Quick Summary: While it’s not possible to get a traditional pimple inside your mouth (no oil glands exist there), several conditions create pimple-like bumps including canker sores, mucoceles, oral papillomas, and perioral dermatitis around the mouth. These bumps have different causes than facial acne and require specific treatments ranging from saltwater rinses to professional removal.
Ever noticed a suspicious bump inside your mouth and wondered if it’s a pimple? Here’s the thing—technically, you can’t get a true pimple inside your mouth. Real acne requires sebaceous glands (oil glands), and the oral mucosa doesn’t have them.
But that doesn’t mean those bumps aren’t real or bothersome. Several conditions create pimple-like lesions in and around your mouth. Some are harmless and disappear on their own. Others need professional treatment.
Let’s break down what’s actually happening when you spot these bumps.
Why Traditional Pimples Don’t Form Inside Your Mouth
Acne vulgaris develops when sebaceous glands produce excess oil that combines with dead skin cells and bacteria, clogging hair follicles. According to the American Academy of Dermatology, acne is the most common skin condition in the United States, affecting nearly 50 million Americans each year and typically begins during puberty, affecting 85% of adolescents.
The oral mucosa—the lining inside your mouth—lacks sebaceous glands entirely. No oil glands means no traditional acne formation. What people call a “pimple in the mouth” is actually one of several other conditions that mimic pimples.
That said, acne can definitely appear around your mouth on regular facial skin.
Common Conditions That Look Like Mouth Pimples
So what are those bumps? Here are the most common culprits.
Canker Sores (Aphthous Ulcers)
Canker sores are small, painful ulcers that develop on the soft tissues inside your mouth. They typically appear on the inside of cheeks, lips, tongue, or gums.
These sores usually have a white or yellowish center with a red border. Unlike cold sores, they’re not contagious and don’t appear on the outer surface of lips.
Common triggers include:
- Minor mouth injuries from dental work or aggressive brushing
- Stress or hormonal changes
- Certain foods (citrus, spicy foods, chocolate)
- Nutritional deficiencies (vitamin B12, zinc, iron)
- Autoimmune conditions
Most canker sores heal on their own within one to two weeks without treatment.
Oral Mucoceles (Mucous Cysts)
According to data from Cleveland Clinic, oral mucoceles are harmless, painless fluid-filled cysts that form on the inner surface of your mouth. People younger than 30 years old are most affected, with those between ages 3 and 20 making up 70% of cases.
These bumps develop when salivary glands become blocked or damaged, usually from accidentally biting your cheek or lip. The trapped mucus creates a soft, round, translucent bump.
Mucoceles typically appear on the lower lip, but can show up on the cheeks, tongue, or floor of the mouth. They’re usually painless unless they become large.

Cold Sores (Oral Herpes)
Cold sores are caused by the herpes simplex virus (HSV-1) and typically appear on or around the outer edges of lips. They start as small blisters that eventually break open and crust over.
Unlike canker sores, cold sores are highly contagious. They can spread through direct contact, shared utensils, or kissing.
The virus remains dormant in your body after initial infection and can reactivate due to stress, illness, sun exposure, or hormonal changes.
Oral Papillomas
Squamous papillomas are small, painless growths that can appear anywhere in the mouth. They’re caused by the human papillomavirus (HPV) and typically have a cauliflower-like appearance.
These bumps are usually harmless but should be evaluated by a healthcare provider to rule out more serious conditions.
Perioral Dermatitis: Pimples Around the Mouth
According to the National Institutes of Health, perioral dermatitis is a benign eruption consisting of small inflammatory papules and pustules or pink, scaly patches around the mouth. The condition most commonly affects young female adults.
This rash often looks like small, red, acne-like breakouts in people with light-colored skin and skin-colored breakouts in those with darker skin tones. The bumps can itch or cause a burning sensation.
Despite appearing around the mouth, perioral dermatitis can also affect skin around the nose and eyes, which is why some dermatologists call it periorificial dermatitis.
Common triggers include:
- Topical corticosteroid use on the face
- Heavy moisturizers or facial creams
- Fluorinated toothpaste
- Hormonal changes
The American Academy of Dermatology notes that if patients have been using topical corticosteroids to treat the eruption, abrupt discontinuation may lead to rebound flaring. The condition typically worsens temporarily before improving with appropriate treatment.
Treatment Options for Mouth Bumps
Treatment depends entirely on what’s causing the bump.
| Condition | Home Treatments | Professional Treatments |
|---|---|---|
| Canker Sores | Saltwater rinses, avoid trigger foods, over-the-counter gels | Prescription mouth rinses, topical corticosteroids for severe cases |
| Mucoceles | Warm compresses, avoid biting the area | Surgical removal or laser therapy for large or persistent cysts |
| Cold Sores | Antiviral creams (docosanol), ice packs, lip balm | Prescription antivirals (acyclovir, valacyclovir) |
| Perioral Dermatitis | Stop using facial steroids, switch toothpaste, gentle cleansers | Topical antibiotics (metronidazole), oral antibiotics (tetracyclines) |
When to See a Healthcare Provider
Most mouth bumps resolve without medical intervention. But certain warning signs warrant professional evaluation:
- Bumps that persist longer than two weeks
- Rapidly growing or changing lesions
- Bumps accompanied by fever or swollen lymph nodes
- Severe pain or bleeding
- Difficulty eating, drinking, or speaking
- Multiple recurring sores
Persistent oral lesions can sometimes indicate more serious conditions, including oral cancer or autoimmune diseases. Research published in the Journal of Immunology Research shows that oral signs are frequently the first manifestation of autoimmune diseases, with systemic lupus erythematosus showing skin damage in 85% of cases.
