Quick Summary: Falling asleep with a concussion is generally safe and even beneficial for recovery. The old myth about staying awake after a concussion has been debunked by medical research. However, 30-70% of concussion patients experience sleep disturbances including insomnia, hypersomnia, and sleep apnea that can complicate recovery and require medical attention.
The moment someone sustains a head injury, panic often sets in. Friends hover nervously, someone inevitably says “don’t let them fall asleep,” and the injured person fights to keep their eyes open. Sound familiar?
Here’s the thing though—that advice is outdated. Decades of medical research have completely changed how healthcare providers approach concussion care, particularly when it comes to sleep.
Concussions affect approximately 2.5 million people in emergency rooms annually, according to research on traumatic brain injury. Yet misinformation about proper concussion care persists, especially regarding sleep.
The Old Myth: Why People Thought You Couldn’t Sleep After a Concussion
For generations, conventional wisdom held that sleeping after a concussion was dangerous. The fear? That an injured person might slip into a coma or lose consciousness without anyone noticing.
This concern wasn’t entirely unfounded. In severe brain injuries with bleeding or swelling, consciousness levels can deteriorate rapidly. Medical professionals needed to monitor patients closely for signs of worsening conditions.
But somewhere along the line, this precaution for severe injuries got applied to all concussions. And that’s where the myth took hold.
The reality is far more nuanced. Most concussions are mild traumatic brain injuries that don’t involve skull fractures or dangerous bleeding. Through modern imaging and monitoring techniques, healthcare providers can now distinguish between cases that require vigilant observation and those that don’t.
What Actually Happens When You Sleep With a Concussion
Contrary to popular belief, sleep after a concussion is not dangerous. In fact, it’s a crucial part of recovery.
According to the CDC, rest is one of the most important treatments after a concussion. The brain needs time to heal, and sleep provides exactly that opportunity.
The Brain’s Healing Process During Sleep
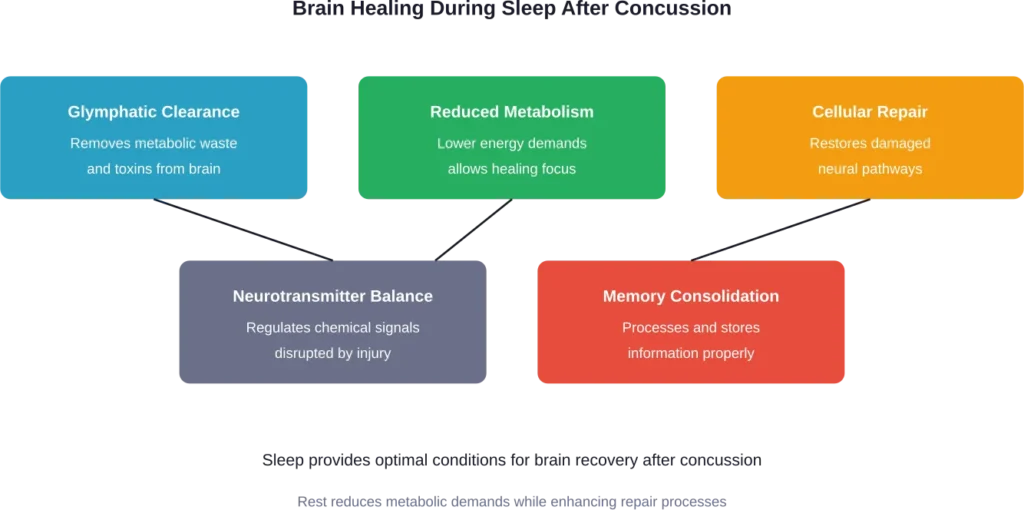
When someone sleeps after a concussion, several important processes occur. The brain’s glymphatic system—essentially its waste removal system—becomes more active during sleep. This system clears out metabolic byproducts and toxins that accumulate during waking hours.
Research published by the NIH shows that the neurometabolic cascade following concussion modulates sleep-wake physiology through alterations in neurotransmitter release, glymphatic clearance, and extracellular ionic concentration. Sleep becomes even more critical when the brain is healing from injury.
The injured brain requires additional energy to repair damaged cells and restore normal function. Sleep reduces the brain’s metabolic demands, allowing more resources to be directed toward healing.
