Quick Summary: Yes, crying blood is medically possible—a rare condition called hemolacria where tears contain blood. It can result from infections, injuries, tumors, or even hormonal changes, and while often benign, it requires medical evaluation to rule out serious underlying causes.
Bloody tears sound like something straight out of a horror film. But here’s the thing—people actually can cry blood, and it’s a documented medical phenomenon with multiple case reports spanning decades.
The medical term is hemolacria (or haemolacria), derived from the Greek words for blood and tears. While extremely rare, this condition has been observed in patients ranging from infants to adults, with causes that vary dramatically from benign to potentially serious.
So what exactly makes tears turn red? And should someone experiencing bloody tears rush to the emergency room or wait it out?
What Is Hemolacria?
Hemolacria is defined as the presence of blood in tears. According to the National Institutes of Health’s StatPearls database, hemolacria occurs when tears become partially or fully composed of blood.
The condition presents in different ways. Some people notice faint pink or red streaks in their tears. Others experience what looks like pure blood streaming from their eyes.
Medical literature reveals that hemolacria shows a notable female preponderance, with women more frequently affected than men. Case reports published in medical journals describe patients across all age groups—from a 4-month-old infant documented in a Saudi Journal of Ophthalmology report to elderly patients experiencing the condition alongside other health issues.
Most cases involve one eye, though bilateral (both eyes) presentations occur too. A case report published in the Journal of Family Medicine and Primary Care notes that unilateral right eye presentation appeared particularly common in their case series.
How Tears Normally Work
Understanding bloody tears requires knowing how normal tear production functions.
Tears come from the lacrimal gland located above the outer corner of each eye. These glands constantly produce tears that spread across the eye surface with each blink, then drain through small openings called puncta into the tear ducts.
The tear drainage system includes the lacrimal sac and nasolacrimal duct, which ultimately connects to the nasal cavity. That’s why crying often leads to a runny nose—tears drain directly into nasal passages.
Blood can enter this system at multiple points: the lacrimal gland itself, the conjunctiva (the membrane covering the white of the eye), the tear drainage passages, or even retrograde flow from nasal and sinus areas.
What Causes Bloody Tears?
Hemolacria isn’t a disease itself—it’s a symptom with numerous potential underlying causes. Medical research identifies several categories of causes ranging from completely harmless to life-threatening.
Infections and Inflammation
Bacterial conjunctivitis (pink eye) represents one of the more common causes. When blood vessels in the inflamed conjunctiva rupture, blood mixes with tear fluid.
Case reports in medical literature describe patients experiencing episodic bilateral bloody tears associated with epistaxis (nosebleed) that resolved without intervention. Similarly, a 4-month-old infant case published in the Saudi Journal of Ophthalmology showed bloody tears that resolved within three to four days after treatment with fusidic acid eye drops, with no recurrence during four months of follow-up.
Structural Lesions
According to research published in Optometry and Visual Science, occult conjunctival lesions like pyogenic granulomas can cause unilateral hemolacria. These small, benign vascular growths on the conjunctiva bleed easily.
The case report emphasized that thorough evaluation including eyelid eversion is critical—some lesions hide under the eyelid and get missed during routine examination.
Until recently, steroid treatment was the only topical option for conjunctival pyogenic granulomas. However, recent reports show success with topical timolol, offering an alternative treatment approach.
Tumors and Malignancy
Here’s where things get serious. Research published in the journal Eye reviewed patients presenting with blood in their tears over a 20-year period at a tertiary ophthalmic hospital.
The study found that blood-stained tears can indicate occult malignancy of the lacrimal drainage apparatus. Tumors in the tear drainage system, nasal passages, or paranasal sinuses can cause bleeding that appears as bloody tears.
This makes thorough medical evaluation absolutely essential—what seems benign might signal something requiring urgent treatment.
Trauma and Injury
Eye injuries can directly damage blood vessels, causing blood to mix with tears. Contact lens wearers occasionally develop small corneal or conjunctival injuries that bleed.
Facial trauma affecting the eye area, nasal fractures, or foreign bodies lodged in the conjunctiva can all produce bloody tears as a secondary symptom.
Valsalva-Related Bleeding
Research published in PubMed documents cases where hemolacria associates with Valsalva maneuvers—activities that increase pressure in the chest and head, like coughing, vomiting, or straining.
The sudden pressure spike can rupture tiny blood vessels in the conjunctiva or tear drainage system, causing transient bleeding.
Systemic Diseases
A PubMed case report describes hemolacria in a patient with severe systemic diseases. The bleeding resolved spontaneously within 24 hours after blood pressure normalized, though the patient later died from kidney failure.
