Quick Summary: ADHD cannot truly develop for the first time in adulthood—it’s a neurodevelopmental disorder that begins in childhood. However, many adults receive their first ADHD diagnosis later in life because symptoms were missed, misattributed, or became more noticable as life demands increased. Research suggests most cases of “late-onset” ADHD are actually childhood ADHD that went undiagnosed.
The question keeps popping up in search bars and doctor’s offices: Can someone suddenly develop ADHD as an adult?
It’s not surprising. An estimated 2.5% of adults have ADHD, though some sources cite higher figures like 4.4% or up to 6% when including undiagnosed cases, and according to Dr. Len Adler, at least 75% of adults who have ADHD don’t even know they have the condition. Social media has amplified awareness, with countless adults sharing their late-diagnosis stories and wondering whether ADHD appeared out of nowhere.
But here’s the thing—the science tells a more nuanced story than a simple yes or no.
Understanding ADHD as a Neurodevelopmental Disorder
Attention-deficit/hyperactivity disorder (ADHD) is classified as a neurodevelopmental disorder. That classification matters because it means ADHD originates during brain development in childhood.
According to the National Institute of Mental Health, ADHD is marked by persistent symptoms of inattention, hyperactivity, and impulsivity. Symptoms begin in childhood and can interfere with daily life, including social relationships, school performance, and work.
Research from NIMH shows that in youth with ADHD, the brain matures in a normal pattern but is delayed three years on average in some regions, particularly at the front of the brain’s cortex, compared to youth without the disorder. This developmental difference doesn’t suddenly appear at age 30 or 40.
The official diagnostic criteria reflect this understanding. Diagnostic criteria require evidence of ADHD symptoms before age 12 for formal diagnosis, as reflected in current classification systems.
What the Research Actually Shows About Late-Onset ADHD
So can ADHD develop later in life? The scientific consensus is clear: true late-onset ADHD—where symptoms first appear in adulthood with no childhood history—is extremely rare and debated.
Multiple longitudinal studies paint a compelling picture. Research published in the Journal of the American Academy of Child & Adolescent Psychiatry found that adults presenting with ADHD symptoms rarely show evidence of the disorder starting in adulthood when childhood history is carefully examined.
Research examining late-onset ADHD in women found that while a portion of women without childhood ADHD met symptom criteria during adolescence or adulthood, very few showed the needed combination of impairment and cross-situational symptoms without significant co-occurring mental health problems.
Research examining ADHD trajectories from childhood to adulthood suggests the existence of distinct presentations with different developmental patterns—but evidence indicates symptoms originate in early development, not adulthood.
Real talk: If someone receives an ADHD diagnosis at 35, the disorder didn’t suddenly materialize. The symptoms were there earlier but went unnoticed or undiagnosed.
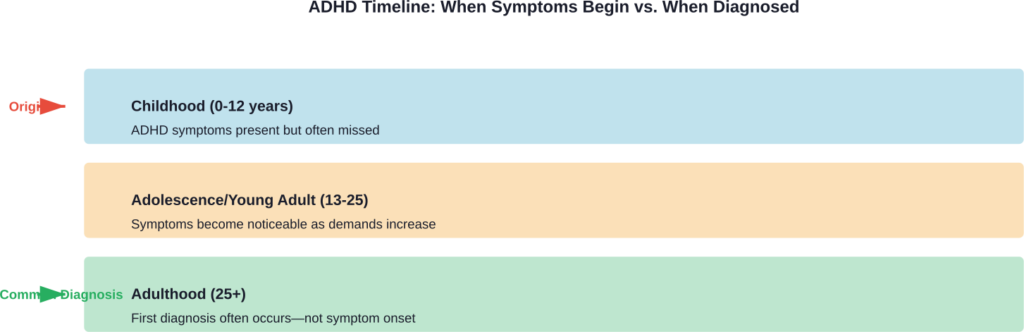
Why Adults Get Diagnosed With ADHD Later in Life
If ADHD doesn’t develop in adulthood, why are so many adults being diagnosed for the first time?
Several factors contribute to late diagnosis:
Childhood Symptoms Were Missed or Dismissed
Many adults with late diagnoses had symptoms as children that flew under the radar. Girls and women are particularly affected—they’re more likely to present with inattentive symptoms rather than hyperactivity, making their struggles less visible to parents and teachers.
A child who daydreams, seems scattered, or struggles with organization might be labeled “spacey” or “not applying themselves” rather than evaluated for ADHD.
Compensatory Strategies Masked Symptoms
Smart, creative kids often develop workarounds for their ADHD symptoms. They might rely on natural intelligence to compensate for poor focus, or use external structures provided by parents and teachers to stay organized.
These coping mechanisms can work well enough through high school. But when adult life removes those supports—hello, college or first job—the symptoms become impossible to ignore.
