Quick Summary: Type 2 diabetes can be put into remission through significant weight loss, with studies showing that losing just 5-7% of body weight can restore normal blood sugar levels without medication. While not technically a cure, remission is achievable through intensive lifestyle changes, low-calorie diets, or bariatric surgery. Type 1 diabetes cannot be reversed, as it’s an autoimmune condition requiring lifelong insulin therapy.
More than 38 million Americans live with diabetes, and many receive their diagnosis believing it’s a lifelong sentence. The conventional wisdom for decades painted diabetes as a chronic, progressive disease that only gets worse over time.
But here’s the thing — that paradigm is shifting.
Research now demonstrates that Type 2 diabetes doesn’t have to be permanent. With the right interventions, it’s possible to achieve remission, meaning blood sugar levels return to normal without medication. The key lies in understanding what actually causes the condition and which interventions can reverse those underlying mechanisms.
Understanding the Different Types of Diabetes
Not all diabetes is the same, and this distinction matters when discussing reversal potential.
Type 1 diabetes is an autoimmune condition where the body’s immune system attacks and destroys insulin-producing cells in the pancreas. This results in little to no insulin production, requiring lifelong insulin therapy. Type 1 diabetes cannot be reversed because the insulin-producing cells are permanently destroyed.
Type 2 diabetes develops differently. It begins with insulin resistance, where cells don’t respond properly to insulin, forcing the pancreas to produce more and more insulin to keep blood sugar levels in check. Over time, the pancreas can’t keep up with this demand, and blood sugar levels rise. According to the CDC, almost 35% of U.S. adults have prediabetes, the precursor stage to Type 2 diabetes.
The critical difference? Type 2 diabetes is rooted in metabolic dysfunction that can potentially be reversed, rather than permanent cell destruction.
What Does Diabetes Remission Actually Mean?
Medical professionals have moved away from using the term “cure” and instead refer to “remission” when discussing diabetes reversal.
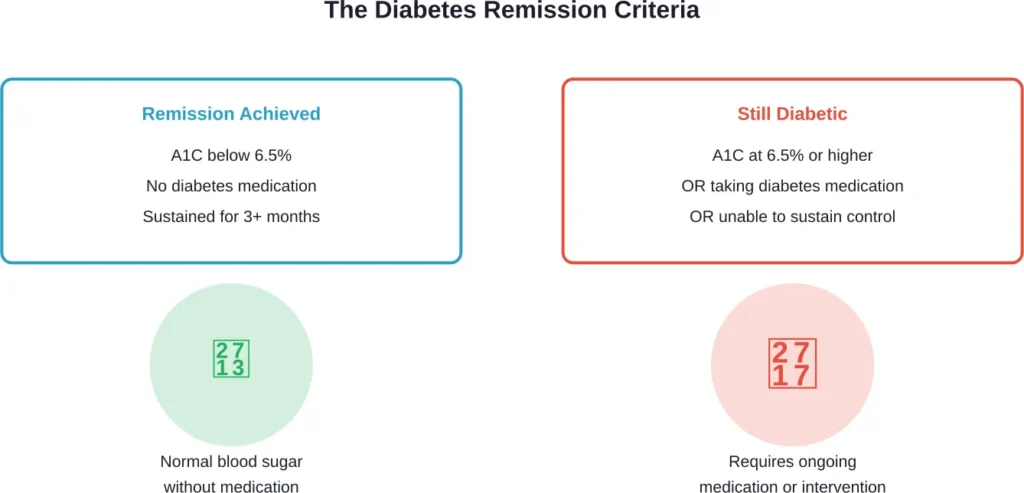
Diabetes remission is defined as having an A1C level below 6.5% (the diagnostic threshold for diabetes) while being off diabetes medications for at least three months. This represents a return to normal blood sugar regulation without pharmaceutical intervention.
Remission doesn’t mean diabetes is gone forever. The condition can return, especially if someone regains weight or reverts to previous lifestyle patterns. That’s why sustained lifestyle changes are essential for maintaining remission long-term.
The Role of Weight Loss in Diabetes Reversal
Weight loss stands as the most powerful intervention for achieving Type 2 diabetes remission.
According to the CDC, losing just 5% of body weight can help reverse prediabetes. For someone weighing 200 pounds, that’s only 10 pounds. Even this modest weight loss can significantly improve insulin sensitivity and blood sugar control.
