Quick Summary: Yes, it’s possible to take too much vitamin D, though it’s rare. Vitamin D toxicity (hypervitaminosis D) typically occurs from taking very high doses of supplements—well above 4,000 IU daily—over extended periods. Symptoms include nausea, vomiting, weakness, and dangerous calcium buildup in the blood, requiring medical attention.
Vitamin D has become something of a superstar supplement. From bone health to immune function, the research showing its benefits keeps piling up. But here’s the thing—more isn’t always better.
Can you actually take too much vitamin D? The short answer is yes. While vitamin D toxicity is uncommon, it does happen, and the consequences can be serious.
Let’s break down what the science says about safe upper limits, who’s most at risk, and what happens when supplementation crosses the line from helpful to harmful.
Understanding Vitamin D Toxicity
Vitamin D toxicity—also called hypervitaminosis D—occurs when vitamin D levels in the body become dangerously high. Unlike water-soluble vitamins that the body can flush out relatively easily, vitamin D is fat-soluble. It gets stored in fatty tissues and the liver, which means excessive amounts can accumulate over time.
But getting too much vitamin D from sunlight or food alone is virtually impossible. According to research published in medical journals, toxicity almost exclusively results from taking very high doses of supplements.
What Counts as ‘Too Much’?
The Institute of Medicine established a Tolerable Upper Intake Level (UL) of 4,000 IU per day for adults. This represents the maximum intake unlikely to cause adverse health effects for nearly all individuals.
That said, vitamin D toxicity typically requires much higher doses sustained over weeks or months. Research indicates that symptomatic toxicity usually requires very high doses sustained over weeks or months, though individual responses vary considerably.

How Vitamin D Toxicity Develops
Vitamin D toxicity doesn’t happen overnight. The mechanism behind it centers on calcium—specifically, too much of it.
When vitamin D levels spike excessively, the body absorbs far more calcium from food than it should. This leads to hypercalcemia—elevated blood calcium levels. According to research from the National Institutes of Health, hypercalcemia is the hallmark of vitamin D toxicity and the source of most symptoms.
Excessive calcium in the bloodstream can cause mineral deposits in soft tissues, including the kidneys, blood vessels, and heart. It also disrupts normal kidney function and can lead to kidney stones or even kidney failure in severe cases.
Common Causes of Vitamin D Overdose
Research examining vitamin D toxicity cases reveals several common patterns:
- Overzealous supplementation: Taking mega-doses without medical supervision, often based on misunderstanding of dosing guidelines
- Liquid formulation errors: Studies highlight liquid vitamin D supplements as particularly problematic due to measurement errors or confusion about concentration
- Multiple overlapping sources: Combining fortified foods, prescription vitamin D, and over-the-counter supplements without accounting for total intake
- Unmonitored correction protocols: Aggressive correction of vitamin D deficiency without proper blood level monitoring
According to research from Harvard Health published in JAMA, national survey data from 1999 to 2014 showed a 2.8% uptick in people taking potentially unsafe amounts of vitamin D—more than 4,000 IU daily.
Symptoms and Warning Signs
Recognizing vitamin D toxicity early matters. The symptoms stem primarily from elevated calcium levels and can range from mild to severe.
Early Warning Signs
Initial symptoms often include:
- Nausea and vomiting
- Poor appetite and weight loss
- Excessive thirst (polydipsia)
- Frequent urination (polyuria)
- Weakness and fatigue
- Constipation
According to research published in medical journals, confusion and apathy are also frequently noted in clinical presentations of vitamin D toxicity.
