Quick Summary: Mixing prednisone and alcohol is not recommended because both substances can intensify shared side effects including gastrointestinal irritation, immune system suppression, blood sugar fluctuations, and bone density loss. While there’s no direct drug interaction, research shows alcohol use among corticosteroid users increases fracture risk by 22-26% and can worsen stomach bleeding risks. The safest approach depends on your dosage, treatment duration, and individual health factors.
Prednisone is a synthetic corticosteroid widely prescribed for inflammatory conditions ranging from rheumatoid arthritis to asthma. According to StatPearls (NIH), prednisone is a synthetic glucocorticoid converted in the liver to the active metabolite prednisolone and works by suppressing immune activity and reducing inflammation throughout the body.
When patients receive this prescription, one question comes up consistently: can they still drink alcohol?
Here’s the thing though—there’s no direct chemical interaction between prednisone and alcohol that creates a toxic reaction. But that doesn’t mean combining them is safe. Both substances stress similar body systems, and together they can amplify risks that neither poses alone.
Understanding What Prednisone Does to Your Body
Prednisone belongs to a class of medications called glucocorticoids. These drugs mimic cortisol, a hormone naturally produced by the adrenal glands. When prescribed at therapeutic doses, prednisone produces powerful anti-inflammatory and immunosuppressive effects.
The medication treats dozens of conditions: lupus, inflammatory bowel disease, severe allergies, skin disorders, and organ transplant rejection. According to StatPearls medical reference, prednisone remains a cornerstone treatment for both chronic and acute inflammatory diseases.
But this effectiveness comes with trade-offs. Prednisone affects multiple body systems simultaneously—immune function, bone metabolism, blood sugar regulation, stomach acid production, and mood chemistry all shift when corticosteroids enter the picture.
These effects become more pronounced at higher doses and with longer treatment duration. Research published in healthcare journals shows patients on doses above 10 mg daily face notably increased risks for complications including infections and bone density loss.
The Core Problem: Overlapping Side Effects
The primary danger when mixing prednisone and alcohol isn’t a direct drug interaction. It’s that both substances produce similar stress on the body.
Think of it like this: if prednisone irritates the stomach lining and alcohol does the same thing, combining them doesn’t just add those effects together—it can multiply them.
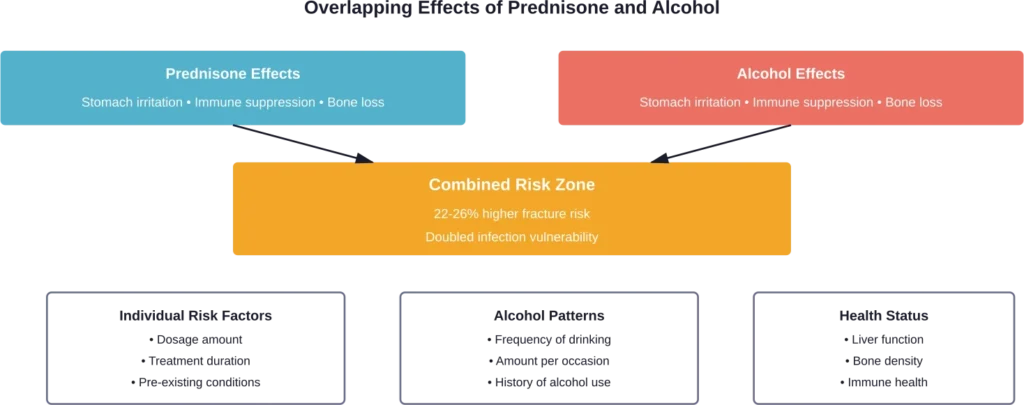
Gastrointestinal Bleeding and Ulcer Risks
Both prednisone and alcohol independently irritate the stomach lining. Prednisone increases stomach acid production and reduces protective mucus. Alcohol does essentially the same thing.