When Sleep Becomes Problematic
While sleeping itself isn’t dangerous, there are circumstances where immediate sleep should be delayed. If the injured person hasn’t been medically evaluated yet, sleeping might delay diagnosis and treatment of more serious complications.
According to research on sleep disturbances after traumatic brain injury, approximately 30-70% of patients experience sleep problems following their injury. These disruptions can actually hinder recovery if left unaddressed.
The key isn’t preventing sleep—it’s ensuring proper medical evaluation first and monitoring for concerning symptoms.
Recognizing Dangerous Concussion Symptoms
Not all head injuries are created equal. Some require immediate emergency care, regardless of whether the person wants to sleep.
The CDC identifies specific danger signs that warrant emergency medical attention:
- One pupil appearing larger than the other
- Drowsiness that makes it impossible to wake the person
- Severe or worsening headaches that don’t improve
- Weakness, numbness, or decreased coordination
- Repeated vomiting or persistent nausea
- Slurred speech or unusual behavior
- Seizures or convulsions
- Loss of consciousness lasting more than 30 seconds
- Increasing confusion or disorientation
These symptoms suggest something more serious than a simple concussion—possibly bleeding in or around the brain that requires urgent intervention.
Real talk: if any of these symptoms appear, don’t wait. Get to an emergency room immediately.
The Sleep Disturbances That Actually Matter
Here’s where things get complicated. While falling asleep with a concussion won’t hurt recovery, the sleep problems that often develop after concussion definitely can.
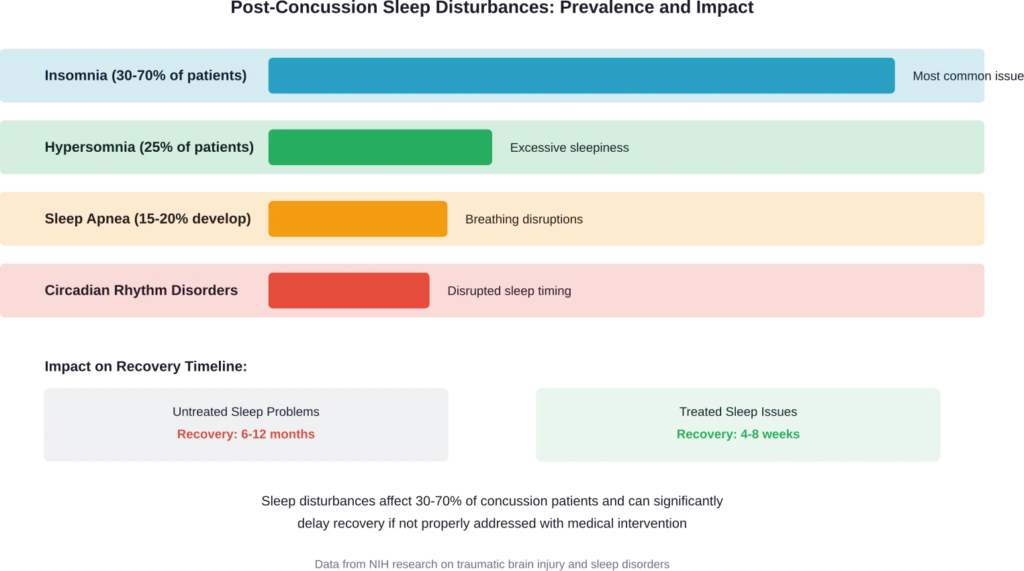
Research shows that between 30% and 80% of concussion patients experience various sleep disturbances, including sleep apnea, hypersomnia, and insomnia. These problems can persist for weeks or even months after the initial injury.
Common Post-Concussion Sleep Issues
Medical studies on traumatic brain injury-induced sleep disorders have identified several patterns that emerge after concussion:
Insomnia: Difficulty falling asleep or staying asleep affects many concussion patients. The brain’s altered neurotransmitter levels and disrupted circadian rhythms contribute to this problem.
Hypersomnia: Excessive daytime sleepiness occurs in approximately 25% of traumatic brain injury patients in the first few days after injury. These individuals sleep far more than normal but still feel exhausted.
Sleep Apnea: Some patients develop breathing disruptions during sleep following their injury, reducing sleep quality and oxygen delivery to the healing brain.
