Quick Summary: Yes, it is possible to miscarry one twin in a multiple pregnancy, a phenomenon known as vanishing twin syndrome. This occurs most commonly in the first trimester when one embryo stops developing and is reabsorbed by the body, while the surviving twin continues to grow normally. The condition affects approximately 7% to 36% of twin pregnancies detected on early ultrasound.
Finding out you’re carrying twins brings a unique mix of excitement and anxiety. But what happens when one of those babies suddenly disappears from ultrasound scans? It’s a reality that affects more twin pregnancies than many people realize.
The loss of one twin during pregnancy is medically recognized and relatively common, especially with the increased use of early ultrasound technology. Understanding what causes this, how it impacts the surviving baby, and what mothers can expect helps navigate this emotionally complex situation.
What Is Vanishing Twin Syndrome?
Vanishing twin syndrome (VTS) describes a specific type of miscarriage where one embryo in a multiple pregnancy stops developing and disappears. The term “vanishing” refers to how the lost twin is reabsorbed by the mother’s body, the placenta, or the surviving twin.
Beginning around 1945, doctors started recognizing that some singleton births were originally twin pregnancies. One baby was miscarried during the first trimester while the other continued developing normally. Today, with widespread use of early ultrasound technology, this phenomenon is detected far more frequently than in previous decades.
The condition differs significantly depending on when it occurs during pregnancy. Early first-trimester losses typically result in complete reabsorption with minimal complications. Later losses present more complex medical scenarios.
How Common Is It?
The incidence of vanishing twin syndrome varies based on several factors, particularly the timing of initial ultrasound and method of conception.
According to available data, approximately 7% to 36% of IVF twin pregnancies experience vanishing twin syndrome. Couples undergoing in vitro fertilization often have ultrasounds as early as weeks six or seven of pregnancy, which increases the likelihood of detecting very early twin pregnancies that might otherwise go unnoticed.
Research indicates the rate of disappearance could be as high as 29% in some populations. Natural conception twin pregnancies show different rates than IVF pregnancies. One study found the incidence of VT was statistically significantly higher after natural conception (18.2% of twins) compared to IVF-ICSI (12.6% of twins).
Here’s the thing though—these numbers are higher than historical estimates precisely because modern ultrasound technology detects pregnancies earlier than ever before. Many vanishing twin cases would have gone completely undetected in previous generations.

What Causes One Twin to Be Miscarried?
The exact causes of vanishing twin syndrome aren’t always clear, but several factors contribute to why one embryo stops developing.
Chromosomal abnormalities represent the most common cause. Just as with singleton miscarriages, genetic issues that prevent normal development often lead to early pregnancy loss. The embryo with chromosomal problems stops growing while the genetically healthy twin continues.
Implantation issues can also play a role. If one embryo doesn’t implant properly in the uterine wall, it may not receive adequate nutrition and oxygen to sustain development.
Insufficient placental support affects twin pregnancies uniquely. In cases where twins share a placenta (monochorionic twins), unequal blood flow can cause one twin to receive insufficient resources.
According to ACOG data, advances in laboratory techniques and professional standards have significantly reduced the incidence of twins and higher-order multiple births through improved embryo transfer protocols. Between 1980 and 2009, the twin birth rate had increased 76%, from 18.9 to 33.3 per 1,000 live births, though it has since declined.
Risk Factors
Certain conditions increase the likelihood of vanishing twin syndrome:
- Advanced maternal age (over 35)
- IVF and assisted reproductive technologies
- Pre-existing maternal health conditions
- Poor embryo quality
- Suboptimal implantation conditions
One study found that pregnancies complicated with pregestational or gestational diabetes showed different odds of vanishing twin occurrence, suggesting maternal metabolic conditions may influence twin survival rates.
When Does Vanishing Twin Syndrome Occur?
The timing of twin loss matters significantly for both medical management and outcomes.
First Trimester Loss
Most vanishing twin cases happen during the first trimester, particularly between weeks 6 and 12. According to ACOG, early pregnancy loss is common during this period, and the terms miscarriage, spontaneous abortion, and early pregnancy loss are used interchangeably in medical literature for first-trimester losses.
Early first-trimester vanishing typically results in complete reabsorption. The mother’s body, placenta, or surviving twin absorbs the tissue from the lost embryo. By the time of later ultrasounds, little to no evidence of the second twin remains visible.
