Quick Summary: No, you cannot physically cough up an entire lung—your windpipe is far too narrow for lung tissue to pass through. However, rare medical cases document people expectorating lung tissue fragments, blood clots shaped like airways, or bronchial casts. While extreme coughing can cause rib fractures or diaphragm rupture, actually expelling a whole lung remains anatomically impossible.
After a brutal coughing fit, most people have joked about “coughing up a lung.” But could it actually happen?
The short answer is no. Your anatomy makes it physically impossible to expel an entire lung through your throat. But here’s where things get interesting—you can cough out pieces of lung tissue, blood clots that perfectly match your airway shape, and thick casts that look disturbingly organic.
Let’s examine what medical science actually documents about this phenomenon.
Why You Can’t Physically Cough Up an Entire Lung
Your trachea (windpipe) measures roughly 2.5 centimeters in diameter. Your lungs? Each one measures about 25 centimeters long and weighs approximately 450 grams.
The math doesn’t work. There’s simply no way for an organ that large to pass through such a narrow passage. Think of trying to push a basketball through a garden hose—it’s anatomically impossible.
But that’s not the whole story.
What You Can Actually Cough Out: Documented Medical Cases
While expelling an entire lung remains impossible, medical literature documents several shocking cases of people coughing out substantial biological material.
The 2012 Lung Tissue Case
According to a case published in the New England Journal of Medicine, a 40-year-old woman with asthma arrived at Good Hope Hospital in Birmingham, United Kingdom, after two days of severe chest pain. She’d been coughing intensely.
What she expectorated shocked her physicians: actual lung tissue. Not mucus shaped like tissue—genuine pieces of her lung.
How does this happen? In extremely rare circumstances, violent coughing combined with underlying lung disease can tear small fragments of damaged tissue loose from the airways.
Plastic Bronchitis: Coughing Out Airway Casts
Plastic bronchitis represents one of the most visually disturbing things people can expel from their lungs. This condition causes thick, fibrous material to form inside airways, creating perfect casts of the bronchial tree.
According to NIH research on pulmonary hemorrhage, these casts can emerge intact during severe coughing episodes. Patients literally cough out structures that match the exact branching pattern of their airways—complete with all the splits and divisions.
The condition affects some cystic fibrosis patients and those with certain congenital heart defects. According to medical literature, cystic fibrosis patients can develop plastic bronchitis and other complications severe enough to produce bronchial casts.
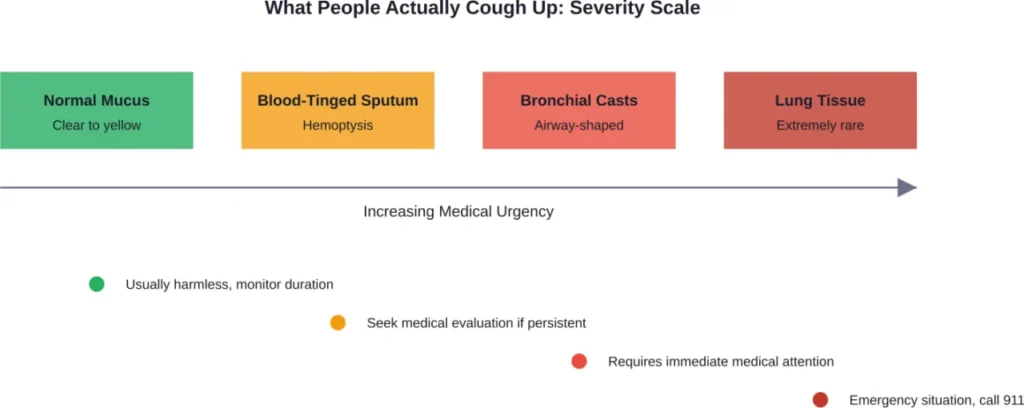
Hemoptysis: Coughing Up Blood
According to research published in Deutsches Ärzteblatt International, hemoptysis has an annual incidence of approximately 0.1% in ambulatory patients and 0.2% in inpatients.
