Quick Summary: Yes, it is medically possible to have both penis-like and vaginal tissue, a condition known as intersex or differences of sex development (DSD). According to medical research, approximately 1-2% of people are born with intersex traits where reproductive anatomy doesn’t fit typical male or female patterns. These variations occur naturally during fetal development and involve chromosomes, hormones, gonads, or genitalia.
The question of whether someone can have both a penis and a vagina touches on a medically recognized reality that many people don’t learn about until they encounter it directly. The simple answer is yes, though the specifics are more nuanced than most expect.
According to Cleveland Clinic, an estimated 1 in 100 Americans is intersex, with around 2% of people worldwide having intersex traits. That makes intersex variations more common than having red hair or identical twins.
But what does this actually look like in practice? And what causes these variations?
What Does Intersex Mean?
Intersex is an umbrella term for people born with reproductive or sexual anatomy that doesn’t fit typical definitions of male or female. According to MedlinePlus, differences of sex development (DSD) involve a discrepancy between external genitals (penis, scrotum, vulva, labia) and internal genitals (testes, vagina, ovaries).
The National Institutes of Health notes that most people with intersex traits are born with genitals that appear to be male or female and are therefore assigned either male or female at birth. Often, they aren’t identified as having an intersex variation until later in life—sometimes in adolescence or adulthood, if at all.
Here’s the thing though—intersex isn’t one single condition. It encompasses dozens of different variations involving chromosomes, hormones, gonads, or genital development.
Understanding the Spectrum of Variations
Some intersex people have what appears to be a penis but also have internal structures associated with female anatomy, like a uterus or ovaries. Others may have external genitalia that appears more ambiguous, with features of both typical male and female anatomy.
According to research published in StatPearls, a newborn with bilateral non-palpable testes or a unilateral impalpable testis and severe hypospadias should be regarded as having a DSD until proven otherwise, whether or not the genitalia appears ambiguous.
The variations are highly heterogeneous and can involve any sex trait.
How Common Is Having Both Penis and Vaginal Tissue?
WebMD reports that it’s estimated 1% to 2% of the population has intersex traits. That makes it more common than having red hair.
Now, not all intersex people have what would be described as both a penis and a vagina. According to interACT, about 1 in 2,000 babies (0.05% of humans) are born with genital differences that a doctor might suggest changing with unnecessary surgery.
Research published in PMC references Sax’s (2010) prevalence statistic of 0.018 percent as a more conservative estimate that corrects earlier statistics of around 1.7 percent.
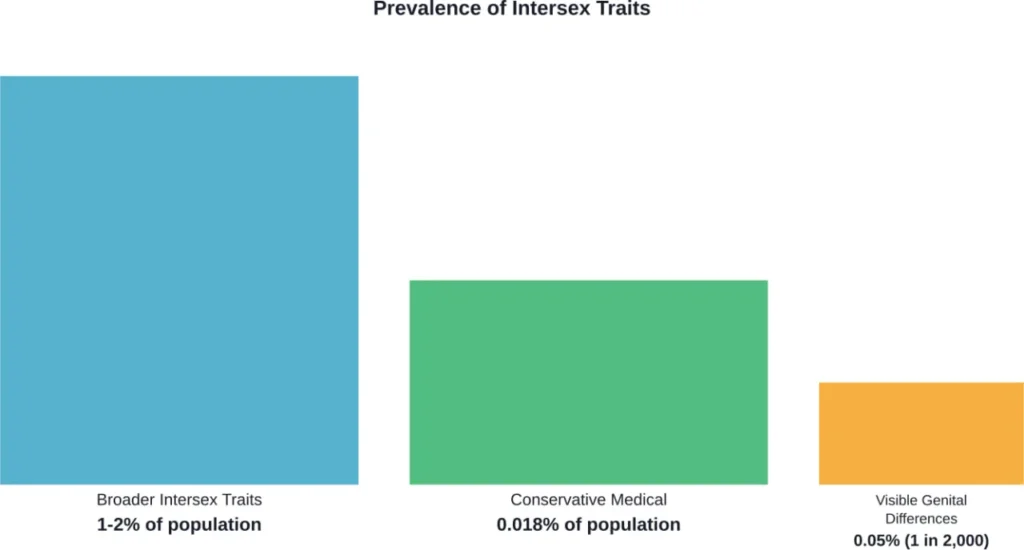
The discrepancy between these numbers comes down to definitions. Broader definitions include anyone with chromosomal, hormonal, or gonadal variations. Narrower definitions focus specifically on ambiguous external genitalia visible at birth.
What Causes Someone to Be Born with Both Penis and Vaginal Tissue?
