Quick Summary: While most people don’t get enough fiber, consuming too much—especially when increased too quickly—can cause uncomfortable symptoms like bloating, gas, and constipation. According to CDC research, less than 5% of US workers meet fiber recommendations, yet excessive intake beyond recommended levels can lead to digestive distress. The key is gradual adjustment and staying within guidelines of 25-38 grams daily for adults.
Here’s something that might surprise you: while health authorities constantly remind us to eat more fiber, it’s actually possible to overdo it. And when that happens, the consequences can be just as uncomfortable as not getting enough.
Most Americans struggle on the opposite end of the spectrum. According to CDC research on US workers, less than 5% meet the recommended fiber intake. But for those who suddenly embrace a high-fiber lifestyle—loading up on chia seeds, flaxseeds, and whole grains—the digestive system can rebel.
Understanding Fiber and Your Digestive System
Fiber comes in two main types, and both behave differently in the body. Soluble fiber dissolves in water and helps manage blood sugar levels while promoting feelings of fullness. Insoluble fiber doesn’t dissolve and instead helps keep things moving through the digestive tract.
Here’s the thing though—not all fiber gets processed the same way. Research published in the World Journal of Gastroenterology (2007) found that up to 80% of insoluble fiber is excreted in normal subjects. That means the more fiber consumed, the more stool must be passed.
The fermentation process matters too. Certain fibers undergo fermentation in the gut, which according to recent research helps improve insulin sensitivity and regulate blood sugar levels. But excessive fermentation can also lead to significant gas production and bloating.
How Much Fiber Should You Actually Eat?
The general recommendation sits at about 14 grams of fiber for every 1,000 calories consumed. That translates to specific targets based on age and gender.
| Age Group | Men | Women |
|---|---|---|
| 19-30 years | 34 grams | 28 grams |
| 31-50 years | 31 grams | 25 grams |
| 51+ years | 28 grams | 22 grams |
Some sources recommend targets of 25-28 grams per day for women and 28-34 grams per day for men. But these are guidelines, not rigid rules.
Real talk: individual tolerance varies significantly. What works perfectly for one person might cause digestive chaos for another.
Warning Signs You’re Eating Too Much Fiber
The symptoms of excessive fiber intake often mirror the problems fiber is supposed to solve. Sound familiar? That’s because fiber works best in moderation.
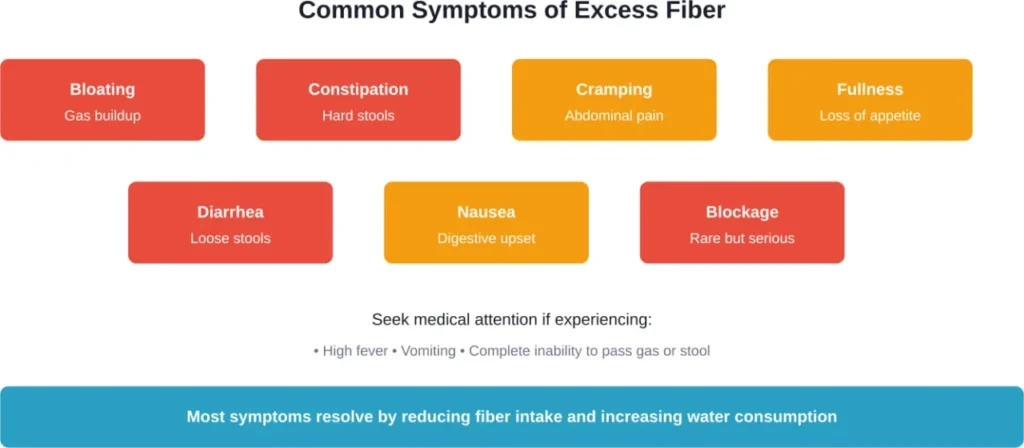
Bloating and gas rank as the most common complaints. When fiber intake jumps too quickly, gut bacteria go into overdrive fermenting the extra material. The result? Uncomfortable abdominal distension and excessive flatulence.
Constipation might seem counterintuitive since fiber typically relieves this condition. But here’s what happens: without adequate water intake, high fiber consumption can actually slow things down. The fiber absorbs available moisture, creating hard, difficult-to-pass stools.
Other symptoms include abdominal cramping, diarrhea, and a feeling of persistent fullness. In rare cases, extremely high fiber intake can cause intestinal blockage—a serious condition requiring medical attention.
The Speed Problem: Why Sudden Increases Cause Issues
Many people run into trouble not because they eat too much fiber overall, but because they ramp up too quickly. The digestive system needs time to adapt.
Think about someone who typically eats 10 grams of fiber daily, then suddenly jumps to 35 grams after reading about health benefits. That 25-gram leap overwhelms the gut bacteria and digestive processes.
