Quick Summary: Yes, it’s possible to get a false negative pregnancy test. Research shows up to 5% of tests may incorrectly indicate a woman isn’t pregnant when she actually is. Common causes include testing too early, using diluted urine, expired tests, or the rare ‘hook effect’ in advanced pregnancies with extremely high hCG levels.
Each year, millions of women rely on home pregnancy tests to answer one of life’s most significant questions. These tests promise convenience and accuracy—often claiming 99% reliability right on the package.
But here’s the thing: false negative results happen more often than most people realize.
Research at Washington University School of Medicine over the past decade revealed that up to 5% of pregnancy tests return results indicating a woman isn’t pregnant when she actually is. That’s not a small margin of error when the stakes are so high.
Understanding what causes false negatives, when they’re most likely to occur, and what steps to take next can make all the difference between confusion and clarity.
How Pregnancy Tests Actually Work
Home pregnancy tests detect the presence of human chorionic gonadotropin (hCG) in urine. This hormone is produced by cells that form the placenta shortly after a fertilized egg attaches to the uterine lining.
Most point-of-care urine pregnancy kits can detect pregnancy as early as the first day of a missed period. According to medical research, these tests have a maximum sensitivity of 90% at this early stage. Most kits detect the beta subunit of hCG in the range of 25 to 50 mIU/ml, though some versions range from 15 to 100 mIU/ml.
The FDA recommends using freshly voided first-morning urine specimens because the hCG concentration is highest at this time. When specimens can’t be tested immediately, they should be stored at 2-8°C for up to 48 hours.
The test works through a simple chemical reaction. When urine contacts the test strip, antibodies bind to hCG molecules if they’re present. This binding triggers a color change or displays a positive symbol on the test window.
Sounds straightforward, right? In theory, yes. In practice, several factors can interfere with this process.
What Causes False Negative Pregnancy Test Results
False negatives occur when a pregnancy test indicates someone isn’t pregnant despite being pregnant. Multiple factors contribute to these inaccurate readings.
Testing Too Early
This is the most common culprit behind false negative results.
HCG levels need time to build up after conception. In the earliest days following implantation, hCG concentrations may fall below the detection threshold of home pregnancy tests. Even tests claiming to detect pregnancy before a missed period can fail if used when hormone levels haven’t risen sufficiently.
Implantation typically occurs 6-12 days after ovulation. HCG production begins immediately after implantation, but detectable levels in urine take additional time to accumulate. Testing before sufficient hCG accumulation increases the risk of a false negative.
Diluted Urine
Drinking excessive fluids before testing can dilute urine and reduce hCG concentration below detectable levels.
First-morning urine contains the highest concentration of hCG because it’s been accumulating in the bladder overnight. Testing later in the day after consuming large amounts of water creates a less concentrated sample that may not contain enough hCG to trigger a positive result, even when pregnancy exists.
Expired or Faulty Tests
Pregnancy tests have expiration dates for a reason. The chemical reagents that detect hCG degrade over time, reducing accuracy.
Never use a test that has gone past its expiration date. Additionally, tests stored improperly—exposed to heat, moisture, or sunlight—may malfunction even before their stated expiration.
Research at Washington University tested multiple brands and found varying susceptibility to false negatives. Seven brands were somewhat susceptible, two were highly susceptible, and only two tests weren’t susceptible. The worst performer gave false negatives in 5% of urine samples from pregnant women tested.
The Hook Effect
Here’s where things get counterintuitive.
The hook effect is a rare phenomenon where extremely high hCG levels actually cause a false negative result. This typically occurs in advanced pregnancies or multiple gestations where hCG concentrations become so elevated they overwhelm the test’s antibody binding sites.
Medical research has documented cases of negative urine pregnancy tests in multiple gestation pregnancies due to this effect. When hCG levels are extraordinarily high, the antibodies become saturated and can’t form the proper sandwich complex needed to trigger a positive result.
The hook effect is uncommon in early pregnancy testing but becomes more likely after the first trimester or in pregnancies with twins or higher-order multiples.
Ectopic Pregnancy
Ectopic pregnancies produce lower-than-normal hCG levels because the pregnancy develops outside the uterus. These abnormal implantations may generate insufficient hCG to trigger a positive home pregnancy test, particularly in the early stages.
This creates a dangerous situation where someone experiencing an ectopic pregnancy receives a false negative result and delays seeking medical attention.
Certain Medical Conditions
Some health conditions can interfere with pregnancy test accuracy.
Research has found that 30% of sera from patients with IgA deficiency yielded positive pregnancy tests by one or more beta-hCG assays when none of the patients were actually pregnant. This demonstrates how immune system variations can create both false positives and potentially false negatives by interfering with test antibodies.
