Quick Summary: Yes, it’s entirely possible to get the flu twice in a month. Multiple influenza strains circulate simultaneously during flu season, and catching one strain doesn’t protect you from others. Reinfection can also occur if your immune system is weakened or if you’re exposed to a different viral strain shortly after recovery.
The idea sounds miserable, doesn’t it? Battling through fever, chills, and body aches only to find yourself sick again just weeks later.
But here’s the thing—it absolutely can happen. And it’s more common than most people realize.
According to research, median annual influenza infection rates were estimated at approximately 18% from 1968 to 2015, with substantial variation between years. Research indicates influenza infects approximately 20% of children and 5% of adults annually, though rates vary by year and location. With multiple strains circulating simultaneously, the possibility of sequential infections within the same month isn’t just theoretical.
Understanding why this happens requires looking at how influenza viruses behave, how immunity works, and what makes certain people more vulnerable to repeat infections.
Why Multiple Flu Infections Are Possible
The flu isn’t caused by a single virus. It’s an entire family of constantly changing pathogens.
According to the CDC, influenza viruses change through two primary mechanisms: antigenic drift and antigenic shift. Drift involves small mutations in surface proteins—hemagglutinin (HA) and neuraminidase (NA)—that allow the virus to evade immune recognition. These surface proteins are antigens, meaning they trigger immune responses.
When these proteins mutate even slightly, antibodies from a previous infection may not recognize the new variant. That’s why catching one flu strain doesn’t necessarily protect against another.
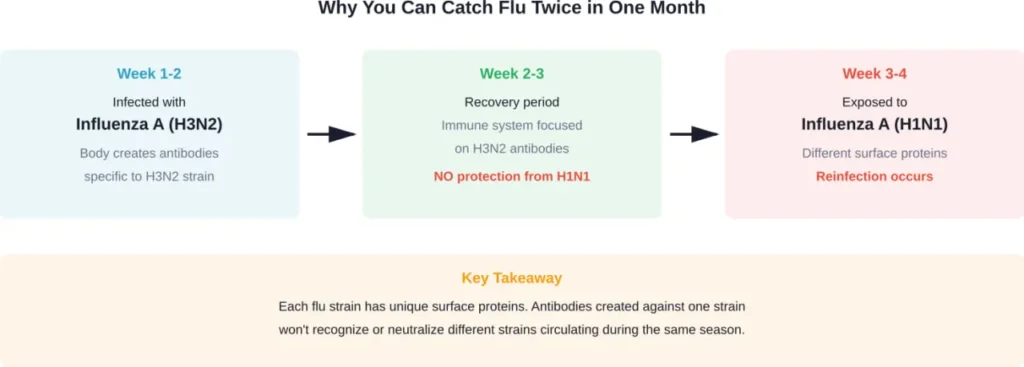
During any given flu season, multiple strains circulate at once. Influenza A subtypes like H1N1 and H3N2 can both be active simultaneously, along with Influenza B lineages. Catching H3N2 in early January provides zero protection against H1N1 later that month.
The Strain Diversity Problem
Seasonal influenza includes distinct viral lineages that don’t cross-protect. The WHO recommends that trivalent vaccines for the 2025-2026 northern hemisphere season contain protection against three different viruses—highlighting just how many variants circulate concurrently.
Each strain represents a separate infectious threat. Immunity to one doesn’t transfer to others.
What Increases Your Risk of Repeat Flu Infections
Not everyone faces the same likelihood of catching flu multiple times in a short period.
Certain factors significantly elevate risk. Age plays a major role—young children and adults over 65 experience different immune responses. According to CDC data, people with compromised immune systems and those 65 and older may experience lower protection levels even after vaccination.
Compromised Immune Function
When the immune system is already taxed from fighting one infection, vulnerability to new pathogens increases. The recovery period after influenza can leave the body in a weakened state for days or even weeks.
During this window, exposure to a different flu strain can lead to reinfection before the immune system fully rebuilds its defenses.
Medical research shows that influenza can exacerbate underlying conditions like pulmonary or cardiac disease, lead to secondary bacterial pneumonia, or occur as coinfection with other pathogens. These complications further strain immune resources.
Environmental and Behavioral Factors
High-exposure environments dramatically increase infection risk. Schools, healthcare facilities, public transportation, and large gatherings all facilitate viral transmission.
Someone working in healthcare or teaching might encounter multiple flu strains within days. Behavioral factors matter too—inadequate hand hygiene, touching the face frequently, and close contact with symptomatic individuals all raise exposure likelihood.
| Risk Factor | Why It Matters | Impact Level |
|---|---|---|
| Age (under 5 or over 65) | Immune system less robust or declining | High |
| Chronic health conditions | Baseline immune function compromised | High |
| Recent illness | Immune system still recovering from first infection | Very High |
| High-exposure occupation | Frequent contact with infected individuals | Moderate to High |
| Unvaccinated status | No baseline immunity to circulating strains | High |
| Poor nutrition or stress | Weakens overall immune response | Moderate |
How to Tell If It’s Actually the Flu Again
Respiratory illness caused by influenza can be difficult to distinguish from illness caused by other respiratory pathogens based on symptoms alone, according to CDC guidance.
