Quick Summary: While uncommon, pregnancy during menstruation is possible. According to ACOG, sperm can survive in the body for up to 5 days, and some women ovulate earlier than expected. Women with shorter or irregular cycles face higher risk, as do those who experience breakthrough bleeding mistaken for a period.
The belief that menstruation offers complete protection against pregnancy is surprisingly common. But here’s the thing—biology doesn’t always follow a predictable schedule.
Many women rely on cycle timing to avoid pregnancy, assuming their period creates a “safe zone.” Research found that about 85% of women lack correct knowledge about the fertile window. This misconception can lead to unintended pregnancies.
Understanding the nuances of ovulation, sperm survival, and menstrual cycle variability is essential for anyone trying to prevent or achieve pregnancy.
Understanding the Fertile Window
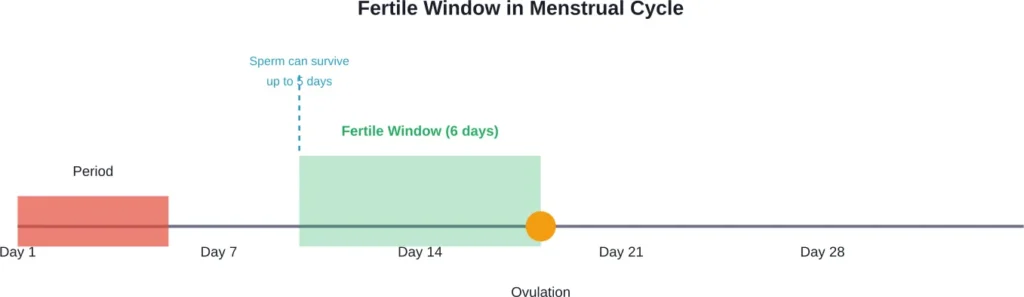
The fertile window represents the days when pregnancy can occur. According to NIH research (Wilcox et al., BMJ 2000) tracking 221 healthy women planning pregnancy, the fertile window spans approximately six days ending on ovulation day.
According to ACOG, sperm can survive inside a woman’s body for about 3 days (and sometimes up to 5 days) after sexual intercourse. Meanwhile, an egg remains viable for about 12 to 24 hours after ovulation. This creates a window where intercourse occurring days before ovulation can still result in pregnancy.
The math matters here. If intercourse happens five days before ovulation, sperm can wait in the fallopian tubes until the egg releases. This biological reality explains why timing isn’t as straightforward as many assume.
Why Pregnancy During Your Period Can Happen
The textbook menstrual cycle lasts 28 days, with ovulation occurring around day 14. Reality? Much messier.
Some studies suggest that only about 30% of women ovulate between days 10 and 17 of their cycle. Some ovulate significantly earlier, particularly women with shorter cycles.
Early Ovulation Risk
Women with 21-24 day cycles may ovulate as early as day 7 or 8. If menstruation lasts 5-7 days and intercourse occurs on days 4-5 of the period, sperm can survive until ovulation occurs just days later.
This overlap creates genuine pregnancy risk during what appears to be a “safe” time.
Breakthrough Bleeding Confusion
Not all vaginal bleeding represents menstruation. Breakthrough bleeding—light spotting that occurs mid-cycle—can be mistaken for a period. Women may believe they’re menstruating when they’re actually in their fertile window.
Hormonal fluctuations, cervical irritation, or implantation bleeding can all cause spotting that mimics menstruation.
Cycle Length and Pregnancy Risk
Cycle variability directly impacts pregnancy risk during menstruation. According to the CDC’s Standard Days Method guidance, approximately 13 out of 100 SDM users become pregnant in the first year with typical use.
| Cycle Length | Typical Ovulation Day | Period Sex Risk |
|---|---|---|
| 21-23 days | Day 7-9 | Higher risk |
| 24-27 days | Day 10-13 | Moderate risk |
| 28-32 days | Day 14-18 | Lower risk |
| Irregular cycles | Unpredictable | Unpredictable risk |
Women with irregular cycles face the highest uncertainty. When ovulation timing varies significantly month to month, predicting safe days becomes nearly impossible.
