Quick Summary: Missing a dose of blood thinner increases your risk of developing dangerous blood clots, which can lead to stroke, heart attack, or pulmonary embolism. The action you should take depends on the specific medication—some allow you to take a late dose within a few hours, while others require skipping the missed dose entirely. Never double up on doses, and contact your healthcare provider if you frequently miss doses or are unsure what to do.
Blood thinners—medically known as anticoagulants—prevent dangerous blood clots from forming in the body. Millions take these medications daily for conditions like atrial fibrillation, deep vein thrombosis, or after procedures like hip or knee replacement.
But what happens when you forget a dose?
The reality is that missing doses of anticoagulants can have serious consequences. According to research published in JACC Asia, adequate adherence to direct oral anticoagulants (DOACs) is achieved in only 70% of patients in real-world practice. That means nearly one-third of people struggle with consistent dosing.
Here’s everything that happens when a dose gets skipped—and exactly what to do about it.
Why Missing a Blood Thinner Dose Is Dangerous
Anticoagulants work by interfering with the body’s natural clotting process. When taken consistently, they maintain a therapeutic level in the bloodstream that prevents harmful clots without causing excessive bleeding.
Skip a dose, and that protective level drops.
The immediate risk? Blood clots can start forming within hours to days, depending on the medication. These clots can reduce or completely block blood flow to vital organs or extremities. The potential outcomes include stroke, pulmonary embolism (clot in the lungs), heart attack, or deep vein thrombosis.
Research from the University of California San Francisco published in Blood Advances found that missed or delayed doses of DOACs cause patients to spend more time outside the therapeutic range—the safe zone where the medication prevents clots without causing bleeding.
Real talk: consistency matters more with anticoagulants than with almost any other medication class.
Different Blood Thinners, Different Rules
Not all anticoagulants behave the same way in your body. The action needed after a missed dose depends entirely on which medication has been prescribed.
Warfarin (Coumadin, Jantoven)
Warfarin stays in the system longer than newer anticoagulants. It has a half-life of about 40 hours, meaning it takes nearly two days for half the dose to leave the body.
According to the American Heart Association, if a dose of warfarin is missed, take it as soon as remembered on the same day. If it’s already the next day, skip the missed dose entirely and take the regular scheduled dose.
Never take a double dose to compensate.
There’s less room for error with warfarin because it requires regular blood monitoring (INR tests) to ensure therapeutic levels. Research on temporary discontinuation of warfarin shows the INR decreases exponentially after stopping, with wide variation between patients. Age plays a role—older patients experience slower decreases in anticoagulation effect.
Apixaban (Eliquis)
Apixaban is typically taken twice daily. According to Mayo Clinic guidance and NHS recommendations, timing matters here.
If the missed dose is remembered within a few hours of the scheduled time, take it immediately. If it’s nearly time for the next dose (within 6 hours), skip the missed dose and continue with the regular schedule.
The market share data shows apixaban represents 51.3% of DOAC prescriptions in the United States, making it the most commonly prescribed direct oral anticoagulant.
Rivaroxaban (Xarelto)
Rivaroxaban dosing schedules vary by indication—some patients take it once daily, others twice daily.
For once-daily dosing: take the missed dose as soon as remembered on the same day, then resume the normal schedule the next day. For twice-daily dosing: take the dose immediately to ensure two doses are taken that day, then return to the regular twice-daily schedule.
According to pharmacokinetic/pharmacodynamic modeling published in medical research, remedial dosing strategies for rivaroxaban can help minimize both bleeding and thromboembolism risk after missed doses.
Dabigatran (Pradaxa)
Dabigatran is taken twice daily. The window for taking a late dose is smaller than with other anticoagulants—generally within 6 hours of the scheduled time.
If more than 6 hours have passed since the scheduled dose, skip it and take the next dose at the regular time.
Dabigatran represents less than 5% of the DOAC market share, partly due to higher rates of adverse events compared to newer alternatives.
Edoxaban (Savaysa, Lixiana)
Edoxaban is taken once daily. If a dose is missed, take it as soon as possible on the same day. If it’s already the next day, skip the missed dose and resume the regular schedule.
