Quick Summary: Taking too much vitamin D can lead to vitamin D toxicity (hypervitaminosis D), a rare but serious condition caused by excessive supplementation. Symptoms include nausea, vomiting, weakness, and dangerously high blood calcium levels (hypercalcemia), which can damage kidneys, bones, and the heart. Most cases occur from taking extremely high doses of supplements—typically over 60,000 IU daily for extended periods—not from diet or sun exposure.
Vitamin D has earned a reputation as the sunshine vitamin, essential for bone health, immune function, and overall wellness. But here’s the thing: more isn’t always better.
While vitamin D deficiency affects millions worldwide, the opposite problem—vitamin D toxicity—poses serious health risks. And it’s entirely preventable.
Most people can’t get too much vitamin D from sunlight or food. The real danger comes from supplements, particularly when taken in excessive doses without medical supervision. Understanding the risks can help you harness vitamin D’s benefits without crossing into dangerous territory.
What Is Vitamin D Toxicity?
Vitamin D toxicity, also called hypervitaminosis D, occurs when vitamin D levels in the blood become dangerously elevated. This condition is rare but potentially serious.
The body needs vitamin D to absorb calcium and maintain strong bones. According to the CDC, children need vitamin D beginning shortly after birth to support healthy bone development and prevent rickets. But excessive amounts disrupt this delicate balance.
Here’s what makes vitamin D different from water-soluble vitamins: it’s fat-soluble. That means excess amounts get stored in body fat and liver tissue rather than being excreted through urine. Over time, these stores can build to toxic levels.
According to research published by the National Institutes of Health, vitamin D toxicity typically requires prolonged intake of very high doses—usually far exceeding 10,000 IU daily. You can’t get toxic levels from sun exposure because the body regulates vitamin D production in skin naturally.
How Much Vitamin D Is Too Much?
Recommended vitamin D intake varies by age and life stage. The Office of Dietary Supplements provides these daily guidelines:
| Life Stage | Recommended Amount | Upper Limit |
|---|---|---|
| Birth to 12 months | 10 mcg (400 IU) | 25-38 mcg (1,000-1,500 IU) |
| Children 1-13 years | 15 mcg (600 IU) | 63-75 mcg (2,500-3,000 IU) |
| Teens 14-18 years | 15 mcg (600 IU) | 100 mcg (4,000 IU) |
| Adults 19-70 years | 15 mcg (600 IU) | 100 mcg (4,000 IU) |
| Adults 71+ years | 20 mcg (800 IU) | 100 mcg (4,000 IU) |
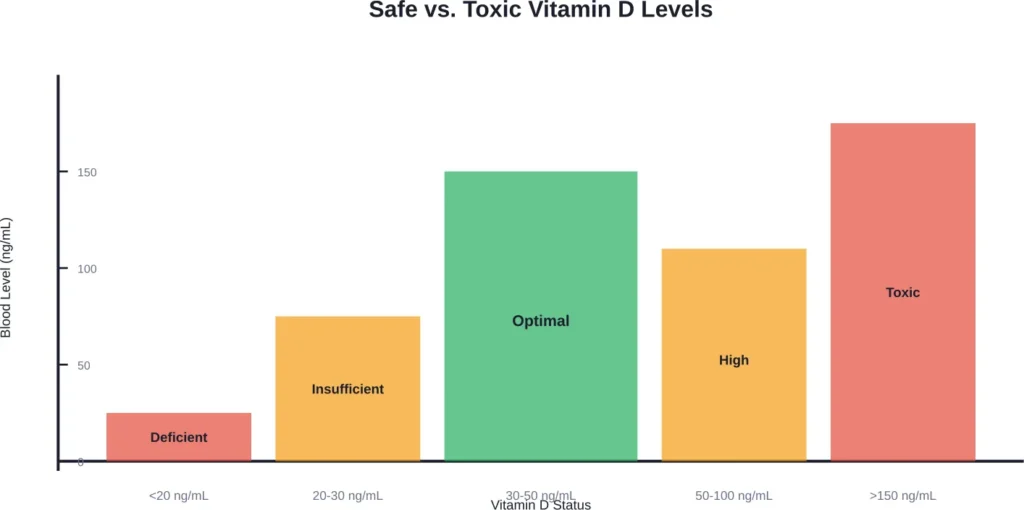
The upper limit represents the maximum daily intake unlikely to cause harm. But toxicity typically requires much higher doses sustained over weeks or months.