When combined, the risk of developing gastric ulcers or gastrointestinal bleeding climbs significantly. Community discussions frequently mention stomach pain as a common complaint when mixing these substances.
The danger intensifies for people taking prednisone long-term or at higher doses. According to medical sources, the stomach lining damage can progress from mild irritation to serious bleeding ulcers.
Real talk: if someone already experiences heartburn or stomach discomfort from prednisone alone, adding alcohol creates a recipe for acute gastrointestinal problems.
Immune System Suppression Compounds
Prednisone deliberately suppresses immune function—that’s how it controls inflammation. Research shows that at doses of 10 mg/day or higher, pneumonia risk increases substantially. The immune system simply can’t respond to pathogens as effectively.
Alcohol similarly impairs immune defenses. It damages lung tissue barriers and reduces white blood cell activity. According to research published by the National Institutes of Health, alcohol disrupts immune responses at multiple levels.
Put them together, and infection risk escalates. This matters most for people on chronic prednisone therapy for conditions like lupus or rheumatoid arthritis, where maintaining some immune function becomes critical for preventing opportunistic infections.
When Infections Become Dangerous
The combination doesn’t just increase common cold frequency. It raises risks for serious bacterial infections, fungal infections, and viral complications that healthy immune systems typically handle without issue.
For patients already immunocompromised by their underlying condition, adding alcohol while taking prednisone creates a vulnerability window that can lead to hospitalizations.
Bone Health Deteriorates Faster
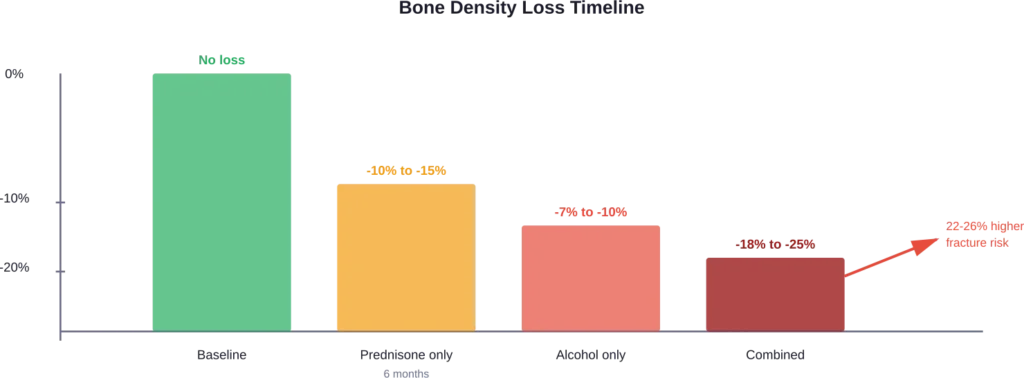
Here’s where the research gets specific. Medical studies examining alcohol use among corticosteroid users found fracture risk increases by approximately 22 to 26 percent compared to those who abstain from drinking.
According to research on osteonecrosis published in Healthcare (2023), in non-traumatic osteonecrosis, alcohol abuse and corticosteroids are involved in up to 80% of cases. Most affected patients fall between ages 30 and 50—prime years when people don’t expect bone problems.
According to Hospital for Special Surgery, a person can lose 10% to 20% bone mass within the first six months of corticosteroid therapy. Alcohol accelerates this process by interfering with calcium absorption and disrupting bone cell activity.
The concern extends beyond fractures. Osteonecrosis—actual bone tissue death—becomes a real possibility, particularly in weight-bearing joints like hips and knees. This condition often requires surgical intervention and affects quality of life substantially.
Blood Sugar Fluctuations Worsen
Prednisone raises blood glucose levels by triggering glucose production in the liver and reducing insulin sensitivity. This effect happens even in people without diabetes—though diabetics face particularly serious challenges managing blood sugar while on corticosteroids.
