Quick Summary: Yes, you can be allergic to the sun—though it’s technically not a true allergy. Polymorphous light eruption (PMLE) is the most common sun-related skin condition, causing itchy rashes after UV exposure. Other conditions like solar urticaria and photoallergic reactions can also trigger sun sensitivity.
The first warm day of spring arrives, and within hours of basking in the sunshine, your skin erupts into an itchy, red rash. Sound familiar?
While the term “sun allergy” gets tossed around casually, what’s actually happening on your skin is more complex than a simple allergic reaction. According to the National Institutes of Health, polymorphous light eruption is the most common idiopathic photodermatosis worldwide—a condition where your skin reacts abnormally to ultraviolet radiation.
But here’s the thing: several different conditions can cause sun-related skin reactions, and understanding which one affects you matters for proper treatment.
What Does “Sun Allergy” Actually Mean?
The term “sun allergy” serves as an umbrella descriptor for several conditions that cause skin reactions after sun exposure. These aren’t true allergies in the technical sense—where your immune system reacts to a foreign protein like pollen or peanuts.
Instead, these conditions involve abnormal skin responses to ultraviolet radiation. The most common types include polymorphous light eruption, solar urticaria, and photoallergic contact dermatitis.
Research from the National Institutes of Health shows that PMLE appears to cluster in families. Studies found the prevalence was 21% in monozygotic twins and 18% in dizygotic twins, suggesting a strong genetic component.
Polymorphous Light Eruption: The Most Common Culprit
Polymorphous light eruption accounts for roughly 70% of all sun-related skin reactions. This condition typically affects young women with lighter skin tones who live in regions with distinct seasonal changes.
The NIH defines PMLE as a delayed, abnormal cutaneous reaction to UV radiation. Unlike a sunburn that appears within hours, PMLE symptoms emerge hours to days after exposure—most commonly during spring or early summer when your skin hasn’t adapted to stronger UV levels yet.
Why the Name “Polymorphous”?
The “polymorphous” part refers to how the rash looks different from person to person. One individual might develop small red bumps, while another gets larger raised patches or tiny blisters.
That said, each person’s rash typically stays consistent. If you get small papules this year, you’ll likely see the same pattern next spring.
The Hardening Effect
Here’s something interesting: many people with PMLE experience improvement as summer progresses. This “hardening” phenomenon happens because repeated UV exposure gradually desensitizes the skin.
Research indicates that sun exposure between 30 minutes to several hours can trigger PMLE, with the rash appearing several minutes to hours later. The condition often presents cyclically—beginning in spring and fading by autumn.
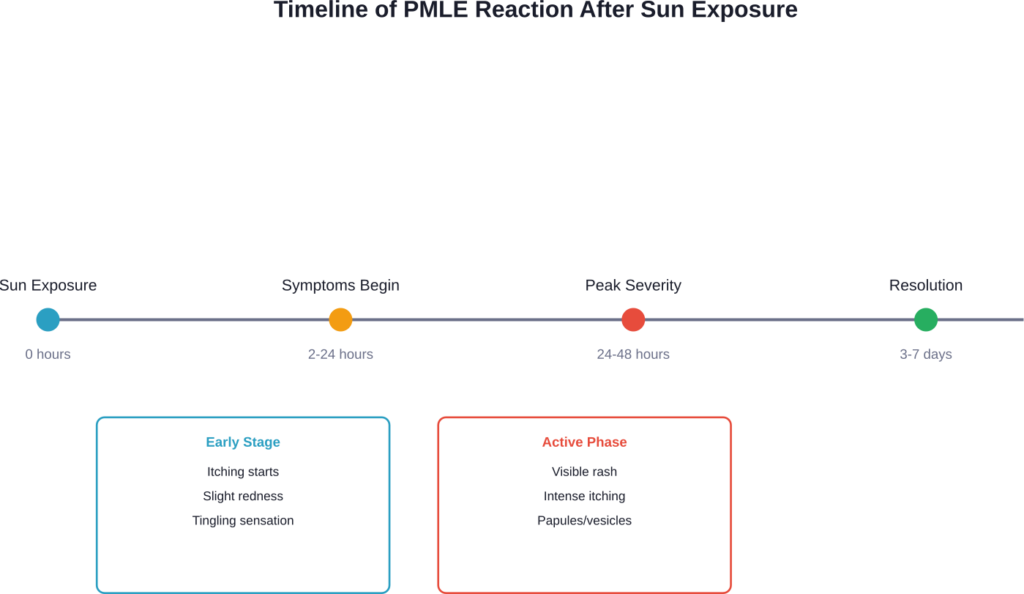
Solar Urticaria: A Rarer Form of Sun Sensitivity
Solar urticaria represents a much less common photodermatosis. According to research published through the NIH, its pathogenesis most likely involves an allergic type I reaction to an autoantigen activated by UV radiation or visible light.
