Quick Summary: Waking a sleepwalker won’t cause a heart attack or serious harm—that’s a myth. However, sudden awakening can temporarily confuse or disorient them. The safest approach is to gently guide them back to bed without waking them, while keeping the environment safe to prevent injury.
You shuffle into the hallway at 2 a.m. for a glass of water and freeze. Your spouse is standing in the kitchen, eyes open, rearranging spice jars with robotic precision. They’re sleepwalking.
Now what? Should you wake them? Will they freak out?
The old myth says waking a sleepwalker could trigger a heart attack or cause brain damage. Here’s the truth: that’s completely false. But there are safety considerations worth knowing about.
The Heart Attack Myth: Completely Debunked
Let’s clear this up first. Dr. Raghu Reddy, a pulmonologist and sleep medicine specialist at UAMS, confirms that waking a sleepwalker won’t cause a heart attack or serious medical trauma.
This myth has persisted for decades, likely because sleepwalking looks eerie and because people who are suddenly awakened during deep sleep can react with confusion or even mild aggression. But that’s temporary disorientation, not medical danger.
The real concern isn’t the act of waking someone—it’s what happens during the sleepwalking episode itself.
What Actually Happens When You Wake a Sleepwalker
If you do wake someone who’s sleepwalking, they’ll likely experience brief confusion or disorientation. According to the Sleep Foundation, they may not remember the incident at all.
Think about how groggy you feel when someone wakes you from deep sleep. Now multiply that by the fact that their brain is stuck between sleep stages. It’s jarring.
Some people might startle, become momentarily frightened, or react defensively. This isn’t because waking them is inherently dangerous—it’s because their brain hasn’t fully transitioned to wakefulness.
According to medical research published in StatPearls, somnambulism (the medical term for sleepwalking) occurs during incomplete arousals from deep NREM sleep. The person is neither fully asleep nor awake, which explains the confusion when forced into consciousness.
The Disorientation Factor
When awakened mid-episode, sleepwalkers often don’t know where they are or what they’re doing. This can be embarrassing or distressing for them.
They might also feel extremely tired, since their deep sleep was interrupted. Each complete sleep cycle (with both NREM and REM sleep) lasts approximately 90 minutes in adults, and disrupting these cycles affects sleep quality.
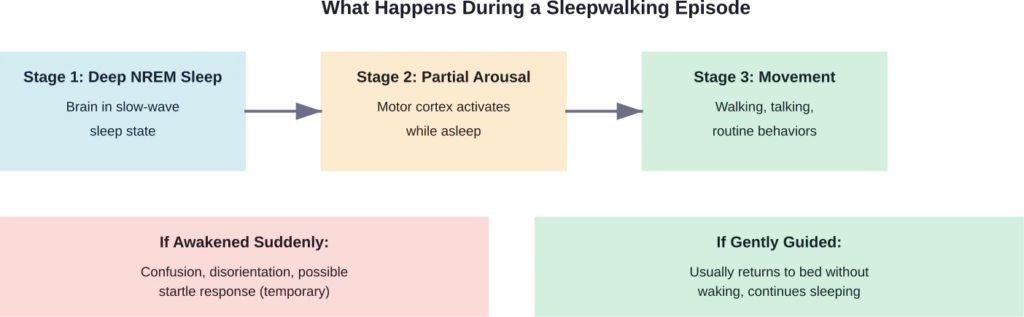
Understanding Sleepwalking: More Than Just Walking
Sleepwalking isn’t just about wandering around. According to the NHS, people who are sleepwalking may appear to wake up, sit up or get out of bed, have their eyes open but look blank, and not respond normally to their environment.
They might do routine things like rearranging furniture, getting dressed, or even attempting to leave the house. The behaviors can range from harmless to potentially dangerous.
A comprehensive review published in Cureus found that amongst NREM parasomnias, the prevalence rate of sleepwalking in children under 12 years of age is 17%. That’s roughly one in six kids. In adults, the lifetime prevalence is 6.9%, according to research on disorders of arousal.
Why Does Sleepwalking Happen?
Sleepwalking occurs during NREM sleep, particularly during slow-wave sleep stages. According to research from the American Academy of Sleep Medicine, several factors can trigger or increase the frequency and severity of episodes in 59 percent of cases:
- Stressful events or strong emotional experiences
- Sleep deprivation (not getting adequate sleep for your age group)
- Alcohol or drug intake
- Certain medications that affect sleep architecture
- Genetic factors (monozygotic twins have higher concordance than dizygotic twins)
The CDC recommends specific sleep durations by age group. Toddlers need 11–14 hours, school-age kids need 9–11 hours, teenagers need 8–10 hours, and adults need 7 or more hours per night. Not meeting these recommendations increases parasomnia risk.
