Quick Summary: Yes, it’s possible to be allergic to semen. Known as seminal plasma hypersensitivity (SPH), this rare but real condition occurs when someone develops an allergic reaction to specific proteins in seminal fluid. Symptoms range from localized burning and itching to severe systemic reactions, and the condition affects primarily women but can also occur in men allergic to their own semen.
The burning sensation after sex. The unexplained redness and swelling. The itching that starts minutes after intimacy and won’t quit.
Sound familiar? These symptoms often get dismissed as yeast infections, sexually transmitted infections, or simple irritation. But for some people, the culprit is something most medical professionals rarely consider: an actual allergy to semen.
Seminal plasma hypersensitivity is real, underdiagnosed, and more common than medical literature once suggested. Here’s what the research shows about this condition and what to do if these symptoms sound like yours.
What Is Seminal Plasma Hypersensitivity?
Seminal plasma hypersensitivity, often called semen allergy or human seminal plasma (HSP) hypersensitivity, is an allergic reaction to proteins found in seminal fluid. According to research published on PubMed, the major antigen is believed to be prostate-specific antigen (PSA), though other proteins are likely involved in this heterogeneous disorder.
This isn’t a psychological condition or a sensitivity to latex condoms. It’s a legitimate type I hypersensitivity reaction—the same immunological mechanism behind peanut allergies and bee sting reactions.
The condition primarily affects women, with estimates suggesting the condition may affect up to 40,000 women in the United States. But here’s where things get interesting: men can also be allergic to their own semen, experiencing what’s called post-orgasmic illness syndrome (POIS).
How Common Is Semen Allergy Really?
For years, medical texts labeled seminal plasma hypersensitivity as “extremely rare.” But emerging research challenges that assumption.
According to one analysis, among women reporting postcoital symptoms, approximately 12% could be classified as having probable SPH. That’s not rare at all—it suggests the condition is significantly underdiagnosed rather than genuinely uncommon.
The American Academy of Allergy, Asthma & Immunology notes that awareness among healthcare professionals remains limited, which means many cases get misdiagnosed as chronic vaginitis or recurrent yeast infections.
Recognizing the Symptoms of Semen Allergy
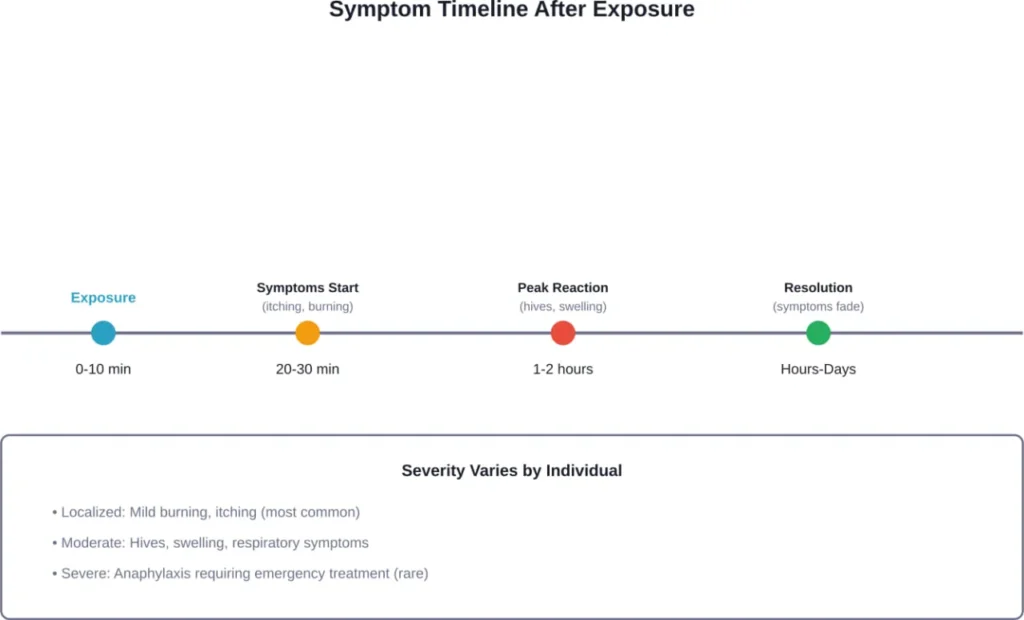
Symptoms typically appear within 20 to 30 minutes of exposure to seminal fluid. They can last anywhere from a few hours to several days, depending on severity.
Localized Reactions
Most people with seminal plasma hypersensitivity experience localized symptoms at the point of contact:
- Itching, redness, swelling, or burning of the vagina, vulva, or penis
- Hives or welts in the affected area
- Irritation of the mouth, throat, or eyes (depending on contact location)
- Pain during or after intercourse (dyspareunia)
These localized symptoms often get mistaken for other conditions, which delays proper diagnosis.