NIH clinical research defines hemoptysis as the expectoration of blood or blood-tinged sputum from the lungs or tracheobronchial tree. The blood originates from the lower respiratory tract, below the vocal cords.
In fewer than 5% of cases, hemoptysis becomes massive, representing a life-threatening emergency. According to NIH research, this can lead to hemodynamic instability and potentially fatal outcomes due to suffocation or shock.
Blood in sputum appears bright red and frothy when fresh. People sometimes cough up blood clots that have formed inside airways, creating disturbing shapes that mirror the branching structure of bronchi.
Real Injuries from Severe Coughing
While you can’t expel an entire lung, violent coughing absolutely causes physical damage. These injuries are well-documented in medical literature.
Rib Fractures
Medical literature, including research cited in clinical studies, documents cases of cough-induced rib fractures. The violent muscular contractions during severe coughing fits can literally crack ribs, particularly in people with osteoporosis or other bone-weakening conditions.
The pain from fractured ribs then makes breathing more difficult, creating a vicious cycle where the patient needs to cough but can’t without excruciating pain.
Diaphragm Rupture and Abdominal Herniation
In extreme cases documented by medical researchers, severe coughing has ruptured the diaphragm—the muscle separating your chest from your abdomen. This same case study documented abdominal herniation, where abdominal contents pushed through the tear.
These represent rare but serious complications requiring surgical intervention.
Pneumothorax: Collapsed Lung
Intense coughing can rupture small air sacs in the lungs, allowing air to leak into the chest cavity. This condition, called pneumothorax, causes the lung to collapse partially or completely.
According to NIH research, pneumothorax requires immediate medical attention and sometimes emergency chest tube placement to re-expand the lung.
| Injury Type | Mechanism | Risk Factors | Treatment Required |
|---|---|---|---|
| Rib Fractures | Muscle force during coughing | Osteoporosis, age, steroid use | Pain management, rest |
| Diaphragm Rupture | Extreme pressure differential | Pre-existing weakness, trauma | Surgical repair |
| Pneumothorax | Air sac rupture | COPD, asthma, smoking | Chest tube, observation |
| Hemoptysis | Blood vessel damage | Lung disease, infection, cancer | Varies by severity and cause |
Medical Conditions That Cause Severe Coughing
Several respiratory conditions trigger the kind of violent coughing that might make someone feel like they’re expelling internal organs.
Chronic Obstructive Pulmonary Disease (COPD)
COPD causes chronic inflammation and mucus production. Patients develop what medical professionals call a “productive cough”—one that brings up phlegm and mucus from congested airways.
The American Lung Association notes that worsening COPD symptoms often involve increased coughing with thicker, more abundant phlegm production.
Bronchiectasis
This condition permanently damages and widens airways, creating pockets where mucus accumulates. According to NIH research, bronchiectasis frequently causes hemoptysis and represents one of the leading conditions associated with coughing up blood.
Lung Cancer
Research published in Annals of Translational Medicine indicates that approximately 20% of lung cancer patients experience hemoptysis during their disease course. Hemoptysis related to malignancy accounts for nearly a quarter of all hemoptysis cases in the United States.
Tuberculosis and Aspergilloma
According to NIH clinical data, tuberculosis and fungal infections like aspergilloma commonly cause hemoptysis. The aspergilloma “fungus ball” moves within lung cavities, causing local friction, triggering blood vessel proliferation, and releasing enzymes that contribute to bleeding.

When to See a Doctor About Your Cough
The American Lung Association emphasizes that while occasional coughs are normal protective reflexes, certain symptoms warrant medical evaluation.
