Quick Summary: Stopping steroids suddenly can trigger serious health complications including adrenal crisis, severe withdrawal symptoms, and potentially life-threatening drops in blood pressure. Your body needs time to resume natural cortisol production after prolonged steroid use, which is why medical professionals recommend gradual tapering under supervision rather than abrupt cessation.
Steroids have helped millions manage inflammatory conditions, autoimmune disorders, and other serious health issues. But here’s the thing—stopping them isn’t as simple as just not taking the next pill.
According to research published in Diagnostics, as many as 1–3% of the population are currently on glucocorticoid treatment. That’s millions of people who need to understand the risks of sudden discontinuation.
The consequences of stopping steroids abruptly can range from uncomfortable to potentially fatal. Let’s break down exactly what happens in your body when steroid treatment stops without proper tapering.
Why Your Body Depends on Steroids After Extended Use
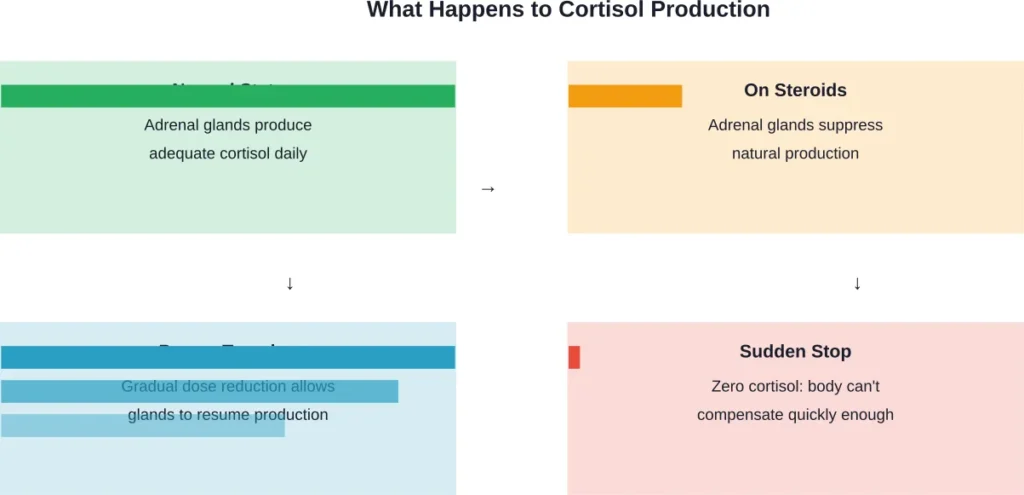
When taking steroids like prednisone for more than a few days, something critical happens in the body. The adrenal glands—small organs that sit on top of the kidneys—normally produce cortisol, a natural steroid hormone essential for life.
External steroid medication signals the body that enough cortisol is present. In response, the hypothalamic-pituitary-adrenal (HPA) axis suppresses natural cortisol production. The adrenal glands essentially go dormant.
This isn’t a problem while taking steroids. But it becomes dangerous the moment treatment stops suddenly.
Adrenal Insufficiency: The Primary Danger
When steroids stop abruptly, the body suddenly has no cortisol—neither from medication nor from natural production. This condition is called adrenal insufficiency, and it’s serious.
According to the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK), the most common symptoms of adrenal insufficiency include chronic fatigue, muscle weakness, loss of appetite, weight loss, and abdominal pain.
But it can get worse. Much worse.
Adrenal Crisis: A Medical Emergency
The most severe complication is adrenal crisis—a life-threatening condition that requires immediate medical attention. Research published in StatPearls defines adrenal crisis as acute deterioration with systolic blood pressure below 100 mm Hg.
The mortality rate? According to the same source, adrenal crisis has a substantial mortality rate and requires immediate recognition and intervention to prevent fatal outcomes.
Symptoms of adrenal crisis include severe weakness, confusion, pain in the lower back or legs, severe abdominal pain, high fever, and drastically low blood pressure leading to shock.
Steroid Withdrawal Syndrome: What to Expect
Even when adrenal crisis doesn’t occur, stopping steroids suddenly triggers what medical professionals call steroid withdrawal syndrome (SWS). A case report published in the Korean Journal of Family Medicine documented this phenomenon in detail.
The symptoms aren’t pleasant. Common withdrawal symptoms include:
- Severe fatigue and lethargy
- Body aches and joint pain
- Nausea and vomiting
- Headaches
- Fever
- Low blood pressure and dizziness
- Mood changes including depression and anxiety
- Sleep disturbances
Here’s what makes withdrawal tricky—these symptoms can mimic the original condition being treated. That makes it difficult to distinguish between disease relapse and withdrawal effects.
How Long Does Recovery Take?