Certain medications containing hCG or diuretics that dilute urine can also impact results.
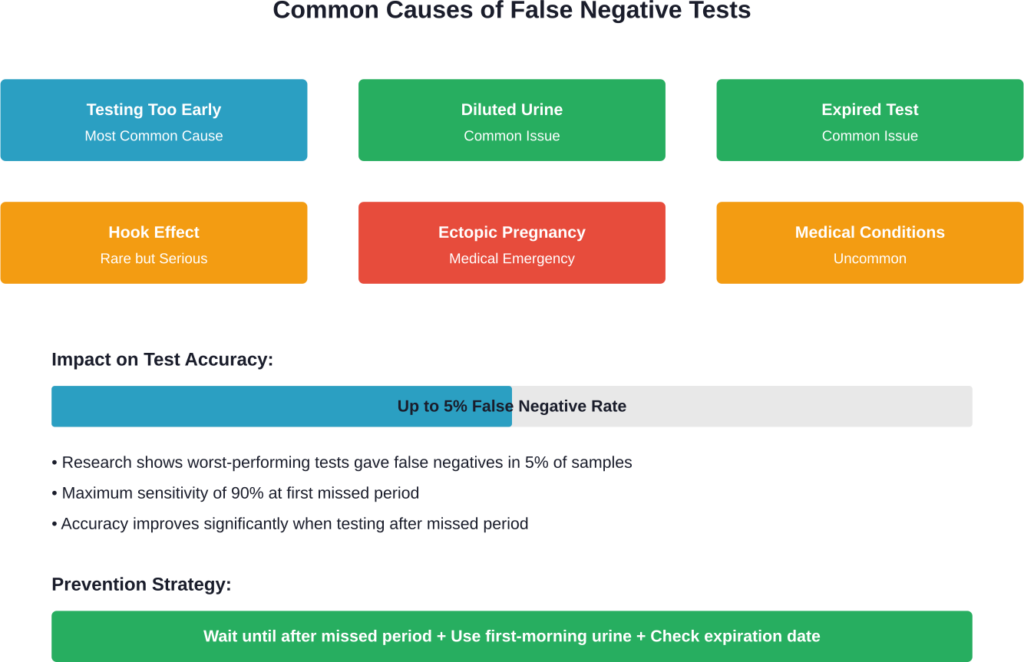
How Accurate Are Home Pregnancy Tests Really?
Marketing claims boast 99% accuracy, but the reality is more nuanced.
That 99% figure typically applies only under ideal conditions: testing after a missed period, using concentrated first-morning urine, following instructions precisely, and using an unexpired test stored properly.
When real-world variables enter the picture, accuracy drops. Testing too early is the biggest factor reducing reliability. At the time of the first missed period, urine pregnancy tests have a maximum sensitivity of 90%, according to medical research.
A retrospective study at an urban academic emergency department examined false negative point-of-care urine pregnancy tests. Researchers identified patients with a positive urine beta-hCG, serum beta-hCG greater than 5 mIU/mL, or a diagnosis of pregnancy within 3 months of the initial visit. The study revealed that false negatives occurred with measurable frequency, particularly among patients with early pregnancies or specific medical complications.
Brand matters too. The Washington University research tested multiple commercial pregnancy tests and found significant variation in susceptibility to false negatives. Not all tests perform equally.
When to Retest After a Negative Result
Getting a negative pregnancy test doesn’t always mean the story is over.
If your period hasn’t started within several days after the negative test, retest. This allows hCG levels additional time to rise to detectable concentrations if pregnancy exists.
Retest if experiencing pregnancy symptoms despite a negative result. Common early pregnancy signs include:
- Missed period
- Nausea or vomiting
- Breast tenderness or swelling
- Increased urination
- Fatigue
- Light spotting or cramping
Wait at least several days between tests. HCG levels increase significantly in early pregnancy, so waiting several days between tests allows levels to rise to detectable concentrations.
Use first-morning urine for the retest. This maximizes hCG concentration and reduces the likelihood of dilution affecting results.
Blood Tests vs. Urine Tests: Understanding the Difference
Blood tests offer advantages over home urine tests for detecting pregnancy.
Serum beta-hCG tests performed in medical settings can detect pregnancy earlier than urine tests. Blood tests can detect hCG concentrations below the threshold of home tests, which typically detect 25-50 mIU/ml.
Two types of blood pregnancy tests exist:
Qualitative hCG tests simply confirm whether hCG is present, providing a yes-or-no answer similar to home urine tests.
Quantitative hCG tests measure the exact amount of hCG in blood. This allows healthcare providers to monitor how hCG levels change over time, which helps assess pregnancy viability and detect potential problems like ectopic pregnancy or miscarriage.
