Quick Summary: No, you cannot sweat out a fever. Sweating is a result of the body cooling down as fever breaks naturally, not a cure. Artificially inducing sweat through extra blankets or exercise doesn’t speed recovery and may cause dangerous dehydration or overheating.
It’s advice that’s been passed down for generations: pile on the blankets, crank up the heat, and sweat out that fever. But does this folk remedy actually work, or is it just another health myth that refuses to die?
The short answer? Sweating doesn’t cure a fever—it’s simply what happens when your fever breaks on its own. Let’s dig into the science behind fevers, why the sweating myth persists, and what actually helps when your body temperature spikes.
What Is a Fever, and Why Does It Happen?
A fever is your body’s natural defense mechanism, not the enemy itself. According to research published in StatPearls, fever represents an elevation of the body’s core temperature above the normal set-point regulated by the hypothalamus in the brain.
Normal body temperature averages around 98.6°F (37°C), though this varies by measurement method. The same research notes that oral temperatures average 36.57°C (97.83°F), while rectal temperatures run slightly higher at 37.04°C (98.67°F).
When your immune system detects an infection or inflammatory trigger, it releases immunological mediators that signal the hypothalamus to raise the body’s temperature set-point. This elevated temperature creates a less hospitable environment for many pathogens and enhances immune function.
Common causes of fever include:
- Viral infections (colds, flu, COVID-19)
- Bacterial infections
- Inflammatory conditions
- Heat-related illness
- Certain medications
- Autoimmune disorders
The Sweating Myth: Where Did It Come From?
The belief that sweating cures fever likely stems from a simple observation: people often sweat when their fever breaks. But correlation isn’t causation.
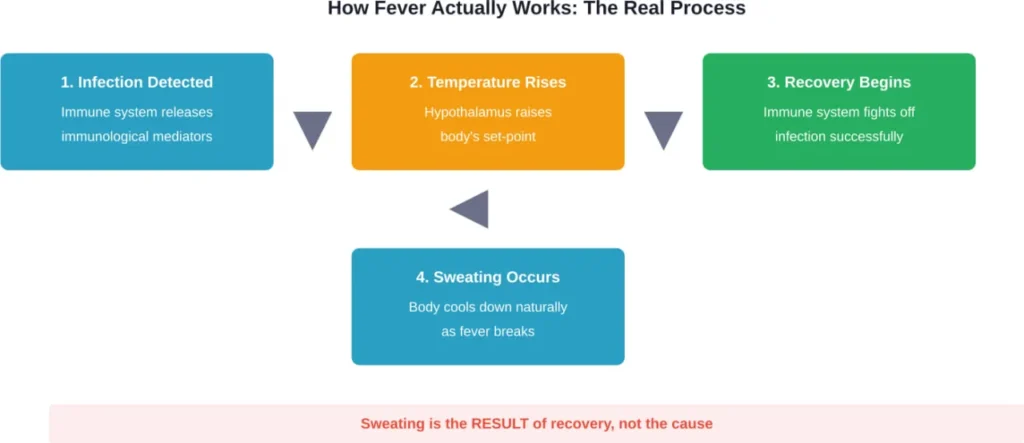
Here’s what actually happens. When the underlying infection improves, the immune system stops signaling for elevated temperature. The hypothalamus lowers the body’s set-point back to normal. Now the body needs to shed excess heat—and sweating is one mechanism it uses to cool down.
So sweating is the result of recovery, not the cause. It’s the body returning to baseline, not fighting off the illness.
Why Trying to Sweat Out a Fever Is Dangerous
Deliberately inducing sweat—through extra blankets, hot baths, or exercise—doesn’t just fail to help. It can make things worse.
Dehydration Risk
According to the CDC, maintaining proper hydration is critical during illness. When someone with a fever bundles up excessively, the body loses fluids through increased perspiration without any therapeutic benefit. The CDC recommends that for moderate activity in moderate conditions, each worker should drink 1 cup of water every 15 to 20 minutes—and fever increases fluid needs even more.
Dehydration during fever can lead to:
- Dizziness and confusion
- Rapid heart rate
- Decreased urination
- Worsening fever symptoms
- Prolonged recovery time
Overheating Danger
Research on heat-related illness shows that adding external heat when the body is already running hot creates a dangerous situation. The body struggles to regulate temperature effectively, potentially leading to heat exhaustion or worse.
