Quick Summary: Intentional weight loss during pregnancy is not recommended, even for women with obesity. According to the CDC and ACOG, the focus should be on healthy eating and moderate physical activity rather than losing weight. Some weight loss in early pregnancy due to morning sickness is normal, but sustained weight loss throughout pregnancy can pose risks to both mother and baby.
The question of losing weight during pregnancy is more common than most people realize. With maternal obesity rates increasing significantly worldwide, many women enter pregnancy carrying extra weight and wonder if it’s safe—or even beneficial—to shed pounds while expecting.
Here’s the thing though: pregnancy isn’t the time for traditional weight loss efforts.
But that doesn’t tell the whole story. The relationship between pregnancy, weight, and health is more nuanced than a simple yes or no answer. Let’s break down what medical authorities actually recommend and why.
The Medical Consensus: Weight Loss During Pregnancy
According to the American College of Obstetricians and Gynecologists (ACOG), intentional weight loss during pregnancy isn’t recommended for any woman, regardless of starting weight. This includes women who begin pregnancy with obesity.
The CDC supports this position, emphasizing that physical activity and healthy eating during pregnancy should focus on overall health—not weight reduction. Their 2025 guidelines confirm that moderate-intensity physical activity is safe for healthy pregnant women, with a recommendation of 150 minutes of aerobic activity per week.
Sound familiar? It’s the same recommendation for non-pregnant adults, but with a crucial difference in purpose.
Why Not Lose Weight While Pregnant?
The developing baby needs consistent nutrition throughout all stages of pregnancy. Restricting calories or following weight-loss diets can deprive the fetus of essential nutrients needed for growth and development.
Research published by NIH shows that even women with obesity need adequate nutrition during pregnancy. The focus has shifted from weight loss to preventing excessive weight gain and maintaining healthy behaviors.
That said, some weight loss can occur naturally—and that’s where things get interesting.
When Weight Loss During Pregnancy Is Normal
Not all pregnancy weight loss is cause for concern. In fact, some scenarios are perfectly normal and expected.
First Trimester Weight Loss
Many women lose weight during the first trimester due to morning sickness, nausea, and food aversions. This temporary weight loss is typically not harmful if the woman returns to gaining weight appropriately in the second and third trimesters.
Some women report losing weight in early pregnancy due to morning sickness and still go on to have healthy babies. The key is that this weight loss is unintentional and resolves as pregnancy progresses.
Lifestyle Changes Without Dieting
Some women naturally lose weight or maintain their weight during pregnancy by adopting healthier habits. This might include:
- Eliminating alcohol and reducing caffeine intake
- Eating more whole foods and fewer processed items
- Staying active with pregnancy-safe exercise
- Reducing stress-related or emotional eating
These changes aren’t about restricting calories—they’re about improving overall health. The weight loss, if it happens, is a side effect rather than the goal.

Weight Gain Guidelines for Different Body Types
The Institute of Medicine provides gestational weight gain guidelines based on pre-pregnancy body mass index (BMI). These recommendations acknowledge that not all women should gain the same amount of weight during pregnancy.
| Pre-Pregnancy BMI Category | BMI Range | Recommended Total Weight Gain |
|---|---|---|
| Underweight | Less than 18.5 | 28-40 pounds |
| Normal Weight | 18.5-24.9 | 25-35 pounds |
| Overweight | 25.0-29.9 | 15-25 pounds |
| Obese | 30.0 or higher | 11-20 pounds |
Real talk: these are guidelines, not absolute rules. Individual circumstances vary, and healthcare providers may adjust recommendations based on specific health conditions, pregnancy complications, or other factors.
The Obesity Exception
Women with obesity face unique considerations during pregnancy. According to NIH research on clinical management of pregnancy in obese mothers, these women have increased risks of complications including gestational diabetes, preeclampsia, and cesarean delivery.
However—and this is crucial—the recommendation is still not to lose weight during pregnancy. Instead, the focus shifts to gaining less weight than a woman at normal weight would gain, while still ensuring adequate nutrition for fetal development.
