Quick Summary: Yes, it is possible to have two vaginas. This rare congenital condition, known as uterus didelphys or uterine duplication, occurs when a female develops two separate reproductive structures instead of one during fetal development. According to Cleveland Clinic, uterus didelphys affects about 0.3% of the population and can include two vaginas, two cervixes, and two uteruses.
When British television featured Hazel Jones, a 27-year-old woman born with two vaginas, two cervixes, and two uteruses, the internet erupted with responses. Commenters shared their own experiences with similar conditions, revealing just how many people live with this rare but not unheard-of anatomical variation.
But what exactly causes someone to develop two vaginas? And how does this condition affect daily life, pregnancy, and overall health?
What Is Uterus Didelphys?
Uterus didelphys, commonly called a double uterus, is a congenital condition present at birth. During typical fetal development, two small tubes called Müllerian ducts fuse together to form a single hollow organ—the uterus. Sometimes these tubes don’t join completely.
Instead, each develops into a separate structure. The result? Two uteruses instead of one pear-shaped organ.
According to Cleveland Clinic, uterus didelphys affects roughly 0.3% of the population. Some people with this condition also have two cervixes and two vaginal canals. Instead of having a pear-shaped uterus, if you have uterus didelphys, your uteruses resemble bananas.
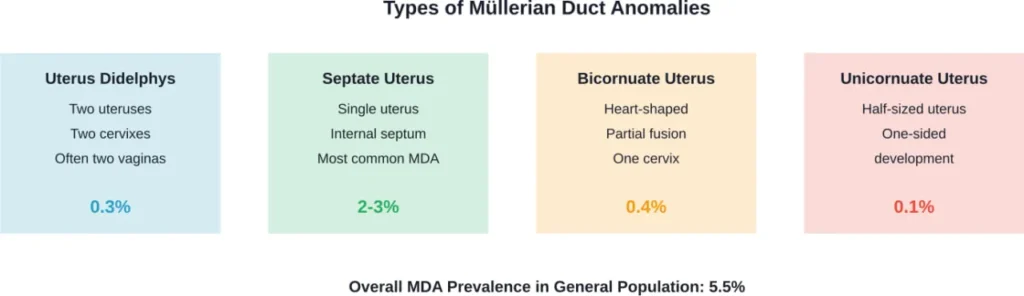
The Spectrum of Müllerian Duct Anomalies
Uterus didelphys belongs to a broader category of Müllerian duct anomalies (MDAs). Research published in medical journals indicates that uterine anomalies affect an estimated 5.5% of the general female population, with prevalence increasing to 24.5% in populations experiencing miscarriage and infertility.
These anomalies include septate uterus, bicornuate uterus, unicornuate uterus, and complete duplication. The classification systems used by the American Society for Reproductive Medicine and the European Society of Human Reproduction and Embryology help doctors categorize these variations.
Symptoms and Signs
Here’s the thing though—many people with uterus didelphys don’t even know they have it. The condition often goes undiagnosed until a routine pelvic exam, pregnancy, or investigation for other issues.
When symptoms do occur, they might include:
- Painful periods (dysmenorrhea)
- Painful intercourse (dyspareunia)
- Abnormal bleeding or spotting
- Recurrent pregnancy loss
- Premature delivery
A double uterus may be diagnosed during a routine pelvic exam when a doctor observes a double cervix or feels an unusually shaped uterus. But many women go through their entire reproductive years without knowing about their anatomical variation.
How Is It Diagnosed?
Diagnosis typically involves imaging tests that provide detailed views of the reproductive structures. The most common diagnostic methods include:
Ultrasound: High-frequency sound waves create images of internal structures. A transvaginal ultrasound, where the transducer is inserted into the vagina, provides the clearest views.
MRI: Magnetic resonance imaging offers detailed cross-sectional images and is considered the gold standard for classifying Müllerian duct anomalies.
3D Imaging: Advanced imaging techniques help doctors distinguish between different types of uterine anomalies, which is crucial for treatment planning.
Research in radiology journals emphasizes that accurate classification matters. Different anomalies require different management approaches, and misclassification can lead to inappropriate treatment.
Pregnancy and Uterus Didelphys
Can women with two uteruses get pregnant? Absolutely. In fact, medical literature documents cases of women carrying pregnancies in both uteruses simultaneously.
One published case study described a woman with uterus didelphys who spontaneously conceived two singleton pregnancies, one in each uterus, and delivered healthy breech infants at term via caesarean section in both instances.