Alcohol creates unpredictable blood sugar swings. Initially it may spike glucose, then cause dangerous drops hours later as the liver processes the alcohol instead of maintaining blood sugar balance.
When combined, the metabolic chaos intensifies. Blood sugar might swing wildly between dangerous highs and concerning lows, making diabetes management nearly impossible.
Dosage and Duration Matter Significantly
Not all prednisone prescriptions carry the same risk profile when mixed with alcohol. Short-term use at low doses presents different considerations than long-term high-dose therapy.
| Treatment Type | Dosage | Duration | Alcohol Risk Level |
|---|---|---|---|
| Short-term acute | Under 10 mg daily | 5-7 days | Lower risk, but not recommended |
| Short-term higher dose | Above 10 mg daily | 5-14 days | Moderate risk, abstinence preferred |
| Long-term low dose | Under 10 mg daily | Months to years | Significant cumulative risk |
| Long-term high dose | Above 10 mg daily | Months to years | High risk, complete abstinence recommended |
Research indicates that doses above 10 mg daily correlate with substantially increased complication rates. At these levels, adding alcohol becomes particularly problematic.
For someone taking a prednisone taper pack for poison ivy—maybe 40 mg tapering down over five days—occasional light drinking might not cause major problems, though it’s still not advised. But someone managing lupus with 20 mg daily long-term? That’s a completely different risk equation.
When Complete Abstinence Becomes Critical
Certain situations demand complete alcohol avoidance while taking prednisone. These aren’t flexible guidelines—they’re medical necessities.
Anyone with pre-existing liver disease should avoid alcohol entirely while on corticosteroids. The liver metabolizes both substances, and compromised liver function magnifies every risk discussed here.
People with histories of gastrointestinal ulcers or bleeding face dangerous complications if they drink while taking prednisone. The stomach lining damage can progress rapidly to serious medical emergencies.
Those with osteoporosis or low bone density can’t afford the additional bone loss that alcohol contributes. Research on osteonecrosis shows the combination can be devastating for skeletal health.
Diabetics need strict blood sugar control, which becomes nearly impossible when alcohol enters the mix alongside prednisone’s glucose-raising effects.
Hypothalamic Pituitary Adrenal Axis Suppression
Research indicates that both chronic alcohol use and long-term corticosteroid therapy can disrupt the hypothalamic-pituitary-adrenal axis—the body’s stress response system.
Prednisone suppresses natural cortisol production. When someone takes corticosteroids long-term then suddenly stops, the adrenal glands may not resume normal function immediately. This creates a dangerous deficiency during times of physical stress.
Alcohol similarly disrupts HPA axis function. Studies show that central corticosterone concentration alterations can persist at extended times after alcohol withdrawal, even as long as two months. Combined effects can create serious hormonal imbalances that affect stress response, metabolism, and immune function.
Practical Timing Considerations
If someone on short-term prednisone decides to drink despite medical advice against it, timing becomes relevant. Both substances tax the liver, so spacing them reduces immediate metabolic burden.
Prednisone typically stays active in the body for 18-36 hours. Alcohol metabolism varies by person but generally processes at about one standard drink per hour.
For short-term prescriptions, waiting until the course finishes provides the safest approach. For chronic therapy, the conversation with a healthcare provider needs to address individual health status, dosage levels, and specific risk factors.
But here’s the reality: there’s no truly safe interval that eliminates risk. The damage both substances inflict—to stomach lining, bones, immune function—accumulates whether they’re taken simultaneously or hours apart.
Signs Something’s Wrong
Community discussions reveal common symptoms people experience when mixing prednisone and alcohol:
- Severe stomach pain or persistent heartburn
- Black or bloody stools indicating gastrointestinal bleeding
- Unusual bruising or bleeding
- Frequent infections or wounds that won’t heal
- Extreme mood swings or depression
- Severe blood sugar fluctuations
- Joint pain or mobility problems
Any of these symptoms warrants immediate medical attention. They can indicate serious complications requiring intervention.
