Quick Summary: Yes, it is possible to exercise too much. Excessive exercise without adequate recovery can lead to overtraining syndrome, exercise-induced rhabdomyolysis (a dangerous muscle breakdown condition), mental health issues, and weakened immune function. The key is balancing training intensity with proper rest and listening to your body’s warning signals.
Health experts universally recommend regular physical activity. According to the World Health Organization, adults should aim for moderate-intensity exercise most days of the week. Physical inactivity is one of the leading risk factors for noncommunicable diseases worldwide.
But here’s the thing though—you can absolutely get too much of a good thing.
When exercise crosses from beneficial to harmful, the consequences can range from frustrating performance plateaus to life-threatening medical emergencies. Understanding where that line exists matters for everyone from casual gym-goers to competitive athletes.
What Happens When Training Becomes Overtraining
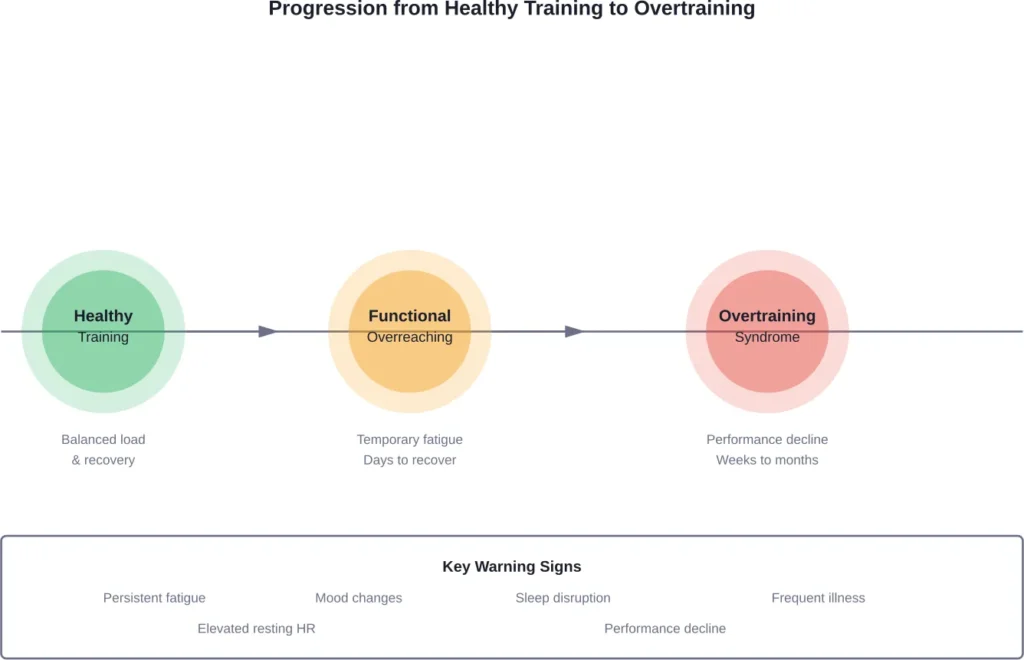
Overtraining syndrome happens when the body doesn’t have adequate time to recover between intense physical activity sessions. The condition develops gradually as training load exceeds recovery capacity over weeks or months.
The physiology behind overtraining involves complex disruptions to hormonal balance, immune function, and cellular repair processes. Without sufficient rest, muscle tissue breaks down faster than it rebuilds. Stress hormones remain chronically elevated while performance paradoxically declines.
Athletes and fitness enthusiasts often miss the early warning signs. Many interpret fatigue and declining performance as signals to train harder rather than rest more. This creates a vicious cycle that drives deeper into overtraining territory.
Common Overtraining Symptoms
Physical symptoms include persistent muscle soreness that doesn’t resolve, unexplained fatigue even after rest days, increased susceptibility to colds and infections, and elevated resting heart rate. Performance markers decline—previously manageable workouts feel impossibly hard.