Delayed Sleep Phase: The body’s internal clock gets thrown off, making it difficult to fall asleep at normal times and wake up refreshed.
Why Sleep Problems Develop After Concussion
The mechanisms behind post-concussion sleep disturbances are complex. Research on concussion and the sleeping brain suggests that the neurometabolic cascade triggered by injury affects multiple systems.
Neurotransmitter imbalances disrupt the brain’s natural sleep-wake signals. Glutamate levels spike while GABA—the brain’s calming neurotransmitter—may decrease. This creates a state of hyperarousal that makes restful sleep difficult.
The injury can also affect the orexin system, which regulates wakefulness and sleep transitions. Damage to this system explains why some patients develop narcolepsy-like symptoms after traumatic brain injury.
Additionally, research on acute concussion in youth shows that stress responses become dysregulated. Studies found longer sleep onset times and elevated fatigue levels in injured patients, with melatonin levels lower at bedtime compared to uninjured controls.
When to Seek Medical Care for Concussion
Getting proper medical evaluation after a head injury isn’t optional—it’s essential. Even if someone feels “fine” initially, symptoms can worsen over the first 24-72 hours.
According to the World Health Organization and FIFA’s concussion awareness campaign, symptoms may take up to 72 hours to fully manifest. This delayed presentation makes initial medical assessment crucial.
Initial Evaluation
Healthcare providers assess several factors when evaluating suspected concussions:
- Mechanism of injury and impact force
- Immediate symptoms and their severity
- Loss of consciousness duration
- Memory problems or amnesia
- Physical examination findings
- Neurological signs
- Previous concussion history
Research published in January 2025 emphasizes the importance of diagnosing cervical spine injuries that can occur with concussion and mimic concussion symptoms. If these injuries go untreated, they can become a risk for persisting symptoms.
Follow-Up Care
The CDC recommends returning to a healthcare provider if symptoms aren’t improving or are getting worse. Providers may refer patients to specialists such as neurologists, sports medicine physicians, or neuropsychologists.
Most children and adults recover from concussions with proper care, but recovery timelines vary. Some people feel better within days, while others experience symptoms for weeks or months.
The Right Way to Sleep After a Concussion
Once medical evaluation confirms that sleeping is safe, creating optimal sleep conditions supports recovery.
Monitoring in the First 24 Hours
While keeping someone awake isn’t necessary, periodic check-ins during the first night provide peace of mind. Waking someone every few hours to ask simple questions—their name, location, and current date—ensures they’re responsive.
This practice doesn’t prevent complications, but it helps detect worsening symptoms that require emergency care.
Optimizing Sleep Environment
Good sleep hygiene becomes even more important during concussion recovery:
- Maintain a dark, quiet bedroom
- Keep room temperature cool
- Avoid screens for 1-2 hours before bed
- Establish consistent sleep and wake times
- Limit daytime naps to 20-30 minutes
Research on behavioral therapies for post-traumatic sleep problems suggests that sleep hygiene modifications, while basic, form the foundation of effective treatment.
Activity Modifications
According to research from the University of Buffalo published in January 2025, active management is the most effective concussion treatment. This doesn’t mean complete rest—it means carefully calibrated activity that doesn’t worsen symptoms.
During the first few days after concussion, cognitive and physical rest remains important. This means limiting:
- Screen time and digital device use
- Reading and mentally demanding tasks
- Physical exercise and sports
- Loud environments and bright lights
As symptoms improve, gradual return to normal activities under medical supervision helps recovery.
Post-Concussion Syndrome and Chronic Sleep Issues
Some individuals develop post-concussion syndrome—persistent symptoms lasting months beyond the initial injury. Sleep problems feature prominently in this condition.
Studies on factors associated with persisting symptoms after concussion found that acute cognitive symptoms, medical history of anxiety or depression, history of sleep disorders, and clinical signs like loss of consciousness were associated with the greatest odds of prolonged recovery.
When sleep disturbances persist beyond expected recovery timelines, specialized treatment becomes necessary.
Treatment Approaches for Chronic Sleep Problems
Medical research on treating post-traumatic brain injury sleep disorders shows mixed results. Unfortunately, treatment of sleep disorders associated with traumatic brain injury may not always improve neuropsychological function or sleepiness as much as hoped.