What You Should Do When Someone Is Sleepwalking
Here’s the thing: safety comes first. Always.
If the person is in immediate danger—about to walk down stairs, out a door, or into something hazardous—gently wake them. Yes, they might be confused, but that’s better than injury.
But if they’re safe? Don’t wake them.
The Gentle Guidance Approach
Most experts recommend calmly guiding the sleepwalker back to bed without waking them. Use a soft voice, gentle touch, and simple directions.
Something like: “It’s time for bed now. Let’s go back to your room.”
They’ll often comply without fully waking up. According to Northwestern Medicine, this approach minimizes confusion and allows them to continue sleeping naturally.
Avoid:
- Sudden movements or loud noises
- Grabbing or restraining them aggressively
- Asking complex questions (they can’t process them properly)
- Making them feel embarrassed if they do wake up
Safety Precautions for Frequent Sleepwalkers
If sleepwalking happens regularly, environmental modifications become critical. According to patient handouts from medical research, these precautions can prevent injuries:
| Safety Measure | Purpose | Implementation |
|---|---|---|
| Remove obstacles | Prevent trips and falls | Clear hallways, stairs, and bedroom floors |
| Secure windows | Prevent falls from heights | Install locks or window guards |
| Lock exterior doors | Keep person inside | Use deadbolts or alarms on doors |
| Remove sharp objects | Reduce injury risk | Store knives, scissors, and tools safely |
| Install safety gates | Block access to stairs | Use childproof gates at stairways |
| Consider alarms | Alert others to episodes | Door alarms or motion sensors |
According to a study from Guy’s Hospital involving 512 patients with NREM parasomnias, environmental safety measures are a cornerstone of parasomnia management.
When Sleepwalking Becomes a Health Concern
Occasional sleepwalking, especially in children, usually isn’t cause for alarm. Kids typically outgrow it by their teen years.
But adult sleepwalking is different. Research from the American Academy of Sleep Medicine found that adult sleepwalking is associated with higher frequency of daytime sleepiness, fatigue, insomnia, depressive and anxiety symptoms, and altered quality of life.
See a healthcare provider if:
- Episodes happen frequently (more than once or twice per week)
- The sleepwalker injures themselves or others
- Episodes involve dangerous behaviors (driving, using knives, leaving the house)
- Sleepwalking starts suddenly in adulthood
- Episodes disrupt household sleep regularly
- Daytime fatigue or other symptoms develop
According to the CDC, sleep disorders are associated with increased risk of anxiety, depression, obesity, heart disease, and injury. That’s worth taking seriously.
Treatment Options That Actually Work
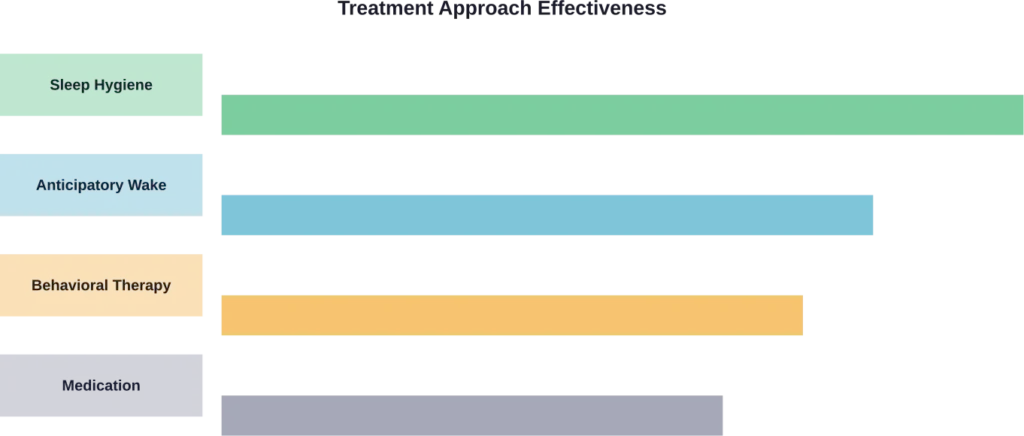
For chronic or dangerous sleepwalking, several treatment approaches show promise. According to Mayo Clinic treatment guidelines, options include:
Anticipatory Awakenings: This involves waking the person about 15 minutes before they usually sleepwalk, then staying awake for a few minutes before falling asleep again. It disrupts the sleep cycle pattern that triggers episodes.