Research from PMC indicates that clinical vitamin D toxicity usually involves blood levels exceeding 150 ng/mL (375 nmol/L). A study by Bischoff-Ferrari reported higher risk of falls at 60,000 IU/month (not daily), with serum 25(OH)D concentrations reaching 40 ng/mL in the affected group.
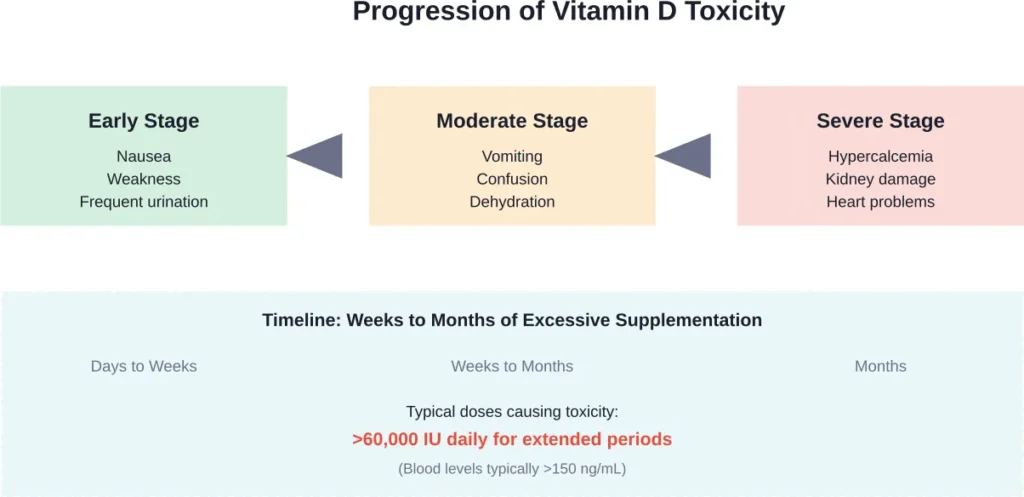
Symptoms of Vitamin D Toxicity
According to NIH research, confusion, apathy, recurrent vomiting, abdominal pain, polyuria, polydipsia, and dehydration are the most commonly noted clinical symptoms of vitamin D toxicity.
Early warning signs include:
- Nausea and vomiting
- Weakness and fatigue
- Frequent urination
- Excessive thirst
- Loss of appetite
- Constipation
As toxicity progresses, more severe symptoms develop. Muscle pain and weakness were prominent symptoms of vitamin D deficiency in studies. The blog does not cite evidence that excessive vitamin D specifically causes similar neuromuscular symptoms.
The most dangerous consequence? Hypercalcemia—dangerously elevated blood calcium levels.
What Is Hypercalcemia and Why Is It Dangerous?
Hypercalcemia—elevated calcium in the bloodstream—represents the primary mechanism behind vitamin D toxicity’s dangerous effects.
According to the Endocrine Society research, hypercalcemia occurs in up to 4% of the population in association with malignancy, primary hyperparathyroidism, ingestion of excessive calcium and vitamin D, ectopic production of metabolically active vitamin D, and impaired vitamin D degradation.
When vitamin D levels spike, the body absorbs far more calcium from food than needed. This excess calcium accumulates in the blood, creating a cascade of problems:
- Kidney damage: Calcium deposits can form in kidney tissue, impairing function and potentially causing kidney stones or irreversible damage
- Bone problems: Paradoxically, excessive vitamin D can weaken bones by disrupting normal bone remodeling
- Heart issues: Calcium buildup in blood vessels and heart tissue can affect heart rhythm and cardiovascular function
- Digestive distress: High calcium levels interfere with digestive system function
Blood calcium levels above 10.5 mg/dL generally indicate hypercalcemia, though symptoms typically become severe above 12 mg/dL.