Blood clotting disorders, severe hypertension, and other systemic conditions can manifest with bleeding from multiple sites including tears.
Hormonal Factors
A 1991 study of healthy subjects found that 18 percent of menstruating women had blood in their tears, compared to 8 percent of men and 7 percent of pregnant women.
None of the post-menopausal women showed blood in tears. This pattern suggests hormonal influences on tear composition, though the exact mechanism remains unclear.
The term “occult haemolacria” refers to blood present in tears that isn’t visible to the naked eye—detected only through laboratory testing.
Psychiatric Disorders
Case reports published in Clinical Case Reports document hemolacria secondary to major depressive disorder and generalized anxiety disorder in a 24-year-old man.
The researchers concluded that hemolacria can occur based on psychiatric disorder without an organic cause. However, this should remain a diagnosis of exclusion—ruling out physical causes first is mandatory. Treatment of the underlying psychiatric illness may relieve the condition.
Idiopathic Cases
Literature review reveals many case reports with undetermined source of hemolacria. Even after extensive evaluation including imaging, blood tests, and specialist examination, some cases have no identifiable cause.
According to the NIH’s StatPearls resource, close observation is needed when no apparent cause is detected to rule out malingering (intentionally produced symptoms), though genuine idiopathic cases do exist.
Diagnosis and Medical Evaluation
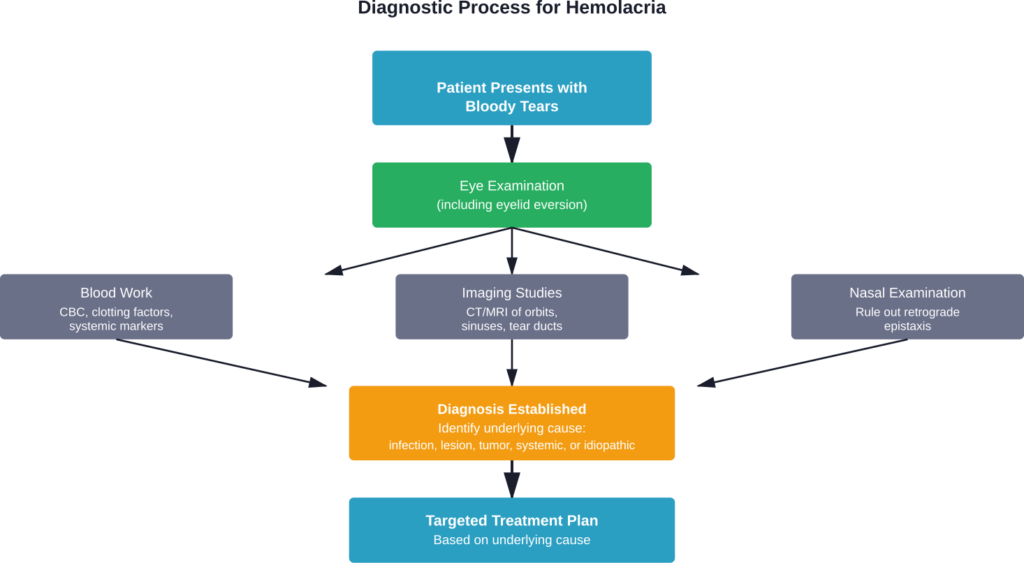
Anyone experiencing bloody tears should see an eye doctor promptly. The evaluation typically includes several components.
Thorough clinical examination comes first. The ophthalmologist examines both eyes with magnification, carefully checking the conjunctiva, cornea, and surrounding structures. Eyelid eversion allows inspection of areas normally hidden.
The nasal passages require examination too, since retrograde epistaxis (nosebleed flowing backward) can present as bloody tears.
Blood work may be ordered to check clotting function, complete blood counts, and markers of systemic disease.
Imaging studies like CT or MRI scans help visualize the lacrimal drainage apparatus, nasal sinuses, and surrounding structures to detect tumors or anatomical abnormalities.
In some cases, biopsy of suspicious lesions provides definitive diagnosis.
Treatment Options
Treatment depends entirely on the underlying cause. There’s no universal treatment for hemolacria itself—management targets the specific condition producing bloody tears.
Bacterial infections respond to antibiotic eye drops. Viral conjunctivitis typically resolves without specific treatment.
Pyogenic granulomas may be treated with topical timolol or steroid drops. Surgical excision becomes necessary if medical treatment fails.
Tumors require oncologic management—surgery, radiation, chemotherapy, or combination approaches depending on the type and extent of malignancy.
Trauma-related cases often heal spontaneously as injured tissues recover. Systemic disease management focuses on controlling the underlying condition.
