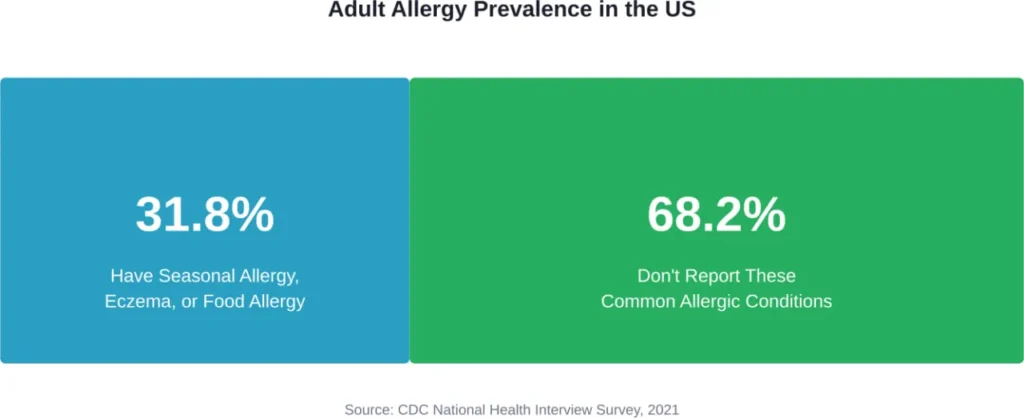
Quick Summary: Most people do have at least one allergy, but it’s entirely possible to have no allergies at all. According to CDC data, approximately 31.8% of adults have seasonal allergies, eczema, or food allergies—which means roughly 68% may have none of these common allergic conditions. Allergies develop when the immune system mistakenly identifies harmless substances as threats, but not everyone’s immune system responds this way.
The assumption that everyone suffers from some type of allergy is surprisingly common. Walk into any pharmacy during spring, and the rows of antihistamines suggest allergies are universal.
But here’s the thing—they’re not.
According to the CDC’s National Health Interview Survey from 2021, nearly one-third of adults aged 18 and over had a seasonal allergy, eczema, or food allergy. That’s 31.8% of the adult population. Flip that statistic around, and roughly 68% of adults don’t report these common allergic conditions.
So yes, it’s absolutely possible to go through life without being allergic to anything. The real question is: what determines who develops allergies and who doesn’t?
What Are Allergies, Anyway?
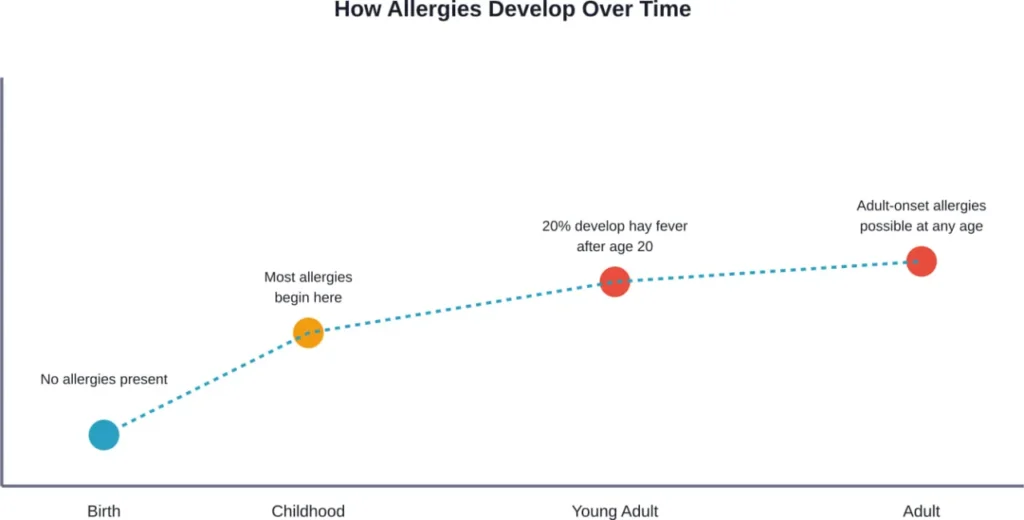
Allergies are conditions in which the immune system mistakes a specific substance for a danger and launches an attack. The American Academy of Allergy, Asthma & Immunology explains that no individual is born with allergies—they develop over time.