Like other DOACs, doubling up is never recommended.

What Actually Happens in the Body
When an anticoagulant dose is missed, several physiological changes begin almost immediately.
First, the drug concentration in the bloodstream starts declining. How quickly depends on the medication’s half-life—the time it takes for half the drug to be eliminated from the body.
Warfarin has a long half-life (about 40 hours), so one missed dose won’t immediately drop levels dramatically. But newer DOACs like apixaban and rivaroxaban have much shorter half-lives (around 12 hours), meaning their protective effect diminishes faster.
As drug levels fall, the blood’s clotting factors become more active. Platelets become stickier. Clotting proteins that were being suppressed start functioning normally again.
For someone with atrial fibrillation, this creates an immediate window where blood can pool in the heart’s upper chambers and form clots. Those clots can then travel to the brain, causing stroke.
The timeline varies. Some patients might develop clots within 24-48 hours of missing doses. Others might go longer without incident—but the risk steadily climbs with each missed dose.
The Nonadherence Problem
Medication nonadherence with anticoagulants isn’t rare. Research published in JACC Advances indicates that nonadherence to direct oral anticoagulants affects a substantial portion of atrial fibrillation patients.
Why do so many people struggle?
The reasons vary widely. A cross-sectional survey of patients identified several common factors:
- Forgetfulness or confusion about dosing schedules
- Side effects like bleeding or bruising
- Cost concerns (though apixaban is described as the cheapest DOAC)
- Complexity of twice-daily dosing
- Lack of symptoms, leading to questioning medication necessity
- Difficulty swallowing pills
The consequences of poor adherence go beyond individual missed doses. Studies measuring adherence by proportion of days covered (PDC) or medication possession ratio (MPR) show that only patients maintaining at least 80% adherence achieve the full protective benefits seen in clinical trials.
Below that threshold, stroke risk increases substantially.
When Bleeding Becomes the Concern
Here’s where things get complicated. Blood thinners exist in a delicate balance—prevent clots without causing excessive bleeding.
Missing doses tips that balance toward clotting. But there’s a counterintuitive danger: when patients realize they’ve missed doses, some panic and take extra medication to “catch up.”
This is dangerous.
Taking a double dose or multiple missed doses at once can spike blood levels into the danger zone for bleeding. According to the American Heart Association, signs of serious bleeding requiring immediate medical attention include:
- Confusion, weakness, or numbness
- Coughing up large amounts of bright red blood
- Vomiting blood
- Bleeding that won’t stop within 10 minutes
The guidance is universal across all anticoagulants: never double dose. If unsure what to do, contact a healthcare provider or call a medical helpline for advice rather than guessing.
Steps to Take Right Now
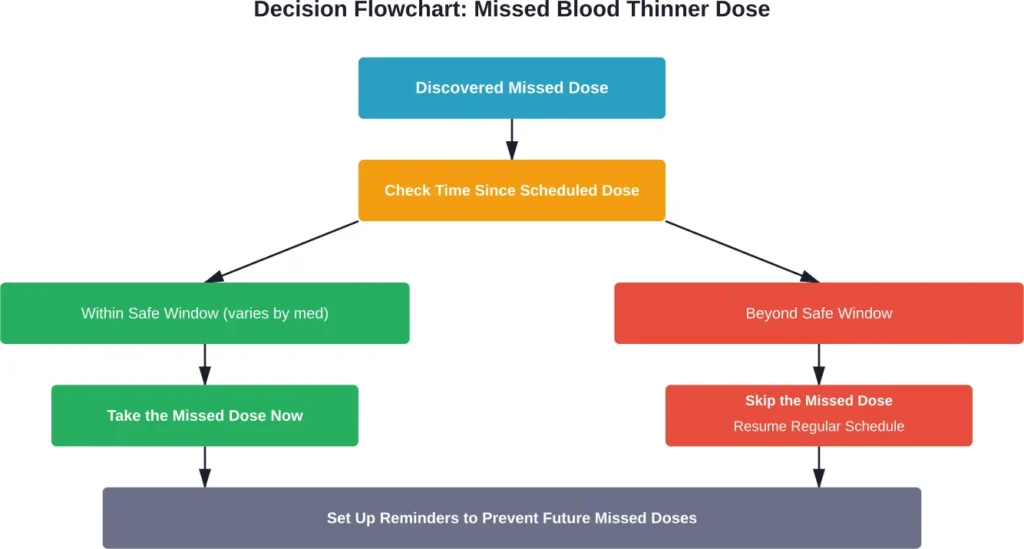
Discovered a missed dose? Here’s the decision tree.
