Quick Summary: Yes, you can absolutely be allergic to weed (cannabis). Cannabis allergies are becoming more common as usage increases, with reactions ranging from mild symptoms like sneezing and skin rashes to severe responses including anaphylaxis. Allergic reactions can occur through smoking, touching the plant, or consuming cannabis products.
With cannabis legalization expanding across the globe and 219 million people using cannabis in 2021 (4% of the global adult population), a surprising issue has emerged: cannabis allergies are becoming increasingly common. According to research published in medical journals, approximately 4% of the global adult population uses cannabis, yet many remain unaware that the plant can trigger legitimate allergic reactions.
The American Academy of Allergy, Asthma & Immunology confirms that Cannabis sativa—the same plant used for medicinal treatment, recreational use, and industrial hemp production—can cause allergic responses similar to other pollen-bearing plants. And here’s the thing: as more people encounter cannabis through medical use, recreational smoking, or even workplace exposure, allergists expect to see more patients experiencing allergic reactions.
So what does a cannabis allergy actually look like? How common is it? And what should someone do if they suspect they’re allergic?
Understanding Cannabis Allergy: The Basics
Cannabis allergy occurs when the immune system identifies proteins in the marijuana plant as harmful invaders. The body produces immunoglobulin E (IgE) antibodies in response, triggering allergic symptoms that range from annoying to life-threatening.
Research published by the National Center for Biotechnology Information identifies several specific allergens in Cannabis sativa. The most significant is Can s 3, a non-specific lipid transfer protein (nsLTP) that constitutes an important allergen, particularly in Europe. Other identified allergens include profilin (Can s 2) and oxygen-evolving enhancer protein (Can s 4).
Cannabis allergies can develop through multiple exposure routes. Inhaling marijuana smoke or pollen represents the most common trigger, but direct contact with the plant can also cause reactions. Even consuming edibles or hempseed—promoted as a protein-rich superfood—can trigger symptoms in sensitized individuals.
Common Symptoms: What Cannabis Allergy Looks Like
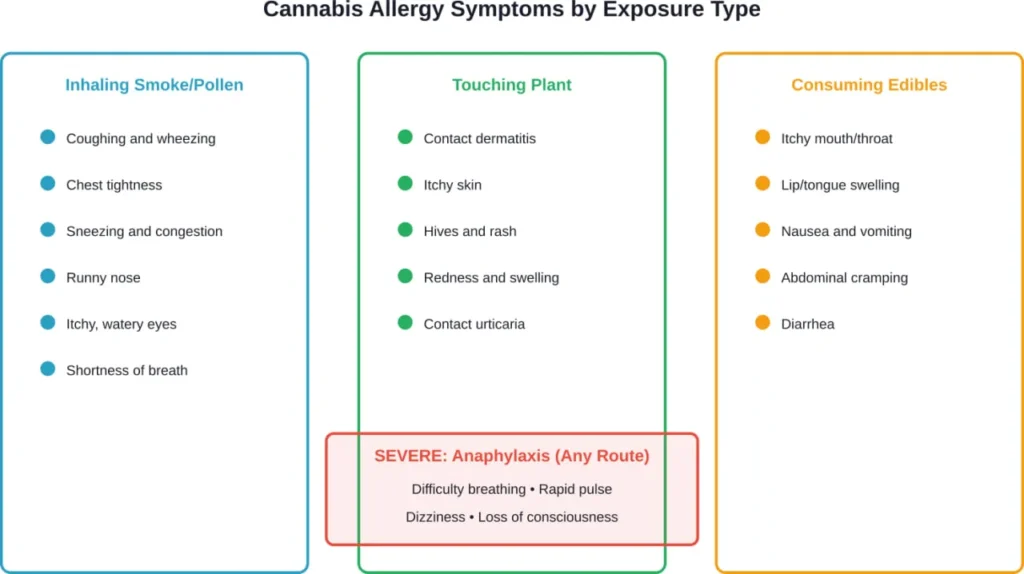
Marijuana allergy symptoms vary significantly depending on how someone encounters the plant. The type of exposure largely determines which symptoms appear.