When someone encounters a food, pollen, or pet dander for the first time, their immune system might identify a protein in that substance as an allergen. The body then produces IgE antibodies specific to that allergen.
The next time exposure happens, these antibodies trigger the release of histamine and other chemicals, causing symptoms ranging from sneezing and itching to life-threatening anaphylaxis.
But not everyone’s immune system operates this way. Some people’s immune systems correctly identify harmless substances as, well, harmless.
The Numbers: How Common Are Allergies?
The CDC data from 2021 provides concrete insight into allergy prevalence among American adults. Seasonal allergies topped the list as the most common allergic condition.
The prevalence varied by demographic factors. Sex, age, and race all influenced allergy rates. Younger adults showed different patterns than older populations.
Food allergies impact millions of children and adults, often developing in infancy or early childhood. But the AAAAI notes that allergies can develop at any time and affect individuals of all ages.
Community discussions reveal varying experiences. Some people report never experiencing allergic reactions to anything, while others develop new allergies in adulthood.
Why Some People Don’t Develop Allergies
The factors that protect some people from developing allergies remain an active area of research. Genetics play a significant role.
A recent study from UT Southwestern Medical Center published in February 2026 used whole exome sequencing to examine DNA from 56 patients and their family members. Nearly 40% carried a rare loss-of-function mutation in genes known to increase allergy risk.
This research helps explain why food allergies run in families. Children where one or both parents have an allergic disease are more likely to develop these conditions themselves.
But genetics aren’t the whole story. Environmental factors matter tremendously.
The hygiene hypothesis suggests that reduced exposure to microbes during childhood might increase allergy susceptibility. Early-life exposures to animals, farm environments, and diverse microorganisms may train the immune system to tolerate harmless substances.
Genome-wide association studies (GWAS) have identified significant associations for nearly 100 asthma genes/loci. These findings underscore the complex interplay between multiple genetic variants and environmental triggers.
Can You Develop Allergies Later in Life?
One persistent myth suggests allergies only develop during childhood. The AAAAI directly addresses this misconception: while many allergies present during childhood, developing allergies as an adult is not uncommon.
Approximately 30-90 million individuals in the U.S. are affected by hay fever, with 20% of those developing symptoms after age 20. Real talk: your immune system doesn’t stop learning and adapting just because you’re an adult.
Several factors can trigger adult-onset allergies. Changes in environment, moving to a new location with different pollen types, increased exposure to pets, or occupational allergens can all prompt new allergic responses.
The CDC reports that occupational rhinitis affects between 5% and 65% of workers depending on occupation, costing an estimated $593 per year per employee due to productivity losses. Contact dermatitis ranks as the second most commonly reported occupational illness after repeated traumatic injury.
So even if someone spent their first 30 years allergy-free, new sensitivities can emerge based on exposures and immune system changes.
Common Allergy Myths Debunked
Several misconceptions about allergies persist despite evidence to the contrary. The AAAAI addresses multiple food allergy myths that apply broadly.
Myth: Pet allergies are triggered by animal hair.
Fact: Allergies are actually caused by proteins found in pet skin (dander), saliva, and urine. Some dog breeds are labeled hypoallergenic because they shed less, but no dog is 100% hypoallergenic—even hairless dogs produce allergens.
Myth: If there’s no allergic reaction within 30 minutes of exposure, there won’t be one.
Fact: Symptoms can start within seconds of eating a food allergen, but it can take longer depending on the allergen and individual. Delayed reactions do occur.
Myth: Everyone eventually develops at least one allergy.
Fact: Based on available data, the majority of adults don’t report common allergic conditions. It’s entirely possible to remain allergy-free throughout life.
Living Without Allergies: The Reality
For those who don’t experience allergies, life looks markedly different during peak pollen season. No antihistamines, no avoiding certain foods, no epinephrine auto-injectors.
But wait. Does having no diagnosed allergies mean someone is completely immune to developing them?
Not necessarily. The immune system continuously encounters new substances and can develop sensitivities at any point. Environmental changes, increased exposure to specific allergens, or shifts in immune function can trigger new allergic responses.
