Quick Summary: Yes, it’s possible to get a pimple on your penis. These bumps form when pores become clogged with oil and dead skin cells, just like pimples elsewhere on the body. While most penile pimples are harmless and resolve on their own, some bumps may indicate other conditions like pearly penile papules, Fordyce spots, ingrown hairs, or sexually transmitted infections.
Finding a bump on the penis can be alarming. The good news? Pimples can develop anywhere on the body where pores exist, and that includes the penis.
But here’s the thing: not every bump on the penis is actually a pimple. Some lesions that look similar are completely normal anatomical features, while others might signal a condition that needs medical attention.
Understanding the difference matters. This guide covers what causes genuine penile pimples, how to distinguish them from other bumps, and when a healthcare visit becomes necessary.
What Does a Pimple on the Penis Actually Look Like?
A true pimple on the penis appears similar to acne anywhere else on the body. These lesions form when hair follicles or pores become clogged with oil, dead skin cells, and bacteria.
Penile pimples typically present as small, raised bumps. They may have a white or yellowish center (pustule) or appear as red, inflamed spots without visible pus. The surrounding area might show slight redness or irritation.
Most penile pimples develop on the shaft where hair follicles exist. They’re less common on the glans (head of the penis) since this area lacks typical pore structures found elsewhere on the body.
Common Causes of Pimples on the Penis
Several factors contribute to pimple formation in the genital area. Understanding these causes helps prevent future breakouts.
Blocked Pores and Oil Buildup
The most straightforward cause: pores get clogged. Sebaceous glands produce oil to keep skin moisturized, but excess production combined with dead skin cells creates blockages.
When bacteria enter these blocked pores, inflammation occurs. The result is what we recognize as a pimple.
Poor Hygiene Practices
Infrequent washing allows sweat, bacteria, and dead skin cells to accumulate. But the opposite extreme causes problems too—washing too frequently strips natural oils and irritates sensitive skin.
Finding the right balance matters for penile health.
Friction and Irritation
Tight clothing, rough fabrics, or frequent sexual activity can irritate skin and trigger pimple formation. Physical friction damages hair follicles and creates entry points for bacteria.
Athletic activities that involve extended periods in sweaty clothing increase this risk.
Ingrown Hairs
Shaving or trimming pubic hair sometimes results in ingrown hairs. These hairs curl back into the skin instead of growing outward, causing inflammation that resembles a pimple.
Ingrown hairs often appear as red, tender bumps with a visible hair trapped beneath the surface.

Conditions That Look Like Pimples But Aren’t
Several benign conditions create bumps that resemble pimples. Knowing the difference prevents unnecessary worry.
Pearly Penile Papules
These small, dome-shaped bumps appear in rows around the corona (the ridge where the glans meets the shaft). According to research, pearly penile papules are present in 14% to 48% of males, according to research published by the NIH.
They’re completely normal anatomical structures—not infections, not caused by poor hygiene, and not sexually transmitted. Treatment isn’t medically necessary, though removal options exist for cosmetic reasons.
Fordyce Spots
Fordyce spots are small, pale bumps that represent visible sebaceous glands. These glands exist throughout the body but become more noticeable on the penis due to thinner skin in this area.
They’re entirely harmless and extremely common. Most people have them somewhere on their body.
Folliculitis
According to the American Academy of Dermatology, folliculitis develops when hair follicles become infected or inflamed. It often resembles sudden acne breakouts.
Each affected follicle may show a red ring around it. Most people see breakouts about 12 to 48 hours after exposure to hot tubs, with symptoms appearing during community discussions about folliculitis.
Razor Bumps
The American Academy of Dermatology notes that razor bumps develop when shaved hairs curl back into the skin. These painful, itchy bumps differ from true pimples but look similar.
Changing shaving habits helps prevent them.
When Bumps Signal Something More Serious
Some penile bumps indicate conditions requiring medical evaluation. Recognizing warning signs matters.
Genital Herpes
Genital herpes causes fluid-filled blisters that eventually rupture and form painful sores. These lesions differ significantly from pimples in appearance and behavior.
Other symptoms may include itching, burning during urination, and flu-like symptoms during initial outbreaks.
Genital Warts
Caused by certain strains of human papillomavirus (HPV), genital warts appear as flesh-colored or gray growths. They may be raised or flat, single or in clusters that resemble cauliflower.
These warts transmit through direct skin contact during sexual activity.