Respiratory Symptoms From Inhaling
Smoking marijuana or inhaling its pollen can trigger asthma-like symptoms including coughing, wheezing, chest tightness, and shortness of breath. Many people experience allergic rhinitis symptoms: sneezing, runny nose, nasal congestion, and postnasal drip.
According to the CDC, workers in the cannabis industry face particular risk for work-related asthma and allergies. With approximately 428,000 people working in the legal cannabis industry as of January 2022, occupational exposure has become a significant concern.
Some individuals report conjunctivitis symptoms—red, itchy, watery eyes—after exposure to marijuana smoke or pollen.
Skin Reactions From Contact
Direct contact with cannabis plants commonly causes contact dermatitis. Symptoms include itching, redness, hives, and rash at the contact site. Research documents work-related contact urticaria in forensic science laboratory technicians who handle marijuana regularly.
These skin reactions can occur in growers, processors, and anyone handling raw cannabis material.
Oral and Digestive Symptoms
Consuming cannabis through edibles or hempseed products can trigger oral allergy syndrome. Symptoms include itching or swelling of the lips, mouth, tongue, and throat. Some individuals experience nausea, vomiting, abdominal cramping, or diarrhea after ingestion.
Severe Reactions: Anaphylaxis
Though rare, cannabis can trigger anaphylaxis—a severe, potentially life-threatening allergic reaction. Anaphylaxis symptoms develop rapidly and include difficulty breathing, rapid pulse, dizziness, loss of consciousness, and severe drops in blood pressure.
The CDC notes that some reactions are severe enough to require emergency treatment. Anyone experiencing anaphylaxis symptoms needs immediate medical attention and epinephrine administration.
What Causes Cannabis Allergies?
Cannabis allergy develops through sensitization to specific proteins found in the plant. Research has identified several allergenic proteins in Cannabis sativa, with the lipid transfer protein Can s 3 being the most clinically significant.
But why do some people develop cannabis allergies while others don’t? Several factors increase risk.
Increased Exposure
The primary driver of rising cannabis allergy cases is increased exposure. According to NIH research, approximately 192 million people (3.9% of the global population) use Cannabis sativa for medical or recreational purposes. As legalization expands and social acceptance increases, more individuals encounter cannabis through various routes.
Occupational exposure presents particularly high risk. Cannabis industry workers—growers, processors, dispensary employees, and laboratory technicians—face repeated contact with cannabis pollen, trichomes, and plant proteins. The CDC specifically highlights work-related asthma and allergies as concerns for this growing workforce.
Cross-Reactivity
Some marijuana allergic patients show positive skin prick test results to ragweed, pigweed, and tomato plants, indicating possible cross-reactivity. Cross-reactivity occurs when proteins in different plants share similar structures, causing the immune system to react to multiple related allergens.
People with existing plant allergies may have higher risk of developing cannabis allergy due to this cross-reactivity phenomenon.
Contamination Factors
Not all cannabis allergic reactions result from the plant itself. Several reports implicate contamination with Aspergillus mold as a potential allergen source in marijuana. Improperly stored cannabis can develop mold, and smoking or inhaling contaminated products may trigger allergic reactions to the mold rather than the plant.
Pesticides, chemicals, and other contaminants present in cannabis products may also cause adverse reactions that mimic or complicate true cannabis allergy.
Can CBD Products Trigger Allergies?
Yes, cannabidiol (CBD) products can also cause allergic reactions in sensitive individuals. CBD comes from the same Cannabis sativa plant, containing many of the same proteins that trigger marijuana allergies.
CBD products vary widely in composition. Some contain isolated CBD, while others include full-spectrum or broad-spectrum extracts containing additional plant compounds, terpenes, and proteins. Full-spectrum products carry higher allergy risk because they contain more plant proteins.
Additionally, CBD products may contain carrier oils (like hemp seed oil, coconut oil, or MCT oil), flavorings, and other ingredients that could trigger separate allergic reactions. Someone experiencing symptoms after using CBD should consider both the cannabis-derived components and other product ingredients as potential triggers.
Diagnosing Cannabis Allergy
Proper diagnosis requires medical evaluation by an allergist or immunologist. Self-diagnosis proves unreliable because cannabis allergy symptoms overlap with many other conditions.
