Quick Summary: True alcohol allergies are extremely rare, affecting a small fraction of the population. Most adverse reactions to alcohol are actually alcohol intolerance, a genetic condition that prevents proper breakdown of alcohol. According to NIH research, approximately 10% of the general population experiences hypersensitivity reactions to alcoholic beverages, particularly wine, with symptoms including flushing, nasal congestion, and respiratory issues.
That uncomfortable reaction after a glass of wine might feel like an allergy. The flushed face, the stuffy nose, maybe some hives. But here’s the thing—you’re probably not actually allergic to alcohol itself.
Real alcohol allergies are incredibly rare. What most people experience is something different entirely.
According to research published by the National Institutes of Health, hypersensitivity reactions to alcoholic beverages affect approximately 10% of the general population. But the vast majority of these aren’t true allergies in the immunological sense.
The Truth About Alcohol Allergies vs. Intolerance
Let’s clear this up right away. True allergic reactions to ethanol (the alcohol molecule itself) are exceptionally uncommon.
A genuine alcohol allergy means the immune system creates antibodies against alcohol molecules. The NIH has documented case reports of life-threatening ethanol-induced anaphylaxis, but these cases are so rare they warrant individual medical case studies. In documented cases, positive skin test responses to acetic acid (a breakdown product of ethanol) were found, and reactions were confirmed through double-blind placebo-controlled challenges accompanied by rises in serum tryptase levels.
What’s far more common? Alcohol intolerance.
This condition stems from a genetic inability to break down alcohol efficiently. According to the National Institute on Alcohol Abuse and Alcoholism (NIAAA), alcohol intolerance is caused by a genetic polymorphism of aldehyde dehydrogenase (ALDH2), particularly prevalent in people of East Asian descent.
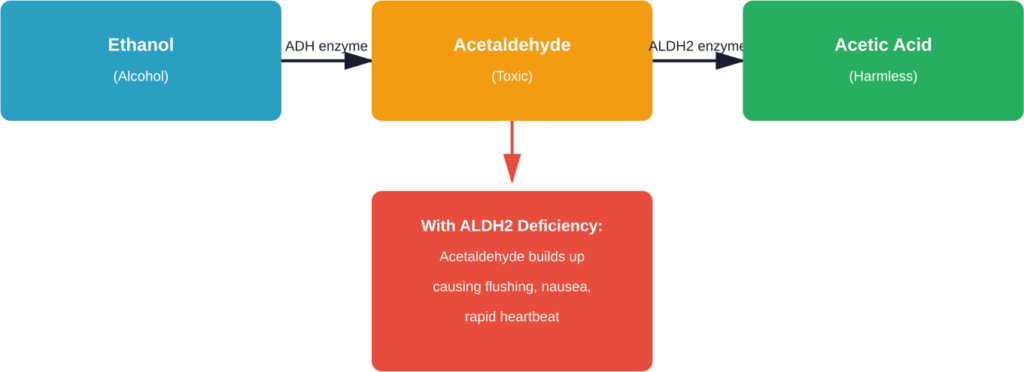
Here’s what happens: When the body metabolizes alcohol, it first converts ethanol into acetaldehyde. Then another enzyme (ALDH2) should convert that acetaldehyde into harmless acetic acid. But when someone has the genetic variant, acetaldehyde accumulates, triggering uncomfortable symptoms.
Recognizing the Symptoms
The symptoms of alcohol intolerance typically show up quickly—sometimes after just a few sips.
The most common sign? Facial flushing. The NIAAA identifies this alcohol flush reaction as the primary feature, often called “Asian flush” or “Asian glow” because of its prevalence in East Asian populations.
But that’s not all. Other symptoms include:
- Nasal congestion or stuffy nose
- Skin flushing beyond the face
- Nausea and vomiting
- Rapid heartbeat
- Low blood pressure
- Headaches or migraines
- Worsening of asthma symptoms
Research from the NIH shows that airway reactions, particularly rhinitis and asthma, are among the most frequent hypersensitivity responses to alcoholic drinks. These occur significantly more often in people with pre-existing allergic conditions.