Advanced Symptoms
If untreated, vitamin D toxicity can progress to more serious complications:
- Severe dehydration
- Kidney stones
- Irregular heartbeat (cardiac arrhythmias)
- Bone pain (paradoxically, despite vitamin D’s role in bone health)
- Kidney damage or failure
Research from the NIH indicates that in severe cases, calcium deposits can form in vital organs, potentially causing permanent damage.
| Symptom Category | Specific Signs | Severity Level |
|---|---|---|
| Gastrointestinal | Nausea, vomiting, poor appetite, constipation | Early/Moderate |
| Urinary | Excessive thirst, frequent urination, kidney stones | Early/Moderate |
| Neurological | Confusion, apathy, weakness, fatigue | Moderate |
| Cardiovascular | Irregular heartbeat, high blood pressure | Severe |
| Renal | Kidney dysfunction, elevated creatinine | Severe |
Who’s Most at Risk?
While anyone taking excessive vitamin D can develop toxicity, certain groups face higher risk.
People with pre-existing kidney disease process vitamin D differently and may accumulate toxic levels more easily. Those with conditions affecting calcium metabolism—like hyperparathyroidism or sarcoidosis—are also more vulnerable.
Interestingly, research suggests that older adults may face particular risks. Research reported that older adults over 70 who received 60,000 IU monthly showed higher fall risk compared to those receiving 24,000 IU monthly, with serum 25(OH)D concentrations reaching 40 ng/mL (100 nmol/L).
Real talk: the vast majority of toxicity cases result from well-intentioned but misguided supplementation. According to research examining vitamin D toxicity patterns, irrational use of mega-doses represents the primary cause in documented cases.
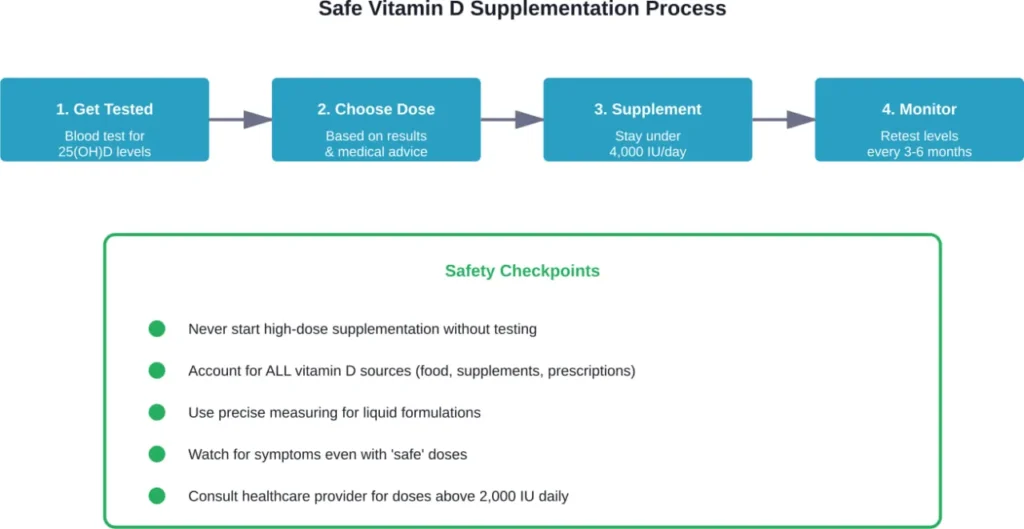
Safe Supplementation Guidelines
So how do you get the benefits of vitamin D without overdoing it?
Know Your Baseline
Before starting supplementation, get tested. A blood test measuring 25-hydroxyvitamin D—the standard marker for vitamin D status—establishes your starting point and helps determine appropriate dosing.
Optimal blood levels generally fall between 20-50 ng/mL, though some experts suggest targeting 30-40 ng/mL for most health benefits.
Follow Evidence-Based Dosing
For most adults, daily vitamin D intake recommendations look like this:
- General maintenance: 600-800 IU daily (from all sources)
- Deficiency correction: 1,000-2,000 IU daily, with medical supervision
- Upper safety limit: 4,000 IU daily maximum without medical oversight
According to the Institute of Medicine guidelines, these levels maintain adequate vitamin D status while staying well below toxicity thresholds.