For idiopathic cases, observation with regular follow-up proves appropriate. Many resolve spontaneously without intervention.
| Cause Category | Common Treatments | Expected Outcome |
|---|---|---|
| Bacterial Infection | Antibiotic eye drops, warm compresses | Resolution in 3-7 days |
| Pyogenic Granuloma | Topical timolol, steroids, or surgical excision | Good with treatment |
| Tumor/Malignancy | Surgery, radiation, chemotherapy | Depends on cancer type and stage |
| Trauma | Supportive care, time | Usually resolves spontaneously |
| Systemic Disease | Treat underlying condition | Varies with primary disease |
| Idiopathic | Observation, follow-up monitoring | Often spontaneous resolution |
When to Seek Medical Care
Any episode of bloody tears warrants medical evaluation. But some situations require urgent attention.
Seek immediate care if bloody tears occur alongside vision changes, severe eye pain, recent head trauma, or signs of serious illness like high fever or altered mental status.
Persistent or recurrent hemolacria needs thorough workup even without alarming symptoms—remember that occult malignancies can hide behind seemingly benign presentations.
Parents noticing bloody tears in children should seek prompt pediatric ophthalmology evaluation. While often benign in young patients, proper examination rules out serious causes.
Prognosis and Outlook
Most cases of hemolacria have excellent prognosis. Infections clear with treatment. Benign lesions respond to medical or surgical management. Even many idiopathic cases resolve without specific intervention.
The key factor determining outcome is the underlying cause. Malignancy-related hemolacria carries the prognosis of the specific cancer involved—highlighting why thorough evaluation matters so much.
Recurrence rates vary. Some people experience a single isolated episode. Others have intermittent recurrences, particularly if related to hormonal fluctuations or chronic conditions.
Hemolacria in Popular Culture
Bloody tears appear frequently in horror films, religious iconography, and supernatural fiction. Statues “weeping blood” become pilgrimage sites. Movie villains cry blood to signal their evil nature.
The term “stigmata” refers to apparent bleeding from areas corresponding to Christ’s crucifixion wounds, sometimes including bloody tears. Academia.edu hosts scholarly articles examining alleged stigmatic phenomena, including contemporary ostensible cases.
While these cultural representations often attribute supernatural causes to bloody tears, medical science provides rational explanations for genuine cases.
Frequently Asked Questions
Not inherently, but it signals the need for medical evaluation. Many causes are benign and self-limiting, but hemolacria can indicate serious conditions like tumors or systemic diseases that require urgent treatment. The danger depends on the underlying cause, not the bloody tears themselves.
Research suggests yes. A 1991 study found that 18 percent of menstruating women showed blood in their tears compared to much lower rates in men, pregnant women, and post-menopausal women. This pattern indicates hormonal influence on tear composition, though the exact mechanism remains unclear.
Extremely rare. Medical literature consists mainly of individual case reports rather than large studies, indicating the condition’s rarity. Most ophthalmologists encounter only a handful of cases throughout their careers. The exact incidence rate remains unknown due to the condition’s infrequency.
Yes, though rare. Case reports document hemolacria in infants as young as four months old. In documented infant cases, the condition typically resolved quickly with appropriate treatment and showed no recurrence during follow-up periods.
Not necessarily. Blood can originate from the nasal passages or sinuses and flow retrograde through the tear drainage system, appearing to come from the eyes. This is why nasal examination forms part of the diagnostic workup for hemolacria.
Case reports link hemolacria to psychiatric conditions like major depression and anxiety disorders. However, this represents a diagnosis of exclusion—physical causes must be ruled out first. The mechanism connecting psychological stress to bloody tears remains poorly understood.
Sometimes. Many documented cases resolved spontaneously within days without specific treatment. However, waiting without evaluation risks missing serious underlying conditions. Medical assessment determines whether observation alone is appropriate or if active treatment is needed.
Conclusion
So yes—crying blood is absolutely possible, and it’s a recognized medical phenomenon rather than horror movie fiction. Hemolacria results from various causes ranging from minor infections to serious tumors, with most cases falling on the benign end of that spectrum.
The critical takeaway? Bloody tears always warrant medical evaluation. While often harmless, they can signal conditions requiring urgent intervention.
Anyone experiencing hemolacria should schedule an ophthalmology appointment promptly. Thorough evaluation identifies the underlying cause and guides appropriate treatment, ensuring the best possible outcome.
Medical science continues documenting cases and expanding understanding of this rare condition. Each case report adds to the knowledge base, helping clinicians recognize patterns and improve diagnostic accuracy.
If you notice blood in your tears—or someone else’s—don’t panic, but don’t ignore it either. Reach out to an eye care professional for proper evaluation and peace of mind.