According to Cleveland Clinic, experts don’t know exactly what causes being intersex in all cases. What they do understand is the developmental process and where it can vary.
During typical fetal development, sex differentiation occurs in stages. Phenotypic sex results from the differentiation of internal ducts and external genitalia under the influence of hormones and other factors.
When discordance occurs among the three processes—chromosomal, gonadal, and phenotypic sex determination—a DSD results, according to research in StatPearls.
Congenital Adrenal Hyperplasia
Congenital adrenal hyperplasia (CAH) is the most common cause of intersex variations, though the source material does not specify that “over 80%” of intersex cases are CAH. Approximately 95% of CAH cases are caused by a 21-hydroxylase deficiency, a mutation in the gene that codes for the enzyme 21-OH.
A deficiency in 21-OH can result in the overproduction of androgens, which can cause virilization of external genitalia in individuals with XX chromosomes.
Androgen Insensitivity Syndrome
Another common cause involves androgen insensitivity. According to interACT, people with Complete Androgen Insensitivity have XY chromosomes, a vulva and clitoris externally, but testes internally with no uterus and sometimes a partial or complete vagina.
This occurs when cells don’t respond to androgens during development despite the presence of testes and testosterone production.
Environmental Factors
Research published in Environmental Health Insights suggests that exposure to endocrine-disrupting chemicals (EDCs) in the environment may contribute to increased incidence of intersex variations. These chemicals can interfere with hormonal signaling during critical developmental windows.
That said, the majority of intersex variations have genetic or spontaneous developmental origins rather than environmental causes.
What Do Different Intersex Conditions Look Like?
The physical presentation of intersex traits varies enormously. Some people have what appears to be typical male anatomy externally but have ovaries or a uterus internally. Others have ambiguous external genitalia with a structure that resembles both a small penis and a vaginal opening.
MedlinePlus explains that these conditions involve discrepancies between external and internal genitals. The external appearance might not match chromosomes or internal reproductive structures.
| Condition | Chromosomes | External Features | Internal Features |
|---|---|---|---|
| Complete Androgen Insensitivity | XY | Vulva, clitoris | Testes, no uterus, vagina (partial or complete) |
| Congenital Adrenal Hyperplasia | XX | Virilized genitalia | Ovaries, uterus |
| Partial Androgen Insensitivity | XY | Ambiguous genitalia | Testes, may have partial internal structures |
| Ovotesticular DSD | Variable | Ambiguous genitalia | Both ovarian and testicular tissue |
Real talk: most intersex people look completely typical externally. The variations might only become apparent through genetic testing, imaging, or when expected puberty changes don’t occur.
Medical Perspectives on Intersex Surgery
Historically, doctors recommended surgery on infants with ambiguous genitalia to make their anatomy appear more typically male or female. This approach has become increasingly controversial.
According to research cited in Healthcare literature, approximately 50% of intersex/DSD people abandoned health services due to disappointment and frustration with the results of surgeries and attention received.
Cleveland Clinic notes that most intersex people are healthy and surgery isn’t necessary from a medical standpoint.
The Shift Away from Early Surgery
Many medical organizations now recommend delaying cosmetic genital surgery until the person is old enough to participate in the decision. One major reason is that people may decide later that they were given the wrong gender and want sexual organs different from those their parents and doctors chose.
Stanford Medicine emphasizes that more attention needs to be paid to intersex individuals as complete people, rather than as specimens of unusual biology. The focus should be on what contributes to the flourishing of human beings in general.

Living with Intersex Traits
Being intersex affects different people in different ways. According to Cleveland Clinic, intersex variations may affect genitals, chromosomes, hormones, reproductive systems, or gonads.
But here’s what matters most: most intersex babies are healthy. The variations in their anatomy don’t inherently cause medical problems, though some underlying conditions (like certain forms of CAH) may require medical management.
Can Intersex People Have Children?
Fertility varies enormously depending on the specific intersex variation. Some intersex people have functional reproductive systems and can conceive or father children. Others may have reduced fertility or be infertile.
The presence of both penis-like tissue and vaginal tissue doesn’t automatically determine fertility. What matters more is whether functional reproductive organs (ovaries, testes, uterus) are present and whether hormone levels support reproductive function.
Psychological and Social Considerations
Research published in Healthcare notes that intersex conditions are divergences among genitalia, gonads, and chromosome patterns that have been present for millennia and socially defined according to established cultural systems.
Many intersex individuals face unique psychological challenges related to medical interventions, social stigma, and identity development. Stanford Medicine’s research emphasizes the struggles intersex individuals, their families, and doctors face when navigating these complex situations.