The question often arises in community discussions: is having zero allergies rare?
Based on CDC data showing 68.2% of adults without the most common allergic conditions, being allergy-free appears to be the statistical majority—at least when considering seasonal allergies, eczema, and food allergies specifically. Other allergic conditions like drug allergies or insect sting allergies weren’t included in that particular dataset.
Testing and Diagnosis
Determining whether someone has allergies involves specific medical testing. Skin testing is common: a small amount of extract made from the suspected allergen is placed on the back or arm.
If a raised bump or small hive develops within 20 minutes, it indicates a possible allergy. If nothing develops, the test is negative.
Blood tests measuring allergen-specific IgE antibodies provide another diagnostic approach. These tests can identify sensitivities even when someone hasn’t experienced noticeable symptoms.
Some people may have low-level sensitivities that never produce clinical symptoms. In these cases, the immune system generates some response to certain substances but not enough to cause noticeable reactions.
| Allergy Type | Common Triggers | Likelihood of Outgrowing |
|---|---|---|
| Seasonal Allergies | Pollen, mold spores, grass | Low – typically lifelong |
| Food Allergies (milk, egg) | Proteins in specific foods | High – often outgrown by adulthood |
| Food Allergies (peanuts, tree nuts) | Nut proteins | Low – usually persist |
| Pet Allergies | Dander, saliva, urine proteins | Low – typically lifelong |
| Drug Allergies | Antibiotics, NSAIDs | Varies by medication |
Treatment Options for Those With Allergies
For the 31.8% who do experience allergies, multiple treatment approaches exist. Avoidance of known allergens forms the first line of defense.
Prescription nasal sprays, antihistamines, and other medications help manage symptoms. When allergies are severe enough and medications don’t provide adequate relief, immunotherapy becomes an option.
Allergy shots work well for 80 percent of patients, because they can desensitize patients to the allergen. Some patients report significant improvement or even resolution of symptoms over time.
The treatment involves gradually increasing doses of the allergen, training the immune system to tolerate it rather than attack it.
Frequently Asked Questions
Yes, it’s completely normal. According to CDC data, approximately 68% of adults don’t report having seasonal allergies, eczema, or food allergies. Having no allergies is actually more common than having them.
Absolutely. The AAAAI confirms that allergies can develop at any age. About 20% of people with hay fever develop symptoms after age 20. Environmental changes, new exposures, or shifts in immune function can trigger adult-onset allergies.
Genetics play a significant role in allergy susceptibility. Recent research from UT Southwestern found that nearly 40% of patients with food allergies carried rare loss-of-function mutations in genes that increase allergy risk. However, environmental factors also strongly influence whether allergies develop.
It’s possible but not guaranteed. The immune system can develop new sensitivities throughout life based on exposures and other factors. However, many people remain allergy-free their entire lives. There’s no way to predict with certainty.
Yes, allergies tend to run in families. Children with one or both parents who have allergic diseases are more likely to develop allergies themselves. Genome-wide association studies have identified nearly 100 genes associated with asthma and allergic diseases.
Allergy testing can identify sensitivities to specific tested allergens. Skin tests and blood tests measure immune responses to particular substances. However, testing every possible allergen isn’t practical. A negative test result for common allergens suggests low allergy risk but doesn’t guarantee zero allergies to all substances.
People with no allergies don’t produce IgE antibodies against common allergens and experience no symptoms upon exposure. Those with mild allergies do produce these antibodies and experience symptoms—they’re just less severe. Mild allergies still represent an immune system overreaction, just with less intense manifestations.
The Bottom Line
The short answer? Yes, it’s absolutely possible to not be allergic to anything. The data supports this—the majority of adults don’t report the most common allergic conditions.
Allergies result from complex interactions between genetic predisposition and environmental factors. Some immune systems correctly identify harmless substances as non-threatening, while others mount unnecessary defensive responses.
For those living without allergies, count it as a genetic and environmental win. For those who do experience allergies, effective management strategies exist, from simple avoidance to immunotherapy.
If concerns about potential allergies arise, consultation with an allergist can provide clarity through proper testing and evaluation. Understanding individual allergy status helps inform decisions about environments, foods, and activities.