Scientific evidence reviewed by the Institute of Medicine was inadequate to support recommendations below 11-20 pounds for women with obesity. Going lower could pose risks that outweigh potential benefits.
Healthy Eating vs. Dieting During Pregnancy
There’s a massive difference between eating healthy during pregnancy and going on a diet. One supports both mother and baby. The other can cause harm.
What Healthy Eating Looks Like
According to ACOG guidelines on healthy eating during pregnancy, the focus should be on nutrient-dense foods rather than calorie restriction:
- Dark leafy greens and colorful vegetables
- Whole grains instead of refined carbohydrates
- Lean proteins from various sources
- Pasteurized dairy products (fat-free or low-fat options available)
- Healthy fats from sources like avocados and nuts
The old saying about “eating for two” is misleading. Pregnant women need additional calories in the second and third trimesters to support fetal growth—roughly equivalent to a sandwich or a serving of yogurt with fruit.
What to Avoid
Restrictive diets, extreme calorie cutting, and weight-loss programs are off the table during pregnancy. This includes popular approaches like intermittent fasting, keto diets, or any program specifically designed for weight loss.
The WHO emphasizes that nutrition counseling during pregnancy should focus on maintaining good nutrition rather than reducing intake.
The Role of Physical Activity
Exercise during pregnancy offers numerous benefits without requiring weight loss as a goal. The CDC’s 2025 guidelines confirm that moderate-intensity physical activity is safe for healthy pregnant women.
Breaking down the recommendation: 150 minutes per week equals just 30 minutes of activity five days a week. And it doesn’t have to happen all at once—three 10-minute walks throughout the day counts toward the total.
Safe Exercise Options
ACOG recommends these activities for most pregnant women:
- Brisk walking
- Swimming and water aerobics
- Stationary cycling
- Modified yoga and Pilates
- Low-impact aerobics
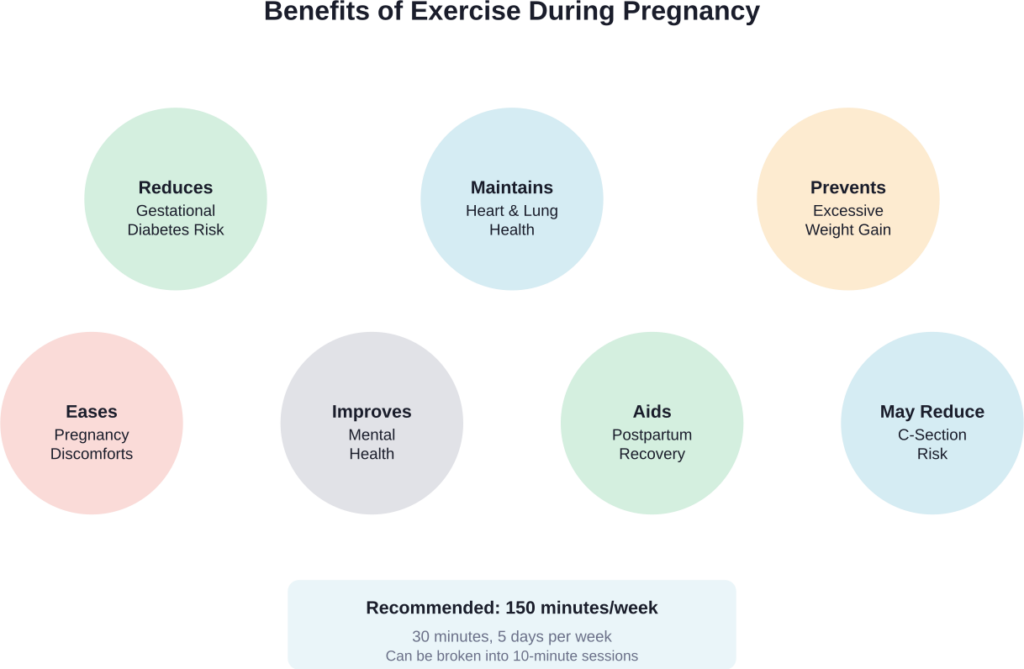
The benefits extend beyond weight management. Regular physical activity during pregnancy can reduce the risk of excessive weight gain, gestational diabetes, preeclampsia, and cesarean delivery. It also helps maintain cardiovascular health and can ease common pregnancy discomforts.