That presents a diagnostic challenge. Is it truly a second flu infection, or could it be COVID-19, RSV, or even a bacterial infection?
Symptom Overlap and Diagnostic Testing
Classic flu symptoms include sudden fever, body aches, fatigue, dry cough, and headache. But these symptoms aren’t unique to influenza.
Healthcare providers often rely on symptom presentation combined with epidemiological information to make treatment decisions. Early diagnosis matters because antiviral treatments like oseltamivir work best when started within 48 hours of symptom onset.
Testing becomes essential when symptoms return shortly after recovery. Rapid influenza diagnostic tests can confirm whether influenza virus is present, though they’re not always perfectly sensitive or specific.
More comprehensive respiratory pathogen panels can distinguish between flu, COVID-19, RSV, and other causes. This differentiation guides appropriate treatment and prevents unnecessary antibiotic use.
The Role of Vaccination in Preventing Repeat Infections
Flu vaccines aren’t perfect, but they remain the most effective preventive tool available.
Research from one study found approximately 45% of the MESA population was vaccinated against influenza each year. These vaccines work by exposing the immune system to inactivated or weakened virus components, prompting antibody production before natural exposure occurs.
Here’s what matters: flu vaccines typically protect against three or four different strains simultaneously. That means even if you catch one strain not well-matched to the vaccine, you still have protection against the others.
Why Vaccination Reduces (But Doesn’t Eliminate) Risk
Vaccination significantly reduces the likelihood of severe illness and complications, even when it doesn’t prevent infection entirely. Studies demonstrate that vaccinated individuals who do contract flu experience shorter symptom duration and lower hospitalization rates.
For preventing sequential infections within one month, vaccination provides partial protection by reducing overall circulating virus in communities. When more people are vaccinated, transmission rates drop, lowering everyone’s exposure risk.
That said, vaccines aren’t 100% effective. Viral mutations, individual immune variation, and timing of vaccination all affect protection levels.

Practical Steps to Prevent Reinfection
Prevention strategies extend beyond vaccination.
Basic hygiene remains crucial. Frequent handwashing with soap and water for at least 20 seconds removes viral particles before they can enter the body. Alcohol-based hand sanitizers work when soap isn’t available.
Avoiding face-touching reduces transmission from contaminated hands to mucous membranes in the eyes, nose, and mouth—the primary entry points for influenza virus.
Isolation and Recovery Protocols
After recovering from flu, the body needs time to rebuild immune strength. Rushing back to high-exposure environments too quickly increases reinfection risk.
Generally speaking, individuals remain most contagious during the first three to four days after symptoms begin. Fever-free status for 24 hours without fever-reducing medications typically indicates reduced contagiousness.
However, coughs can persist for weeks and may still spread virus particles, albeit at lower concentrations.
Proper nutrition, adequate sleep, stress management, and hydration all support immune recovery during the post-infection period. These factors strengthen the body’s ability to resist subsequent exposures.
When to Consider Extended Precautions
For those at high risk—whether due to age, chronic conditions, or immune compromise—extended precautions make sense during peak flu season.
Wearing masks in crowded indoor spaces reduces exposure to respiratory droplets. Avoiding sick individuals seems obvious but bears repeating. Social distancing during conversations helps, particularly when someone is coughing or sneezing.
Cleaning frequently-touched surfaces at home and work removes viral particles that can survive on hard surfaces for up to 48 hours.
When Repeat Flu Symptoms Warrant Medical Attention
Not all flu cases require emergency care. But certain warning signs demand immediate medical evaluation.
Difficulty breathing or shortness of breath signals potential pneumonia or respiratory distress. Persistent chest pain or pressure shouldn’t be ignored—research on laboratory-confirmed influenza has documented cases of acute cardiac injury, with some studies finding myocardial infarctions among affected individuals.
Sudden dizziness, confusion, severe or persistent vomiting, and symptoms that improve then suddenly worsen all indicate potential complications requiring professional assessment.
For children, additional warning signs include bluish skin color, rapid breathing, fever with rash, and inability to wake up or interact normally.
High-Risk Populations and Medical Intervention
According to WHO, 99% of deaths in children under 5 years of age with influenza-related lower respiratory tract infections are in developing countries. In industrialized nations, most influenza-associated deaths occur among people aged 65 or older.
These populations benefit most from early antiviral intervention. Medications like oseltamivir can reduce symptom duration and severity when started within 48 hours of symptom onset.