Step 1: Check the time. How long has it been since the scheduled dose? Compare this to the medication-specific windows described earlier.
Step 2: Consult the medication guide. The patient information leaflet that came with the prescription contains specific missed-dose instructions. When in doubt, this is the authoritative source.
Step 3: Take action based on timing. If within the safe window, take the missed dose. If beyond that window, skip it and resume the regular schedule.
Step 4: Document it. Note when the dose was missed and what action was taken. This information may be valuable for healthcare providers.
Step 5: Set up prevention. One missed dose is a signal to implement reminder systems—phone alarms, pill organizers, or medication reminder apps.
If multiple doses have been missed over several days, contact a healthcare provider before resuming. Depending on the medication and indication, bridging therapy or monitoring may be needed.
Special Situations and Complications
Before Surgery or Procedures
Medical procedures often require temporarily stopping anticoagulants to reduce bleeding risk. This is intentional interruption, not a missed dose.
Research on minimally interrupted DOACs shows these strategies can maintain safety during procedures like atrial fibrillation ablation. The key difference: healthcare providers plan the interruption, calculate the timing, and may provide bridging therapy if needed.
Never stop anticoagulants before a procedure without explicit instructions from the healthcare team.
Multiple Missed Doses
Missing several consecutive doses creates a more serious situation. The anticoagulant effect may have worn off completely, leaving the patient unprotected.
After multiple missed doses, some patients may need:
- Blood tests to check coagulation levels (especially for warfarin)
- Temporary bridging with injectable anticoagulants
- Monitoring for signs of clot formation
- Dose adjustments when restarting
Contact a healthcare provider immediately if more than two consecutive doses have been missed.
Drug Interactions
Certain medications, supplements, and foods can interact with anticoagulants, affecting their levels in the bloodstream. Missing a dose while taking interacting substances can create unpredictable effects.
Common interactions include antibiotics, antifungals, NSAIDs, and for warfarin specifically, vitamin K-rich foods.
Prevention Strategies That Actually Work
The best approach to managing missed doses is preventing them in the first place.
Medication adherence research points to several effective strategies:
Pill organizers: Weekly organizers with morning/evening compartments make it immediately obvious if a dose was missed.
Phone alarms: Set daily alarms for exact dosing times. Consider setting a backup alarm 30 minutes later.
Habit stacking: Link medication to an existing daily routine—breakfast, brushing teeth, bedtime rituals. The established habit triggers medication memory.
Medication synchronization: Ask the pharmacy to align all prescription refills to the same date, reducing trips and confusion.
Simplify when possible: If struggling with twice-daily dosing, ask the healthcare provider if a once-daily alternative exists for the specific condition.
Address side effects: Many patients skip doses because of side effects like nausea or bruising. Report these issues—dose adjustments or medication changes may help.
Automatic refills: Set up auto-refill at the pharmacy to ensure the medication is always available.
| Prevention Strategy | Best For | Effectiveness |
|---|---|---|
| Phone Alarms | Tech-comfortable patients | High if used consistently |
| Pill Organizers | Visual learners, multiple medications | Very high |
| Habit Stacking | Routine-oriented individuals | High over time |
| Caregiver Reminders | Memory issues, elderly patients | Very high |
| Medication Apps | Smartphone users, tracking needs | High with engagement |
When to Contact Your Healthcare Provider
Some situations require immediate professional guidance rather than self-management.
Contact a healthcare provider or pharmacist if:
- More than two consecutive doses have been missed
- Unsure which medication was missed (for those on multiple anticoagulants or medications)
- Experiencing symptoms like chest pain, shortness of breath, or sudden leg swelling
- Frequently missing doses due to side effects or other barriers
- The medication guide’s instructions are unclear or contradictory
- New medications or supplements have been started that might interact
According to guidance from medical researchers studying anticoagulant errors, clear communication between patients and providers significantly reduces adverse events. Don’t hesitate to ask questions or report concerns.