Risks of Being Overweight During Pregnancy
Understanding the risks associated with maternal obesity helps explain why healthcare providers emphasize healthy behaviors rather than weight loss during pregnancy.
NHS guidance on obesity and pregnancy outlines several potential complications for the mother:
- Gestational diabetes
- Preeclampsia (high blood pressure disorder)
- Blood clots
- Postpartum hemorrhage
- Increased likelihood of cesarean delivery
- Difficulties with anesthesia and wound healing
The baby also faces increased risks when the mother has obesity:
- Macrosomia (larger than average birth weight)
- Premature birth
- Birth defects
- Stillbirth (though the absolute risk remains low)
But wait—before this becomes overwhelming, remember that these are statistical increases in risk, not certainties. Many women with obesity have healthy pregnancies and healthy babies, especially with appropriate prenatal care.
When Weight Loss Is a Warning Sign
While some early pregnancy weight loss is normal, sustained or sudden weight loss can signal problems that need medical attention.
Seek immediate healthcare if experiencing:
- Inability to keep food or liquids down for 24 hours
- Signs of dehydration (dark urine, dizziness, rapid heartbeat)
- Severe or persistent nausea and vomiting beyond the first trimester
- Unintentional weight loss of more than 5% of body weight
- Rapid weight loss in the second or third trimester
These symptoms could indicate hyperemesis gravidarum (severe morning sickness), thyroid problems, or other conditions requiring treatment.
The Postpartum Period: A Window of Opportunity
Here’s where the conversation about weight and pregnancy gets more encouraging. CDC research on postpartum weight changes shows that the year after delivery represents a crucial window for addressing weight and reducing future cardiometabolic disease risk.
For women with gestational diabetes, changes in postpartum weight and waist circumference were associated with changes in cardiometabolic risk factors. This finding is particularly significant for women who had obesity during pregnancy.
The postpartum period offers an opportunity to:
- Establish sustainable healthy eating patterns
- Gradually increase physical activity as recovery allows
- Address weight concerns without the constraints of pregnancy
- Build habits that support long-term health
According to ACOG, it’s safe for postpartum women to engage in moderate-intensity physical activity, and the same 150-minute weekly recommendation applies during the first year after delivery.
Working With Healthcare Providers
Managing weight concerns during pregnancy requires partnership with healthcare providers who understand both the risks and the appropriate interventions.
Women with obesity should expect more frequent monitoring during pregnancy. This might include:
- Earlier and more frequent gestational diabetes screening
- Regular blood pressure monitoring for preeclampsia
- Additional ultrasounds to monitor fetal growth
- Consultation with a registered dietitian or nutritionist
- Discussion of appropriate activity levels
These measures aren’t about weight loss—they’re about ensuring the healthiest possible pregnancy outcome given individual circumstances.
Having Honest Conversations
Many women feel judged or uncomfortable discussing weight with healthcare providers. However, research on maternal obesity management emphasizes that addressing this issue is crucial for achieving better health outcomes.
Prepare for prenatal appointments by:
- Tracking current eating patterns honestly
- Documenting physical activity levels
- Writing down questions or concerns about weight
- Being open about any previous weight loss attempts
- Discussing realistic goals for the pregnancy
Healthcare providers should offer evidence-based guidance without shame or blame. If that’s not happening, it may be worth seeking care elsewhere.
Common Myths About Pregnancy Weight
Let’s clear up some misconceptions that circulate in online communities and even among well-meaning friends and family.
Myth: Eating for two means doubling food intake.
