Quick Summary: Using too much clobetasol can lead to serious side effects including skin thinning, stretch marks, HPA axis suppression (affecting adrenal function), increased infection risk, and potential systemic absorption causing Cushing syndrome. Overuse is particularly dangerous in children, on sensitive areas like the face or genitals, and when used beyond recommended duration without medical supervision.
Clobetasol propionate is one of the most potent topical corticosteroids available. While it’s highly effective for treating inflammatory skin conditions like psoriasis, eczema, and dermatitis, its strength becomes a double-edged sword when used improperly.
The medication’s power to reduce inflammation and itching quickly makes it tempting to use more than prescribed. But what actually happens when you cross that line?
Let’s break down the real risks backed by medical research and clinical data.
Understanding Clobetasol’s Potency
Clobetasol ranks as a Class I (super-potent) topical corticosteroid. This classification matters because it determines both effectiveness and risk profile.
According to research published in the Indian Dermatology Online Journal, topical steroids have revolutionized dermatologic therapy. However, their usefulness has become “a double edged sword with constantly rising” complications when misused.
Here’s the thing though—less than 2% of topically applied hydrocortisone (a much weaker steroid) gets absorbed into systemic circulation after a single application. But clobetasol’s super-potent nature changes this equation significantly, especially with prolonged or excessive use.
Immediate Local Side Effects of Overuse
The first signs of excessive clobetasol application typically appear right where the medication contacts skin.
Skin Thinning and Atrophy
Skin atrophy represents one of the most common consequences of overusing potent topical steroids. The skin becomes noticeably thinner, more fragile, and almost translucent in appearance.
This happens because corticosteroids inhibit collagen synthesis and cause dermal tissue breakdown. Once significant atrophy occurs, reversing it becomes challenging and sometimes impossible.
Stretch Marks (Striae)
Permanent stretch marks can develop from excessive topical steroid use, particularly in areas where skin naturally stretches—like the groin, armpits, and inner thighs.
These aren’t the typical stretch marks from weight changes. They’re medication-induced and tend to be more prominent and difficult to treat.
Skin Discoloration
Hypopigmentation (lightening of skin) commonly occurs with prolonged clobetasol use. The affected areas may become noticeably lighter than surrounding skin, creating an uneven skin tone that persists long after stopping the medication.

Telangiectasia (Spider Veins)
Visible dilated blood vessels near the skin surface can develop, creating a spider-web appearance. These typically don’t disappear after discontinuing the medication.
Increased Infection Risk
Topical steroids suppress local immune function. That’s part of how they reduce inflammation—but it’s also why they increase infection susceptibility.
Research published in the Indian Dermatology Online Journal documented multiple infection risks associated with prolonged topical steroid use, including tinea versicolor, onychomycosis caused by Trichophyton, and various bacterial infections.
The skin’s natural defense mechanisms become compromised. Fungal infections particularly thrive because the anti-inflammatory effects mask early warning signs like redness and itching.
Sound familiar? That’s why infections can progress significantly before becoming obvious.
HPA Axis Suppression: When Topical Becomes Systemic
Here’s where things get serious. The hypothalamic-pituitary-adrenal (HPA) axis controls cortisol production—essential for stress response, metabolism, and immune function.
Excessive topical steroid use can suppress this system. According to prescribing information for clobetasol propionate foam documented by the FDA, HPA axis suppression is a known risk that requires monitoring, especially with high doses or prolonged application.
How Absorption Happens
While topical absorption is normally minimal, several factors dramatically increase it:
- Application to large surface areas
- Use on thin skin (face, genitals, skin folds)
- Occlusive dressings or bandages over application sites
- Damaged or inflamed skin barriers
- Prolonged duration of use
- Pediatric use (children have higher surface area to body weight ratios)
Research in the Indian Dermatology Online Journal found that less than 2% of hydrocortisone absorbs systemically. But clobetasol is exponentially more potent, and absorption increases dramatically under occlusion or on compromised skin.
Symptoms of HPA Suppression
When the HPA axis becomes suppressed, cortisol production decreases. This can manifest as:
- Unusual fatigue and weakness
- Weight loss or poor weight gain in children
- Nausea and vomiting
- Low blood pressure
- Hypoglycemia (low blood sugar)
Testing for HPA suppression typically involves morning cortisol levels or ACTH stimulation tests.
Cushing Syndrome from Topical Steroids
Real talk: systemic steroid absorption can cause Cushing syndrome—a condition normally associated with oral steroid use or tumors.
A case documented in literature discussed a 6-year-old girl with vulvar lichen sclerosus who developed Cushing syndrome (moon facies, plethora, and weight gain) after 8 weeks of clobetasol.
That’s not an isolated case. Cushing syndrome from topical clobetasol overuse includes:
| Clinical Feature | Description |
|---|---|
| Moon facies | Rounded, full facial appearance |
| Central obesity | Weight gain in trunk and abdomen |
| Buffalo hump | Fat accumulation between shoulders |
| Skin changes | Easy bruising, purple striae |
| Muscle weakness | Particularly in limbs |
| Metabolic effects | Elevated blood sugar, hypertension |
These effects can develop surprisingly quickly with super-potent topical steroids, especially in vulnerable populations.