Medical History Assessment
Diagnosis begins with detailed medical history. Allergists ask about symptom patterns, timing of reactions, exposure routes, and other allergies. Addressing marijuana exposure can be difficult because patients may not voluntarily disclose cannabis use, even when experiencing symptoms. Open, honest communication with healthcare providers proves essential for accurate diagnosis.
Skin Prick Testing
Skin prick testing represents the primary diagnostic tool. The Tessmer 2012 study describes preparing cannabis extract by macerating buds and flowers in water (5 ml) for 15 minutes and storing at 4°C until use within 3 months. A 2012 study by Tessmer describing the testing of 17 subjects with suspected marijuana hypersensitivity observed large wheal and flare responses suggesting type 1 sensitization to cannabis plant proteins.
The challenge? Diagnostic tests for cannabis allergy are still poorly standardized compared to common allergen testing.
Blood Tests
Specific IgE blood tests can detect antibodies to cannabis allergens. Research by Decuyper et al. examining hemp-specific IgE found a sensitivity of 86% but a low specificity of 32%. The basophil activation test (BAT) with crude cannabis extract was not superior in sensitivity or specificity compared to sIgE hemp testing.
Tests focusing on Can s 3 (the lipid transfer protein) showed equally performant results across BAT, sIgE, and SPT with positive and negative predictive values around 80% and 60% respectively, though clinical availability remains limited.
Diagnostic Challenges
Cannabis allergy diagnosis faces several obstacles. Lack of standardized testing reagents, variable allergen content in different cannabis strains, and potential contamination with molds or chemicals complicate accurate testing. Future studies with standardized extracts will be needed to determine specific allergens and develop better diagnostic strategies.
Treatment and Management Options
The most effective treatment for cannabis allergy is complete avoidance. But what about people who use marijuana for legitimate medical purposes or those exposed through work?
Avoidance Strategies
For recreational users, stopping cannabis use eliminates allergy symptoms. Medical marijuana patients should discuss alternative treatments with healthcare providers.
Cannabis industry workers face more complex challenges. The CDC recommends engineering controls (improved ventilation, enclosed processing systems), administrative controls (rotation schedules, limiting exposure time), and personal protective equipment (gloves, masks, protective clothing) to reduce occupational exposure.
Medication Management
Antihistamines can relieve mild allergic symptoms like sneezing, itching, and hives. Over-the-counter options include cetirizine, loratadine, and fexofenadine.
Nasal corticosteroid sprays help manage allergic rhinitis symptoms. Bronchodilators may be necessary for respiratory symptoms and asthma exacerbations.
For skin reactions, topical corticosteroids reduce inflammation and itching at contact sites.
Emergency Treatment for Anaphylaxis
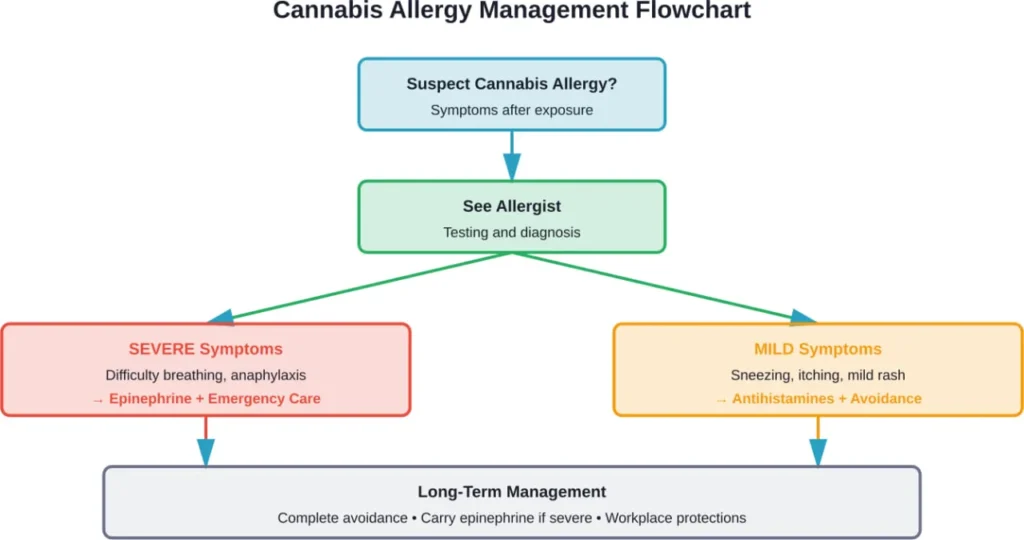
Individuals with history of severe reactions should carry epinephrine auto-injectors. Anaphylaxis requires immediate epinephrine administration followed by emergency medical care.