Mental health symptoms deserve equal attention. Overtraining frequently causes mood disturbances, increased irritability, depression, difficulty concentrating, and disrupted sleep patterns. The cognitive impact can be substantial enough that tests like the Stroop Colour Test show measurable deficits in overtrained endurance athletes.
Recovery timelines vary based on severity. According to Cleveland Clinic, providers typically recommend reducing training intensity and frequency by 50% to 70%. Real talk: if training ramps up again before full recovery, all progress resets and the condition worsens.
Exercise-Induced Rhabdomyolysis: A Medical Emergency
Exercise-induced rhabdomyolysis represents the most dangerous consequence of excessive exercise. This condition involves the breakdown of skeletal muscle tissue, releasing muscle cell contents into the bloodstream.
The released proteins, particularly myoglobin, can cause acute kidney injury and in severe cases, death. According to medical research published in the National Library of Medicine, five out of 25 patients in one study experienced acute kidney injury requiring temporary renal replacement therapy.
Rhabdomyolysis most commonly strikes after intense, unfamiliar exercise—particularly eccentric movements or high-intensity workouts in hot conditions. Case reports document young, otherwise healthy individuals developing this condition after starting aggressive exercise programs.
Recognizing Rhabdomyolysis Symptoms
The classic triad includes severe muscle pain, weakness, and dark urine (often described as tea or cola-colored). Additional symptoms include muscle swelling, dehydration, elevated heart rate, and general malaise.
One documented case involved a 19-year-old man who presented to the emergency department with bilateral leg pain and dark urine after starting intense aerobic exercise. His creatine kinase levels—a marker of muscle damage—were significantly elevated, and he developed acute kidney injury.
Medical attention is critical. Rhabdomyolysis requires prompt recognition and aggressive treatment with intravenous fluids to prevent permanent kidney damage.
Mental Health Impacts of Excessive Exercise
The relationship between exercise and mental health isn’t purely linear—more isn’t always better.
Compulsive exercise behaviors can develop, particularly among athletes and performers. While no single factor causes eating disorders, research confirms that athletes face higher risk than the general population. The emphasis on size, weight, diet, and perfectionism in competitive environments creates additional vulnerability.
Exercise addiction shares characteristics with other addictive behaviors. Individuals feel compelled to exercise despite injury, fatigue, or other negative consequences. They experience withdrawal symptoms when unable to train and continue increasing volume despite diminishing returns.
The psychological burden of overtraining includes increased anxiety, depression, irritability, and reduced self-esteem. These mental health effects often precede measurable physical performance declines.
Special Populations at Higher Risk
Young athletes deserve particular attention. Research on overuse injuries shows that imbalances between training load and recovery have important negative consequences for children and adolescents. Their developing bodies require proportionally more recovery time.
According to the CDC, individuals with certain conditions like ME/CFS (Myalgic Encephalomyelitis/Chronic Fatigue Syndrome) must be especially cautious. For these patients, post-exertional malaise represents a core symptom where physical or mental exertion triggers symptom worsening that can last days or weeks.
Endurance athletes face unique challenges. The cumulative training volume required for marathon running, cycling, or triathlon training pushes recovery systems to their limits. Small miscalculations in training progression can tip the balance toward overtraining.
| Population | Specific Risks | Key Considerations |
|---|---|---|
| Young Athletes | Growth plate injuries, burnout, psychological stress | Require more recovery time; limit sport specialization |
| Endurance Athletes | Overtraining syndrome, immune suppression | Monitor training load carefully; prioritize recovery |
| Individuals with ME/CFS | Post-exertional malaise, severe symptom worsening | Exercise must be carefully managed with healthcare provider |
| Older Adults (50+) | Longer recovery times, increased injury risk | Focus on recovery strategies, hydration, adequate rest |
Finding Your Optimal Exercise Balance
So how much exercise is appropriate? The answer varies individually based on fitness level, training history, genetics, stress levels, sleep quality, and nutrition.
According to the American College of Sports Medicine (ACSM), recovery strategies become increasingly important for active adults over 50. While post-workout recovery looks different compared to younger decades, this shift allows for strategic approaches to maintain performance.