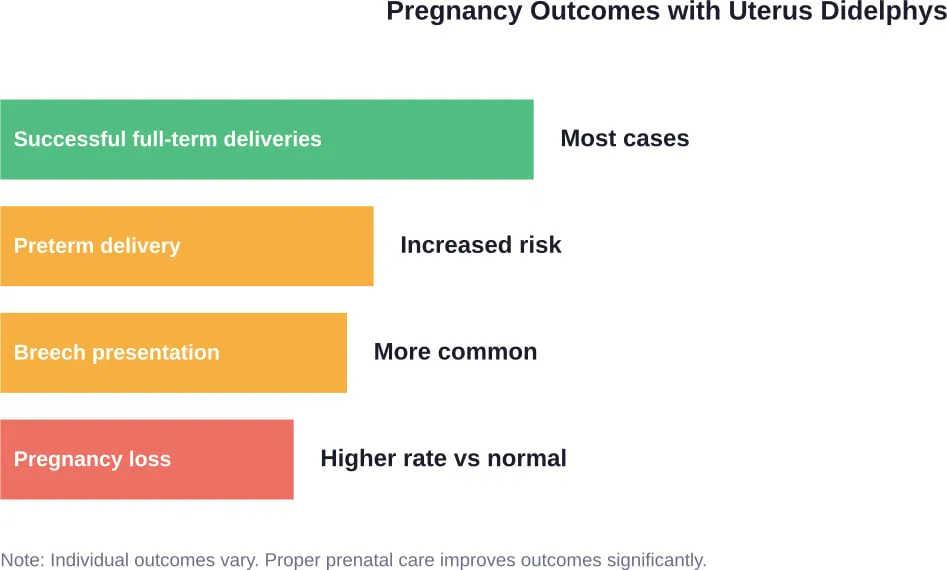
That said, uterus didelphys is associated with certain pregnancy complications. According to research on Müllerian duct anomalies, these can include:
- Fetal growth restriction
- Preterm delivery
- Breech presentation
- Higher rates of caesarean delivery
The good news? Many women with uterus didelphys carry pregnancies to term and deliver healthy babies. Medical monitoring and appropriate prenatal care make a significant difference.
Treatment Options
Does everyone with uterus didelphys need treatment? Not necessarily.
If the condition isn’t causing symptoms or pregnancy complications, many doctors recommend a watch-and-wait approach. Regular monitoring ensures any issues get caught early.
When treatment becomes necessary, options include:
Surgical correction: In cases where a vaginal septum causes discomfort or interferes with intercourse, minimally invasive surgery can remove the tissue dividing the two vaginal canals.
Laparoscopic procedures: Research shows that minimally invasive surgery has transformed the management of Müllerian duct anomalies, enabling effective correction with reduced morbidity in appropriately selected patients.
Fertility support: Women experiencing recurrent pregnancy loss or infertility may benefit from reproductive medicine interventions.
According to the American College of Obstetricians and Gynecologists, management decisions should be individualized based on symptoms, reproductive goals, and specific anatomical variations.
Related Conditions
Uterus didelphys sometimes occurs alongside other congenital anomalies. Herlyn-Werner-Wunderlich syndrome, for instance, typically involves uterus didelphys with an obstructed hemivagina and renal anomalies.
Medical research documents cases with contralateral duplex kidneys and duplication of ureters occurring with uterine duplication. This highlights why comprehensive evaluation matters when Müllerian duct anomalies are diagnosed.
Living with Two Vaginas
Community discussions reveal that many people with this condition lead completely normal lives. Some discover their anatomical variation only during pregnancy or routine gynecological care.
Challenges can include:
- Difficulty obtaining cervical screening (Pap smears require checking both cervixes)
- Finding healthcare providers familiar with the condition
- Navigating questions about sexual health and function
But most people adapt well once they understand their anatomy and find knowledgeable healthcare providers.
Frequently Asked Questions
Yes, though it’s extremely rare. Medical literature documents cases of women carrying simultaneous pregnancies in both uteruses. Each uterus can function independently, ovulate, and support pregnancy.
For most people, no. If a vaginal septum causes discomfort during intercourse, surgical removal is a straightforward outpatient procedure. Many individuals report normal sexual function.
According to Cleveland Clinic, uterus didelphys affects approximately 0.3% of the population, making it quite rare. However, the actual prevalence may be higher since many cases go undiagnosed.
Not necessarily. While breech presentation is more common with uterus didelphys, many women deliver vaginally. The delivery method depends on fetal position, medical history, and individual circumstances.
Uterus didelphys is linked to higher rates of infertility compared to typical anatomy, but many women with this condition conceive naturally and carry pregnancies successfully. Fertility varies by individual.
Research suggests some Müllerian duct anomalies may have genetic factors, though most cases occur sporadically. Family history doesn’t typically predict these conditions.
Regular gynecological care is important, particularly ensuring both cervixes receive screening during Pap smears. Finding a provider familiar with Müllerian duct anomalies improves care quality.
Moving Forward
Having two vaginas, two cervixes, or two uteruses might sound unusual, but for the thousands of people born with uterus didelphys, it’s simply their anatomy. Medical advances in imaging and minimally invasive surgery mean better diagnosis and treatment options than ever before.
If you’ve been diagnosed with uterus didelphys or suspect you might have a Müllerian duct anomaly, seek care from a healthcare provider experienced with these conditions. Organizations like the American College of Obstetricians and Gynecologists and Cleveland Clinic offer specialized programs for managing reproductive tract anomalies.
Understanding your anatomy empowers you to make informed decisions about your reproductive health, pregnancy planning, and overall wellbeing. You’re not alone—and with proper care, most people with uterus didelphys live healthy, fulfilling lives.