Blood tests also aren’t subject to the same user error as home tests. No need to worry about diluted urine, improper timing, or reading results incorrectly.
That said, blood tests require a medical appointment and take longer to process. Results typically return within a few hours to a day, whereas home tests provide answers in minutes.
Warning Signs That Require Medical Attention
Certain symptoms warrant immediate medical evaluation regardless of pregnancy test results.
Seek medical care promptly if experiencing:
- Severe abdominal or pelvic pain
- Heavy vaginal bleeding
- Dizziness or fainting
- Shoulder pain (can indicate internal bleeding)
- Severe nausea and vomiting
These symptoms could indicate ectopic pregnancy, miscarriage, or other serious complications that require immediate treatment. Ectopic pregnancies are medical emergencies that can be life-threatening if not treated promptly.
Don’t rely solely on a negative home pregnancy test when experiencing concerning symptoms. Medical evaluation with blood testing and ultrasound provides definitive answers.
According to CDC recommendations, a detailed medical history provides the most accurate assessment of pregnancy risk in patients where pregnancy status is uncertain. Healthcare providers can use multiple indicators beyond just pregnancy test results to determine whether pregnancy exists.
Maximizing Pregnancy Test Accuracy
Following best practices increases the likelihood of getting accurate results the first time.
Optimal Timing
Wait until at least the first day of a missed period before testing. Better yet, wait 5-7 days after your expected period for maximum accuracy. This allows sufficient time for hCG to reach detectable levels.
Testing earlier than this increases the probability of a false negative, even if pregnancy exists.
Use First-Morning Urine
The first urine of the day contains the highest concentration of hCG. Avoid drinking large amounts of fluids before testing, as this dilutes urine and may reduce hCG below detectable thresholds.
Read Instructions Carefully
Different brands have varying instructions regarding how long to wait before reading results and how to interpret them. Some tests require holding the stick in the urine stream for a specific duration, while others involve dipping into a collected sample.
Follow the manufacturer’s instructions exactly. Reading results too early or too late can lead to misinterpretation.
Check the Expiration Date
Always verify the test hasn’t expired before use. Store tests in a cool, dry place away from direct sunlight and moisture. Bathroom cabinets exposed to shower steam aren’t ideal storage locations.
Consider Test Sensitivity
Some tests are more sensitive than others. Tests claiming to detect hCG at lower thresholds can theoretically identify pregnancy earlier than those with 25-50 mIU/ml thresholds. However, higher sensitivity also increases the risk of detecting pregnancies that wouldn’t have continued (chemical pregnancies).
| Testing Factor | Impact on Accuracy | Best Practice |
|---|---|---|
| Timing | Testing too early causes most false negatives | Wait until first day of missed period or later |
| Urine Concentration | Diluted urine reduces hCG detection | Use first-morning urine |
| Test Quality | Expired or improperly stored tests fail | Check expiration date and storage conditions |
| Instructions | Improper use leads to misinterpretation | Follow manufacturer directions exactly |
| Test Sensitivity | Lower threshold detects earlier pregnancy | Choose tests detecting 15-25 mIU/ml hCG |
The Hook Effect: A Rare but Real Phenomenon
The hook effect deserves special attention because it’s counterintuitive and potentially dangerous.
This rare occurrence happens when hCG levels become so extraordinarily high that they actually interfere with test accuracy. The excess hCG molecules saturate both the capture and detection antibodies, preventing the formation of the antibody-hCG sandwich complex necessary for a positive result.
Medical literature documents cases where women with advanced pregnancies or multiple gestations received negative urine pregnancy tests due to this phenomenon. One published case report described a patient with a multiple gestation pregnancy who presented to the emergency department with pregnancy symptoms but received a negative urine pregnancy test.
The hook effect typically occurs after the first trimester when hCG levels peak, or in cases of molar pregnancy where hCG production is abnormally elevated.
If the hook effect is suspected, diluting the urine sample can resolve the issue. When urine is diluted, the hCG concentration drops back into the range where antibody binding can occur properly, revealing the true positive result.
Healthcare providers in clinical settings can perform serial dilutions of urine or serum to overcome the hook effect and obtain accurate results.
Understanding Clinical Laboratory Testing
Medical facilities use pregnancy testing that differs from home tests in important ways.
Research on false-negative urine human chorionic gonadotropin testing in clinical laboratories emphasizes that under certain conditions, urine tests can fail to detect pregnancy with serious consequences for patients. This has prompted clinical centers to develop strategies minimizing risk.