True allergic reactions, when they do occur, look different. They can include severe symptoms like difficulty breathing, rapid pulse, dizziness, and in extreme cases, anaphylaxis. These symptoms could be triggered by as little as one sip and result from the body creating antibodies against specific allergens.
What About Ingredients in Alcoholic Drinks?
Here’s where things get more complicated. Many people aren’t reacting to alcohol at all—they’re reacting to other ingredients in alcoholic beverages.
Wine, beer, and spirits contain numerous potential allergens:
| Ingredient | Found In | Reaction Type |
|---|---|---|
| Histamines | Red wine, fermented drinks | Flushing, headaches, congestion |
| Sulfites | Wine, beer (preservative) | Asthma, allergic reactions |
| Grains (wheat, barley) | Beer, whiskey, vodka | True allergic reactions |
| Grapes | Wine, brandy | Allergic reactions |
| Hops | Beer | Allergic reactions |
| Yeast | Beer, wine | Allergic reactions |
According to NIH research, red wine triggers hypersensitivity reactions more frequently than other alcoholic beverages. One study found that 7.2% of individuals self-reported wine intolerance, with women affected more than men (8.9% verse 5.2%).
The American Academy of Allergy, Asthma & Immunology notes that reactions can occur to various drinks including beer, wine, liquor, and malt-based drinks. The specific trigger often depends on individual sensitivities to ingredients beyond the ethanol itself.
The Serious Health Implications
The NIAAA emphasizes something crucial: alcohol flush reaction isn’t just uncomfortable—it’s linked to higher risk of certain cancers.
When acetaldehyde accumulates due to ALDH2 deficiency, this toxic compound can damage DNA and cause cancer. People with this genetic variant who continue drinking alcohol face elevated risks for cancers of the esophagus, head, and neck.
That flushing isn’t just an embarrassing side effect. It’s a warning sign.
Can Alcohol Intolerance Develop Suddenly?
Yes, and it’s more common than people realize.
While genetic alcohol intolerance is present from birth, symptoms can develop or worsen at any point in life. Several factors can trigger sudden onset alcohol intolerance:
Medical conditions: Hodgkin’s lymphoma, other lymphomas, and certain autoimmune conditions can cause new alcohol sensitivity.
Medications: According to NIAAA research, dozens of common medications can interact with alcohol. Approximately 40% of adults took a medication in the past year that could interact dangerously with alcohol.
Post-viral syndromes: Recent NIH case studies documented new alcohol sensitivity in patients with post-acute sequelae of SARS-CoV-2 (long COVID). In studies of myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS), a condition that can be triggered by viral infections, 65-80% of patients experienced increased alcohol sensitivities.
Age-related changes: Aging affects how the body processes alcohol, sometimes leading to increased sensitivity.

Getting Proper Diagnosis
Think you might have alcohol intolerance or allergy? Don’t self-diagnose.
Medical evaluation typically involves several steps. A healthcare provider will take a detailed history of symptoms, timing, and which beverages trigger reactions. They’ll ask about family history, since ALDH2 deficiency is genetic.
For suspected allergies to ingredients in alcoholic beverages, allergists can perform skin prick tests or blood tests for specific allergens like grains, grapes, or sulfites.
According to the American Academy of Allergy, Asthma & Immunology, positive skin test responses can identify sensitivities. In documented cases of ethanol-induced anaphylaxis, skin testing to acetic acid (a breakdown product of ethanol) showed positive responses in patients but not in healthy controls.
But here’s something important: Humans naturally produce ethanol, up to 0.5-0.8 gm per day, so specific IgE antibodies against ethanol itself are unlikely to develop.
Managing Reactions and Staying Safe
The most effective treatment for alcohol intolerance? Avoiding alcohol.
There’s no cure for the genetic enzyme deficiency. Antihistamines might reduce some symptoms like nasal congestion or flushing, but they don’t address the underlying problem or reduce cancer risk.
Never try to “push through” symptoms or mask them with medication so you can keep drinking. The accumulated acetaldehyde damages your cells regardless of whether you feel the symptoms.