Pediatric Risks: Why Children Are More Vulnerable
Children face disproportionate risks from topical steroid overuse. Their higher surface area to body weight ratio means the same application amount results in proportionally higher systemic exposure.
According to a clinical trial documented at Purdue University’s pharmacy database, studies specifically evaluate HPA axis suppression potential in pediatric subjects because the risk is significantly elevated.
A retrospective case series of 14 pediatric females aged 2 to 10 years with lichen sclerosus treated with clobetasol 0.05% topical ointment and systematically bridged to tacrolimus 0.1% topical ointment was conducted.
But wait. There’s more.
Growth suppression can occur in children experiencing prolonged HPA axis suppression. Cortisol plays crucial roles in growth and development, and disrupting this system during critical developmental periods can have lasting effects.
Ocular Complications
Using clobetasol near the eyes or on eyelids creates specific risks. The FDA-documented prescribing information includes warnings about ophthalmic adverse reactions.
Prolonged use increases the risk of:
- Glaucoma (increased intraocular pressure)
- Cataracts
- Central serous chorioretinopathy
The prescribing information explicitly states: “If visual symptoms occur, consider referral to an ophthalmologist.”
These aren’t minor inconveniences—they’re sight-threatening conditions requiring immediate medical attention.
Steroid Addiction and Rebound Phenomena
Topical steroid addiction (also called Red Skin Syndrome or topical steroid withdrawal) represents a controversial but documented phenomenon.
Research in the Indian Dermatology Online Journal describes it as “chronic dermatitis not responding to locally applied steroids or rarely, as acute eczema, urticaria, acute local edema, immediate-type reaction, or id eruption like spread over the body.”
The Withdrawal Cycle
When someone stops using potent topical steroids after prolonged use, the original condition often flares dramatically—sometimes worse than before treatment started.
This creates a vicious cycle: the flare prompts reapplication, which provides temporary relief, but discontinuation causes an even worse rebound. Dependency develops.
Breaking this cycle requires medical supervision and often involves a controlled tapering strategy rather than abrupt cessation.
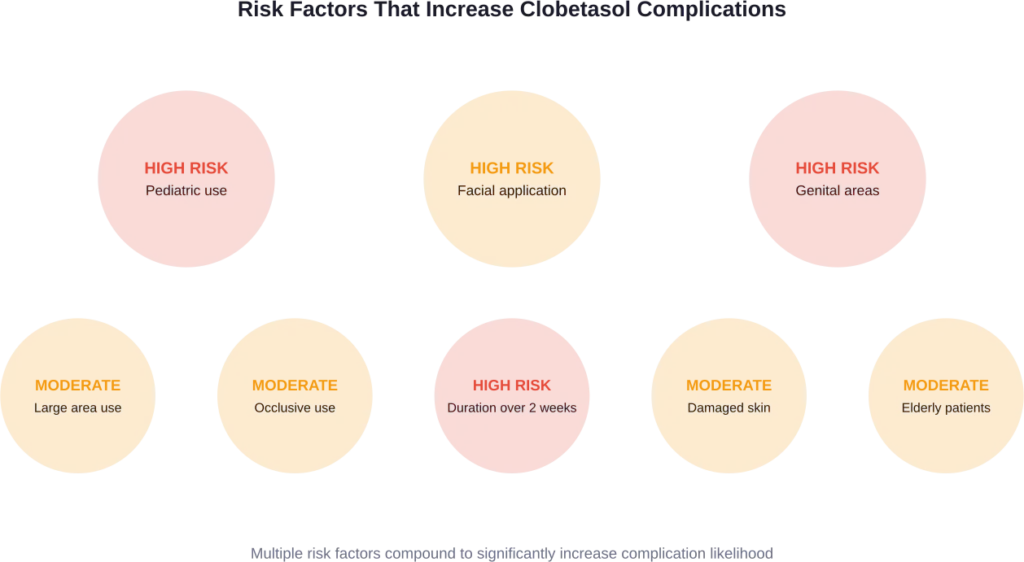
Safe Usage Guidelines
Given these risks, how should clobetasol be used safely?
Duration Limits
Treatment duration should not exceed 2 consecutive weeks under standard prescribing guidelines, with medical supervision required for any longer duration.
Application Amount
Apply only a thin layer to affected areas. More is not better—excess medication doesn’t improve results but does increase side effect risk.
The “fingertip unit” measurement helps standardize amounts: one fingertip unit (from the tip to the first joint) covers an area roughly twice the size of an adult’s hand.
Frequency
Once or twice daily application is standard. Applying more frequently doesn’t enhance effectiveness but does increase exposure and risk.