The distinguishing feature? Speed. Solar urticaria produces hives within minutes of sun exposure—not hours or days like PMLE.
Individual hives typically fade within 30 minutes to two hours. However, they return immediately upon repeat sun exposure. For severe cases, this can be severely disabling, limiting daily activities and significantly reducing quality of life.
Photoallergic Contact Dermatitis: When Substances React With Sunlight
This condition occurs when certain substances on your skin react chemically when exposed to UV radiation. The American Academy of Dermatology notes that foods, medications, and skincare products can trigger symptoms like itching, redness, blistering, or burning.
Research from the North American Contact Dermatitis Group analyzed 454 patients tested between 2009-2020. Of the 119 positive photopatch tests, sunscreen agents comprised 88.2% of those positive reactions, with benzophenones being the most common photoallergens. Benzophenones were the most common among sunscreen photoallergens.
That’s right—sunscreen ingredients themselves can sometimes cause sun-related reactions. The irony isn’t lost on anyone dealing with this condition.
| Condition | Onset Time | Duration | Common Triggers |
|---|---|---|---|
| Polymorphous Light Eruption | 2-24 hours after exposure | 3-7 days | UVA and UVB rays, spring/summer sun |
| Solar Urticaria | Within minutes | 30 minutes to 2 hours | UV radiation, sometimes visible light |
| Photoallergic Contact Dermatitis | 24-48 hours after exposure | Several days to weeks | Sunscreens, medications, fragrances + UV |
Common Symptoms to Watch For
Recognizing sun allergy symptoms helps distinguish them from ordinary sunburn. The NIH reports that PMLE can significantly impair quality of life, leading to social avoidance, anxiety, and occupational limitations.
Classic PMLE Symptoms
The most common presentations include itchy red bumps, raised patches, or small blisters on sun-exposed areas. These typically appear on the chest, arms, legs, and back of hands—areas that see sudden increased sun exposure after winter months.
Interestingly, the face is often spared, possibly because facial skin receives more consistent year-round sun exposure. Research notes recognized variants including juvenile spring eruption, which usually affects the ear helices of young boys.
PMLE Sine Eruption
Some individuals experience an unusual variant where intense itching occurs without visible lesions. This “PMLE sine eruption” can be particularly frustrating because there’s no visible rash to show healthcare providers.
Who Gets Sun Allergies?
Certain factors increase susceptibility to photodermatoses. Analysis of North American photopatch testing data from 2009-2020 found that most tested patients were female (70.3%), between 21-60 years old (66.7%), and White (66.7%).
But genetics matter significantly. The genetic component shows that if your parents or siblings have PMLE, your chances increase substantially.
People with connective tissue diseases like lupus also show higher rates of photosensitivity. Research found that 70% of CLE patients reported adverse reactions to sunlight.
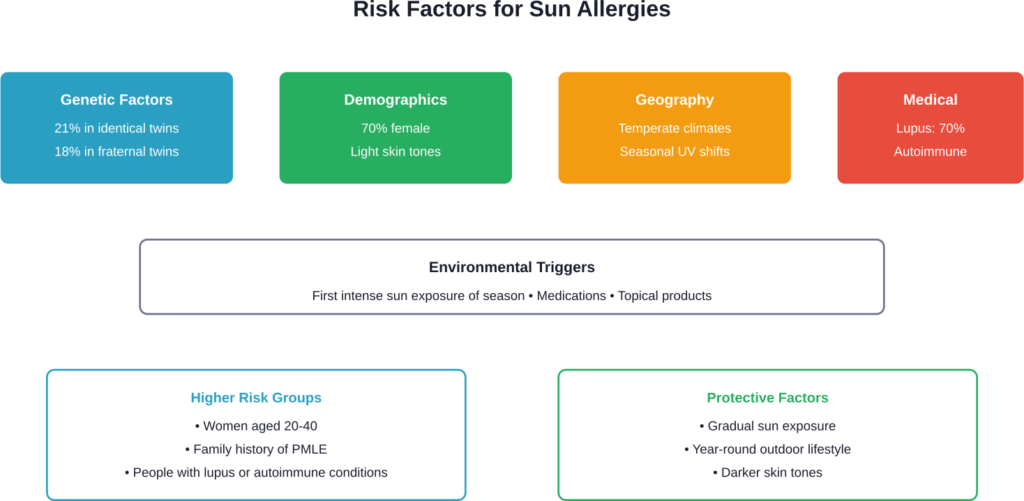
Diagnosis and Testing
Healthcare providers typically diagnose sun allergies through clinical examination and patient history. The appearance of lesions, timing relative to sun exposure, and pattern of recurrence provide strong diagnostic clues.
For unclear cases, photopatch testing becomes necessary. This specialized test involves applying potential allergens to the skin, then exposing those areas to controlled UV light.
Treatment and Management Options
Despite its benign course, PMLE can significantly impact daily life. The NIH notes it can lead to social avoidance, anxiety, and occupational limitations. Treatment approaches vary based on severity.