The Future of Anticoagulant Management
Research continues advancing how missed or delayed doses are handled.
Model-informed remedial dosing approaches, as described in recent Blood Advances publications, use patient-specific factors to calculate individualized catch-up regimens. Web-based dashboards now exist that can provide personalized remedial dosing strategies based on which medication was missed, when it was supposed to be taken, and individual patient characteristics.
These tools offer more precision than the one-size-fits-all guidance currently in medication guides. Early results suggest they minimize time outside the therapeutic range better than standard recommendations.
But these remain research tools for now. The practical guidance remains: follow the medication-specific windows, never double dose, and contact healthcare providers when uncertain.
Frequently Asked Questions
It depends on the specific medication. For warfarin and edoxaban taken once daily, if a full day has passed, skip the missed dose and take the next scheduled dose. For twice-daily medications like apixaban or dabigatran, never try to make up for the previous day’s doses—just resume the regular schedule. Taking extra doses to compensate creates dangerous bleeding risk.
The timeline varies based on individual risk factors and which anticoagulant is prescribed. DOACs with short half-lives (like apixaban and rivaroxaban) lose protective effect within 24 hours of the last dose. Warfarin’s longer half-life provides some coverage for 2-3 days. However, patients with high-risk conditions like atrial fibrillation could potentially develop clots within 24-48 hours. This variability is why consistent dosing is critical.
Contact a healthcare provider, pharmacist, or poison control immediately. Don’t try to skip the next dose to compensate. Monitor for signs of bleeding: unusual bruising, red or dark brown urine, red or black stools, bleeding gums, or bleeding that won’t stop. According to the American Heart Association, seek emergency care if experiencing confusion, weakness, coughing blood, or uncontrolled bleeding.
A single missed dose doesn’t guarantee a stroke will occur, but it does increase risk. The likelihood depends on why the anticoagulant was prescribed. Patients with atrial fibrillation face higher stroke risk than those taking anticoagulants after surgery. Studies show that even occasional nonadherence reduces the protective effect seen in clinical trials, which is why maintaining at least 80% adherence (PDC ≥80%) is the target.
No. Blood thinners are dosed specifically to maintain consistent levels throughout the day. Splitting doses or altering the schedule without medical guidance can create dangerous fluctuations—either leaving periods without adequate protection or creating bleeding risk from too-high levels. Always follow the medication-specific guidance for missed doses rather than improvising.
Effective strategies include setting phone alarms for exact dosing times, using weekly pill organizers to visually track doses, linking medication to established daily habits like meals or tooth-brushing, and asking family members for reminder help. For patients struggling with adherence, discussing once-daily alternatives with healthcare providers may be worthwhile if twice-daily dosing is the barrier.
Not necessarily. While DOACs like apixaban, rivaroxaban, and edoxaban don’t require the regular blood monitoring that warfarin does, they actually have shorter half-lives. This means they clear from the system faster when doses are missed. Warfarin’s longer half-life provides more cushion after a single missed dose. Regardless of which anticoagulant is prescribed, consistent adherence remains essential for maintaining protection against clots.
The Bottom Line on Missed Doses
Missing blood thinner doses creates real danger. The medications work only when maintained at consistent therapeutic levels—and that requires taking them exactly as prescribed.
When a dose is missed, the specific action depends on the medication and timing. Warfarin allows same-day makeup doses. Apixaban and dabigatran have 6-hour windows. Rivaroxaban rules vary by dosing frequency.
But one rule is universal: never double dose. The bleeding risk from excessive anticoagulation can be just as dangerous as the clotting risk from inadequate treatment.
If doses are being missed frequently, that’s a signal to address the underlying cause. Side effects, cost barriers, complex schedules, or simple forgetfulness—all these issues have solutions. Talk to healthcare providers about what’s really happening.
Because here’s the thing: anticoagulants only work in patients who actually take them. And taking them means every scheduled dose, on time, consistently.
Set up whatever systems are needed to make that happen. The stakes are too high for anything less.