However, several interventions show promise:
Cognitive Behavioral Therapy for Insomnia (CBT-I): This evidence-based approach addresses the thoughts and behaviors that interfere with sleep.
Light Therapy: Timed light exposure can help reset disrupted circadian rhythms.
Medications: In some cases, sleep medications or melatonin supplements may be prescribed, though they’re not first-line treatments.
Treatment of Sleep Apnea: CPAP therapy or other interventions for breathing-related sleep disorders.
Manual Therapy: Research exploring manual therapy for traumatic brain injury management shows growing interest in addressing physical symptoms, particularly cervical spine issues that can contribute to sleep problems.
| Treatment Approach | Target Symptoms | Timeline to Improvement | Success Rate |
|---|---|---|---|
| Cognitive Behavioral Therapy | Insomnia, sleep anxiety | 4-8 weeks | Moderate to High |
| Light Therapy | Circadian rhythm disorders | 2-4 weeks | Moderate |
| Sleep Medications | Severe insomnia | Immediate but temporary | Variable |
| CPAP Therapy | Sleep apnea | 1-2 weeks | High for apnea |
| Manual Therapy | Physical symptoms, neck pain | 4-6 weeks | Moderate |
Special Considerations for Different Age Groups
Concussion management varies across different populations, with unique considerations for children, adults, and older individuals.
Children and Adolescents
The CDC’s resources on caring for children with concussions emphasize that most children feel better with the right care. However, pediatric brains are still developing, making them potentially more vulnerable to injury effects.
Sleep disturbances in children after concussion can significantly impact school performance and social development. According to CDC guidance on returning to school after concussion, support and accommodations should be based on the student’s symptoms.
Parents should monitor for behavioral changes that might indicate sleep problems: increased irritability, difficulty concentrating, declining grades, or social withdrawal.
Athletes and Sports-Related Concussions
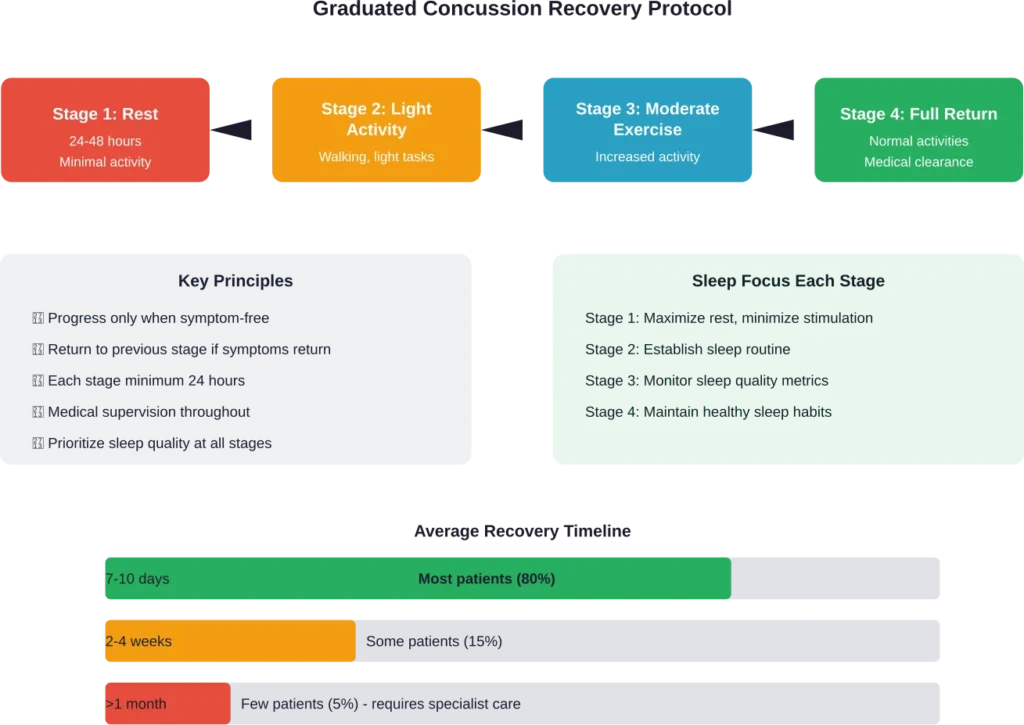
Sports medicine has led much of the advancement in concussion care. The recognition that rest is crucial but excessive rest may be counterproductive has changed return-to-play protocols.