What Healthcare Providers Recommend
Medical consensus leans strongly toward alcohol avoidance during prednisone therapy. While no absolute contraindication exists—meaning it won’t kill someone immediately like certain drug combinations—the risk profile doesn’t support drinking.
Healthcare providers typically advise:
- Complete abstinence for high-dose or long-term therapy
- Extreme caution and minimal consumption for short-term low-dose prescriptions
- Individual risk assessment based on underlying health conditions
- Close monitoring for anyone who chooses to drink despite recommendations
The decision ultimately involves weighing personal circumstances against documented medical risks. Someone taking 5 mg daily for a few weeks faces different odds than someone on 40 mg daily for months.
Frequently Asked Questions
While one drink likely won’t cause immediate catastrophic effects, it’s not recommended. Both substances stress the stomach lining, suppress immune function, and affect bone health. The risks compound even with small amounts of alcohol, particularly at higher prednisone doses or with longer treatment duration.
Prednisone typically clears the system within 18-36 hours after the last dose for short-term use. However, the physiological effects—particularly on bone density and immune function—persist much longer. For short courses, waiting 2-3 days after completion provides reasonable caution. For long-term therapy, discuss timing with a healthcare provider based on individual recovery factors.
Prednisone doesn’t directly increase alcohol absorption or intoxication rates. However, both substances affect the liver, and prednisone can alter how efficiently the body processes various substances. Some people report feeling alcohol’s effects more strongly while on corticosteroids, though this varies individually.
A single accidental exposure typically won’t cause permanent damage, especially with low-dose short-term therapy. Monitor for stomach pain, unusual bleeding, or other concerning symptoms. Contact a healthcare provider if symptoms develop. The greatest dangers emerge with repeated combined use, not isolated incidents.
No. Beer, wine, and liquor all contain ethanol, which creates the same physiological effects regardless of beverage type. The alcohol content matters more than the drink format—a standard beer, glass of wine, and shot of liquor contain roughly equivalent alcohol amounts and pose similar risks when combined with prednisone.
Alcohol doesn’t directly interfere with prednisone’s anti-inflammatory action. However, alcohol triggers inflammation in various body tissues, potentially working against the therapeutic effects. Additionally, the combined metabolic stress may compromise treatment outcomes for the underlying condition being treated.
People with liver disease, history of gastrointestinal ulcers or bleeding, osteoporosis, poorly controlled diabetes, or compromised immune systems should completely avoid alcohol during prednisone therapy. Those on high doses (above 10 mg daily) or long-term treatment also face risks serious enough to warrant complete abstinence regardless of other health factors.
The Bottom Line on Prednisone and Alcohol
No direct chemical interaction between prednisone and alcohol exists that creates an immediate toxic reaction. That technical fact misleads some people into thinking the combination is safe.
The real danger lies in overlapping biological effects. Both substances irritate the stomach, suppress immune function, weaken bones, and stress the liver. Research demonstrates that alcohol use among corticosteroid users increases fracture risk by 22-26% and contributes to up to 80% of non-traumatic osteonecrosis cases.
Medical evidence strongly supports avoiding alcohol during prednisone therapy, particularly for high-dose or long-term treatment. The risks—gastrointestinal bleeding, bone density loss, increased infection vulnerability, and metabolic disruption—outweigh any temporary enjoyment alcohol provides.
Certain health conditions make the combination especially dangerous: liver disease, ulcer history, osteoporosis, and diabetes all create situations where drinking while taking prednisone can lead to serious medical complications.
If prescribed prednisone, discuss alcohol use honestly with a healthcare provider. Individual factors—dosage, treatment duration, underlying health conditions, and personal medical history—determine specific risk levels and appropriate guidelines.
The safest approach? Skip the alcohol while taking prednisone. The medication works to manage serious health conditions that deserve optimal treatment outcomes, not compromised results from preventable risks.