Many women experience no symptoms during early vanishing twin syndrome. The pregnancy simply continues as a singleton pregnancy without complications.
Late Second or Third Trimester Loss
The death of a twin in the late second or third trimester is considerably rarer but represents a more serious obstetric complication. According to medical research, this scenario is associated with increased maternal and fetal morbidity and mortality.
When fetal demise occurs later in pregnancy, the lost twin doesn’t vanish through reabsorption. Instead, it may become what’s called a fetus papyraceus—a flattened, mummified fetus that remains alongside the living twin until delivery.
Late-term single fetal demise requires careful medical management in a tertiary center with competent neonatal support, according to obstetric guidelines.
Symptoms of Losing One Twin
The symptoms of vanishing twin syndrome vary considerably. Some women experience noticeable signs while others have none at all.
Common Symptoms
When symptoms do occur, they may include:
- Mild cramping or pelvic pain
- Light vaginal bleeding or spotting
- Decrease in pregnancy symptoms (nausea, breast tenderness)
- Passage of tissue or clots
But here’s what makes this tricky: these same symptoms can occur in normal pregnancies due to other causes like subchorionic hematomas or implantation bleeding.
Community discussions reveal that some women report significant bleeding events. According to a Reddit account from a parent in the r/pregnant community, at 12 weeks they woke in a pool of blood and passed what appeared to be a gestational sac, yet ultrasound confirmed the remaining baby was still alive and well. They had previously been diagnosed with a subchorionic hematoma at 10 weeks.
Silent Vanishing
Many cases produce no symptoms whatsoever. The loss is discovered only during routine ultrasound when healthcare providers note that a previously detected second embryo is no longer visible.
This silent presentation is actually the most common scenario, especially for very early first-trimester losses detected on 6-7 week ultrasounds.
How Vanishing Twin Syndrome Is Diagnosed
Diagnosis occurs almost exclusively through ultrasound imaging.
An initial ultrasound shows two gestational sacs or two embryos with heartbeats. A follow-up scan reveals only one continuing pregnancy. The second gestational sac has either disappeared completely or shows an embryo without cardiac activity.
First-trimester ultrasound has become a method of choice for detection of major structural fetal anomalies in multiple gestations, according to medical research. Increased nuchal translucency (NT) measurements between 11-14 weeks in multiple pregnancies can serve as a screening tool for chromosomal anomalies.
Healthcare providers confirm vanishing twin syndrome by:
- Documenting the presence of two embryos on early ultrasound
- Confirming the absence or non-viability of one embryo on subsequent scans
- Ruling out other causes of bleeding or symptoms
- Monitoring the continuing pregnancy for normal growth
No additional testing is typically required for first-trimester vanishing twin syndrome. The diagnosis is clinical based on ultrasound findings.
Risks to the Surviving Twin
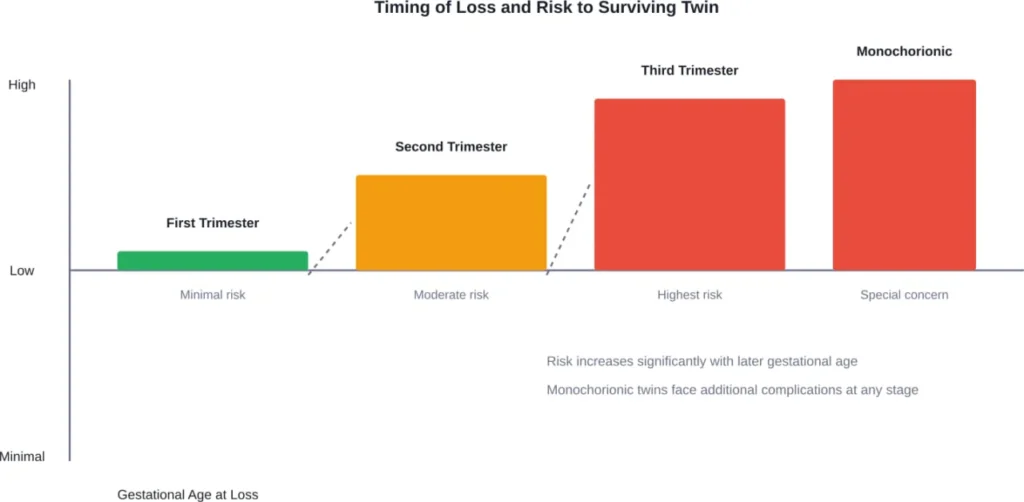
The impact on the remaining baby depends heavily on when the loss occurs and the type of twin pregnancy.