Reality: Additional calories are needed in the second and third trimesters to support the pregnancy—not double the calories.
Myth: All pregnancy weight is fat.
Reality: Weight gain includes the baby, placenta, amniotic fluid, increased blood volume, breast tissue, and stored nutrients—not just body fat.
Myth: Losing weight during pregnancy is always dangerous.
Reality: Some first-trimester weight loss is normal, and adopting healthier habits may result in weight maintenance or modest loss without deliberate restriction.
Myth: Women with obesity shouldn’t gain any weight during pregnancy.
Reality: Even women with obesity should gain 11-20 pounds according to Institute of Medicine guidelines to support fetal development.
Myth: Exercise during pregnancy is risky.
Reality: Moderate-intensity exercise is safe and beneficial for most pregnant women according to CDC and ACOG guidelines.
Frequently Asked Questions
Weight loss during the first trimester is common due to morning sickness, nausea, and food aversions. This is typically not concerning if it’s unintentional and resolves as pregnancy progresses. However, if experiencing severe vomiting or inability to keep food down, contact a healthcare provider as this may indicate hyperemesis gravidarum requiring treatment.
No. Even women with obesity should not intentionally lose weight during pregnancy. The recommendation is to gain less than women at normal weight (11-20 pounds total), but still gain some weight to support fetal development. Focus on healthy eating and appropriate physical activity rather than weight loss.
Recommended weight gain depends on pre-pregnancy BMI. Women at normal weight should gain 25-35 pounds, overweight women 15-25 pounds, and women with obesity 11-20 pounds. Individual circumstances may lead healthcare providers to adjust these recommendations.
Yes. According to the CDC and ACOG, moderate-intensity physical activity is safe for most pregnant women regardless of starting weight. Aim for 150 minutes per week of activities like brisk walking, swimming, or prenatal yoga. Always discuss exercise plans with a healthcare provider, especially if new to physical activity.
Seek medical attention for inability to keep food or liquids down for 24 hours, signs of dehydration, severe nausea persisting beyond the first trimester, or unintentional weight loss exceeding 5% of body weight. Rapid weight loss in the second or third trimester also requires immediate evaluation.
Restrictive diets are not recommended during pregnancy. Instead, focus on eating nutrient-dense whole foods, appropriate portion sizes, and staying active. Working with a registered dietitian can help create a healthy eating plan that supports pregnancy without unnecessary restriction.
Gaining within recommended guidelines doesn’t necessarily make postpartum weight loss harder. The postpartum period actually represents an important opportunity for establishing healthy habits. Many women gradually return to their pre-pregnancy weight within a year through balanced eating and appropriate physical activity as recovery allows.
Moving Forward With Confidence
The question of whether it’s possible to lose weight during pregnancy has a clear answer from medical authorities: intentional weight loss isn’t recommended, but healthy behaviors absolutely are.
The focus during pregnancy should be on nourishing the body, supporting fetal development, and maintaining overall health through balanced nutrition and appropriate physical activity. For women with obesity, this means gaining less weight than women at normal weight, but still gaining some weight to support the baby’s growth.
Some weight loss may occur naturally in early pregnancy or as a side effect of healthier habits, and that’s typically fine. The distinction lies in intention—pursuing weight loss as a goal versus allowing it to happen naturally while prioritizing health.
Working closely with healthcare providers throughout pregnancy ensures that both mother and baby receive appropriate monitoring and support. This partnership becomes even more important for women with obesity who face increased risks but can still achieve healthy pregnancy outcomes with proper care.
The postpartum period offers a genuine opportunity to address weight concerns when the constraints of pregnancy no longer apply. That first year after delivery represents a window for establishing sustainable habits that support long-term health.
If currently pregnant or planning pregnancy, schedule a preconception or prenatal visit to discuss weight, nutrition, and activity with a healthcare provider. Getting individualized guidance based on specific circumstances provides the foundation for the healthiest possible pregnancy journey.
