Quick Summary: Yes, it’s possible to have two periods in one month, especially if your menstrual cycle is naturally shorter than 28 days. According to the ACOG, normal menstrual cycles range from 21 to 35 days, so someone with a 21-day cycle could legitimately experience two periods within one calendar month. However, frequent occurrences may signal underlying conditions like hormonal imbalances, uterine fibroids, or thyroid disorders that warrant medical evaluation.
Getting two periods in one month can feel alarming, especially if it’s never happened before. But here’s the thing—this occurrence isn’t automatically a cause for concern.
The reality is more nuanced than most people realize. Sometimes it’s just calendar math working against you. Other times, it signals something that needs medical attention.
Understanding the difference matters. A lot.
Understanding Normal Menstrual Cycle Variations
The typical menstrual cycle lasts 28 days, but that’s just an average. According to the ACOG, normal cycles range from 21 to 35 days for adults, and can extend even longer for adolescents—up to 38 days or more.
Here’s where calendar confusion happens: if someone has a 24-day cycle and their period starts on the 1st of the month, the next period arrives around the 25th. That’s two periods in one calendar month, but it’s entirely normal menstrual function.
The CDC notes that normal menstrual periods last up to 7 days. When combined with a shorter cycle length, this creates a pattern that can seem irregular but falls within healthy parameters.

When Two Periods Indicates Normal Physiology
Research published in medical journals indicates that 2 years after menarche, up to 85% of the cycles are still anovulatory. This means adolescents naturally experience irregular cycles as their reproductive system matures.
For teens and young adults, cycle length variations are physiological, not pathological. The hypothalamic-pituitary-ovarian axis takes time to stabilize.
Another normal scenario: perimenopause. During this transitional phase, hormonal fluctuations cause unpredictable bleeding patterns. During perimenopause, cycle irregularities are common and require medical evaluation.
Medical Conditions That Cause Frequent Periods
When two periods per month becomes a regular pattern rather than an occasional occurrence, underlying conditions deserve investigation.
Uterine Fibroids
These non-cancerous growths in the uterus frequently disrupt normal menstrual patterns. Fibroids can cause heavy bleeding, prolonged periods, and shortened cycles—all of which contribute to experiencing periods more frequently than expected.
The bleeding occurs because fibroids increase the surface area of the uterine lining and can interfere with normal uterine contractions that control blood flow.
Thyroid Dysfunction
Both hyperthyroidism and hypothyroidism affect menstrual regularity. The thyroid hormones directly influence reproductive hormones, and when thyroid function is disrupted, menstrual patterns follow suit.
Medical literature confirms that menstrual disturbances are fundamental problems in endocrine disorders, with prevalence of irregular cycles ranging from 14.2% to 27% globally.
Polycystic Ovary Syndrome
According to research from the Apple Women’s Health Study conducted by Harvard T.H. Chan School of Public Health, PCOS creates complex relationships between cycle irregularity and other health outcomes. The condition causes hormonal imbalances that can paradoxically result in both skipped periods and unexpectedly frequent bleeding episodes.
Bleeding Disorders
The CDC reports that up to 1.6 million (or about 1 in every 100) women and girls in the United States have a bleeding disorder, with many remaining unaware of their condition. Von Willebrand disease is the most common bleeding disorder, found in up to 1% of the U.S. population, and can manifest as heavy menstrual bleeding and irregular cycle timing.
According to the CDC, periods requiring a new tampon or pad after less than 2 hours, passing large clots, or soaking through one or more pads/tampons every hour are considered heavy and may indicate an underlying bleeding disorder.
| Condition | How It Affects Cycles | Other Symptoms |
|---|---|---|
| Uterine Fibroids | Heavy flow, shortened cycles | Pelvic pressure, frequent urination |
| Thyroid Disorders | Irregular timing, flow changes | Weight changes, fatigue, temperature sensitivity |
| PCOS | Unpredictable bleeding patterns | Acne, excess hair growth, weight gain |
| Bleeding Disorders | Heavy flow, prolonged bleeding | Easy bruising, frequent nosebleeds |
| Endometriosis | Heavy periods, spotting between | Severe cramping, pain during intercourse |
Hormonal and Lifestyle Factors
External factors significantly influence menstrual regularity. Stress, in particular, affects the hypothalamic-pituitary-adrenal axis, which directly communicates with the reproductive system.
Research found that during periods of high stress, menstrual periods began four days late on average. Some women (13%) experienced delays of eight or more days—creating situations where the following month might include two periods as cycles reset.
Birth control changes also trigger temporary irregularities. Starting, stopping, or switching contraceptive methods disrupts the body’s hormonal equilibrium, sometimes resulting in breakthrough bleeding or shortened cycles until hormones stabilize.
Significant weight fluctuations, intense exercise regimens, and certain medications all contribute to menstrual pattern changes.
What Heavy Bleeding Really Means
The CDC provides specific criteria for heavy menstrual bleeding: periods lasting more than 7 days, requiring pad or tampon changes more frequently than every 2 hours, or involving large blood clots.
Heavy menstrual bleeding is very common, with about one third of women seeking treatment for it, making it a concern that warrants medical evaluation. It’s not just uncomfortable—it can lead to anemia and significantly impact quality of life.
According to the ACOG, determining the etiology of abnormal uterine bleeding requires comprehensive assessment including medical history, physical examination, and appropriate laboratory and imaging tests.
Diagnostic Approaches and Treatment Options
Healthcare providers use multiple diagnostic tools to identify the cause of frequent periods. Blood tests assess hormone levels, thyroid function, and potential bleeding disorders. Pelvic ultrasounds visualize structural abnormalities like fibroids or polyps.