Medication Adjustments: If sleepwalking appears related to a particular drug, changing medications may help.
Benzodiazepines: These medications slow down activity in the central nervous system and can reduce parasomnia frequency.
Behavioral Therapy: A systematic review on behavioral and psychological treatments for NREM parasomnias found that mental health therapy can address underlying stress, anxiety, or other triggers.
Sleep Hygiene Improvements: Getting adequate sleep, maintaining consistent sleep schedules, and managing stress through breathing exercises, stretching, and journaling all reduce episode frequency.
The Genetic Connection
Sleepwalking runs in families. According to StatPearls research, monozygotic twins have a higher chance of somnambulism than dizygotic twins, suggesting strong genetic components.
Scientists have identified that a higher proportion of people with sleepwalking test positive for the DQB1*0501 gene compared to those without sleepwalking. This suggests that DQB1 genes play a role in motor disorders during sleep.
If sleepwalking runs in your family, you’re at increased risk. But genetics isn’t destiny—environmental factors and sleep hygiene still matter enormously.
Sleepwalking vs. Other Parasomnias
Sleepwalking isn’t the only NREM parasomnia. Understanding the differences helps with proper identification and treatment.
| Parasomnia Type | Key Characteristics | Prevalence |
|---|---|---|
| Sleepwalking | Walking and complex behaviors during sleep | 17% in children under 12, 6.9% lifetime in adults |
| Confusional Arousals | Confusion upon waking, disorientation, slow speech | 17.3% in children ages 3-13, 6.9% in adults over 15 |
| Sleep Terrors | Screaming, intense fear, difficult to wake | Common in children ages 1-12, rare in adults |
| REM Behavior Disorder | Acting out dreams, violent movements during REM | More common in adults, especially older males |
REM behavior disorder differs significantly from sleepwalking. According to research on REM sleep behavior disorder, it involves physically acting out vivid dreams with vocal sounds and sudden, often violent arm and leg movements during REM sleep—not the deep NREM sleep where sleepwalking occurs.
Frequently Asked Questions
No. This is a complete myth with no medical basis. Medical experts confirm that waking a sleepwalker won’t cause heart attacks, brain damage, or other serious medical trauma. The person may be temporarily confused or disoriented, but that’s not dangerous.
Not necessarily. If they’re safe and not in danger, it’s better to gently guide them back to bed without waking them. Only wake them if they’re about to hurt themselves or are in immediate danger.
Children spend more time in deep NREM sleep, where sleepwalking occurs. Their brains are also still developing, which affects sleep architecture. Most children naturally outgrow sleepwalking by their teenage years as their sleep patterns mature.
Not usually. Occasional sleepwalking, especially in children, is typically benign. However, frequent sleepwalking in adults, or episodes that involve dangerous behaviors or cause injuries, should be evaluated by a healthcare provider. It can sometimes indicate underlying sleep disorders or other health issues.
Absolutely. Research shows that stressful events and strong emotional experiences are among the most common triggers that increase both frequency and severity of sleepwalking episodes. Managing stress through relaxation techniques, adequate sleep, and potentially therapy can reduce episodes.
Usually not. Most sleepwalkers have no memory of their episodes. If awakened during the event, they may have brief, fragmented memories, but typically the entire episode is forgotten because their brain wasn’t fully conscious during the activity.
Benzodiazepines are the most commonly prescribed medications for chronic sleepwalking, as they slow central nervous system activity and reduce parasomnia frequency. However, medication should only be used under medical supervision, and behavioral approaches should be tried first. Some cases require adjusting existing medications that may be triggering episodes.
Bottom Line: Safety Over Myths
The notion that waking a sleepwalker causes heart attacks is pure fiction. What matters is handling the situation safely and calmly.
If someone you know sleepwalks occasionally and isn’t in danger, guide them gently back to bed. If episodes are frequent, dangerous, or affecting quality of life, it’s time to see a sleep specialist.
Create a safe environment, address underlying triggers like sleep deprivation and stress, and remember that most childhood sleepwalking resolves naturally. For adults with persistent problems, effective treatments exist—from anticipatory awakenings to medication to behavioral therapy.
The key takeaway? Stop worrying about old myths and start focusing on what actually keeps sleepwalkers safe.
If sleepwalking is disrupting your household or causing safety concerns, schedule a consultation with a sleep medicine specialist. Getting adequate sleep and addressing parasomnia triggers can dramatically improve both sleep quality and overall health.
