two weeks after ovulation.
Testing too early can produce false negatives. For the most reliable results, wait until at least the first day of the expected period, or ideally a week after.
If the test is negative but the period doesn’t arrive, test again a few days later.
Choosing Effective Contraception
Understanding precum pregnancy risk highlights why effective contraception matters.
The CDC’s Selected Practice Recommendations for Contraceptive Use emphasizes that persons should seek advice from health care providers when considering family planning options. Multiple criteria exist for assessing pregnancy risk with high accuracy.
When selecting contraception, consider:
- Effectiveness rates (both perfect use and typical use)
- Ease of use and whether it requires daily action
- Side effects and health considerations
- STI protection needs
- Cost and accessibility
- Reversibility if planning future pregnancy
- Personal preferences and lifestyle factors
Many sexually active individuals express anxiety about precum pregnancy risk, especially among younger people or those new to sexual activity. This anxiety often stems from relying on withdrawal or having gaps in contraceptive use.
The WHO found that two-thirds of sexually active women who wished to delay or limit childbearing stopped using contraception due to fears of side effects, health concerns, or underestimating conception likelihood. Many of these concerns could be addressed through effective family planning counseling.
Beyond Pregnancy: STI Considerations
While this article focuses on pregnancy risk, it’s important to note that precum can also transmit sexually transmitted infections.
Infections like HIV, gonorrhea, chlamydia, and others can be present in pre-ejaculate fluid. The withdrawal method offers zero protection against STIs.
Barrier methods like condoms remain the only contraceptive approach that simultaneously addresses both pregnancy prevention and STI protection.
FAQs About Precum and Pregnancy
Yes, pregnancy is possible from precum even if ejaculation occurs outside the vagina. Research shows that some healthy males have motile sperm in their pre-ejaculate fluid, which is released before ejaculation and without conscious control.
Urination may theoretically flush residual sperm from the urethra, potentially reducing sperm content in subsequent precum. However, no conclusive research confirms this protective effect reliably enough to depend on it for contraception.
The withdrawal method has been reported to have failure rates around 22% in typical use annually—meaning roughly one in five couples relying on it will become pregnant annually. This is significantly less effective than condoms (13% typical use failure rate), birth control pills (7%), or IUDs (0.1-0.4%).
Yes, and the risk is highest during the fertile window surrounding ovulation. Sperm can survive in the female reproductive tract for 3-5 days, while an egg survives about 24 hours after ovulation. Even small amounts of sperm from precum can cause pregnancy during this time.
If you’re taking hormonal birth control correctly and consistently, the pregnancy risk from precum is extremely low. The pill prevents ovulation, so there’s no egg to fertilize. However, missed pills or medications that interfere with effectiveness can increase risk.
Home pregnancy tests are most accurate when taken around the time of the expected period—roughly two weeks after ovulation or potential conception. Testing earlier often produces false negatives because hCG levels aren’t yet high enough to detect.
Yes, precum typically contains lower concentrations of sperm than ejaculate (when sperm is present at all). This means lower probability of pregnancy, but not zero risk. Ejaculate contains millions of sperm specifically for reproduction, while precum may contain residual sperm picked up from the urethra.
The Bottom Line on Precum and Pregnancy
The science is clear: pregnancy from precum is medically possible and occurs more frequently than many realize.
Research shows that some healthy males have motile sperm in their pre-ejaculate fluid, with studies finding varying results. The withdrawal method, which many couples use to avoid this risk, has been reported to have failure rates around 22% in typical use annually.
These aren’t just statistics—they represent real pregnancies, often unintended, that could be prevented with more reliable contraception.
For anyone sexually active and not planning pregnancy, understanding these risks is essential. Effective contraception options exist that dramatically reduce pregnancy risk while accommodating different health needs, preferences, and lifestyles.
The CDC emphasizes seeking advice from health care providers when considering family planning options. Medical professionals can provide personalized guidance based on individual health factors, relationship circumstances, and reproductive goals.
Don’t rely on chance or incomplete information when it comes to reproductive health. Whether that means consistent condom use, hormonal contraception, long-acting reversible methods, or a combination approach with barrier methods for STI protection—effective options exist.
Take control of reproductive health with accurate information and appropriate contraception. Planning ahead promotes better outcomes and peace of mind.