The timeline for HPA axis recovery varies considerably between individuals. According to research in Translational Pediatrics, most patients showed recovery of the HPA axis by 4–12 weeks. However, 13% of patients had persistent adrenal insufficiency at 20 weeks after receiving glucocorticoid therapy.
Some people need months—occasionally over a year—for their adrenal glands to fully resume normal function.
Recovery time depends on several factors:
| Factor | Impact on Recovery Time |
|---|---|
| Duration of steroid use | Longer use = longer recovery |
| Dose taken | Higher doses suppress the HPA axis more |
| Type of steroid | Different steroids have varying potency |
| Individual variation | Genetic and physiological differences matter |
| Underlying condition | Some diseases affect adrenal function |
Why Tapering Is Non-Negotiable
According to Mayo Clinic, if steroids are stopped abruptly or tapered too quickly, withdrawal symptoms can occur including fatigue, joint pain, and fever. The solution? Gradual dose reduction.
Tapering allows the adrenal glands to gradually wake up and resume cortisol production. The body adjusts incrementally rather than experiencing the shock of sudden deprivation.
But wait. There’s no universal tapering protocol. The optimal tapering schedule depends on treatment duration, dose, and individual factors. A review in PubMed noted that current guidelines for corticosteroid tapering rely heavily on expert opinion and small case series with a trial-and-error approach. The exact schedule must be individualized based on individual patient factors.
Special Considerations and Risk Factors
Some people face higher risks when discontinuing steroids. Those who’ve taken high doses for extended periods are particularly vulnerable.
Other risk factors include previous adrenal insufficiency, pituitary disorders, and concurrent use of certain medications that affect cortisol metabolism.
Real talk: never adjust steroid doses without medical supervision. Community discussions on platforms like Mayo Clinic Connect reveal numerous accounts of people experiencing severe symptoms after attempting self-directed tapering.
Anabolic Steroids vs. Corticosteroids
It’s worth noting that this discussion focuses on corticosteroids like prednisone and dexamethasone—medications prescribed for inflammation and autoimmune conditions.
Anabolic steroids, used for muscle building, present different withdrawal concerns. According to the National Institute on Drug Abuse (NIDA), anabolic-androgenic steroids are synthetic variations of testosterone with distinct risks.
Both types shouldn’t be stopped suddenly, but for different physiological reasons.
What to Do If Steroids Were Already Stopped Abruptly
If steroids have already been discontinued suddenly and symptoms develop, seek immediate medical attention. Don’t wait.
Emergency treatment for adrenal crisis typically involves intravenous hydrocortisone, fluids, and electrolyte replacement. The faster treatment begins, the better the outcome.
For less severe withdrawal symptoms, a physician may restart steroids at a low dose and implement a proper tapering schedule.
Frequently Asked Questions
Withdrawal symptoms can appear within hours to several days after the last dose, though timing varies based on the steroid’s half-life and individual factors.
While most people recover fully with proper treatment, severe adrenal crisis can cause permanent complications or death if not treated promptly. The adrenal glands themselves typically recover function over time, though this process can take months.
Generally, steroid use for more than a few weeks may suppress the HPA axis enough to require tapering. However, even shorter courses at high doses can necessitate gradual reduction. Always consult a physician before stopping any steroid medication.
Yes. The ACTH stimulation test measures adrenal gland response and is considered the gold standard for diagnosing adrenal insufficiency. Morning cortisol levels can also provide useful information about HPA axis recovery.
Not necessarily. Steroid withdrawal syndrome can mimic disease symptoms, making differentiation challenging. Medical evaluation is necessary to distinguish between withdrawal effects and actual disease relapse.
No supplements have been proven to accelerate adrenal gland recovery or prevent withdrawal symptoms. The safest approach is proper medical supervision with gradual dose reduction. Some physicians may recommend adequate hydration and salt intake, but this should be discussed individually.
Physical and emotional stress can worsen withdrawal symptoms and increase cortisol demands when the body can’t meet them. Avoiding strenuous activity, getting adequate rest, and managing stress are important during the tapering period.
The Bottom Line
Stopping steroids suddenly isn’t just uncomfortable—it’s potentially dangerous. The body needs time to restore natural cortisol production after the HPA axis has been suppressed.
Adrenal crisis remains a medical emergency with real mortality risk. Even less severe withdrawal syndrome can significantly impact quality of life and complicate medical management.
The evidence is clear: proper tapering under medical supervision is the only safe approach to discontinuing steroid therapy. The specific tapering schedule should be individualized based on treatment duration, dose, and individual risk factors.
If currently taking steroids or planning to discontinue them, work closely with a healthcare provider. Never adjust doses independently, and seek immediate medical attention if severe symptoms develop after stopping steroids.