Systemic Reactions
Some individuals experience more severe, body-wide reactions:
- Widespread hives or skin reactions
- Swelling of lips, tongue, or throat
- Difficulty breathing or wheezing
- Dizziness or lightheadedness
- Diarrhea, nausea, or vomiting
- Anaphylactic shock (rare but life-threatening)
According to PubMed case reports, some patients have experienced recurrent anaphylaxis requiring emergency treatment. One 23-year-old woman with atopic dermatitis experienced three attacks of angioedema, urticaria, wheezing, and weakness after sexual contact.
Male-Specific Symptoms (Post-Orgasmic Illness Syndrome)
Men allergic to their own semen report a distinct symptom pattern. According to the American Academy of Allergy, Asthma & Immunology, symptoms typically begin within 30 minutes of ejaculation and include:
- Severe fatigue and flu-like state
- Nasal congestion
- Conjunctivitis and puffy eyes
- Intense warmth or sweating
- Irritability and anhedonia
These symptoms can persist for days, significantly impacting quality of life.
What Causes Semen Allergy?
The immune system mistakenly identifies proteins in seminal plasma as dangerous invaders. In response, it produces immunoglobulin E (IgE) antibodies that trigger the release of histamine and other chemicals, causing allergic symptoms.
Research published on PubMed has identified prostate-specific antigen as a primary allergen, but other seminal proteins are involved. Interestingly, one study documented IgE cross-reactivity between proteins from dog dander and human PSA, suggesting complex immunological relationships.
Risk Factors
Certain factors appear to increase susceptibility:
- Personal or family history of allergies (atopy)
- Other existing allergies, particularly drug allergies
- Hymenectomy or genital surgeries
- Autoimmune conditions
The condition can develop suddenly, even after years of symptom-free sexual contact with the same partner. It can also vary in severity between different partners, depending on the specific proteins in their seminal fluid.
Getting Diagnosed: Skin Prick Testing and Beyond
Diagnosis relies on thorough patient history combined with confirmatory testing. According to research from Mount Sinai’s Icahn School of Medicine, skin prick testing remains the gold standard for diagnosis.
The Diagnostic Process
A skin prick test uses a partner’s undiluted seminal plasma. Case reports describe positive skin prick test reactions with varying wheal diameters. In one documented case, the semen reaction measured 5 × 5 mm compared to 3 × 3 mm for the histamine control.
The procedure is straightforward:
- Collect fresh seminal sample (typically from the partner)
- Perform skin prick test on forearm or back
- Compare wheal response to positive control (histamine)
- Document reaction size and characteristics
Testing must be conducted by allergists or immunologists experienced with this condition. The use of IgE blood assays is controversial and less accurate, particularly for localized SPH.
Intravaginal Graded Challenge
For some patients, intravaginal graded challenge provides the most definitive diagnosis. This controlled exposure test measures reactions to increasing concentrations of seminal fluid under medical supervision.
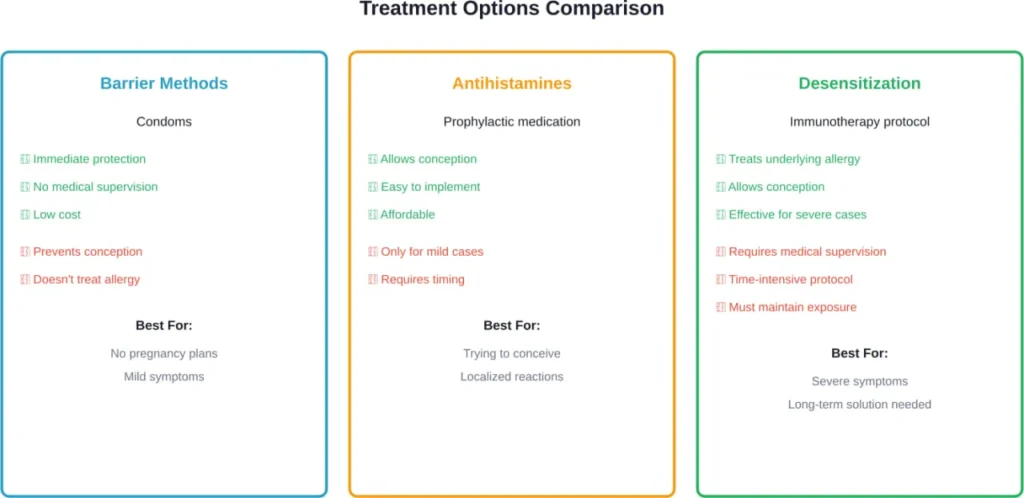
Treatment Options: From Condoms to Desensitization
Treatment varies based on symptom severity, future pregnancy plans, and personal preferences.
Avoidance and Barrier Methods
The simplest approach is using condoms consistently to prevent exposure. This works well for individuals who don’t plan to conceive and have mild to moderate reactions.
Antihistamine Prophylaxis
According to a case report published in Asia Pacific Allergy, one woman achieved successful pregnancy after prophylactic antihistamine treatment. She took antihistamines before intercourse, which prevented or reduced allergic symptoms enough to conceive naturally.
This approach may be helpful for localized, mild reactions.