For ingredient-specific reactions, you might tolerate some alcoholic beverages but not others. Someone allergic to grapes might react to wine but handle grain-based spirits. Someone with sulfite sensitivity might do better with sulfite-free wines.
But if reactions are severe or involve breathing difficulties, complete avoidance is essential. Anyone with a history of anaphylaxis to any component of alcoholic beverages should carry an epinephrine auto-injector.
The Social Pressure Challenge
Real talk: Not drinking in social situations can feel awkward.
But risking serious health consequences isn’t worth fitting in. According to CDC data, about 178,000 people die from excessive alcohol use each year in the United States. For people with alcohol intolerance, the risks multiply.
Keep explanations simple if needed: “I have a medical condition that makes me react badly to alcohol.” Most reasonable people accept this immediately.
The American Academy of Allergy, Asthma & Immunology highlights additional concerns for young people with food allergies who begin encountering alcohol in social settings. Alcohol impairs judgment, potentially leading to risky choices about food consumption and reduced vigilance about carrying epinephrine.
Frequently Asked Questions
While genetic alcohol intolerance is present from birth, symptoms can develop or worsen suddenly due to medications, medical conditions like lymphoma, post-viral syndromes including long COVID, or age-related changes in how the body processes alcohol. True allergies to alcohol are extremely rare but reactions to ingredients in alcoholic beverages can develop at any time.
Alcohol intolerance is a genetic enzyme deficiency (particularly ALDH2) affecting approximately 10% of the population, causing uncomfortable but not life-threatening symptoms like flushing and congestion. True alcohol allergy involves immune system antibodies and is exceptionally rare, with only isolated case reports documented in medical literature. True allergies can cause severe reactions including anaphylaxis.
Facial flushing or “alcohol flush reaction” occurs when acetaldehyde accumulates due to ALDH2 enzyme deficiency. This genetic variant, particularly common in East Asian populations, prevents proper breakdown of alcohol’s toxic metabolite. According to the NIAAA, this isn’t just cosmetic—it indicates elevated cancer risk with continued alcohol consumption.
Antihistamines might reduce symptoms like nasal congestion or skin flushing temporarily, but they don’t address the underlying problem. For genetic alcohol intolerance, antihistamines don’t prevent acetaldehyde accumulation or reduce cancer risk. They also don’t protect against true allergic reactions. The only effective management is avoiding alcohol.
Red wine contains higher levels of histamines, sulfites, and other compounds that trigger reactions. NIH research shows red wine causes hypersensitivity reactions more frequently than other alcoholic beverages, with approximately 7.2% of people reporting wine intolerance. Reactions might involve ingredients like grapes, sulfite preservatives, or histamines from fermentation rather than the alcohol itself.
Yes, particularly the long-term cancer risk. The NIAAA emphasizes that alcohol flush reaction is linked to higher risk of esophageal, head, and neck cancers because accumulated acetaldehyde damages DNA. Even without severe immediate symptoms, continuing to drink alcohol with ALDH2 deficiency significantly increases cancer risk over time.
Seek medical evaluation if you experience breathing difficulties, severe skin reactions, rapid pulse, dizziness, or any signs of anaphylaxis after drinking alcohol. Also consult a healthcare provider if reactions are worsening, interfering with quality of life, or if you’re unsure whether symptoms indicate intolerance versus allergy to specific ingredients.
The Bottom Line
So, is it possible to be allergic to alcohol? Technically yes, but extremely unlikely.
What’s far more probable: alcohol intolerance affecting roughly 10% of people, or sensitivity to other ingredients in alcoholic beverages. Both conditions deserve attention, proper diagnosis, and appropriate management.
Those uncomfortable symptoms after drinking aren’t something to ignore or push through. They’re signals from your body that something’s wrong. And when it comes to the cancer risks associated with alcohol flush reaction, those signals could be lifesaving.
If you’re experiencing consistent adverse reactions to alcohol, talk to a healthcare provider. Getting proper diagnosis helps you understand what’s happening, assess your risks, and make informed decisions about alcohol consumption.
Your health matters more than any social situation. Listen to what your body is telling you.