Common Causes of Vitamin D Toxicity
Vitamin D toxicity almost always results from supplement misuse. Natural sources simply can’t deliver toxic doses.
A case study published in BMJ Case Reports documented a patient who experienced severe hypercalcemia after taking 150,000 IU of vitamin D daily (daily requirement: 10 mcg or 400 IU per day)—approximately 375 times the recommended daily amount—for nearly three months on advice from a private nutritionist.
Common scenarios leading to toxicity include:
- Taking prescription-strength vitamin D without proper medical monitoring
- Combining multiple supplements that all contain vitamin D
- Mistaking dosage instructions (confusing IU with mcg)
- Following unqualified health advice from non-medical sources
- Taking mega-doses based on misunderstood research
Research indicates that a study by Bischoff-Ferrari reported higher risk of falls in men and women older than 70 years who received 60,000 IU/month than control groups receiving 24,000 IU/month ± 300 μg of 25(OH)D3/month over 1 year, with serum 25(OH)D concentrations reaching 40 ng/mL (100 nmol/l) in the affected group.
Food sources of vitamin D are safe. According to Oregon State University research, salmon provides about 11.1 mcg per 3-ounce serving, while canned tuna offers 1.7 mcg per 5 ounces—amounts that support health without risk of toxicity.
Who Is at Higher Risk?
Certain groups face elevated risk for vitamin D-related complications:
| Risk Group | Why They’re Vulnerable |
|---|---|
| Older adults | Reduced kidney function affects vitamin D metabolism |
| People with kidney disease | Impaired ability to regulate calcium and vitamin D |
| Those taking certain medications | Some drugs interact with vitamin D metabolism |
| People with granulomatous disorders | Conditions like sarcoidosis increase vitamin D activation |
| Infants | Small body size means lower tolerance for excess |
According to the CDC, breast milk alone doesn’t provide infants with adequate vitamin D, so supplementation is necessary. But the line between sufficient and excessive is narrower for babies than adults.
Diagnosis and Testing
Healthcare providers diagnose vitamin D toxicity through blood tests measuring vitamin D and calcium levels.
The key marker is serum 25-hydroxyvitamin D [25(OH)D], the form circulating in blood. Levels above 150 ng/mL (375 nmol/L) typically indicate toxicity, though symptoms may appear at lower concentrations in susceptible individuals.
Additional tests check for:
- Calcium levels (serum calcium)
- Kidney function (creatinine, BUN)
- Parathyroid hormone (PTH)
- Phosphate levels
Medical history focusing on supplement use is critical. Many patients don’t mention supplements to doctors, assuming they’re too benign to matter.
Treatment and Recovery
Treatment for vitamin D toxicity focuses on reducing calcium levels and eliminating excess vitamin D from the body.
Immediate steps include:
- Stopping all vitamin D supplementation
- Limiting dietary calcium intake
- Increasing fluid intake to promote calcium excretion
- In severe cases, hospitalization for intravenous fluids
Because vitamin D is fat-soluble and stored in body tissues, recovery takes time. Vitamin D has a half-life of approximately two weeks in the body, meaning levels drop by half every 14 days after stopping supplementation.
Most people recover fully with appropriate treatment, but severe cases can cause permanent kidney damage or other lasting complications.
Prevention: Taking Vitamin D Safely
Preventing vitamin D toxicity is straightforward: respect dosage guidelines and communicate with healthcare providers.
Follow these safety principles:
- Don’t exceed 4,000 IU daily without medical supervision
- Tell doctors about all supplements, including vitamin D
- Get blood levels tested before starting high-dose supplementation
- Monitor vitamin D levels periodically if taking supplements long-term
- Check all supplements for vitamin D content to avoid duplication
- Follow package directions precisely
According to the CDC, about 86% of households worldwide use iodized salt. While this demonstrates successful fortification of iodine, this fact does not directly address vitamin D fortification safety. Vitamin D fortification in milk and other foods provides beneficial amounts without toxicity risk.