But for those already diagnosed with Type 2 diabetes, more substantial weight loss typically produces better results. Clinical trials referenced by the NIH demonstrate that significant weight loss through calorie restriction or bariatric surgery can lead to remission in many cases.
How Weight Loss Reverses Diabetes
The mechanism isn’t mysterious. Excess body fat, particularly around the abdomen and organs, drives insulin resistance. This visceral fat releases inflammatory compounds and hormones that interfere with insulin signaling.
When substantial weight is lost, several things happen:
- Fat is removed from the liver and pancreas, allowing these organs to function more normally
- Insulin sensitivity improves as inflammatory markers decrease
- The pancreas can produce adequate insulin without being overworked
- Blood sugar levels normalize as cells become more responsive to insulin
The improvements can happen remarkably quickly. Some patients see blood sugar levels drop within days of starting intensive weight loss interventions, well before significant weight is actually lost.
Evidence-Based Strategies for Diabetes Remission
Low-Calorie Diet Interventions
The Diabetes Remission Clinical Trial (DiRECT) demonstrated substantial success using total diet replacement with low-calorie formulas followed by food reintroduction and behavioral support. While the full details aren’t specified in available sources, the approach showed that structured calorie restriction could achieve remission.
Low-calorie diets typically involve consuming 800-1,200 calories daily for a defined period, usually under medical supervision. This aggressive approach triggers rapid weight loss and metabolic improvements.
Bariatric Surgery
According to NIH research, bariatric surgery produces some of the highest remission rates for Type 2 diabetes. Dr. David Arterburn’s research with the National Patient-Centered Clinical Research Network analyzed five-year outcomes for bariatric surgery patients.
The surgery works through multiple mechanisms beyond just weight loss:
- Physical restriction limits food intake
- Hormonal changes affect hunger and satiety signals
- Alterations in gut hormones like GLP-1 improve insulin secretion
- Changes in bile acid circulation affect metabolism
However, the research also revealed that relapse from diabetes remission can occur within five years for some patients who undergo bariatric surgery, highlighting the need for continued lifestyle management.
Lifestyle Modification Programs
The CDC strongly advocates for structured lifestyle change programs as an evidence-based approach to prevent or delay Type 2 diabetes in people with prediabetes. These programs focus on:
- Achieving and maintaining at least 5-7% weight loss
- Getting at least 150 minutes of physical activity weekly
- Learning behavioral strategies for long-term change
- Receiving ongoing support and accountability
For those already diagnosed with diabetes, similar lifestyle interventions can potentially achieve remission, though more intensive approaches may be needed.
Medications That Support Weight Loss
The NIH notes that the approval of semaglutide (a GLP-1 medication) for obesity treatment has generated significant excitement. According to available sources, weight loss can prevent, delay, or reverse Type 2 diabetes, and medications that facilitate weight loss may help achieve these outcomes.
These medications work by mimicking gut hormones that regulate appetite and blood sugar. They’re not magic bullets, but when combined with lifestyle changes, they can help patients achieve the weight loss necessary for remission.
| Intervention Type | Weight Loss Potential | Remission Likelihood | Long-term Sustainability |
|---|---|---|---|
| Low-calorie diet programs | Moderate to significant | Possible with substantial loss | Requires ongoing commitment |
| Bariatric surgery | Significant | Higher rates initially | Relapse possible; needs lifestyle maintenance |
| Lifestyle modification | Modest to moderate | Possible with 5-7%+ weight loss | Most sustainable with support |
| Weight loss medications | Moderate | Supports other interventions | May require continued use |
Practical Steps to Reverse Type 2 Diabetes
Start With Achievable Weight Loss Goals
According to CDC guidance, if someone is overweight and has prediabetes, shedding just 5% of body weight can help reverse prediabetes. Setting this as an initial target makes the goal feel less overwhelming.
Clinical trials have shown that losing 5-7% of body weight can help prevent or delay Type 2 diabetes. For a 200-pound person, that’s 10-14 pounds — challenging but achievable.
Increase Physical Activity
Movement matters tremendously for blood sugar control. The CDC recommends getting at least 30 minutes of activity five days per week. Walking, dancing, and biking all count.
Research suggests even brief activity helps. Walking for just 10-15 minutes after meals can help muscles use up glucose and prevent blood sugar spikes. For those who spend considerable time sitting, standing up or moving around at least once an hour makes a difference.