General guidelines suggest most adults benefit from 150 minutes of moderate-intensity or 75 minutes of vigorous-intensity activity weekly. But these represent minimums for health benefits—not maximums before harm occurs.
Prevention Strategies
Preventing overtraining requires proactive monitoring. Track resting heart rate, sleep quality, mood, and subjective energy levels. Significant changes in these markers often precede objective performance declines.
Periodization—systematically varying training intensity and volume—gives the body necessary recovery windows. Hard training blocks should be followed by lighter recovery periods.
Nutrition and hydration directly impact recovery capacity. According to ACSM guidance, drink about 2 cups of water in the hour before workouts, about 1 cup every 15 minutes during exercise, and focus on replacement throughout the day after training.
Sleep represents the most powerful recovery tool available. Inadequate sleep undermines all other recovery efforts and accelerates progression toward overtraining.

When to Seek Medical Help
Certain symptoms require immediate medical evaluation. Dark urine following intense exercise suggests possible rhabdomyolysis. Seek emergency care immediately.
Persistent symptoms that don’t improve with rest—lasting more than two weeks—warrant professional assessment. Healthcare providers can order blood tests to check for markers of overtraining, muscle damage, or other underlying conditions.
Performance declines accompanied by mood changes, sleep disturbances, and persistent fatigue may indicate overtraining syndrome requiring structured recovery protocols under medical supervision.
Frequently Asked Questions
There’s no universal threshold because tolerance varies individually. Generally speaking, more than 10-12 hours of intense training weekly without adequate recovery increases overtraining risk for most recreational athletes. Elite athletes may handle more but require careful monitoring and periodization.
Early warning signs include unexplained fatigue that doesn’t resolve with normal rest, elevated resting heart rate, difficulty sleeping, increased irritability or mood changes, and workouts feeling harder than usual at the same intensity. Performance plateaus or declines despite consistent training also signal potential overtraining.
Yes, full recovery is possible but requires significant rest—typically weeks to months depending on severity. Treatment involves reducing training volume by 50-70%, prioritizing sleep and nutrition, and gradually reintroducing activity only after symptoms resolve. Rushing back too quickly resets progress and worsens the condition.
Rhabdomyolysis is the breakdown of skeletal muscle tissue that releases harmful proteins into the bloodstream, potentially causing kidney damage. Anyone can develop it, but risk increases with intense unfamiliar exercise, particularly in hot conditions, after prolonged inactivity, or when combining exercise with dehydration, certain medications, or supplements.
Exercising daily isn’t inherently harmful if intensity, volume, and exercise types are varied appropriately. Light activity or active recovery most days poses minimal risk. However, high-intensity training every day without rest increases injury and overtraining risk. Most experts recommend at least one complete rest day weekly.
Prevention strategies include gradual progression when starting new programs, adequate hydration before and during exercise, avoiding training in extreme heat, listening to body signals, and not combining multiple risk factors like dehydration, stimulants, and intense unfamiliar exercise. Stop immediately if experiencing severe muscle pain or dark urine.
Yes, excessive training volume without adequate recovery suppresses immune function, increasing susceptibility to infections. This phenomenon, sometimes called the “open window” effect, occurs because chronic overtraining creates systemic stress that impairs immune cell function and inflammatory responses.
Conclusion: Balance Is Everything
Exercise remains one of the most powerful tools for physical and mental health. The benefits are well-established and significant.
But the dose matters critically. Training without adequate recovery doesn’t build fitness—it breaks down the body. The line between optimal training and overtraining exists for everyone, though its location varies individually.
Pay attention to your body’s signals. Track recovery markers. Prioritize sleep and nutrition alongside training. Remember that rest days aren’t wasted days—they’re when adaptation actually occurs.
If you’re experiencing persistent fatigue, declining performance, mood changes, or other warning signs, scale back training volume and consult a healthcare provider. The goal isn’t just to exercise more—it’s to optimize the balance between training stress and recovery that allows genuine, sustainable progress.