If someone experiences anaphylaxis symptoms, call emergency services immediately. Administer epinephrine if available, position the person lying down with legs elevated (unless vomiting—then turn them on their side), and stay with them until help arrives. Some people need more than one epinephrine injection; if symptoms don’t improve within 5-15 minutes or return, use a second auto-injector if available.
Allergy Immunotherapy
Currently, no established immunotherapy (allergy shots or tablets) exists for cannabis allergy. Research into cannabis-specific immunotherapy remains in early stages.
Prevention: Can Cannabis Allergy Be Avoided?
Preventing cannabis allergy development proves challenging once sensitization occurs. However, minimizing exposure can help prevent initial sensitization in susceptible individuals.
For cannabis industry workers, implementing proper workplace controls from the start of employment may reduce sensitization risk. Using personal protective equipment consistently, working in well-ventilated areas, and limiting direct plant contact all help minimize exposure.
Individuals with multiple plant allergies or strong family history of allergies may have higher risk and should exercise caution with cannabis exposure.
Once sensitization develops, preventing allergic reactions requires strict avoidance of all cannabis exposure routes—smoking, vaping, touching plants, consuming edibles, and inhaling smoke or pollen.
The Growing Research Landscape
Cannabis allergy remains a relatively new research field. Early case reports from the 1970s first described allergic reactions to marijuana, but systematic research only accelerated recently as legalization expanded.
Research published in medical journals emphasizes that cannabis allergy knowledge among allergists remains limited. As cannabis legalization continues expanding worldwide, researchers anticipate increasing allergy cases and growing need for improved diagnostic tools, standardized testing reagents, and treatment strategies.
Key research priorities include identifying all clinically significant cannabis allergens, developing standardized extracts for diagnostic testing, understanding cross-reactivity patterns with other plants, and potentially developing immunotherapy options for patients who need cannabis for medical purposes.
Workplace Considerations
The rapid expansion of the legal cannabis industry creates unique occupational health challenges. With approximately 428,000 workers in the U.S. cannabis industry as of January 2022, work-related asthma and allergies represent significant concerns.
Cannabis workers face exposure through multiple routes: inhaling pollen and plant particles, direct skin contact during cultivation and processing, and environmental exposure in grow facilities and dispensaries. Research documents occupational allergies in various cannabis-related professions, including growers, trimmers, processors, laboratory technicians, and dispensary staff.
Employers should implement comprehensive exposure control programs including engineering controls, work practice modifications, and personal protective equipment. Workers experiencing symptoms should report them promptly and seek medical evaluation.
| Occupation | Primary Exposure | Common Symptoms | Recommended Protection |
|---|---|---|---|
| Cannabis Grower | Pollen, plant contact | Rhinitis, asthma, contact dermatitis | Gloves, N95 respirator, ventilation |
| Processor/Trimmer | Plant material, trichomes | Respiratory symptoms, skin reactions | Gloves, mask, protective clothing |
| Laboratory Technician | Handling samples | Contact urticaria, respiratory | Gloves, fume hood, proper ventilation |
| Dispensary Staff | Product handling, ambient exposure | Mild rhinitis, eye symptoms | Hand hygiene, ventilation systems |
Cannabis Allergy in Medical Marijuana Patients
Cannabis allergy creates particularly challenging situations for medical marijuana patients who rely on cannabis for symptom management. Patients using marijuana to treat chronic pain, nausea, anxiety, or other conditions face difficult choices when allergic symptoms develop.
Medical marijuana patients experiencing allergic symptoms should consult both their prescribing physician and an allergist. Alternative treatment options may provide similar benefits without allergic complications. Some patients might tolerate different consumption methods—for example, switching from smoking to edibles, or vice versa—though this doesn’t work for everyone.
Patients should never ignore allergic symptoms or continue using cannabis if severe reactions occur. The risks of anaphylaxis outweigh potential therapeutic benefits.
