Quick Summary: Yes, it is theoretically possible to get pregnant while already pregnant through an extremely rare phenomenon called superfetation, where a second egg is fertilized and implants days or weeks after the first conception. However, this occurs in fewer than a handful of documented human cases worldwide, making it one of the rarest pregnancy phenomena known to medicine.
It sounds like something from a sci-fi novel. But the question “can you get pregnant while already pregnant?” has a real answer—and it’s more complicated than you’d think.
The short answer? Yes, but your chances are essentially zero.
This phenomenon is called superfetation, and it’s so rare that medical literature contains only a handful of confirmed human cases. Yet it challenges everything we think we know about how pregnancy works.
Here’s what science tells us about this extraordinary event.
What Is Superfetation?
Superfetation is the occurrence of ovulation, fertilization, and implantation during an ongoing pregnancy. Essentially, the body releases another egg while already pregnant, that egg gets fertilized, and it implants in the uterus alongside the existing pregnancy.
The result? Two fetuses developing at different gestational ages—sometimes days apart, sometimes weeks.
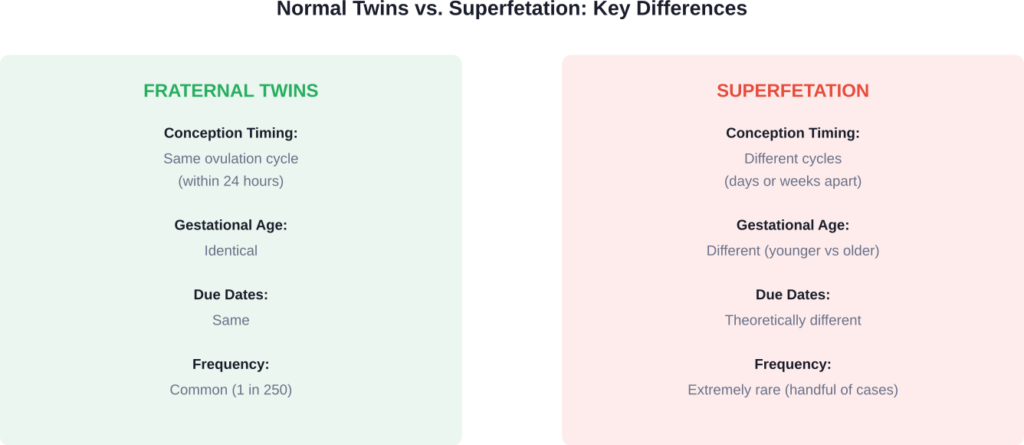
This differs from regular twins. Fraternal twins happen when two eggs are released during the same menstrual cycle and both get fertilized around the same time. With superfetation, the second conception happens after pregnancy has already begun.
According to medical research published in Clinical Case Reports, superfetation represents one of the rarest documented pregnancy phenomena. The babies develop on different timelines, potentially with different due dates.
Why Is Getting Pregnant While Pregnant Nearly Impossible?
The human body has built-in biological locks that prevent superfetation. Understanding these mechanisms shows why this phenomenon almost never occurs.
Hormonal Shutdown of Ovulation
Once conception occurs, hormonal changes rapidly shut down the ovulation process. The corpus luteum produces progesterone, which prevents the release of additional eggs. This hormonal shift typically happens within days of fertilization.
Pregnancy hormones, particularly human chorionic gonadotropin (hCG), signal the body to stop the menstrual cycle entirely.
The Mucus Plug Barrier
Early in pregnancy, the cervix forms a thick mucus plug that seals off the uterus from the vagina. This barrier protects the developing fetus from bacteria and other external threats—including sperm.
For superfetation to occur, sperm would need to bypass this barrier and reach the fallopian tubes.
Uterine Lining Changes
After implantation, the uterine lining (endometrium) transforms to support the existing pregnancy. These changes typically make the environment inhospitable for another embryo to implant.
The endometrium becomes decidualized, creating conditions specifically tailored to the first pregnancy.

How Rare Is Superfetation Really?
Extraordinarily rare. Medical literature contains fewer than a dozen well-documented human cases in peer-reviewed sources.
The phenomenon is better documented in animals. Rabbits, rodents, and some other mammals can experience superfetation more readily because their reproductive physiology differs from humans.
In humans, every confirmed case represents a perfect storm of biological anomalies where all three protective mechanisms failed simultaneously.
The Connection to Assisted Reproductive Technology
Interestingly, heterotopic pregnancy—where one embryo implants in the uterus while another implants outside it (ectopic)—has increased with assisted reproductive technology. According to research published in Clinical Case Reports, heterotopic pregnancy occurs in approximately 1 in 30,000 spontaneous pregnancies but in pregnancies achieved through ART the incidence has been reported as high as 1%.
Some suspected superfetation cases have occurred in women undergoing fertility treatments involving ovulation induction. These treatments intentionally override the body’s normal hormonal controls, potentially creating windows for superfetation.
How Would You Know If You Had Superfetation?
Diagnosing superfetation is extremely challenging. Most cases are identified retrospectively—after delivery—when medical teams realize the babies show different developmental stages that can’t be explained by standard twin growth variations.