Life Demands Increased Beyond Coping Capacity
Research suggests that emergence of ADHD symptoms and corresponding impairment functions as performance demands increase and environmental supports decrease during development.
Managing a career, household, children, and relationships requires executive function skills that ADHD directly impacts. What looked like “just being forgetful” in your twenties becomes a serious problem when juggling multiple responsibilities.
Hormonal Changes Revealed Underlying ADHD
Women often report ADHD symptoms becoming more noticeable during pregnancy, postpartum, or perimenopause. Hormonal fluctuations don’t cause ADHD but can unmask symptoms that were previously manageable.
Other Conditions Were Treated First
ADHD frequently co-occurs with anxiety, depression, and other mental health conditions. Adults might spend years treating these conditions without realizing ADHD is the underlying issue making everything harder to manage.
| Factor | How It Delays Diagnosis | Common in Which Groups |
|---|---|---|
| Inattentive presentation | Less disruptive, easier to overlook | Girls and women |
| High intelligence | Compensates for executive dysfunction | Academically gifted individuals |
| Strong support systems | External structure masks organizational struggles | Those with involved parents/partners |
| Co-occurring conditions | Anxiety or depression treated instead of ADHD | Adults with multiple diagnoses |
How ADHD Symptoms Change From Childhood to Adulthood
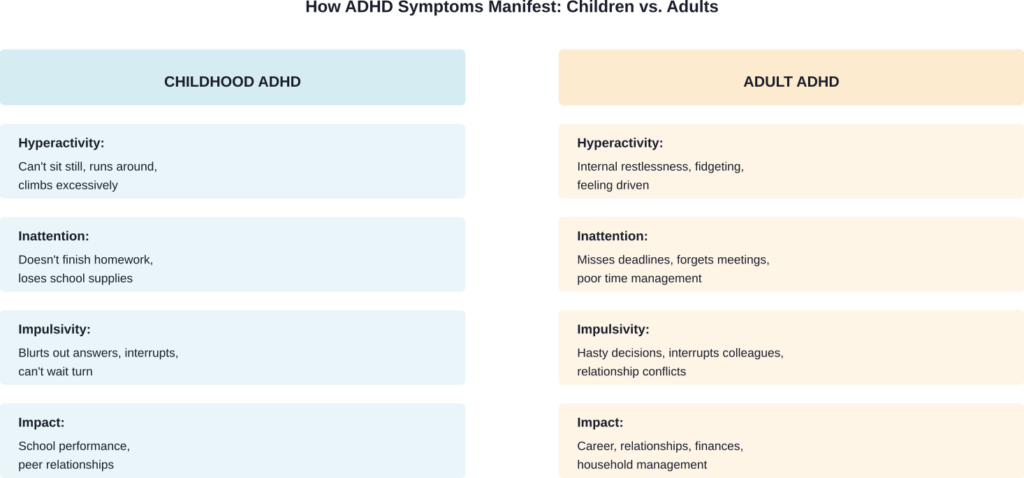
ADHD doesn’t look the same at 8 and 38. That’s another reason late diagnosis is so common.
The hyperactive child who couldn’t sit still might become an adult with internal restlessness rather than obvious physical activity. Impulsivity might shift from blurting out answers in class to interrupting colleagues or making hasty decisions.
Adult ADHD symptoms often affect time management, organization, focus, impulsivity, and restlessness differently than childhood presentations.
Adults with ADHD may experience difficulty paying attention during conversations, trouble completing tasks, forgetfulness about routine activities, and challenges with time management. These symptoms are more severe, frequent, and persistent than typical adult distractibility, interfering with daily life and occurring across multiple situations for at least 6 months.
Sleep problems are especially prevalent in adults with ADHD and can worsen symptoms. Research indicates that sleep deprivation can mimic ADHD and worsen already-present ADHD, as can lack of exercise and nutritional insufficiencies.
Getting an ADHD Diagnosis as an Adult
Recognizing potential ADHD is step one. Getting a proper diagnosis requires thorough evaluation.
ADHD is diagnosed differently in children and adults. A comprehensive screening is important because other conditions can mimic ADHD, including anxiety, depression, stress, sleep disorders, and thyroid problems.
According to the National Institute of Mental Health, proper adult ADHD diagnosis involves:
- Detailed history of symptoms dating back to childhood
- Assessment of current symptoms across multiple life areas
- Evaluation of functional impairment
- Screening for co-occurring conditions
- Sometimes input from family members who knew the person as a child
That childhood history requirement is critical. A clinician making an adult ADHD diagnosis needs evidence that symptoms were present before age 12, even if they weren’t recognized as ADHD at the time.
But wait—what if someone genuinely can’t remember their childhood clearly or doesn’t have family members to corroborate?
Clinicians work with available information, looking for patterns in school records, report cards, or the person’s recollection of struggles that fit ADHD symptom clusters. The diagnosis focuses on whether the presentation is consistent with ADHD’s developmental course.