Frequently Asked Questions
Yes, cannabis allergies can develop at any time, even in people who previously used marijuana without problems. Allergic sensitization occurs after repeated exposure, meaning someone might tolerate cannabis initially but develop allergies after months or years of use. Changes in cannabis strains, increased potency, or higher exposure frequency may trigger sensitization in previously unaffected individuals.
Exact prevalence remains unknown due to limited research and underreporting. However, allergists report increasing cannabis allergy cases as marijuana use expands. Research suggests cannabis allergy may be more common than previously recognized, particularly among heavy users and cannabis industry workers who experience repeated, high-level exposure. As legalization continues, allergists expect allergy prevalence to increase proportionally with usage rates.
Not typically, because CBD comes from the same Cannabis sativa plant containing the allergenic proteins that trigger marijuana allergies. However, reactions to CBD products might result from other ingredients like carrier oils, flavorings, or contaminants rather than the cannabis itself. Some people tolerate isolated CBD better than full-spectrum products containing more plant proteins. Anyone experiencing reactions to CBD products should undergo allergy testing to identify the specific trigger.
Cannabis allergy involves immune system activation and IgE antibody production, causing symptoms like hives, respiratory distress, or anaphylaxis that appear rapidly after exposure. Cannabis intolerance refers to non-immune adverse reactions—like nausea, dizziness, or headaches—that don’t involve the immune system. Allergies can be diagnosed through skin prick tests and IgE blood tests, while intolerance cannot. Allergic reactions tend to be more severe and potentially life-threatening.
Yes, cannabis allergy can trigger asthma attacks in susceptible individuals. Inhaling marijuana smoke or pollen may cause bronchoconstriction, wheezing, coughing, chest tightness, and difficulty breathing. Research published by the CDC specifically identifies work-related asthma as a concern for cannabis industry workers. People with pre-existing asthma face higher risk of severe respiratory reactions to cannabis allergen exposure. Anyone with asthma who experiences breathing difficulties after cannabis exposure should seek immediate medical attention.
Not usually, because standard allergy test panels don’t typically include cannabis allergens. Patients must specifically request cannabis allergy testing. Even then, diagnostic testing remains challenging because standardized cannabis extracts for testing are poorly developed. Allergists may prepare custom cannabis extracts or use hemp-specific IgE tests, though these show variable sensitivity and specificity. Anyone suspecting cannabis allergy should inform their allergist specifically about marijuana exposure to ensure appropriate testing.
Generally no, because hemp and marijuana both come from Cannabis sativa and contain the same allergenic proteins. Industrial hemp (containing less than 0.3% THC) shares the primary allergens with higher-THC marijuana strains. Someone allergic to marijuana will likely react to hemp seeds, hemp protein powder, hemp oil, and other hemp-derived products. Cross-reactivity between hemp and marijuana means avoiding all cannabis-derived products typically proves necessary for allergic individuals.
Key Takeaways
Cannabis allergy represents a real and growing health concern as marijuana use increases globally. Allergic reactions can range from mild annoyances to life-threatening emergencies, affecting recreational users, medical marijuana patients, and cannabis industry workers.
The most important points to remember:
- Cannabis allergies are legitimate IgE-mediated reactions to proteins in the marijuana plant
- Symptoms vary by exposure route and include respiratory problems, skin reactions, digestive issues, and potentially anaphylaxis
- Diagnosis requires medical evaluation by allergists using skin prick tests and IgE blood testing
- Treatment centers on complete cannabis avoidance, with medications managing breakthrough symptoms
- CBD products can trigger allergies just like traditional marijuana
- Cannabis industry workers face occupational exposure risks requiring workplace protections
- Anyone experiencing severe symptoms needs immediate emergency medical care
As cannabis legalization expands and usage increases, awareness of cannabis allergy becomes increasingly important for healthcare providers, users, and employers. Research continues developing better diagnostic tools and treatment options for this emerging allergy concern.
If you suspect cannabis allergy, don’t ignore symptoms or attempt self-diagnosis. Consult an allergist for proper evaluation and testing. Allergic reactions can worsen with repeated exposure, making early diagnosis and avoidance strategies essential for preventing severe complications.
