Quick Summary: True sugar allergies are extremely rare and not well-documented in medical literature. Most adverse reactions to sugar are actually intolerances, not allergies. Sugar intolerances occur when the body lacks specific enzymes to properly digest certain sugars, leading to digestive symptoms rather than immune responses.
The internet buzzes with claims about sugar allergies. People describe feeling awful after eating sweets and wonder if their body is mounting an allergic response.
But here’s what medical research actually shows: genuine sugar allergies are exceptionally rare. So rare, in fact, that scientists continue to question whether they truly exist as distinct allergic conditions.
That doesn’t mean sugar can’t cause problems. It absolutely can. The distinction matters, though, because the mechanisms, symptoms, and treatments differ dramatically between allergies and intolerances.
Let’s break down what science knows about adverse reactions to sugar, why most people experience intolerance rather than allergy, and what to do if sugar makes you feel terrible.
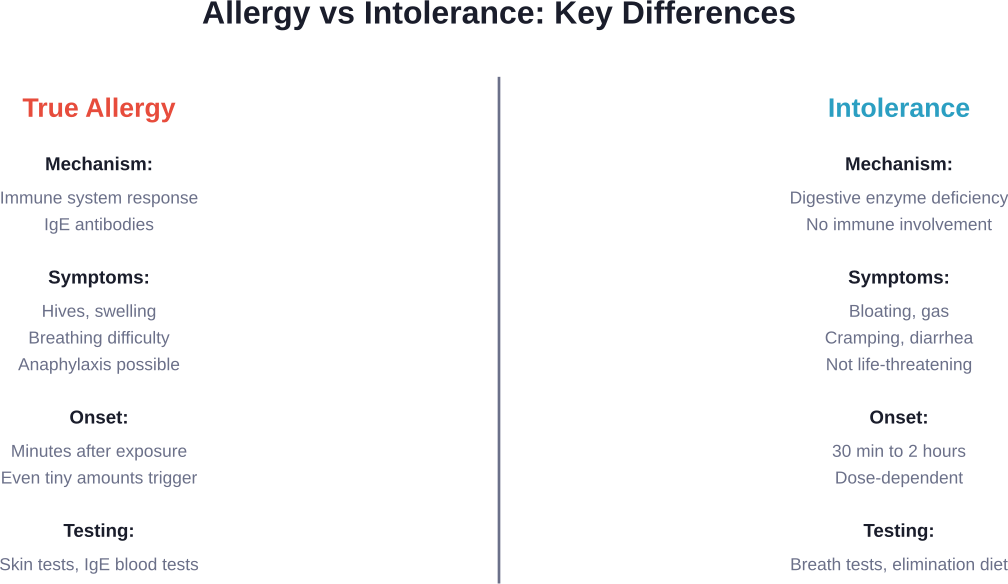
Understanding the Difference: Allergy vs. Intolerance
According to research published in Nutrients, food hypersensitivity encompasses both immune-mediated reactions (allergies) and non-immune-mediated reactions (intolerances). These create very different problems in the body.
Food allergies involve the immune system. When someone with a true food allergy eats the trigger food, their body produces IgE antibodies that recognize proteins as threats. This triggers the release of histamine and other chemicals, causing symptoms that range from mild hives to life-threatening anaphylaxis.
The most common food allergens include shellfish, peanuts, tree nuts, fish, cow’s milk, egg, wheat, sesame, and soy. Notice something? Sugar isn’t on that list.
Food intolerances work differently. They don’t involve the immune system at all. Instead, intolerances typically occur when the body lacks specific enzymes needed to properly digest certain foods or food components.
The NIH explains that adverse food reactions can manifest with various symptoms, from mild discomfort to severe reactions. But the mechanism matters enormously for diagnosis and treatment.
Why Sugar Allergies Are So Rare
True allergic reactions target proteins. The immune system creates antibodies against protein structures it perceives as dangerous.
Sugar molecules are carbohydrates, not proteins. They lack the complex protein structures that typically trigger IgE-mediated allergic responses.