Be Careful With Liquid Forms
Multiple studies examining vitamin D toxicity cases have flagged liquid formulations as particularly problematic. Droppers can be confusing, concentrations vary between products, and measurement errors happen easily.
If using liquid vitamin D, double-check the concentration and measure carefully. When possible, opt for standardized capsules or tablets with clearly labeled doses.
Treatment and Recovery
If vitamin D toxicity occurs, treatment focuses on stopping supplementation immediately and managing hypercalcemia.
Medical interventions typically include:
- Discontinuing all vitamin D supplements
- Restricting dietary calcium intake temporarily
- Intravenous fluids to support kidney function and calcium excretion
- Medications like corticosteroids or bisphosphonates in severe cases
The good news? According to medical research, vitamin D toxicity is generally reversible with appropriate treatment, though recovery can take several weeks to months depending on severity.
The Bottom Line on Safety
Here’s what the evidence tells us: vitamin D is essential for health, but the therapeutic window between deficiency and excess deserves respect.
Toxicity remains rare in the general population. When it does occur, it’s almost always preventable—the result of excessive supplementation without proper monitoring.
The safest approach combines baseline testing, evidence-based dosing, and periodic monitoring. For most people, staying under 4,000 IU daily and getting regular blood work provides the sweet spot of benefits without risks.
Sound familiar? That’s because safe supplementation isn’t complicated—it just requires a bit of common sense and medical guidance.
Frequently Asked Questions
No. The body self-regulates vitamin D production from sun exposure, converting excess into inactive metabolites. Research confirms that toxicity from sunlight alone is physiologically impossible. However, combining sun exposure with high-dose supplements can contribute to excessive levels.
Toxicity typically requires weeks to months of excessive intake. Because vitamin D is fat-soluble and accumulates in tissues, single large doses rarely cause toxicity. According to medical research, symptomatic hypervitaminosis D usually results from sustained daily doses well above 10,000 IU over extended periods.
Toxicity generally occurs when blood levels of 25-hydroxyvitamin D exceed 150 ng/mL. However, research shows highly variable individual responses—some people develop hypercalcemia at levels below this threshold. Optimal therapeutic levels fall between 20-50 ng/mL for most individuals.
While 5,000 IU exceeds the established upper limit of 4,000 IU daily, many people tolerate this dose without issues short-term. However, doses above 4,000 IU should be taken only under medical supervision with periodic blood monitoring. Long-term use at this level may increase toxicity risk for some individuals.
In severe cases, yes. Prolonged hypercalcemia can cause irreversible kidney damage, calcification of soft tissues, and cardiovascular complications. However, according to NIH research, when caught early and treated appropriately, vitamin D toxicity is generally reversible without lasting effects.
Diagnosis requires blood tests measuring 25-hydroxyvitamin D levels (to confirm excessive vitamin D) and serum calcium levels (to detect hypercalcemia). Additional tests may assess kidney function, urine calcium excretion, and parathyroid hormone levels to evaluate the extent of metabolic disruption.
Both forms can cause toxicity at excessive doses, though vitamin D3 (cholecalciferol) is more potent and raises blood levels more effectively than D2 (ergocalciferol). Most documented toxicity cases involve D3 supplements. The upper limit of 4,000 IU applies to combined intake of both forms.
Moving Forward Safely
Vitamin D supplementation offers genuine health benefits when done right. The key is respecting the difference between correcting deficiency and chasing arbitrarily high levels.
Before starting any supplement regimen, get tested. Work with a healthcare provider to determine your individual needs. Monitor your levels periodically, especially if taking doses above 2,000 IU daily.
And remember—more isn’t always better. The goal isn’t to maximize vitamin D levels, but to optimize them within the safe, effective range that supports health without risking harm.
Ready to supplement safely? Start with testing, not guessing. Your body—and your future self—will thank you.