How Long Sperm Actually Survives
Sperm longevity isn’t uniform. According to ACOG, sperm can survive inside a woman’s body for about 3 days, and sometimes up to 5 days under optimal conditions.
Cervical mucus quality affects survival rates. Around ovulation, fertile-quality cervical mucus provides nutrients and protection that extend sperm lifespan. During menstruation, conditions are less hospitable, but resilient sperm can still persist.

What the Research Actually Shows
Research found that only one-third of urban mothers interviewed answered correctly about when during the menstrual cycle pregnancy is most likely. This knowledge gap persists across demographics.
The NIH study tracking 696 menstrual cycles provided specific data on fertile window timing. The research demonstrated that while most fertile days cluster around ovulation, the window’s position within the cycle varies considerably between women.
At least 85% of women who continue to have sex without birth control, even just once in a while, will be pregnant within one year. The timing matters less than many assume.
Contraception Remains Essential
Relying on menstruation for pregnancy prevention is fundamentally unreliable. The CDC’s recommendations for assessing pregnancy risk emphasize that detailed history provides better assessment than assumptions about cycle timing.
Effective contraception options include:
- Hormonal methods (pills, patches, rings, implants)
- Intrauterine devices (IUDs)
- Barrier methods (condoms, diaphragms)
- Permanent options (sterilization)
For those using fertility awareness methods, tracking requires consistent monitoring of multiple fertility signs—not just calendar dates. Basal body temperature, cervical mucus changes, and ovulation predictor kits provide more reliable data than cycle day counting alone.
Special Considerations
Postpartum and Post-Abortion Ovulation
According to CDC guidance, the likelihood of ovulation is low ≤7 days after an abortion. For postpartum nonlactating women, a systematic review reported that the mean day of first ovulation occurred 45–94 days after delivery, with the earliest ovulation reported at 25 days after delivery.
These timelines matter because vaginal bleeding during these periods may not represent true menstruation, yet ovulation can occur before the first period returns.
Age-Related Fertility Changes
ACOG notes that a woman’s peak reproductive years are between the late teens and late 20s, and fertility starts to decline by age 30, with more significant decreases after 35. However, pregnancy remains possible during menstruation at any reproductive age when ovulation timing and sperm survival align.
Frequently Asked Questions
Ovulation during active menstrual bleeding is extremely rare. However, women with very short cycles may ovulate shortly after their period ends, creating overlap when sperm from late-period intercourse remains viable.
Risk increases toward the end of menstruation, particularly for women with shorter cycles. Days 1-2 of heavy bleeding carry minimal risk, while days 5-7 present higher risk if ovulation occurs early.
According to CDC guidance, approximately 13 out of 100 SDM users become pregnant in the first year with typical use. Effectiveness depends heavily on consistent, accurate tracking and cycle regularity.
Irregular bleeding makes pregnancy risk harder to predict because ovulation timing becomes unpredictable. What appears to be menstruation might be breakthrough bleeding occurring during the fertile window.
Pre-ejaculate fluid can contain sperm, making pregnancy possible even without full ejaculation. Withdrawal isn’t reliable contraception during any part of the cycle, including menstruation.
Pregnancy can occur immediately after menstruation ends, especially with shorter cycles. Women with 21-day cycles may ovulate around day 7, making intercourse on days 2-5 potentially lead to conception.
If pregnancy prevention is important and no contraception was used, emergency contraception remains an option. It’s most effective when taken within 72 hours of unprotected intercourse, though some types work up to 5 days after.
The Bottom Line
Pregnancy during menstruation isn’t common, but it’s biologically possible. The combination of early ovulation, sperm longevity, and cycle irregularity creates genuine risk for some women.
Cycle tracking alone provides insufficient protection against unintended pregnancy. Women with shorter cycles, irregular patterns, or those who mistake breakthrough bleeding for menstruation face elevated risk.
Effective contraception remains the only reliable method for pregnancy prevention. Understanding how ovulation timing, sperm survival, and individual cycle characteristics interact helps make informed decisions about sexual health and family planning.
If avoiding pregnancy is the goal, consistent contraceptive use throughout the entire cycle—including during menstruation—is essential. For those trying to conceive, recognizing that fertility extends beyond textbook ovulation days may inform timing strategies.