Some individuals report starting with high-fiber seed combinations in oatmeal, then experiencing difficult bowel movements and sluggish digestion.
The solution? Gradual adjustment. Increase fiber intake by 5 grams per week, allowing the digestive system to adapt at each stage.
Finding Your Personal Fiber Sweet Spot
Individual tolerance varies based on several factors: current gut health, hydration levels, physical activity, and existing digestive conditions.
People with irritable bowel syndrome, Crohn’s disease, or ulcerative colitis often have lower fiber thresholds. Research on high-fiber diets shows these conditions may require modified approaches rather than standard recommendations.
Water intake matters enormously. Fiber absorbs liquid in the digestive tract, so inadequate hydration turns helpful fiber into problematic bulk. Aim for at least 8 glasses of water daily when consuming higher fiber amounts.
Types of Fiber and Their Effects
Different fiber sources produce different results. Soluble fiber from oats, apples, and beans tends to be gentler on the digestive system. Insoluble fiber from wheat bran, vegetables, and whole grains moves through more aggressively.
Balancing both types creates better outcomes than loading up on just one category.
How to Relieve Symptoms of Too Much Fiber
When symptoms strike, several strategies provide relief. First, temporarily reduce fiber intake to comfortable levels. That doesn’t mean eliminating it completely—just scaling back to what the body tolerates.
Increase water consumption significantly. Research shows that more than 70% of sodium Americans consume comes from packaged foods. Focus on plain water rather than caffeinated beverages that can dehydrate.
Physical activity helps stimulate digestion. Even a 15-minute walk can encourage movement through the intestinal tract.
Consider the timing and combination of high-fiber foods. Spreading fiber intake throughout the day rather than concentrating it in one meal reduces digestive burden.

Special Considerations and Medication Interactions
Research published in medical journals has identified cases where fiber supplements interfere with medication absorption. High fiber intake may affect medication absorption in some cases, including potential interactions with certain medications.
People taking other medications should space fiber supplements at least 2-3 hours apart from pills to avoid absorption issues.
Those with pancreatic insufficiency face additional challenges. Studies show high fiber diets can affect fat malabsorption in patients with exocrine pancreatic insufficiency secondary to chronic pancreatitis.
Getting Fiber from Whole Foods vs. Supplements
Whole food sources provide fiber alongside vitamins, minerals, and other beneficial compounds. Fruits, vegetables, whole grains, legumes, nuts, and seeds deliver nutrition beyond just fiber content.
Supplements concentrate fiber without the additional nutrients. While convenient, they’re more likely to cause digestive distress when overdone.
Mayo Clinic research emphasizes choosing foods canned in 100% fruit juice rather than syrup, and selecting low-sodium options for canned vegetables. These choices maximize nutritional benefit while controlling fiber intake.
FAQs About Eating Too Much Fiber
Fiber itself doesn’t cause weight gain. But excessive bloating and water retention from too much fiber can temporarily increase scale weight. The discomfort might also reduce physical activity, indirectly affecting weight management.
Most symptoms improve within 2-4 days after reducing fiber intake and increasing water consumption. Severe cases involving constipation may take up to a week to fully resolve.
While no official upper limit exists, consuming excessive amounts significantly increases the risk of digestive complications. Stick to recommended ranges of 25-38 grams for optimal health without side effects.
Cooking doesn’t eliminate fiber, but it can break down cell walls and make some fiber more digestible. This can actually help people who struggle with raw vegetable tolerance.
Supplements provide fiber but lack the vitamins, minerals, and phytonutrients found in whole foods. They work best as additions to—not replacements for—a varied diet rich in plant foods.
Constipation from increased fiber typically stems from inadequate water intake. Fiber absorbs liquid in the digestive tract, so without enough hydration, stools become hard and difficult to pass.
People with IBS often benefit from moderate fiber intake but may need to avoid certain high-FODMAP fibers that trigger symptoms. Working with a healthcare provider helps identify individual tolerance levels.
Finding Balance for Optimal Health
The paradox of fiber becomes clear: most people need more, but increasing too aggressively creates new problems. The World Health Organization emphasizes dietary adequacy—meeting nutritional needs without exceeding them.
Balance means listening to the body’s signals. Mild gas during adjustment is normal. Severe bloating, pain, or constipation indicates the need to pull back.
Start where current intake sits, then add 5 grams weekly until reaching recommended levels. Monitor symptoms throughout the process. If discomfort develops, maintain the current level for another week before advancing.
Remember that fiber recommendations represent population averages. Individual needs vary based on age, activity level, overall health, and digestive function. What matters most isn’t hitting an exact number, but finding the intake level that supports digestive health without causing distress.
Ready to optimize fiber intake? Track current consumption for a few days to establish a baseline, then make gradual adjustments while monitoring how the body responds. That personalized approach beats following rigid guidelines that might not fit individual circumstances.