That said, medical literature has documented extremely rare cases. A recent letter to the editor described fructose-induced anaphylaxis confirmed via double-blind placebo-controlled oral challenge, though no specific IgE could be detected. This represents an unconventional presentation that challenges current understanding of food allergies.
Alpha-gal syndrome provides another interesting exception. This condition involves IgE-mediated hypersensitivity to the glycan galactose-alpha-1,3-galactose (alpha-gal), not to a food protein. But this syndrome relates to mammalian meat consumption, not table sugar.
Types of Sugar and Related Intolerances
When people say “sugar,” they might mean different things. Several types of sugar exist, and intolerance to each creates distinct problems.
Sucrose Intolerance
Sucrose is common table sugar found in cane sugar, beets, maple syrup, fruits, legumes, and vegetables. The enzyme sucrase-isomaltase, located on small intestine cell surfaces, normally breaks down sucrose into glucose and fructose for absorption.
People with sucrose intolerance lack adequate sucrase-isomaltase. When sucrose reaches the gut undigested, bacteria ferment it, producing gas and drawing water into the intestines. This creates bloating, cramping, diarrhea, and discomfort.
Fructose Intolerance
Fructose appears naturally in fruits, fruit juices, some vegetables, and honey. Two distinct conditions involve fructose: hereditary fructose intolerance (a serious genetic disorder) and fructose malabsorption (a digestive issue).
According to Mayo Clinic, fructose malabsorption occurs when cells lining the small intestine can’t absorb fructose efficiently. The unabsorbed fructose moves to the colon, where bacteria ferment it, causing gas, bloating, and diarrhea.
Lactose Intolerance
Lactose is the sugar in milk and dairy products. Mayo Clinic notes that lactose intolerance occurs when the small intestine doesn’t produce enough lactase enzyme.
As research in the Journal of Food Allergy explains, undigested lactose moves through the gut, where bacterial fermentation releases hydrogen gas and draws liquid into the intestines. This produces the classic symptoms: bloating, cramping, gas, and loose stools.
Approximately 70% of the world’s population has some degree of lactose malabsorption, making this the most common sugar intolerance.

Recognizing Sugar Intolerance Symptoms
Sugar intolerance symptoms appear primarily in the digestive system. They typically start within 30 minutes to two hours after consuming the problematic sugar.
Common symptoms include:
- Bloating and abdominal distension
- Gas and flatulence
- Cramping or abdominal pain
- Diarrhea or loose stools
- Nausea
- Gurgling stomach sounds
These symptoms result from undigested sugar fermenting in the gut and drawing water into the intestines. The severity depends on the amount consumed and the degree of enzyme deficiency.
Some people report experiencing headaches, fatigue, or mood changes after sugar consumption. While these symptoms appear in community discussions online, they’re less consistently documented in medical literature as direct symptoms of sugar intolerance.
What True Allergic Reactions Look Like
If someone did have a genuine sugar allergy (remember, extremely rare), symptoms would look completely different.
According to Mayo Clinic, IgE-mediated food allergy symptoms can include:
- Hives, itching, or eczema
- Swelling of lips, face, tongue, throat, or other body parts
- Wheezing, nasal congestion, or trouble breathing
- Tingling in the mouth
- Dizziness, lightheadedness, or fainting
- Anaphylaxis in severe cases
An estimated 20% of acute urticarial cases are food allergy-related, according to research in Nutrients. Food allergy affects an estimated 8% of children under age 5 and up to 4% of adults.
Anaphylaxis is a life-threatening emergency requiring immediate epinephrine administration. Symptoms include severe difficulty breathing, rapid pulse, blood pressure drop, and loss of consciousness.
Is Sugar Intolerance the Same as Diabetes?
No. This confusion appears frequently, but the conditions are fundamentally different.
Diabetes is a metabolic disorder involving insulin production or function. Type 1 diabetes occurs when the pancreas produces little or no insulin. Type 2 diabetes develops when cells become resistant to insulin or the pancreas can’t produce enough.