Modern concussion management in sports involves graduated return-to-play protocols. Athletes progress through stages only when they can complete each level without symptom recurrence.
Older Adults
Older individuals face unique challenges with concussion recovery. Pre-existing medical conditions, medications, and age-related brain changes can complicate both injury and recovery.
Sleep architecture naturally changes with age, and adding concussion-related sleep disruptions to existing sleep issues creates a complex clinical picture requiring specialized management.
The Connection Between Sleep, Stress, and Concussion Recovery
Research on sleep and stress in acute concussion shows a complex interplay between biological and psychological factors. Studies of acutely injured youth found that stress and sleep onset were significantly related, with most subjects meeting criteria for Acute Stress Disorder.
This relationship works both ways. Poor sleep increases stress and anxiety, which in turn makes sleep more difficult. Breaking this cycle becomes essential for recovery.
Nightmares represent another concerning issue. Research on associations of nightmares and sleep disturbance with neurobehavioral symptoms found that nightmares were independently associated with symptoms representing excess functioning like anxiety and impulsivity, while general sleep disturbance was associated with deficits in normal functioning.
What Healthcare Providers Look for in Sleep Assessments
When concussion patients report sleep problems, comprehensive evaluation becomes necessary. A practical guide for evaluating sleep disturbance in concussion patients outlines appropriate metrics for outpatient settings.
Evaluations typically include:
- Sleep diaries tracking bedtime, wake time, and sleep quality
- Questionnaires assessing insomnia severity and daytime function
- Actigraphy monitoring actual sleep-wake patterns
- Polysomnography for suspected sleep-disordered breathing
- Assessment of melatonin and cortisol rhythms when circadian disorders are suspected
This thorough approach helps distinguish between different types of sleep disorders, ensuring targeted treatment.
Myths vs. Facts About Concussion and Sleep
Let’s clear up some persistent misconceptions:
| Myth | Fact |
|---|---|
| Never let someone sleep after a concussion | Sleep is safe and beneficial after medical evaluation confirms no serious complications |
| You need to wake someone every hour all night | Periodic checks every 2-3 hours in the first 24 hours are sufficient if symptoms aren’t concerning |
| All concussions require CT scans or MRIs | Most concussions are diagnosed clinically without imaging unless specific concerning features are present |
| Rest means complete isolation in a dark room | Modern concussion management recommends 24-48 hours of relative rest followed by gradual activity increase |
| Sleep problems after concussion always resolve on their own | 30-70% of patients experience sleep disturbances that may require specific treatment |
| You can’t do anything until fully recovered | Active management with carefully graded activity promotes better recovery than prolonged complete rest |
When Sleep Problems Indicate Complications
While sleep disturbances are common after concussion, certain patterns suggest more serious issues requiring urgent evaluation.
Warning signs include:
- Sudden worsening of sleep quality after initial improvement
- Development of new symptoms alongside sleep problems
- Extreme difficulty waking or excessive unresponsiveness
- Sleep problems persisting beyond 3 months despite treatment
- Combination of severe insomnia with worsening mood or suicidal thoughts
These situations warrant immediate medical consultation and possible specialist referral.
The Role of Technology in Modern Concussion Care
Advances in technology have transformed how healthcare providers diagnose, monitor, and treat concussions and associated sleep problems.
Wearable devices now track sleep patterns, physical activity levels, and even some cognitive metrics. This objective data supplements patient-reported symptoms, giving providers a more complete recovery picture.
Telemedicine has expanded access to specialist concussion care, particularly important for individuals in areas without local expertise.
Computerized neurocognitive testing helps establish baseline brain function and track recovery, though these tools complement rather than replace clinical evaluation.
Creating a Concussion Recovery Plan
Successful recovery requires a comprehensive approach addressing physical, cognitive, and sleep-related aspects.
A typical recovery plan includes:
Medical Monitoring: Regular check-ins with healthcare providers to assess symptom progression and adjust treatment as needed.
Activity Management: Gradual return to physical and cognitive activities based on symptom tolerance.
Sleep Hygiene: Consistent sleep schedule, optimized sleep environment, and addressing factors that interfere with rest.
Symptom Tracking: Daily recording of symptoms helps identify patterns and triggers.