Diagnostic Indicators
Ultrasound examinations might reveal:
- Two fetuses with significantly different size measurements inconsistent with standard twin development
- Different gestational sac sizes beyond normal twin variation
- Developmental milestones occurring at different times
- Distinct placental structures with different maturity levels
According to ACOG (American College of Obstetricians and Gynecologists), approximately half of women accurately recall their last menstrual period. In superfetation cases, dating pregnancies becomes even more complex since the conceptions occurred at different times.
Superfetation vs. Other Twin Phenomena
It’s crucial to distinguish superfetation from more common scenarios that might appear similar.
| Phenomenon | Timing of Conception | Frequency | Key Difference |
|---|---|---|---|
| Fraternal Twins | Same ovulation cycle | Common (1 in 250 births) | Both eggs fertilized within same 24-hour window |
| Superfecundation | Same cycle, different acts | Rare but documented | Two eggs fertilized by sperm from different partners or different times within same fertile window |
| Superfetation | Different cycles entirely | Extremely rare (handful of cases) | Second conception occurs days/weeks after first pregnancy established |
| Twin Growth Discordance | Same time | Relatively common | Twins conceived simultaneously but one grows slower due to placental issues |
Many suspected superfetation cases turn out to be twin growth discordance, where one twin receives fewer nutrients and develops more slowly.
What Happens During Delivery?
Superfetation creates unique challenges for delivery timing. The fetuses have different gestational ages, meaning they would theoretically have different due dates.
In documented cases, providers typically deliver both babies at the same time, even though one may be slightly less mature. Waiting for the second baby to reach full term would mean the first baby goes well beyond 40 weeks, creating risks.
The delivery decision balances:
- Optimal timing for the more mature fetus
- Viability concerns for the younger fetus
- Maternal health considerations
- Risk of preterm labor
According to data from CDC’s Assisted Reproductive Technology Surveillance, ART procedures in 2006 resulted in 54,656 infants. These advanced reproductive technologies have given medical teams more experience managing unusual twin scenarios, though superfetation remains exceptionally rare even in these contexts.
Can Normal Pregnancy Prevent Future Conception?
For all practical purposes, yes. Once pregnant, the biological mechanisms outlined earlier prevent additional conception.
According to ACOG, sperm can survive inside the female reproductive tract for about 3 days, and sometimes up to 5 days, after intercourse. An egg survives for about 24 hours after ovulation. But during pregnancy, these normal fertility windows become irrelevant because ovulation ceases.
The Bottom Line on Pregnancy Protection
While superfetation exists as a biological curiosity, it shouldn’t factor into any practical pregnancy considerations.
The human body’s natural pregnancy mechanisms provide essentially foolproof protection against additional conception. The convergence of hormonal, physical, and physiological changes makes superfetation one of the rarest documented pregnancy phenomena.
For anyone concerned about birth control during pregnancy—the scenarios that matter involve completely different considerations, like protecting against sexually transmitted infections or understanding when fertility returns postpartum.
Frequently Asked Questions
No, not under normal circumstances. Pregnancy hormones, particularly progesterone and hCG, suppress ovulation. The extremely rare exceptions involve cases of superfetation where hormonal controls fail, but these represent fewer than a handful of documented cases worldwide.
Superfecundation occurs when two eggs from the same ovulation cycle are fertilized by sperm from different acts of intercourse (potentially even different partners) within the same fertile window. Superfetation involves a second ovulation and conception occurring after pregnancy is already established—days or weeks later.
Diagnosis typically occurs through ultrasound showing two fetuses with developmental differences that exceed normal twin variation. However, many cases are only confirmed after delivery when babies show clear gestational age differences. The condition is so rare that it’s rarely considered as an initial diagnosis.
Yes, in documented cases, both babies are delivered simultaneously even though they have different gestational ages. Waiting for the younger fetus to reach full term would mean the older fetus goes significantly past due date, creating health risks. Providers time delivery to optimize outcomes for both babies.
Possibly, though the evidence is limited given how rare superfetation is overall. Fertility treatments involving ovulation induction intentionally override normal hormonal controls, which could theoretically create conditions for superfetation. Some documented cases have occurred in women undergoing such treatments.
Almost certainly not. Twin growth discordance—where twins conceived at the same time grow at different rates—is relatively common and usually results from placental issues affecting nutrient delivery. True superfetation is extraordinarily rare. Size differences alone don’t indicate superfetation.
No. Identical twins result from a single fertilized egg that splits into two embryos. Superfetation by definition involves two separate ovulation and fertilization events. The babies from superfetation would be fraternal, not identical, since they come from different eggs fertilized at different times.
Conclusion: A Biological Curiosity, Not a Practical Concern
So yes, it’s technically possible to get pregnant while already pregnant. But with fewer than a dozen well-documented human cases in medical literature, superfetation ranks among the rarest pregnancy phenomena known to science.
The human body evolved multiple redundant systems to prevent this exact scenario. Hormonal shutdown, cervical barriers, and uterine changes work together to ensure that once conception occurs, no additional pregnancies can begin.
For anyone navigating pregnancy or trying to conceive, superfetation remains a fascinating edge case in reproductive biology—but not something that should influence practical decision-making or pregnancy planning.
If experiencing an unusual twin pregnancy with significant developmental differences, work closely with maternal-fetal medicine specialists who can provide appropriate monitoring and care, regardless of whether the cause is superfetation or the more common twin growth discordance.