Many healthcare facilities now perform both qualitative urine tests and quantitative serum tests when pregnancy status is critical to medical decision-making. This dual approach catches cases where one test might fail.
Laboratories also implement quality control measures that home users can’t replicate, including regular calibration of equipment, standardized procedures, and trained personnel performing and interpreting tests.
When pregnancy status affects treatment decisions—such as before radiation exposure, certain medications, or surgical procedures—healthcare providers rely on multiple methods to ensure accuracy. The CDC provides specific recommendations for how to be reasonably certain that a patient isn’t pregnant before administering contraceptive methods or other treatments.

What to Do If Uncertain About Results
Confusion about pregnancy test results is common and completely understandable.
If a home test shows negative but pregnancy symptoms persist, schedule an appointment with a healthcare provider. Medical professionals can perform blood tests that detect pregnancy earlier and more reliably than home urine tests.
Don’t make important medical decisions based solely on a home test result when uncertainty exists. Delaying necessary medical care because of a false negative can have serious consequences, particularly with ectopic pregnancies or other complications.
Many community health centers and medical facilities offer no-cost or low-cost pregnancy testing services. These medical-grade tests combined with professional interpretation provide greater confidence in results.
Bring information about your last menstrual period, any pregnancy symptoms experienced, and details about when and how the home test was performed. This context helps healthcare providers determine the best next steps.
Frequently Asked Questions
Yes, absolutely. False negative pregnancy tests occur when testing too early, using diluted urine, or with certain medical conditions. Research shows up to 5% of tests may incorrectly indicate someone isn’t pregnant when they actually are. Retesting after a few days or getting a blood test at a medical facility provides more definitive answers.
Wait at least several days before retesting. HCG levels increase significantly in early pregnancy, so testing again too quickly may produce the same false negative result. If your period still hasn’t arrived several days after the first negative test, that’s an ideal time to retest or consult a healthcare provider.
Early pregnancy symptoms like nausea, breast tenderness, and fatigue can appear before hCG levels rise high enough for home tests to detect. Testing too early is the most common cause of this situation. Additionally, some symptoms attributed to pregnancy overlap with premenstrual syndrome. If symptoms persist with negative tests, schedule a medical appointment for blood testing.
Yes, consuming large amounts of fluid dilutes urine and reduces hCG concentration. This can drop hCG levels below the detection threshold of home pregnancy tests even when pregnancy exists. The FDA recommends using first-morning urine specimens because hCG concentration is highest after overnight accumulation in the bladder.
The hook effect occurs when extremely high hCG levels overwhelm pregnancy test antibodies, paradoxically causing a false negative result. This rare phenomenon typically happens in advanced pregnancies past the first trimester or with multiple gestations. While uncommon in early pregnancy testing, medical literature documents cases where women with twins or triplets received false negatives due to extraordinarily elevated hCG levels.
Yes, blood tests detect pregnancy earlier and more accurately than urine tests. Serum beta-hCG tests can identify hCG concentrations below the threshold of home tests, compared to 25-50 mIU/ml for most home tests. Blood tests also provide quantitative measurements that track how hCG levels change over time, helping healthcare providers assess pregnancy viability and detect potential complications.
Absolutely. The chemical reagents in pregnancy tests that detect hCG degrade over time, reducing accuracy. Never use tests past their expiration date. Additionally, tests stored improperly in hot, humid environments may malfunction even before their stated expiration. Always check the expiration date and store tests in cool, dry locations.
Moving Forward With Confidence
Understanding that false negative pregnancy tests occur more frequently than marketing claims suggest empowers better decision-making.
The key takeaways: timing matters enormously, first-morning urine provides the most accurate results, and no single home test offers perfect reliability. Research demonstrates that even under ideal conditions, tests have a maximum sensitivity of 90% at the time of a missed period.
When in doubt, wait a few days and retest. If symptoms persist despite negative results, seek medical evaluation. Blood tests and professional assessment eliminate the guesswork that home testing sometimes creates.
False negatives happen for identifiable, understandable reasons. Testing too early remains the primary culprit, but diluted urine, expired tests, and rare phenomena like the hook effect all contribute to inaccurate results.
The good news? Awareness of these factors allows for strategies that maximize accuracy. Test at the right time, use concentrated first-morning urine, verify the test hasn’t expired, and follow instructions precisely.
And remember: medical professionals exist precisely to help navigate situations where home testing creates uncertainty. Don’t hesitate to reach out for definitive answers when home results don’t align with symptoms or expectations.
Getting accurate pregnancy information shouldn’t feel like solving a mystery. Armed with knowledge about why false negatives occur and how to prevent them, the path forward becomes clearer—whether the goal is confirming pregnancy or ruling it out with confidence.