Stress Management: Techniques like deep breathing, meditation, or gentle yoga can help manage the stress response that interferes with sleep and healing.
Support Systems: Family, friends, coaches, teachers, and employers should understand the injury and accommodate recovery needs.
Frequently Asked Questions About Sleeping With a Concussion
No, falling asleep after a head injury isn’t inherently dangerous. However, it’s essential to get medical evaluation first to rule out serious complications like brain bleeding. Once a healthcare provider has assessed the injury and determined it’s safe, sleep actually helps recovery. The old advice about staying awake was based on concern about missing worsening symptoms, but modern medical understanding shows that sleep is beneficial for brain healing after concussion.
After initial medical evaluation confirms that sleeping is safe, monitoring should continue for the first 24 hours. During this period, checking on the person every 2-3 hours by waking them briefly and asking simple orientation questions provides reassurance. This practice helps detect any concerning changes in consciousness or symptoms. According to the World Health Organization, symptoms may take up to 72 hours to fully manifest, so continued awareness of warning signs remains important even after the first night.
Research shows that 30-70% of concussion patients experience sleep disturbances. The most common problems include insomnia (difficulty falling or staying asleep), hypersomnia (excessive daytime sleepiness affecting about 25% of patients), disrupted circadian rhythms causing difficulty sleeping at normal times, and in some cases, sleep apnea or breathing-related sleep issues. These problems can persist for weeks or months and often require specific treatment to resolve rather than improving on their own.
Absolutely. Sleep disturbances significantly impact concussion recovery timelines. Untreated sleep problems can extend recovery from what might be 4-8 weeks to 6-12 months or longer. Sleep is when the brain’s glymphatic system clears metabolic waste, neurotransmitter balance is restored, and cellular repair occurs most actively. Without quality sleep, these essential healing processes are compromised. Studies have found that addressing sleep issues early in concussion recovery improves overall outcomes and speeds return to normal function.
Seek immediate emergency care if someone with a concussion exhibits danger signs including: extreme difficulty waking or inability to wake them, one pupil larger than the other, severe worsening headaches, repeated vomiting, seizures, slurred speech, increasing confusion, weakness or numbness, or loss of coordination. These symptoms suggest possible bleeding in or around the brain requiring urgent intervention. If any of these develop—whether the person is sleeping or awake—go to the emergency room immediately.
While the basic principles remain the same—sleep is beneficial after medical evaluation—children may need more careful monitoring and different recovery timelines. Pediatric brains are still developing, potentially making them more vulnerable to injury effects. The CDC emphasizes that most children recover well with proper care, but sleep disturbances in children can significantly impact school performance and development. Children often require more structured return-to-school and return-to-play protocols, with accommodations based on their specific symptoms. Parents should work closely with healthcare providers and schools to support recovery.
Several strategies can optimize sleep during recovery: maintain consistent sleep and wake times even on weekends, create a dark, quiet, cool sleeping environment, avoid screens for 1-2 hours before bed since blue light disrupts melatonin production, limit daytime naps to 20-30 minutes if needed, avoid caffeine after early afternoon, and practice relaxation techniques before bed. If sleep problems persist despite these measures, consult a healthcare provider. They may recommend cognitive behavioral therapy for insomnia, light therapy for circadian issues, or other targeted treatments depending on the specific sleep disorder present.
Conclusion: Sleep Is Part of the Solution, Not the Problem
The outdated advice about staying awake after a concussion has been thoroughly debunked by modern medical research. Sleep isn’t dangerous—it’s essential for brain healing.
That said, the relationship between concussion and sleep is complex. While falling asleep with a concussion won’t harm recovery, the sleep disturbances that frequently develop after injury can significantly impact healing if left untreated.
The key takeaways? Get proper medical evaluation after any head injury. Follow healthcare provider recommendations for activity and rest. Monitor for danger signs that require emergency care. And if sleep problems develop or persist, seek treatment rather than assuming they’ll resolve on their own.
With appropriate care, most people recover fully from concussions. Understanding the role of sleep in that recovery process—both its benefits and its potential complications—empowers patients and caregivers to support optimal healing.
If someone in your care has sustained a concussion, don’t let outdated myths guide your decisions. Trust modern medical evidence, work with qualified healthcare providers, and remember that sleep is a powerful ally in the recovery process.