For repeat infections occurring within a month, medical evaluation helps confirm the diagnosis and rule out complications like bacterial superinfection or coinfection with other pathogens.
| Symptom | Severity Level | Action Required |
|---|---|---|
| Difficulty breathing | Emergency | Seek immediate medical care |
| Chest pain or pressure | Emergency | Seek immediate medical care |
| Sudden confusion or dizziness | Emergency | Seek immediate medical care |
| Fever above 103°F lasting 3+ days | Urgent | Contact healthcare provider same day |
| Symptoms improve then worsen | Urgent | Contact healthcare provider same day |
| Severe fatigue preventing daily activities | Moderate | Schedule medical appointment within 48 hours |
| Persistent cough after 2 weeks | Moderate | Schedule medical appointment within a few days |
Understanding Immunity After Flu Infection
Recovering from flu does create immunity. Just not universal immunity.
The immune system generates antibodies specifically targeting the surface proteins of the infecting strain. These antibodies circulate in the bloodstream and mucous membranes, ready to neutralize that exact strain if encountered again.
This protection can last months to years for that specific strain. But remember—influenza viruses mutate constantly through antigenic drift.
Research on reconstructed influenza A/H3N2 infection histories shows variation in incidence and antibody dynamics over the life course. The immune response isn’t static; it evolves based on lifetime exposure history.
Cross-Reactive Immunity Limitations
Some cross-reactive antibody responses do occur between related strains, but they’re typically weaker than strain-specific immunity.
According to CDC research, before vaccination, no cross-reactive antibody to novel strains existed among children. Among adults, cross-reactive antibody was detected in 6%-9% of those aged 18-64 years and in 33% of those aged >60 years.
These low rates explain why new or drifted strains can infect even recently recovered individuals.
Frequently Asked Questions
Reinfection can occur within days if exposed to a different strain. While recovery from one flu strain provides immunity against that specific virus, it offers no protection against other circulating strains. The typical contagious period ends about 24 hours after fever resolves, but exposure to a new strain during or immediately after recovery can lead to sequential infections.
No. Flu vaccines contain inactivated virus or viral components that cannot cause infection. Some people experience mild side effects like soreness or low-grade fever as the immune system responds, but this isn’t influenza. Vaccines protect against multiple strains simultaneously, actually reducing the likelihood of getting flu twice by providing broader immunity.
New infections typically present with sudden onset of acute symptoms—high fever, severe body aches, and intense fatigue. Lingering symptoms from the first infection tend to be milder and gradually improving, particularly persistent cough or fatigue. If symptoms significantly worsen after improvement or new fever develops after being fever-free for 24+ hours, it likely indicates new infection or complication requiring medical evaluation.
Not necessarily. Multiple infections in a short period can result from exposure to different strains rather than immune deficiency. However, certain conditions—chronic illness, immunosuppressive medications, extreme stress, poor nutrition, or age-related immune decline—do increase susceptibility. If repeat infections become a pattern, discussing immune function with a healthcare provider makes sense.
Testing helps confirm whether symptoms represent new influenza infection, a different respiratory pathogen like COVID-19 or RSV, or complications from the initial infection. This information guides appropriate treatment, particularly since antiviral medications work best within 48 hours of symptom onset. For high-risk individuals or those with severe symptoms, testing becomes especially important for proper management.
Unlikely but possible in unusual circumstances. Typically, individuals stop shedding significant virus amounts 5-7 days after symptom onset, though immunocompromised people may shed virus longer. By the time a second infection occurs, the first has usually resolved its contagious phase. However, overlapping infections could theoretically occur if exposure to a second strain happens during the tail end of the first infection’s contagious period.
Prioritize rest, hydration, and nutrition to support immune recovery. Consider antiviral medication if within 48 hours of symptom onset, especially for high-risk individuals. Avoid returning to work or high-exposure environments until fever-free for 24 hours without medication. Manage symptoms with appropriate over-the-counter medications, maintain good hygiene to prevent spreading to others, and seek medical attention if symptoms worsen or complications develop.
The Bottom Line on Repeat Flu Infections
Getting the flu twice in a month is medically plausible and more common than many realize.
Multiple influenza strains circulate simultaneously during flu season. Catching one provides no immunity against others. Add in viral mutation through antigenic drift, and the picture becomes clearer—sequential infections aren’t rare anomalies but predictable consequences of how influenza viruses behave.
Prevention requires layered strategies. Vaccination remains the cornerstone, providing protection against multiple strains and reducing disease severity even when breakthrough infections occur. Basic hygiene practices—handwashing, avoiding face-touching, cleaning surfaces—reduce viral transmission.
For those recovering from flu, allowing adequate time for immune system recovery before resuming high-exposure activities reduces reinfection risk. Proper nutrition, sleep, and stress management support immune function during this vulnerable period.
When symptoms return or worsen after improvement, medical evaluation ensures appropriate diagnosis and treatment. Early antiviral intervention makes a meaningful difference in outcomes, particularly for high-risk populations.
The reality is simple: influenza viruses are diverse, constantly changing, and highly contagious. Understanding these characteristics empowers better prevention and response strategies, reducing the likelihood of experiencing multiple infections in a short timeframe.
Experiencing flu symptoms for the second time this month? Don’t wait—consult a healthcare provider to confirm the diagnosis and explore treatment options that can reduce symptom severity and duration.