First Trimester Vanishing: Minimal Risk
When vanishing occurs in the first trimester, the surviving twin generally faces minimal additional risk. The pregnancy continues normally, and most babies are born healthy at term.
Research shows that early vanishing twin syndrome typically doesn’t compromise the development or health of the continuing singleton pregnancy.
Later Loss: Increased Concerns
Single fetal demise later in pregnancy presents more serious concerns. Both the mother and the surviving baby face increased risks for complications.
The type of placentation matters enormously. According to RCOG guidelines, approximately 30% of twin pregnancies in the UK are monochorionic (identical twins sharing a placenta). MCDA twins (identical twins with separate amniotic sacs) account for approximately 20% of all twins.
According to RCOG research, children born from complicated monochorionic twin pregnancies have a high rate of adverse neurodevelopmental outcomes (14.5%) compared to uncomplicated twin pregnancies (7.6%). The shared placental circulation in monochorionic twins means the death of one twin can affect the surviving co-twin through hemodynamic changes and thromboplastic material transfer.
Prematurity Risks in Multiple Pregnancies
According to RCOG patient information, overall around 8 in 100 babies (8%) are born prematurely (before 37 weeks). For twin pregnancies specifically, if pregnant with twins you have a 60 in 100 (60%) chance of going into labour early.
Multiple pregnancy complications increase the likelihood of preterm labor and birth. According to multiple academic medical sources, over 60 percent of twins and nearly all higher-order multiples are premature (born before 37 weeks). The higher the number of fetuses in the pregnancy, the greater the risk of preterm birth.
Risks to the Mother
Maternal risks also depend on timing and circumstances of the twin loss.
First Trimester Loss
Early vanishing twin syndrome poses minimal risk to maternal health. Most women continue their pregnancies without complications.
Some may experience:
- Emotional distress from the loss
- Anxiety about the surviving baby’s health
- Temporary cramping or bleeding
Physical risks remain low, and the pregnancy typically proceeds as a normal singleton gestation.
Later Pregnancy Complications
Late-term single fetal demise carries greater maternal risks including:
- Preterm labor or delivery
- Hemorrhage
- Infection
- Disseminated intravascular coagulation (rare)
- Psychological trauma
According to ACOG management guidelines for stillbirth, women with a previous stillbirth face increased risk of recurrence. Compared with women with no history of stillbirth, those who experienced stillbirth in an index pregnancy had significantly increased risk in subsequent pregnancies (pooled odds ratio of 4.83; 95% CI, 3.77–6.18), which remained significant after adjustment for confounding factors.
Medical Management and Monitoring
How healthcare providers manage vanishing twin syndrome depends on when it occurs and any associated complications.
First Trimester Management
For early vanishing twin diagnosed in the first trimester:
- Expectant management (watchful waiting) is standard
- Regular ultrasound monitoring of the surviving twin
- Standard prenatal care continues
- No specific intervention needed in most cases
The pregnancy is managed as a singleton pregnancy going forward.
Late Pregnancy Management
According to published medical guidelines, late-term single fetal demise requires:
- Counseling and emotional support
- Individualized management plan
- Management in a tertiary center with competent neonatal support
- Information on chorionicity (placental type)
- Evaluation of fetal anomalies and complications
Healthcare teams must balance the risks of immediate delivery against continued expectant management, considering gestational age, maternal condition, and the health of the surviving twin.
Emotional Impact and Support
Losing one twin creates a complex emotional situation. Parents experience grief for the lost baby while simultaneously celebrating the continuing pregnancy.
This emotional duality can feel isolating. Joy and sorrow coexist, making it difficult to process feelings or seek appropriate support.
Community experiences shared online reveal the confusion many parents feel. Some describe the surreal experience of mourning one baby while preparing for another. Others struggle with guilt or fear about the surviving twin’s health.
Healthcare providers should offer:
- Acknowledgment of the loss and the parents’ grief
- Clear information about what happened and why
- Reassurance about the surviving baby (when appropriate)
- Referrals to counseling or support groups
- Space to discuss fears and concerns
The psychological impact deserves recognition and professional support when needed.
Long-Term Outcomes
Research on long-term outcomes for surviving twins shows generally favorable results, particularly for first-trimester vanishing.