Sugar intolerance involves digestive enzymes, not insulin or blood glucose regulation. Someone can have sugar intolerance without diabetes, diabetes without sugar intolerance, or both conditions simultaneously.
That said, people with diabetes must carefully manage sugar and carbohydrate intake to control blood glucose levels. But this represents disease management, not intolerance.
Getting Tested for Sugar Problems
If sugar consistently causes problems, proper testing can identify the specific issue.
Testing for Intolerances
Lactose intolerance testing typically involves a hydrogen breath test. After consuming lactose, breath samples measure hydrogen levels. Elevated hydrogen indicates bacterial fermentation of undigested lactose in the colon.
Fructose malabsorption uses a similar hydrogen breath test protocol with fructose instead of lactose.
Sucrose intolerance diagnosis may involve genetic testing for sucrase-isomaltase deficiency, breath testing, or intestinal biopsy to measure enzyme activity.
Elimination diets also help identify problematic sugars. Removing suspected triggers for several weeks, then systematically reintroducing them, can reveal which specific sugars cause symptoms.
Testing for Allergies
According to Mayo Clinic, food allergy testing includes several approaches:
- Detailed medical history and symptom tracking
- Skin prick tests exposing small amounts of suspected allergens
- Blood tests measuring IgE antibodies to specific foods
- Oral food challenges under medical supervision
- Elimination diets followed by supervised reintroduction
For suspected sugar allergy specifically, allergists would likely perform oral challenges and blood tests, though established protocols remain limited given the rarity of true sugar allergies.
Managing Sugar Intolerance
Treatment for sugar intolerance centers on dietary management rather than medication.
Avoidance Strategies
The most effective approach is avoiding or limiting the problematic sugar. This sounds simple but requires careful attention to food labels and ingredients.
For sucrose intolerance, limit or avoid:
- Table sugar and cane sugar
- Brown sugar and powdered sugar
- Maple syrup and molasses
- Many processed foods with added sugars
- Fruits high in sucrose
- Some vegetables like sweet potatoes and beets
For fructose intolerance, Mayo Clinic recommends limiting:
- Fruits, especially apples, pears, and watermelon
- Fruit juices and concentrates
- Honey and agave nectar
- High-fructose corn syrup
- Some vegetables like asparagus and artichokes
For lactose intolerance, avoid or limit dairy products or choose lactose-free alternatives.
Enzyme Supplements
Lactase enzyme supplements, taken before consuming dairy, can help people with lactose intolerance digest milk products without symptoms. These are widely available over-the-counter.
Enzyme supplements for sucrose intolerance (containing sucrase) exist but are less commonly available and may require prescription.
No enzyme supplements effectively address fructose malabsorption.
Sugar Alternatives
Several sugar substitutes can provide sweetness without triggering intolerance symptoms:
- Glucose (dextrose) for those with fructose or sucrose issues
- Stevia and monk fruit sweeteners
- Sugar alcohols like erythritol (though some people experience digestive upset)
- Artificial sweeteners like aspartame or sucralose
Individual tolerance varies. What works for one person may cause problems for another.
| Sugar Type | Who Should Avoid | Better Alternatives |
|---|---|---|
| Sucrose (table sugar) | Sucrose intolerance | Glucose, stevia, erythritol |
| Fructose | Fructose intolerance | Glucose, small amounts of stevia |
| Lactose | Lactose intolerance | Lactose-free dairy, plant milks |
| High-fructose corn syrup | Fructose intolerance | Glucose-based sweeteners |
When to See a Healthcare Provider
Mayo Clinic recommends seeking medical evaluation if:
- Symptoms are severe, persistent, or worsening
- Digestive problems significantly impact quality of life
- Unintended weight loss occurs
- Blood appears in stool
- Symptoms suggest allergic reaction (hives, swelling, breathing difficulty)
More than 20% of the population in industrialized countries suffers from food intolerance or food allergy, according to research published in Deutsches Ärzteblatt International. These conditions are understudied and often overlooked.
Getting proper diagnosis matters. Self-diagnosing and unnecessarily restricting foods can lead to nutritional deficiencies. Professional evaluation ensures accurate identification of the problem and appropriate management.