The shock of learning a baby’s sex cannot be immediately determined creates significant stress for families. As one researcher noted, few things are harder for new parents than hearing their doctor say “I don’t know” when asked if the baby is a boy or girl.
Recognizing Intersex Variations
How do people discover they have intersex traits? The timing varies widely.
Some intersex variations are visible at birth. Medical staff might notice ambiguous genitalia immediately, prompting genetic testing and hormone evaluations.
Others aren’t discovered until puberty, when expected changes don’t occur. A person assigned female at birth might not menstruate, or a person assigned male might develop breast tissue.
Still others never know they have intersex traits unless they undergo genetic testing for unrelated reasons or fertility evaluations reveal unexpected anatomy or chromosomes.
Diagnostic Process
According to StatPearls, detailed understanding of embryology and anatomy is crucial for determining the correct approach when intersex conditions are suspected.
Diagnostic evaluation typically includes:
- Physical examination of external genitalia
- Pelvic ultrasound or MRI to visualize internal structures
- Chromosomal analysis (karyotype testing)
- Hormone level testing
- Genetic testing for specific conditions
The NIH notes that measurement of intersex status is complicated by the unique experiences of intersex populations and a limited research base. Intersex variations are highly heterogeneous and can involve any sex trait.
Modern Terminology and Understanding
The language around these conditions has evolved. “Intersex” is increasingly preferred by advocacy organizations and many individuals, while “differences of sex development” or DSD remains common in medical contexts.
MedlinePlus notes that intersex is an older term for DSD, though many in the community prefer “intersex” because it centers the lived experience rather than framing the variation as a disorder.
Understanding this terminology matters because it reflects broader shifts in how society views sex, gender, and bodily diversity.
Frequently Asked Questions
In rare cases, individuals may have tissue from both types of external genitalia, though typically not both fully developed and functional. Most intersex variations involve ambiguous genitalia or a mismatch between external and internal anatomy rather than two complete, functional reproductive systems.
Historically, doctors made assignment decisions based on the appearance of external genitalia and which surgical outcome seemed most achievable. Modern practice increasingly involves genetic testing, hormone evaluations, and input from specialized teams. Many experts now recommend delaying irreversible decisions until the child can participate.
No. Intersex refers to biological variations in sex characteristics present from birth. Transgender refers to gender identity—when someone’s internal sense of gender differs from the sex assigned at birth. Some intersex people are transgender, but most are not. These are distinct experiences that sometimes overlap.
Not necessarily. According to NIH research, most people with intersex traits are born with genitals that appear typically male or female and may never know they have intersex variations unless specific testing reveals it. Some discover their status during puberty, while others never find out.
Yes, though the practice is declining. According to available data, 1 in 2,000 babies are born with genital differences that doctors might suggest changing with surgery. However, growing evidence shows these surgeries often cause harm, and many medical organizations now recommend waiting until the person can consent.
Sexual function varies depending on the specific intersex variation and any medical interventions performed. Many intersex people have completely typical sexual function. Complications are more likely when surgeries were performed in infancy, which is one reason patient advocates oppose early intervention.
Connect with a multidisciplinary team experienced in DSD management, including endocrinologists, geneticists, urologists, and mental health professionals. Research current best practices, which emphasize avoiding irreversible surgeries until the child can participate in decisions. Seek support from intersex advocacy organizations that can provide community connections and resources.
Moving Forward with Understanding
The question of whether someone can have both a penis and a vagina opens up broader conversations about human diversity and medical ethics.
What’s clear from the research is that intersex variations are far more common than most people realize. With 1-2% of the population affected in some way, intersex traits represent a natural part of human biological diversity.
The medical community has made significant strides in understanding these variations, though gaps remain. Research continues to expand knowledge about causes, prevalence, and best practices for supporting intersex individuals.
For intersex individuals and their families, access to accurate information, specialized medical care, and supportive communities makes an enormous difference. Organizations like interACT provide resources, advocacy, and connections for young intersex people and their families.
The broader cultural conversation is shifting too. As awareness grows, more people recognize that sex isn’t strictly binary, that bodies come in infinite variations, and that these differences don’t determine someone’s worth or potential.
If you’re intersex or think you might be, know that you’re not alone. Communities exist to provide support, information, and advocacy. If you’re a parent or family member, specialized medical teams and advocacy organizations can help navigate the complex medical and social landscape.
Understanding intersex variations isn’t just about anatomy—it’s about recognizing the full spectrum of human diversity and ensuring that everyone, regardless of how their body developed, receives respectful, informed, and supportive care.