Molluscum Contagiosum
This viral infection creates small, firm bumps with a characteristic dimpled center. The bumps spread through direct contact with infected lesions or contaminated surfaces.
While generally harmless, the condition spreads easily and requires medical management.
Hidradenitis Suppurativa
According to NIH research on acne inversa, this chronic inflammatory condition affects areas with skin folds, including the anogenital region. Prevalence ranges from less than 1% to 4% in different populations, according to medical literature on acne inversa.
The condition creates painful nodules and abscesses that can significantly impact quality of life. Medical treatment becomes necessary when this develops.
| Condition | Appearance | Key Features | Medical Attention |
|---|---|---|---|
| True Pimple | Red bump, possibly white center | Resolves in days, painless or mildly tender | Usually unnecessary |
| Pearly Penile Papules | Small domes in rows on corona | Normal anatomy, permanent, painless | Not needed |
| Fordyce Spots | Pale, small bumps | Visible oil glands, harmless | Not needed |
| Genital Herpes | Fluid-filled blisters, then sores | Painful, recurring, burning sensation | Required |
| Genital Warts | Flesh-colored, may cluster | Can spread, caused by HPV | Required |
| Molluscum | Firm bumps with dimple | Spreads easily, viral origin | Recommended |
Treatment Options for Penile Pimples
Most genuine pimples on the penis resolve without intervention. But certain approaches speed healing and prevent complications.
What Actually Works
Keep the area clean with gentle, unscented soap and warm water. Pat dry thoroughly—moisture creates breeding grounds for bacteria.
Resist the urge to squeeze or pop pimples. Breaking the skin increases infection risk and can lead to scarring.
Warm compresses applied for 10-15 minutes several times daily can reduce inflammation and encourage natural drainage.
Over-the-Counter Options
Some acne treatments work on penile skin, but caution is essential. The genital area is more sensitive than facial skin.
Benzoyl peroxide or salicylic acid products formulated for sensitive skin may help, but test a small area first. Discontinue immediately if irritation occurs.
When Professional Treatment Becomes Necessary
Medical research on acne vulgaris management shows that persistent or severe cases benefit from professional intervention. A dermatologist can prescribe topical or oral medications stronger than over-the-counter options.
For conditions like hidradenitis suppurativa affecting the genital area, NIH research indicates that aggressive treatment may be required, including surgical intervention in severe cases.
Prevention Strategies That Work
Preventing penile pimples involves consistent hygiene practices and lifestyle adjustments.
Wash the genital area daily with mild, fragrance-free soap. But don’t overdo it—washing too frequently strips protective oils and causes irritation.
Choose breathable, cotton underwear. Synthetic fabrics trap moisture and heat, creating ideal conditions for bacterial growth.
Change out of sweaty clothing promptly after exercise. Extended periods in damp athletic wear increase friction and bacterial exposure.
If shaving or trimming pubic hair, use proper technique. Shave in the direction of hair growth with a sharp, clean razor. Consider electric trimmers as a lower-risk alternative.
Maintain overall skin health through adequate hydration and a balanced diet. Healthy skin resists infection and inflammation more effectively.
When to See a Healthcare Provider
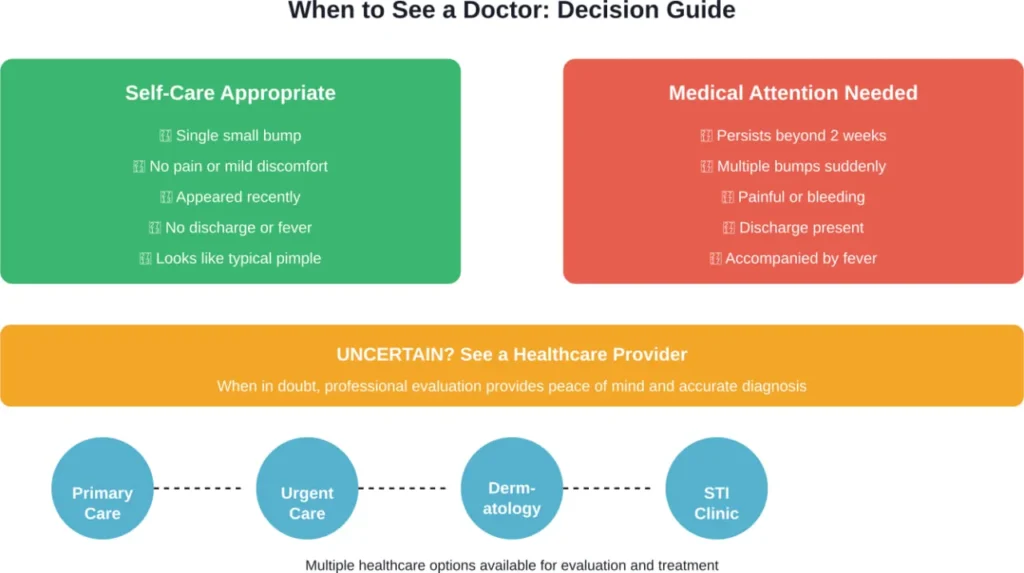
Most penile pimples don’t require medical attention. But certain situations warrant professional evaluation.