Treatment Options for Adults With ADHD
The good news? Treatment is available and effective for adults with ADHD, regardless of when diagnosis occurs.
According to NIMH, treatment approaches include:
Medication: Stimulant medications (like methylphenidate and amphetamines) and non-stimulant options can significantly improve focus, impulse control, and executive function. These work by affecting neurotransmitter activity in the brain.
Cognitive Behavioral Therapy: CBT helps develop practical strategies for managing symptoms, addressing negative thought patterns, and building organizational skills.
Executive Function Coaching: Specialized coaching targets the specific planning, time management, and organizational challenges that ADHD creates.
Lifestyle Modifications: Regular exercise, consistent sleep schedules, stress management, and structured routines all support ADHD management.
Research shows that while 60% of those studied had ADHD symptoms in adulthood, some were no longer impaired by it. The key distinction is between having symptoms and being functionally impaired—treatment targets reducing that impairment.
What Conditions Can Look Like Adult-Onset ADHD
Here’s where things get tricky. Several conditions produce symptoms that overlap with ADHD but have different causes and treatments.
| Condition | Overlapping Symptoms | Key Differences |
|---|---|---|
| Anxiety disorders | Difficulty concentrating, restlessness | Symptoms worsen with specific triggers, respond to anxiety treatment |
| Depression | Poor focus, fatigue, disorganization | Mood symptoms prominent, symptoms episodic rather than lifelong |
| Sleep disorders | Inattention, memory problems, irritability | Resolve with proper sleep treatment |
| Thyroid problems | Concentration issues, restlessness | Physical symptoms present, abnormal thyroid labs |
| Chronic stress | Forgetfulness, difficulty focusing | Related to specific stressors, improves when stress reduces |
This is why thorough evaluation matters. Treating someone for ADHD when they actually have a sleep disorder won’t solve the problem.
Frequently Asked Questions
ADHD doesn’t suddenly appear in adulthood. It’s a neurodevelopmental disorder that begins in childhood. What can happen in your 30s or 40s is finally recognizing and diagnosing ADHD that was present but unidentified earlier. Increased life demands often make previously manageable symptoms become problematic.
Increased awareness, reduced stigma, better understanding of how ADHD presents in adults (especially women), and greater recognition of inattentive presentations have led to more adult diagnoses. Many of these adults had ADHD all along but didn’t fit the stereotypical hyperactive child profile that previously defined the disorder.
Yes, chronic stress, trauma, anxiety, depression, and sleep disorders can all produce symptoms that resemble ADHD. This is why comprehensive evaluation is essential—these conditions require different treatment approaches than ADHD, though they can also co-occur with ADHD.
Women are more likely to have inattentive-type ADHD rather than hyperactive presentations, making symptoms less obvious to observers. Hormonal changes during menstrual cycles, pregnancy, and menopause can affect symptom severity. Women also face delayed diagnosis more often because childhood symptoms were overlooked or attributed to other causes.
Absolutely. Many factors cause childhood ADHD to be missed—inattentive presentation, compensatory strategies, high intelligence, strong support systems, or simple lack of awareness. The diagnostic requirement is that symptoms were present in childhood, not that diagnosis occurred in childhood.
Start by consulting a healthcare provider experienced in adult ADHD—this might be a psychiatrist, psychologist, or specialized ADHD clinic. Gather any childhood records (report cards, evaluations) that might document early symptoms. Be prepared to discuss how symptoms have affected various life areas over time. Avoid self-diagnosis based solely on social media content.
It’s the same disorder at different life stages. The underlying neurodevelopmental differences persist, but symptom expression changes with age. Hyperactivity often becomes internalized restlessness. Impulsivity might shift from physical to verbal or decision-making. Adult responsibilities reveal executive function challenges that structured childhood environments may have masked.
The Bottom Line on ADHD and Age
So can someone develop ADHD later in life? The scientific answer is no—ADHD is a neurodevelopmental disorder that originates in childhood brain development.
But can someone be diagnosed with ADHD for the first time as an adult? Absolutely, and it happens frequently.
The distinction matters for understanding what’s happening, but it doesn’t diminish the validity of late diagnosis or the relief many adults feel finally having an explanation for lifelong struggles.
If symptoms that look like ADHD are genuinely appearing for the first time in adulthood with zero childhood history, other explanations should be explored—sleep disorders, hormonal changes, chronic stress, anxiety, depression, or other medical conditions.
Getting proper evaluation from a qualified professional is the critical next step. ADHD is highly treatable, and adults who receive appropriate treatment often experience significant improvement in functioning and quality of life.
Don’t let uncertainty about when symptoms started prevent seeking help. Whether ADHD was identified at 8 or 38, effective treatment and support can make a meaningful difference going forward.