Intravaginal Desensitization
For severe cases or when pregnancy is desired, intravaginal desensitization (a form of immunotherapy) remains the mainstay treatment. This protocol involves:
- Starting with highly diluted seminal plasma
- Gradually increasing concentration over time
- Maintaining regular exposure to sustain tolerance
Case reports demonstrate this method can be effective when properly maintained, though it requires strict adherence. According to PubMed research, the treatment “remains a mainstay in treatment, but is only effective if maintained correctly.”
One case study described successful pregnancy following intravaginal rush desensitization in a 29-year-old woman with documented seminal fluid allergy.
Emergency Medications
Anyone with systemic reactions should carry epinephrine auto-injectors. Anaphylaxis, though rare, can be life-threatening and requires immediate treatment.
Semen Allergy and Fertility: Can You Still Get Pregnant?
One of the biggest concerns for people diagnosed with seminal plasma hypersensitivity is whether conception is still possible. The answer is yes, but it requires planning.
Several approaches enable pregnancy:
- Antihistamine prophylaxis: Taking antihistamines before intercourse during fertile windows
- Intravaginal desensitization: Building tolerance before attempting conception
- Intrauterine insemination (IUI): Sperm washing removes seminal plasma proteins, leaving only sperm cells for artificial insemination
- In vitro fertilization (IVF): Bypasses exposure to seminal fluid entirely
Multiple case reports document successful pregnancies using these methods. Case reports document successful pregnancies following intravaginal desensitization protocols and prophylactic antihistamine treatment.
Living With Seminal Plasma Hypersensitivity
This condition requires ongoing management, but it doesn’t mean the end of sexual intimacy or reproductive possibilities.
Key considerations include:
- Working with an allergist experienced in SPH
- Communicating openly with partners about symptoms and limitations
- Keeping emergency medications accessible if reactions are severe
- Planning conception attempts with medical guidance
- Maintaining desensitization protocols if pursuing immunotherapy
The psychological impact shouldn’t be underestimated. Community discussions reveal that many people feel isolated or dismissed when they first report symptoms. Finding knowledgeable healthcare providers makes a significant difference.
Frequently Asked Questions
Yes. Seminal plasma hypersensitivity can develop at any time, even after years of symptom-free sexual activity with the same partner. The immune system can begin producing IgE antibodies to seminal proteins without warning, triggered by mechanisms not yet fully understood.
Absolutely. This condition is called post-orgasmic illness syndrome (POIS). According to the American Academy of Allergy, Asthma & Immunology, affected men experience flu-like symptoms, severe fatigue, nasal congestion, and other systemic reactions within 30 minutes of ejaculation. Skin prick testing with extremely diluted autologous semen can confirm the diagnosis.
Timing and pattern matter. Semen allergy symptoms appear consistently within 20-30 minutes after every exposure to seminal fluid and resolve within hours to days. STI symptoms typically develop days to weeks after exposure, persist without treatment, and don’t follow the immediate post-contact pattern. When in doubt, get tested for STIs and see an allergist for proper evaluation.
Unlikely. Seminal plasma hypersensitivity is a true allergic condition involving IgE antibodies. Without treatment, symptoms typically persist or worsen with continued exposure. Desensitization therapy can build tolerance, but this requires active treatment and maintenance—it doesn’t happen spontaneously.
Yes. Seminal plasma composition varies between individuals. Someone might react to specific proteins present in one partner’s semen but not another’s. Severity can also vary between partners. If symptoms disappear with a new partner, this doesn’t mean the allergy has resolved—it means that particular person’s seminal proteins don’t trigger the reaction.
Not reliably. Allergic reactions begin within minutes of exposure as the immune system responds to proteins. Washing afterward may reduce symptom duration by removing residual seminal fluid, but it won’t prevent the initial reaction. Barrier methods that prevent contact in the first place are the only way to avoid reactions entirely.
No, these are completely different conditions. Latex allergy involves reactions to rubber proteins in condoms, gloves, and other latex products. Seminal plasma hypersensitivity is a reaction to proteins in seminal fluid itself. Someone can have one, both, or neither. If symptoms improve with condom use, that suggests semen allergy rather than latex allergy.
When to See a Doctor
Seek medical evaluation if experiencing consistent burning, itching, swelling, or systemic symptoms after sexual contact. Don’t accept dismissive responses—request referral to an allergist or immunologist if primary care providers aren’t familiar with seminal plasma hypersensitivity.
Seek emergency care immediately for difficulty breathing, widespread hives, throat swelling, or signs of anaphylaxis.
The Bottom Line
Semen allergy is real, increasingly recognized, and more common than previously thought. The condition ranges from mildly uncomfortable localized reactions to life-threatening anaphylaxis.
But here’s the good news: effective diagnostic tools exist, multiple treatment options are available, and pregnancy remains possible with proper management.
If these symptoms sound familiar, don’t suffer in silence or accept misdiagnosis. Find an allergist who understands seminal plasma hypersensitivity. Proper diagnosis and treatment can restore quality of life and make family planning achievable.
This isn’t something to ignore or feel embarrassed about. It’s a legitimate medical condition that deserves proper attention and care.