Avoidance Strategies
The most effective strategy involves limiting sun exposure during peak UV hours (10 AM to 4 PM). Protective clothing, wide-brimmed hats, and seeking shade provide first-line defense.
Remember that even on cloudy days, exposure reaches about 80% of the ultraviolet light present on sunny days. Water activities require extra caution since water reflects up to 80% of the sun’s rays.
Preventive Phototherapy
Cochrane review research indicates that controlled UV exposure before peak sun season can help prevent PMLE. This “hardening” approach involves gradually increasing UV doses in clinical settings during late winter or early spring.
The treatment essentially trains the skin to tolerate higher UV levels before seasonal exposure begins.
Topical and Systemic Treatments
Topical corticosteroids can reduce inflammation during flare-ups. For severe cases, oral antihistamines help control itching, while antimalarial medications like hydroxychloroquine may be prescribed for refractory cases.
| Treatment Type | Best For | How It Works |
|---|---|---|
| Sun Avoidance | All severities | Prevents UV exposure that triggers reactions |
| Preventive Phototherapy | Moderate to severe PMLE | Gradually desensitizes skin before sun season |
| Topical Corticosteroids | Active flare-ups | Reduces inflammation and itching |
| Oral Antihistamines | Itching control | Blocks histamine response |
| Antimalarials | Severe, refractory cases | Modulates immune response to UV |
Living With Sun Sensitivity
Managing chronic sun sensitivity requires lifestyle adjustments. Planning outdoor activities for morning or late afternoon hours helps minimize exposure during peak UV times.
For those with photoallergic contact dermatitis, identifying and eliminating the triggering substance proves crucial. This often means switching sunscreens, avoiding certain medications, or eliminating specific skincare products.
The good news? Many people find their symptoms improve with age or with consistent gradual sun exposure that allows their skin to adapt.
When to See a Healthcare Provider
Consult a dermatologist if sun-exposed skin consistently develops rashes, especially if over-the-counter treatments don’t help. Severe reactions involving widespread hives, difficulty breathing, or systemic symptoms require immediate medical attention.
Photopatch testing becomes valuable when the specific trigger remains unclear or when symptoms don’t match typical PMLE patterns.
Prevention Strategies That Work
Research supports several evidence-based prevention approaches. Gradual increase in sun exposure during early spring helps many individuals build tolerance before peak summer UV levels arrive.
Broad-spectrum sunscreens with SPF 30 or higher provide protection—but choose physical blockers (zinc oxide, titanium dioxide) if chemical sunscreens trigger reactions.
Indoor lunches during work hours can make a significant difference in daily UV exposure. Small adjustments accumulate into meaningful protection over time.
Frequently Asked Questions
Yes, polymorphous light eruption commonly first appears in young adults, typically between ages 20-40. While some people experience symptoms from childhood, many develop sun sensitivity later in life without prior history.
No, these are distinct conditions. Sun allergies involve reactions to ultraviolet radiation, while heat urticaria responds to temperature increases regardless of UV exposure. Sun allergies occur even in cool weather if UV levels are high.
Many people experience improvement as summer progresses due to the hardening effect, where repeated exposure gradually desensitizes skin. Some individuals also see symptoms diminish with age, though this varies considerably.
Absolutely—in fact, sunscreen remains essential. However, some chemical sunscreen ingredients trigger photoallergic reactions. Physical sunscreens containing zinc oxide or titanium dioxide typically cause fewer reactions than chemical formulations.
Controlled UV exposure in medical settings under dermatologist supervision can help prevent PMLE through gradual desensitization. However, commercial tanning beds are not recommended—they provide uncontrolled UV doses and increase skin cancer risk significantly.
Yes, several medication classes increase photosensitivity, including some antibiotics (tetracyclines, fluoroquinolones), diuretics, NSAIDs, and certain blood pressure medications. Always check medication information and discuss photosensitivity risks with your pharmacist.
Children can develop photodermatoses, including a variant called juvenile spring eruption that typically affects boys’ ears. However, PMLE more commonly begins in young adulthood. Any persistent rash after sun exposure in children warrants medical evaluation.
Conclusion
So, is it possible to be allergic to the sun? The answer is yes—though the mechanism differs from traditional allergies. Polymorphous light eruption affects millions worldwide, causing uncomfortable rashes that can significantly impact quality of life.
Understanding the specific type of sun sensitivity matters for effective management. Whether dealing with PMLE, solar urticaria, or photoallergic contact dermatitis, treatment options exist ranging from simple avoidance strategies to preventive phototherapy and medications.
The condition doesn’t have to keep you locked indoors. With proper diagnosis, strategic sun protection, and appropriate treatment, most people successfully manage their symptoms and enjoy outdoor activities safely.
If you’re experiencing persistent sun-related rashes, consult a dermatologist. Proper diagnosis opens the door to targeted treatment and better quality of life during sunny seasons.