For most people, 600-800 IU daily meets needs without approaching dangerous levels. Some individuals require higher doses under medical supervision, but that’s different from self-prescribing mega-doses.
Vitamin D Benefits Still Matter
Despite toxicity risks, vitamin D remains essential for health. The goal isn’t to avoid vitamin D—it’s to use it appropriately.
Research shows vitamin D supports:
- Bone health and calcium absorption
- Immune system function
- Muscle strength
- Cardiovascular health
The Vitamin D and Omega-3 Trial (VITAL), which included more than 25,000 participants nationwide, all ages 50 and above, found that those taking a vitamin D supplement did not experience lower rates of heart attack, stroke, or cancer. However, among people who later developed cancer, those taking vitamin D supplements had lower mortality rates.
The CDC notes that vitamin D deficiency and cardiovascular disease risk factors are linked in some populations, with prevalence of vitamin D deficiency reaching 50.8% in certain studied groups.
Balance is key. Adequate vitamin D protects health. Excessive amounts cause harm.
Frequently Asked Questions
Can you overdose on vitamin D from the sun?
No. The body self-regulates vitamin D production from sunlight, preventing toxicity. Once skin produces sufficient vitamin D, production stops automatically. Toxicity only occurs from excessive supplementation.
How long does it take to develop vitamin D toxicity?
Toxicity typically requires weeks to months of taking extremely high doses—usually 60,000 IU or more daily. Because vitamin D is fat-soluble and stored in body tissues, it accumulates gradually over time.
What are the first signs of taking too much vitamin D?
Early symptoms include nausea, vomiting, weakness, frequent urination, and excessive thirst. These result from elevated blood calcium levels caused by excessive vitamin D. If you experience these symptoms while taking vitamin D supplements, contact a healthcare provider.
Is 10,000 IU of vitamin D daily too much?
For most adults, 10,000 IU daily exceeds recommended upper limits and could potentially cause problems with long-term use. The safe upper limit is 4,000 IU daily for adults. Doses above this should only be taken under medical supervision with regular blood monitoring.
How do you flush excess vitamin D from your system?
Stop all vitamin D supplementation immediately, increase fluid intake, and reduce dietary calcium. Because vitamin D is stored in fat tissue, it takes several weeks for levels to decline. Severe cases may require hospitalization with intravenous fluids to accelerate calcium elimination.
Can vitamin D toxicity cause permanent damage?
Most people recover fully when toxicity is caught early. However, severe or prolonged cases can cause permanent kidney damage, cardiovascular problems, or bone issues. The key is recognizing symptoms early and seeking prompt medical attention.
How often should I get my vitamin D levels tested?
Testing frequency depends on individual risk factors. People taking vitamin D supplements regularly should consider annual testing. Those on high-dose therapy need more frequent monitoring—typically every 3-6 months. Discuss appropriate testing schedules with a healthcare provider.
Conclusion
Vitamin D supports critical functions throughout the body, from bone strength to immune response. But the line between beneficial and harmful exists for good reason.
Toxicity remains rare because it requires prolonged intake of extremely high doses—amounts that vastly exceed what the body needs or can use effectively. The vast majority of vitamin D toxicity cases result from supplement misuse rather than responsible supplementation or natural sources.
The solution isn’t fear of vitamin D. It’s respect for proper dosing and medical guidance.
If you’re taking vitamin D supplements, verify your dosage stays within safe limits. If you’re considering high-dose supplementation, consult a healthcare provider first. Get baseline blood testing to understand your actual needs.
Most importantly, remember that more doesn’t automatically mean better. Your body needs adequate vitamin D—not excessive amounts. Stay within recommended guidelines, and you’ll gain vitamin D’s benefits without risking its dangers.