Seek immediate medical attention if experiencing:
- Any amount of blood in sputum or phlegm
- Coughs lasting more than three weeks
- Severe chest pain during coughing episodes
- Difficulty breathing or shortness of breath
- High fever accompanying the cough
- Unexplained weight loss
- Night sweats
According to NIH research, hemoptysis must always be considered serious and potentially life-threatening, regardless of the amount of blood produced.
The Reality Behind the Expression
So where did “coughing up a lung” come from if it’s anatomically impossible?
The phrase captures the feeling of severe respiratory distress. When people cough violently and repeatedly, particularly with conditions like pneumonia or bronchitis, the sensation feels like internal organs might actually dislodge.
That feeling has some basis in reality. As we’ve seen, severe coughing does cause tangible physical damage—broken ribs, torn muscles, ruptured blood vessels. The expression uses hyperbole to communicate genuine distress.
But the documented cases of people expectorating lung tissue fragments or bronchial casts prove the expression isn’t entirely fictional. While you can’t cough out an entire lung, you can expel disturbing pieces of respiratory anatomy under extreme circumstances.
Frequently Asked Questions
Coughing itself rarely causes permanent lung damage in healthy individuals. However, the underlying conditions causing severe coughing—like COPD, bronchiectasis, or tuberculosis—can permanently damage lung tissue. Additionally, complications like pneumothorax or diaphragm rupture from extreme coughing require medical intervention to prevent lasting harm.
Coughing up blood clots indicates hemoptysis and requires immediate medical evaluation. According to NIH research, blood clots from the respiratory tract suggest bleeding from airways or lung tissue. Potential causes include lung cancer, tuberculosis, bronchiectasis, or fungal infections. The amount and frequency help determine urgency, but any hemoptysis warrants professional assessment.
Yes. Medical literature documents numerous cases of cough-induced rib fractures. The violent muscular contractions during severe coughing episodes generate enough force to crack ribs, particularly in people with osteoporosis, advanced age, or those taking corticosteroids long-term. The fractures typically occur in the lower ribs where leverage is greatest.
Bronchial casts are thick, fibrous formations that develop inside airways and take the exact shape of the bronchial tree. Made from mucus, fibrin, and cellular material, they branch and divide just like airways do. When expelled during coughing, they appear disturbingly organic. The condition called plastic bronchitis causes these formations, affecting some cystic fibrosis patients and those with certain heart conditions.
According to medical research, any hemoptysis deserves medical attention, but massive hemoptysis—generally defined as more than 100-600 mL in 24 hours—represents a life-threatening emergency. Even small amounts of persistent blood-tinged sputum require evaluation, as they may indicate serious underlying conditions like lung cancer, tuberculosis, or bronchiectasis.
While extremely rare, the documented 2012 case involved a woman with asthma who coughed up actual lung tissue after severe coughing episodes. This represents an extraordinarily unusual complication. Standard asthma typically causes coughing with mucus production, wheezing, and chest tightness—not tissue expectoration. Such extreme cases involve multiple complicating factors beyond asthma alone.
Seek emergency medical care immediately. Whether it’s actual tissue, a bronchial cast, or a large blood clot, expectorating solid material from your lungs indicates a serious medical situation requiring urgent evaluation. If possible, preserve what was coughed up for medical examination, as this helps physicians diagnose the underlying condition accurately.
Conclusion
The human body has anatomical limits that make coughing up an entire lung impossible. Your trachea simply won’t accommodate an organ that large.
But medical reality proves more nuanced than simple impossibility. People have coughed up lung tissue fragments, bronchial casts that perfectly mirror airway anatomy, and blood clots from deep within respiratory structures. Severe coughing breaks ribs, ruptures diaphragms, and collapses lungs.
The next time someone says they almost “coughed up a lung,” they’re probably exaggerating—but not by as much as you’d think.
If experiencing persistent coughing, blood in sputum, or any concerning respiratory symptoms, consult a healthcare provider immediately. Early evaluation of hemoptysis and severe cough can identify serious conditions when they’re most treatable.