Location Restrictions
Avoid using clobetasol on:
- The face (unless specifically prescribed)
- Genital areas (requires specific formulations and monitoring)
- Skin folds and creases
- Under breasts
- Near the eyes
These areas have thinner skin with higher absorption rates.
Step-Down Therapy
Rather than abruptly stopping clobetasol, transitioning to a less potent steroid can help prevent rebound flares. This approach maintains control while reducing systemic exposure.
When to Seek Medical Attention
Contact a healthcare provider immediately if experiencing:
| Warning Sign | Potential Indication |
|---|---|
| Unusual fatigue or weakness | HPA axis suppression |
| Vision changes or eye pain | Ocular complications |
| Rapid weight gain | Cushing syndrome |
| Facial rounding or puffiness | Cushing syndrome |
| Signs of infection | Immunosuppression |
| Severe skin thinning | Dermal atrophy |
| Worsening condition | Steroid resistance or infection |
These symptoms warrant immediate evaluation because they may indicate serious complications requiring intervention.
Alternative Treatment Strategies
Several approaches can reduce reliance on super-potent topical steroids.
Vitamin D Analogs
Calcipotriol (calcipotriene) offers an effective alternative for psoriasis. Research demonstrates that clobetasol propionate followed by calcipotriol is superior to calcipotriol alone in topical treatment of psoriasis.
The strategy? Use clobetasol short-term for rapid control, then transition to calcipotriol for maintenance.
Topical Calcineurin Inhibitors
Tacrolimus and pimecrolimus work differently from steroids. They don’t cause skin atrophy and can be used on sensitive areas like the face and genitals.
While they have their own side effect profiles, they don’t carry the same HPA axis suppression or skin-thinning risks.
Combination Therapy
Using clobetasol intermittently (such as weekends only) combined with non-steroidal treatments during the week can maintain control while minimizing exposure.
Special Populations
Pregnancy and Breastfeeding
Clobetasol should be used during pregnancy only when potential benefits outweigh risks. Large amounts or prolonged use may affect fetal development.
For breastfeeding, avoid application to the breast area to prevent infant exposure.
Elderly Patients
Older adults often have thinner skin naturally, increasing both absorption and fragility. Lower potency steroids or reduced frequency may be more appropriate.
Diabetic Patients
Systemic steroid absorption can affect blood glucose control. Diabetic patients using clobetasol extensively should monitor blood sugar levels more carefully.
Frequently Asked Questions
Local side effects like skin thinning can begin within 3-6 weeks of excessive use. Systemic effects such as HPA axis suppression may develop after 2-8 weeks, depending on application amount, body area, and individual factors. The 6-year-old patient who developed Cushing syndrome showed symptoms after just 8 weeks of treatment.
Some effects like inflammation and discoloration may improve after discontinuation. However, severe skin atrophy, permanent striae (stretch marks), and telangiectasia often persist indefinitely. Early detection and immediate cessation provide the best chance for recovery.
Generally speaking, continuous use should not exceed 2 consecutive weeks for most conditions. Total cumulative exposure shouldn’t exceed 50 grams per week. Treatment duration should not exceed 2 consecutive weeks under standard prescribing guidelines, with medical supervision required for any longer duration.
Facial use carries significantly higher risks due to thinner skin and increased absorption. It should only be done under explicit medical direction for specific conditions, typically for very short durations (3-7 days maximum), and never near the eyes due to glaucoma and cataract risks.
Abrupt discontinuation after prolonged use can trigger rebound flares—sometimes more severe than the original condition. This occurs because the skin has become dependent on the anti-inflammatory effects. Gradual tapering or transitioning to lower-potency steroids helps minimize rebound phenomena.
While HPA axis suppression from topical clobetasol is usually reversible after discontinuation, recovery can take weeks to months. In rare cases, particularly with very prolonged or extensive use, some degree of adrenal insufficiency may persist. Pediatric patients face higher risks of growth suppression during critical developmental periods.
Testing typically involves morning serum cortisol levels (drawn between 8-9 AM when cortisol should be highest) or ACTH stimulation testing. Abnormal results indicate the adrenal glands aren’t responding properly to normal regulatory signals, requiring gradual withdrawal of the topical steroid under medical supervision.
Conclusion
Clobetasol propionate stands among the most effective treatments for inflammatory skin conditions. But that power demands respect.
Overuse transforms a valuable medication into a source of complications ranging from cosmetic concerns like skin thinning and stretch marks to serious systemic effects including HPA axis suppression and Cushing syndrome.
The risks escalate dramatically in children, on sensitive body areas, and with prolonged duration. What starts as a solution can become a compounding problem when used beyond recommended parameters.
Safe use requires adherence to prescribed amounts, durations, and application sites. When treatment extends beyond 2 weeks or covers large areas, medical monitoring becomes essential.
If currently using clobetasol, review the treatment plan with a healthcare provider. Are there alternatives? Could step-down therapy work? Is the current regimen still appropriate?
The most effective treatment is one that works without causing harm. For clobetasol, that balance exists within narrow parameters—and staying within them makes all the difference.