For suspected allergic reactions, seek immediate emergency care. True food allergies can be life-threatening.
The Bottom Line on Sugar and Health
Research continues to explore the complex relationships between sugar consumption and various health conditions. Community discussions online describe experiences with sugar causing neuropathy symptoms, autoimmune flares, and other issues beyond digestive problems.
Some of these connections may involve inflammation, blood sugar fluctuations, or other metabolic effects rather than allergy or intolerance per se. The science remains incomplete in many areas.
What’s clear: excessive sugar consumption creates health risks regardless of allergy or intolerance status. High-sugar diets contribute to obesity, type 2 diabetes, heart disease, and other chronic conditions.
REMOVE – American Heart Association recommendation not found in provided source materials Most Americans consume far more.
Frequently Asked Questions
Sugar intolerance can develop at any age. Lactose intolerance commonly appears in adolescence or adulthood as lactase production naturally decreases. Sucrose and fructose intolerances may be present from birth or develop later. True sugar allergies remain extremely rare and poorly documented regardless of age of onset.
If specific digestive symptoms (bloating, gas, diarrhea, cramping) consistently appear within hours of eating sugar-containing foods and improve when avoiding those foods, intolerance is possible. Excessive sugar consumption causes different problems like energy crashes, weight gain, and increased disease risk. Professional testing can distinguish between intolerance, other digestive conditions, and general overconsumption effects.
Sucrose intolerance is a digestive problem caused by lack of the sucrase enzyme, leading to undigested sugar fermenting in the gut. Diabetes is a metabolic disorder involving insulin and blood glucose regulation. They’re completely different conditions with different causes, symptoms, and treatments. Someone can have one without the other, or both simultaneously.
Severe sugar intolerance causing chronic diarrhea and malabsorption can potentially contribute to weight loss, though this isn’t the primary symptom. Anyone experiencing unintended weight loss should see a healthcare provider, as this can indicate serious underlying conditions requiring evaluation beyond sugar intolerance.
It depends on the specific intolerance and sweetener. Glucose works for people with fructose or sucrose issues. Stevia and monk fruit typically don’t cause problems. Sugar alcohols like sorbitol and xylitol can cause digestive upset in many people, even without sugar intolerance. Artificial sweeteners like aspartame and sucralose don’t contain sugars but individual tolerance varies. Testing different options helps identify what works best.
For suspected sugar intolerance with primarily digestive symptoms, start with a gastroenterologist or primary care physician who can order appropriate breath tests and coordinate elimination diets. If symptoms suggest allergic reaction (hives, swelling, breathing difficulty, or anaphylaxis), see an allergist immediately. Many cases benefit from coordinated care between both specialists.
This depends on the type and cause. Temporary lactose intolerance can occur after intestinal infections and resolve completely. Congenital sucrase-isomaltase deficiency is genetic and lifelong, though enzyme production may improve somewhat with age. Some children with fructose malabsorption develop better tolerance over time. Unlike some protein-based food allergies that children commonly outgrow, sugar intolerances typically persist or fluctuate rather than completely resolve.
Take Control of Sugar-Related Symptoms
The evidence is clear: true sugar allergies are exceptionally rare. If sugar makes you feel terrible, intolerance is the far more likely culprit.
Understanding the distinction matters enormously. Allergies require strict avoidance and emergency preparedness. Intolerances involve enzyme deficiencies that create dose-dependent digestive symptoms manageable through dietary modification.
Don’t guess about what’s causing your symptoms. Proper testing identifies the specific problem and guides effective treatment. Over 20% of people in industrialized countries experience some form of food intolerance or allergy, yet many never receive accurate diagnosis.
Track your symptoms carefully. Note which foods trigger problems, how much causes issues, and how quickly symptoms appear. This information helps healthcare providers diagnose efficiently.
If sugar consistently causes problems, see a healthcare provider. Whether the issue is intolerance, another digestive condition, or something else entirely, proper diagnosis opens the door to effective management and improved quality of life.