Drug-Induced Acne and Oral Effects
Certain medications can cause acne-like eruptions on the face, including around the mouth. According to NIH research, acneiform eruptions are acne vulgaris-like dermatoses characterized by papules, pustules, nodular, and cystic lesions, distinguished from true acne by sudden onset, uniformity of lesions, and dispersion outside seborrheic regions.
Medications that can cause acneiform eruptions include:
- Corticosteroids (topical or systemic)
- Epidermal growth factor receptor inhibitors (which frequently cause drug-induced acneiform eruptions, with a reported overall incidence ranging from 60% to 80%)
- Lithium
- Certain antiseizure medications
For acne treatment itself, isotretinoin is referred to by dermatologists as “the most effective treatment for severe acne” and can affect oral health. Consult your healthcare provider about potential oral effects during treatment.
Additionally, minocycline, commonly used for long-term acne treatment, can cause oral mucosal pigmentation as a recognized side effect.
Prevention Strategies
While you can’t prevent every mouth bump, certain habits reduce your risk:
- Practice gentle oral hygiene—avoid aggressive brushing
- Use a soft-bristled toothbrush
- Avoid foods that trigger canker sores in your case
- Manage stress through relaxation techniques
- Don’t bite your cheeks or lips
- Stay hydrated to maintain healthy oral mucosa
- For perioral dermatitis, avoid heavy facial products and fluorinated toothpaste
Good oral hygiene remains essential for preventing infections and maintaining overall mouth health.
Frequently Asked Questions
Don’t pop or squeeze bumps inside your mouth. Unlike facial pimples, oral bumps aren’t caused by clogged pores. Attempting to pop them can introduce bacteria, cause infection, or create scarring. If a mucocele ruptures on its own, rinse with warm salt water and maintain good oral hygiene.
Canker sores usually heal within one to two weeks without treatment. Mucoceles may persist for weeks or months and sometimes require removal. Cold sores typically last seven to ten days with or without treatment, though antivirals can shorten duration.
Most mouth bumps aren’t contagious. Canker sores and mucoceles can’t spread to others. Cold sores, however, are highly contagious during active outbreaks and can spread through direct contact or shared items like utensils or towels.
Canker sores appear inside the mouth on soft tissues and aren’t contagious. Cold sores appear on or around the outer lips, are caused by a virus (HSV-1), and are highly contagious. Cold sores start as fluid-filled blisters while canker sores are ulcers with white or yellow centers.
Yes, stress is a common trigger for canker sores. It can also trigger cold sore outbreaks in people who carry the herpes simplex virus. Stress management techniques may help reduce the frequency of stress-related mouth bumps.
Avoid alcohol-based mouthwashes, which can irritate sores and delay healing. Instead, rinse with warm salt water (one teaspoon salt in eight ounces warm water) three to four times daily. Some prescription mouth rinses specifically formulated for canker sores may help if over-the-counter options don’t work.
Nutritional deficiencies in vitamin B12, zinc, folate, or iron can increase susceptibility to canker sores. If you experience frequent mouth sores, ask your healthcare provider about testing for nutritional deficiencies.
The Bottom Line
That bump in your mouth probably isn’t a true pimple—the oral mucosa lacks the oil glands needed for acne formation. More likely, it’s a canker sore, mucocele, or another common oral condition.
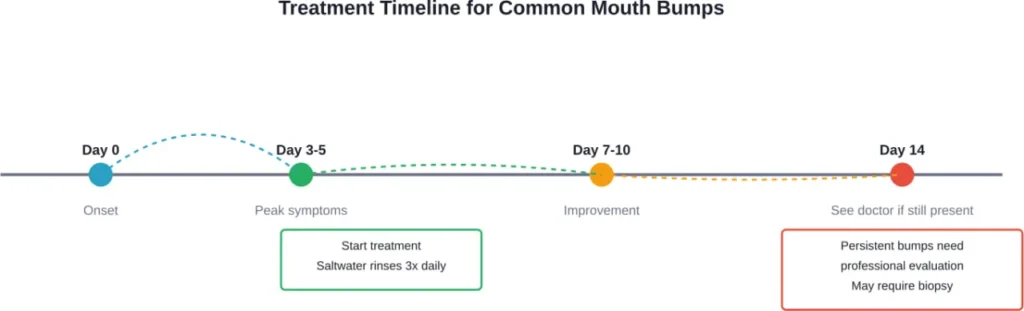
Most mouth bumps are harmless and resolve on their own with basic home care like saltwater rinses and avoiding irritants. However, persistent bumps lasting more than two weeks, rapidly changing lesions, or bumps with concerning symptoms deserve professional evaluation.
If you’re dealing with recurring mouth bumps or perioral acne that won’t clear up, consult a dentist or dermatologist. They can provide accurate diagnosis and targeted treatment to get you back to comfort.
Don’t ignore persistent oral changes—early detection makes all the difference for more serious conditions.