A study on farmworker heat illness published by the CDC identified concerning beliefs about cooling treatments after heat exposure. Some workers believed that cooling should be avoided after heat exposure—a myth that parallels the fever-sweating misconception and can have serious health consequences.
Exercise Makes It Worse
Working out to “burn off” a fever puts additional metabolic stress on an already taxed system. Exercise raises core body temperature further and diverts energy away from immune function toward muscle activity.
What Actually Helps Manage a Fever
Instead of trying to sweat it out, focus on evidence-based fever management strategies.
| Strategy | How It Helps | Best Practice |
|---|---|---|
| Stay Hydrated | Replaces fluid lost through fever and supports immune function | Drink water, clear broths, or electrolyte solutions regularly |
| Rest | Allows body to direct energy toward fighting infection | Get adequate sleep and avoid strenuous activity |
| Light Clothing | Allows body to regulate temperature naturally | Wear breathable fabrics and use light bedding |
| Cool Environment | Helps prevent overheating without forcing temperature down | Keep room at comfortable temperature |
| Medication | Reduces fever and associated discomfort | Use acetaminophen or ibuprofen as directed |
Temperature Regulation Physiology
According to research in StatPearls on temperature regulation, the body has sophisticated mechanisms for maintaining thermal balance. These include vasodilation, sweating, and behavioral adaptations. The hypothalamus orchestrates these responses automatically—external interference typically disrupts rather than helps this process.
When fever is present, the body has deliberately raised its set-point. Fighting against this natural defense by artificially cooling (ice baths) or heating (bundling up) interferes with the immune response.
When to Seek Medical Attention
While most fevers resolve on their own, certain situations require professional evaluation.
For infants and young children, seek immediate medical care when:
- An infant 3 months or younger has a temperature of 100.4°F (38°C) or higher
- A child between 3 months and 2 years has a rectal temperature greater than 102°F (39°C) lasting more than 24 hours
- Any unexplained fever accompanied by lethargy, rash, or difficulty breathing
For adults, contact a healthcare provider if:
- Fever exceeds 103°F (39.4°C)
- Fever persists longer than three days
- Severe symptoms accompany the fever (chest pain, difficulty breathing, severe headache, confusion)
- You have a compromised immune system

Frequently Asked Questions
Yes, sweating often accompanies a fever breaking, but it’s a sign of recovery already in progress—not something that causes recovery. The body sweats to cool down after the hypothalamus has lowered the temperature set-point back to normal.
No, using a sauna during a fever is dangerous. It adds external heat when the body is already overheated, increasing the risk of dehydration and heat-related complications. Avoid saunas, steam rooms, and hot tubs until the fever has completely resolved.
Neither extreme is recommended. Wear light, comfortable clothing and maintain a moderate room temperature. The body’s thermoregulatory system works best when not fighting against artificial heating or cooling.
For adults, consult a healthcare provider if fever persists longer than three days. For infants under 3 months, any fever of 100.4°F or higher requires immediate medical attention. Children between 3 months and 2 years should be evaluated if fever exceeds 102°F for more than 24 hours.
Water doesn’t directly reduce fever, but proper hydration is essential during illness. Fever increases fluid loss through perspiration and increased metabolic activity. Staying well-hydrated supports immune function and helps prevent dehydration-related complications.
Individual variation in sweating patterns relates to differences in eccrine sweat gland density, autonomic nervous system responses, and hydration status. According to research on eccrine sweating mechanisms, these factors influence how much people sweat during heat stress—including fever.
No, exercise during any fever is not recommended. Even low-grade fever indicates active immune response, and exercise diverts energy away from fighting infection while raising body temperature further. Rest is the appropriate activity until fever resolves completely.
The Bottom Line
The myth of sweating out a fever persists despite clear scientific evidence against it. Fever is a deliberate immune response, and sweating is simply what happens when that fever naturally resolves—not a treatment strategy.
Artificially inducing sweat through bundling up, hot baths, or exercise doesn’t speed recovery. It creates unnecessary risks including dehydration and overheating.
The best approach? Support your body with rest, hydration, comfortable clothing, and appropriate medication when needed. Let your sophisticated thermoregulatory system do its job without interference. And if fever persists or worsens, seek medical evaluation rather than trying home remedies that don’t work.
Trust the science, not the sweating myth. Your immune system knows what it’s doing—give it the support it actually needs.