In some cases, endometrial biopsy or hysteroscopy provides direct visualization of the uterine lining to rule out more serious conditions.
Treatment varies dramatically based on the underlying cause. Hormonal contraceptives often regulate cycles and reduce heavy bleeding. For fibroids, options range from medication to minimally invasive procedures to surgical removal.
Thyroid disorders require specific hormone replacement or suppression therapy. Bleeding disorders may necessitate specialized clotting factor treatments.
The ACOG emphasizes that determining the specific etiology is essential for choosing the most appropriate and effective management strategy.
Tracking Your Menstrual Health
Detailed tracking provides invaluable information for healthcare providers. Recording cycle start dates, duration, flow heaviness, and associated symptoms creates a clear pattern that aids diagnosis.
According to CDC guidance on menstrual hygiene, understanding personal menstrual patterns helps identify deviations from normal that warrant attention.
Modern tracking apps simplify this process, but a simple calendar notation works equally well. The key is consistency—tracking for at least three months provides enough data to identify genuine patterns versus random variations.
Frequently Asked Questions
Yes, occasional instances are typically normal, especially with naturally shorter cycles (21-24 days). If your cycle is consistently 21-24 days, experiencing two periods in one calendar month is expected and healthy. However, if this becomes a frequent pattern and your cycles are normally longer, medical evaluation is recommended.
Stress can delay ovulation and disrupt your normal cycle timing. Research shows stress-related delays averaging four days, with some women experiencing delays over eight days. This disruption can result in two periods occurring within the same calendar month as your cycle attempts to reset to its normal pattern.
Uterine fibroids typically cause heavy menstrual bleeding, prolonged periods, pelvic pressure, and frequent urination. However, these symptoms overlap with other conditions. Definitive diagnosis requires pelvic ultrasound or other imaging studies performed by a healthcare provider to visualize the fibroids.
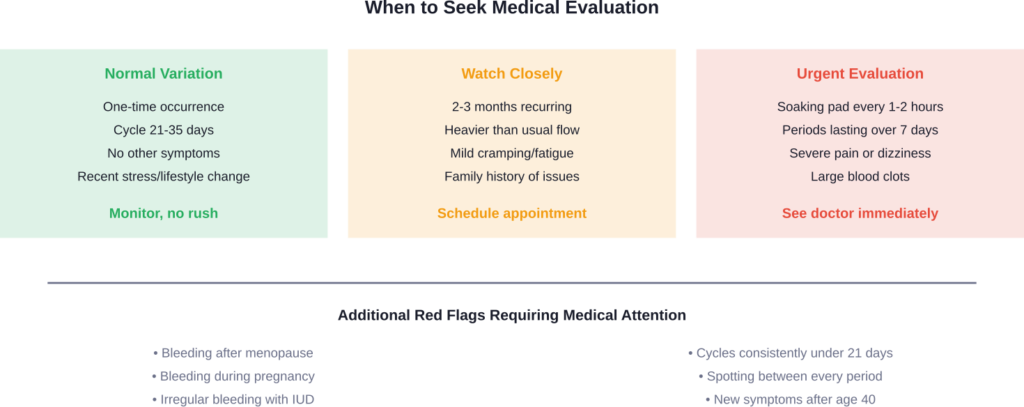
Consult a healthcare provider if this pattern continues for three or more months, if you’re soaking through pads or tampons every 1-2 hours, if periods last longer than 7 days, or if you’re experiencing severe pain, dizziness, or large blood clots. According to the CDC, these symptoms may indicate conditions requiring medical treatment.
Yes, starting new hormonal contraception, switching methods, or missing pills can cause breakthrough bleeding or temporary cycle disruption. This typically resolves within 2-3 months as your body adjusts to the new hormone levels. If irregular bleeding persists beyond three months, consult your healthcare provider about alternative options.
During perimenopause, the transitional phase before menopause, cycle irregularities are common. During this phase, hormonal fluctuations can manifest as closer-together periods, skipped periods, or unpredictable bleeding. If you’re over 40 and experiencing new menstrual irregularities, discuss perimenopause evaluation with your provider.
Not necessarily. While more frequent ovulation theoretically creates more opportunities for conception, the underlying causes of frequent periods often indicate hormonal imbalances or anovulatory cycles that can actually reduce fertility. If you’re concerned about fertility and experiencing irregular cycles, consult a reproductive endocrinologist for proper assessment.
Taking Control of Your Menstrual Health
Experiencing two periods in one month isn’t automatically cause for alarm. But it’s also not something to dismiss without consideration.
The distinction between normal variation and medical concern depends on pattern, frequency, and accompanying symptoms. A single occurrence in someone with a naturally shorter cycle requires no action. A recurring pattern with heavy bleeding and fatigue demands medical attention.
According to authoritative medical organizations including the CDC and ACOG, menstrual health serves as a vital sign of overall health. Changes in menstrual patterns provide important clues about hormonal balance, reproductive health, and potential systemic conditions.
Don’t hesitate to seek medical evaluation when something feels wrong. Healthcare providers have multiple diagnostic tools and treatment options available. Early intervention often prevents complications and significantly improves quality of life.
Track your cycles diligently, note any changes or concerning symptoms, and advocate for your health. Whether it’s a simple explanation or something requiring treatment, getting answers provides peace of mind and appropriate care.
Your menstrual health matters. Take it seriously, and don’t settle for dismissive responses if your concerns persist.