Focus on Nutrition Quality
While calorie restriction drives weight loss, the quality of those calories matters for sustained blood sugar control. Generally speaking, diets that minimize processed carbohydrates and emphasize whole foods, vegetables, lean proteins, and healthy fats tend to support better glucose regulation.
Small changes can make measurable impacts without requiring a complete dietary overhaul initially.
Address Sleep and Stress
Poor sleep can exacerbate metabolic dysfunction and make blood sugar control more difficult. Similarly, chronic stress elevates cortisol, which can increase blood sugar levels and promote abdominal fat storage.
Many experts suggest that addressing these factors as part of a comprehensive approach improves outcomes.
Work With Healthcare Providers
According to NIH guidance from Dr. William T. Cefalu, healthcare professionals should discuss glycemic control goals with patients. In most cases, this means advising patients to keep their A1C level at 7% or below to prevent eye, kidney, and nerve complications.
But for those pursuing remission, the conversation shifts to more intensive interventions under medical supervision.
Who Can Achieve Diabetes Remission?
Not everyone with Type 2 diabetes will achieve remission, and several factors influence the likelihood of success.
Those diagnosed more recently tend to have better outcomes. When diabetes has been present for many years, the pancreas may have sustained more permanent damage, making remission more difficult though not impossible.
The degree of weight loss achieved strongly predicts remission rates. Greater weight loss typically produces higher remission rates.
Individual metabolic factors also play a role. Some people’s bodies respond more readily to interventions than others, and genetic factors influence insulin resistance and diabetes risk.
But even when complete remission isn’t achieved, significant weight loss and lifestyle changes still provide substantial benefits: better blood sugar control, reduced medication needs, lower risk of complications, and improved overall health.
The Challenge of Maintaining Remission
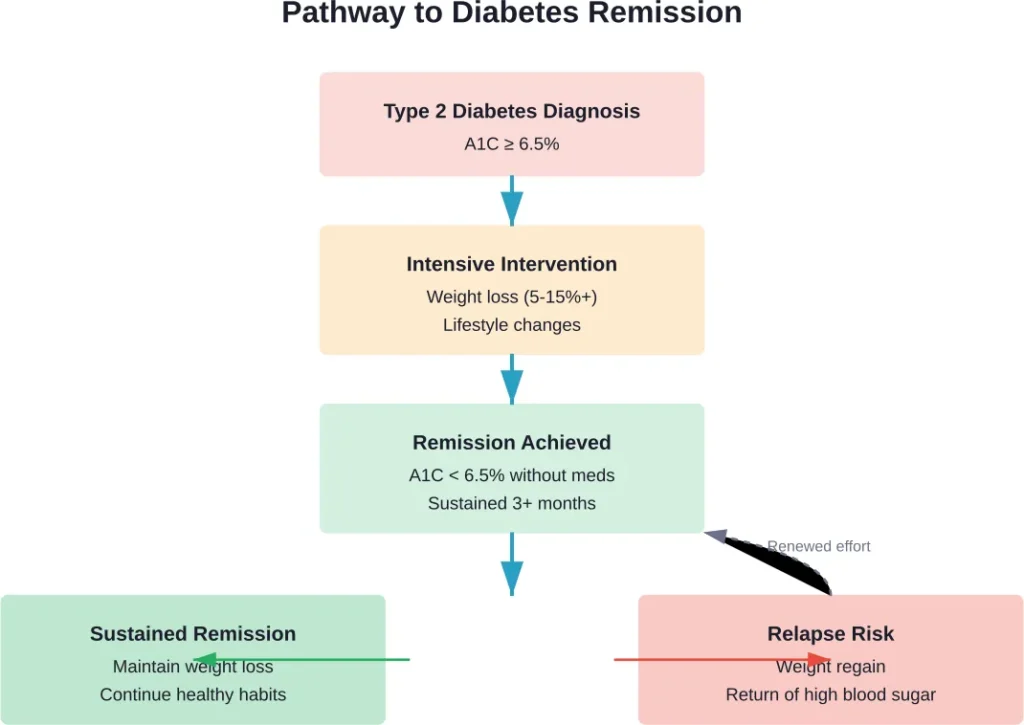
Here’s the hard truth: achieving remission is only half the battle. Maintaining it long-term requires sustained lifestyle changes.