Seek medical care if bumps persist beyond two weeks without improvement. Prolonged lesions may indicate conditions other than simple pimples.
Multiple bumps appearing suddenly, especially if accompanied by pain, discharge, or fever, need prompt evaluation.
Any lesion that bleeds easily, grows rapidly, or changes appearance should be examined. While rare, these characteristics can signal more serious conditions.
If uncertain about what’s causing penile bumps, err on the side of caution. Healthcare providers diagnose these conditions regularly and can provide definitive answers.
Anyone sexually active who develops new genital bumps should consider STI testing. Many sexually transmitted infections present with lesions that resemble or coexist with pimples.
Frequently Asked Questions
No, popping or squeezing penile pimples is not recommended. Breaking the skin increases infection risk and can cause scarring. The genital area has abundant blood vessels and sensitive tissue that makes complications more likely. Allow pimples to heal naturally or consult a healthcare provider for safe removal if necessary.
Most genuine pimples on the penis resolve within 3-7 days without intervention. Larger or more inflamed lesions may take up to two weeks. If a bump persists beyond two weeks or worsens despite proper care, medical evaluation is appropriate to rule out other conditions.
Not necessarily. True pimples form from clogged pores and aren’t related to sexually transmitted infections. However, some STIs cause lesions that resemble pimples, including genital herpes, genital warts, and molluscum contagiosum. If sexually active or uncertain about the cause of bumps, STI testing provides definitive answers.
Absolutely. Penile pimples result from the same pore-clogging process that causes acne anywhere on the body. Sexual activity isn’t required for pimple formation. Factors like hygiene, friction from clothing, and natural oil production affect anyone regardless of sexual history.
Research on acne vulgaris shows diet can influence acne in some individuals, though the connection remains complex. Generally speaking, foods that trigger facial acne might affect body acne similarly. Maintaining overall skin health through balanced nutrition and hydration supports the body’s natural defenses against pimple formation.
Caution is necessary when applying acne treatments to genital skin. Products containing benzoyl peroxide or salicylic acid may work but can cause significant irritation on sensitive penile tissue. Test any product on a small area first and use formulations designed for sensitive skin. Discontinue immediately if burning, stinging, or increased redness occurs.
Yes. Tight-fitting underwear, especially synthetic fabrics, traps heat and moisture against the skin. This environment promotes bacterial growth and creates friction that irritates hair follicles. Breathable cotton underwear that fits comfortably without excessive tightness reduces these risk factors significantly.
The Bottom Line on Penile Pimples
Pimples on the penis are possible and usually harmless. They form through the same biological process as pimples elsewhere—clogged pores, oil buildup, and bacterial involvement.
Most penile pimples resolve on their own within a week. Proper hygiene, avoiding irritation, and resisting the urge to squeeze or pop bumps allows natural healing.
But not every bump is a pimple. Conditions ranging from normal anatomical variations like pearly penile papules to infections requiring medical treatment can create similar-looking lesions.
The key is knowing when to worry. Single bumps that look like typical pimples and cause minimal discomfort rarely need professional attention. Multiple lesions, persistent bumps, painful sores, or any discharge warrant medical evaluation.
When uncertain, err toward caution. Healthcare providers diagnose genital conditions routinely and can distinguish harmless pimples from issues requiring treatment. Getting checked provides both peace of mind and access to appropriate care if needed.
Take action: If experiencing concerning symptoms or bumps that don’t resolve, schedule an appointment with a primary care provider, dermatologist, or sexual health clinic. Early evaluation leads to better outcomes and reduces anxiety about uncertain symptoms.