According to medical literature examining adverse obstetric outcomes, various factors influence final pregnancy outcomes. The specific timing of vanishing, maternal health conditions, and type of twin pregnancy all contribute to prognosis.
Most children born after first-trimester vanishing twin syndrome develop normally without increased risk of developmental delays or health problems compared to singleton pregnancies.
Later losses present more variable outcomes, particularly in monochorionic twins where shared circulation complicates the picture. Some studies indicate higher rates of adverse neurodevelopmental outcomes in complicated monochorionic pregnancies.
Overall, the majority of surviving twins from vanishing twin syndrome are born healthy and reach normal developmental milestones.
Prevention: Is It Possible?
Real talk: vanishing twin syndrome cannot be prevented.
The chromosomal abnormalities and developmental issues that cause most early twin losses occur randomly and aren’t influenced by maternal behavior or medical interventions.
However, optimizing overall maternal health supports the best possible outcomes for any pregnancy:
- Prenatal vitamins with folic acid before conception
- Management of chronic health conditions
- Healthy weight maintenance
- Avoidance of alcohol, tobacco, and harmful substances
- Regular prenatal care starting early in pregnancy
According to ACOG recommendations for multiple pregnancies, low-impact exercise such as swimming, prenatal yoga, and walking (aiming for 30 minutes daily) supports healthy pregnancy, though providers may modify recommendations if problems arise.
These measures support overall pregnancy health but don’t specifically prevent vanishing twin syndrome.
Frequently Asked Questions
Yes, absolutely. Vanishing twin syndrome occurs when one embryo stops developing and is reabsorbed while the other continues growing normally. This happens in approximately 7-36% of twin pregnancies detected on early ultrasound, most commonly during the first trimester. The surviving twin typically continues developing without complications.
Not always. Many women experience no symptoms at all—the loss is discovered only during routine ultrasound. When symptoms do occur, they may include mild cramping, light bleeding, or spotting. However, these symptoms can also happen in normal twin pregnancies for other reasons, so ultrasound confirmation is necessary for diagnosis.
For first-trimester vanishing twin syndrome, the risk to the surviving baby remains minimal. The pregnancy typically continues normally as a singleton. However, if twin loss occurs later in the second or third trimester, particularly in monochorionic twins (those sharing a placenta), the surviving twin faces increased risks for complications including preterm birth and neurological issues.
In first-trimester losses, the embryonic tissue is typically reabsorbed by the mother’s body, the placenta, or the surviving twin—hence the term “vanishing.” This usually leaves little to no visible evidence by later ultrasounds. In rare cases of later pregnancy loss, the deceased twin may become a fetus papyraceus, a flattened, mummified fetus that remains until delivery.
For early first-trimester vanishing twin syndrome, no special treatment is typically needed. The pregnancy is managed as a normal singleton pregnancy with standard prenatal care and monitoring. Late-term single fetal demise requires specialized management in a tertiary care center with expertise in high-risk pregnancies and neonatal care.
Vanishing twin syndrome in one pregnancy doesn’t significantly increase the risk of complications in future pregnancies. Each pregnancy should be evaluated independently. However, if underlying factors like maternal age or health conditions contributed to the loss, those same factors may be relevant in subsequent pregnancies.
Detection rates are higher with IVF primarily because couples undergoing fertility treatments receive earlier and more frequent ultrasounds. Studies show approximately 7-36% of IVF twin pregnancies experience vanishing twin syndrome. The actual biological occurrence rate may be similar to natural conception, but IVF patients are more likely to have very early ultrasounds that detect pregnancies before natural loss occurs.
Moving Forward After Twin Loss
Discovering that one twin has been lost while the other continues developing creates a unique and challenging situation. The good news? Most surviving twins from first-trimester vanishing twin syndrome are born healthy without complications.
Understanding what causes twin loss, recognizing that it’s relatively common, and knowing what to expect helps parents navigate both the medical and emotional aspects of this experience.
If you’re experiencing or have experienced vanishing twin syndrome, maintain open communication with your healthcare provider. Ask questions, express concerns, and don’t hesitate to seek emotional support when needed.
The journey through pregnancy after losing one twin isn’t always straightforward, but with proper medical care and support, the vast majority of these pregnancies result in the birth of a healthy baby.
Work closely with your obstetric team, attend all scheduled appointments, and trust that your surviving baby is being carefully monitored. And remember—seeking counseling or joining support groups for pregnancy loss can provide valuable emotional support during this complex time.