Research shows that relapse from diabetes remission can occur within five years, particularly among those who regain weight. The body doesn’t forget its diabetic state, and the underlying susceptibility remains.
This doesn’t mean remission isn’t worthwhile. Even temporary periods of remission reduce exposure to high blood sugar levels and the associated complications. And many people do maintain remission long-term by continuing the lifestyle practices that got them there.
The key is viewing diabetes management as an ongoing commitment rather than a problem with a one-time solution.
What About Prediabetes?
According to the CDC, more than 2 in 5 American adults have prediabetes, according to the CDC — a condition where blood sugar levels are elevated but not yet high enough for a diabetes diagnosis. According to CDC data, 13.0% of adults in South Carolina have diabetes while 34.9% have prediabetes.
The encouraging news? With early action, prediabetes can be reversed to prevent or delay Type 2 diabetes. The same interventions that work for diabetes remission work even better for prediabetes reversal because the metabolic dysfunction is less advanced.
Losing 5-7% of body weight and increasing physical activity can cut the risk of progressing from prediabetes to Type 2 diabetes in half.
Frequently Asked Questions
No, Type 1 diabetes cannot be reversed. It’s an autoimmune condition where the body permanently destroys insulin-producing cells in the pancreas. People with Type 1 diabetes require lifelong insulin therapy. The remission discussed in research and medical literature applies only to Type 2 diabetes.
The timeline varies considerably based on the intervention used and individual factors. Some people see blood sugar improvements within days of starting intensive calorie restriction, though official remission requires maintaining an A1C below 6.5% without medication for at least three months. Achieving the necessary weight loss may take several months to over a year.
Based on available research, bariatric surgery tends to produce the fastest and most dramatic results, with significant metabolic improvements occurring within days to weeks. However, it’s also the most invasive option. Very low-calorie diet programs under medical supervision can also produce rapid results within weeks to months, though they require strict adherence and professional monitoring.
Yes. Research shows that relapse from diabetes remission can occur, particularly within five years. The risk is highest among those who regain weight or return to previous lifestyle patterns. Remission doesn’t mean diabetes is cured; it means the condition is in abeyance. Continued lifestyle management is essential for maintaining remission long-term.
Clinical evidence suggests that losing 5-7% of body weight can help prevent or delay Type 2 diabetes in people with prediabetes. For those already diagnosed with diabetes, this amount of weight loss improves blood sugar control, though achieving remission often requires more substantial weight loss — typically 10-15% or more, depending on individual factors.
For many people with Type 2 diabetes, lifestyle interventions alone — specifically weight loss through diet and exercise — can potentially achieve remission without pharmaceutical intervention. However, some individuals may need medication initially to bring blood sugar under control while implementing lifestyle changes. Working with healthcare providers to develop an appropriate plan is essential.
Diabetes remission is defined as achieving an A1C below 6.5% (the diagnostic threshold for diabetes) while being off all diabetes medications for at least three months. This represents a return to normal blood sugar regulation without pharmaceutical support.
The Bottom Line on Reversing Diabetes
So, is it possible to reverse diabetes? For Type 2 diabetes, the answer is yes — remission is achievable for many people through significant weight loss and sustained lifestyle changes.
The evidence is clear: structured interventions including low-calorie diets, bariatric surgery, and intensive lifestyle modification programs can restore normal blood sugar levels without medication. The CDC and NIH both recognize that weight loss of 5-7% or more can prevent, delay, or reverse Type 2 diabetes.
But remission requires commitment. It’s not a quick fix or a temporary diet. Those who achieve and maintain remission typically make permanent changes to how they eat, move, and manage their health.
For the millions of Americans living with Type 2 diabetes or prediabetes, this represents genuine hope. Diabetes doesn’t have to be a life sentence. With the right approach and sustained effort, normal blood sugar levels are within reach.
If you have diabetes or prediabetes, talk with your healthcare provider about whether pursuing remission makes sense for your situation. Get screened if you’re at risk. And if you’re diagnosed with prediabetes, act now — it’s your best opportunity to prevent Type 2 diabetes entirely.
The science supporting diabetes reversal continues to grow stronger. The question isn’t whether remission is possible, but whether individuals are willing to make the substantial lifestyle changes required to achieve and maintain it.
