Quick Summary: Red eyes are very possible and extremely common, affecting millions of people daily. Eye redness occurs when blood vessels on the eye’s surface dilate or become inflamed. While most cases result from minor issues like allergies or dry eyes, some red eye conditions require immediate medical attention.
The short answer? Absolutely. Red eyes aren’t just possible—they’re one of the most common eye complaints encountered in medical settings.
According to medical research, eye problems account for 2 to 3% of visits to primary care physicians and emergency facilities, which corresponds to an average of 4 to 10 patients every week presenting with red eye symptoms.
But here’s the thing: not all red eyes signal the same problem. Some cases clear up on their own within hours. Others might indicate vision-threatening conditions that need immediate care.
What Causes the Eye to Turn Red?
Eye redness happens when tiny blood vessels on the surface of the eye expand and become more visible. This makes the white part of your eye (the sclera) appear pink or red.
The conjunctiva—a thin, transparent membrane covering the white of the eye—contains these blood vessels. When irritation or inflammation occurs, blood flow increases to the area, causing that characteristic redness.
Think of it like a traffic jam on the eye’s surface. More blood vessels become visible, and suddenly the whites of your eyes don’t look so white anymore.
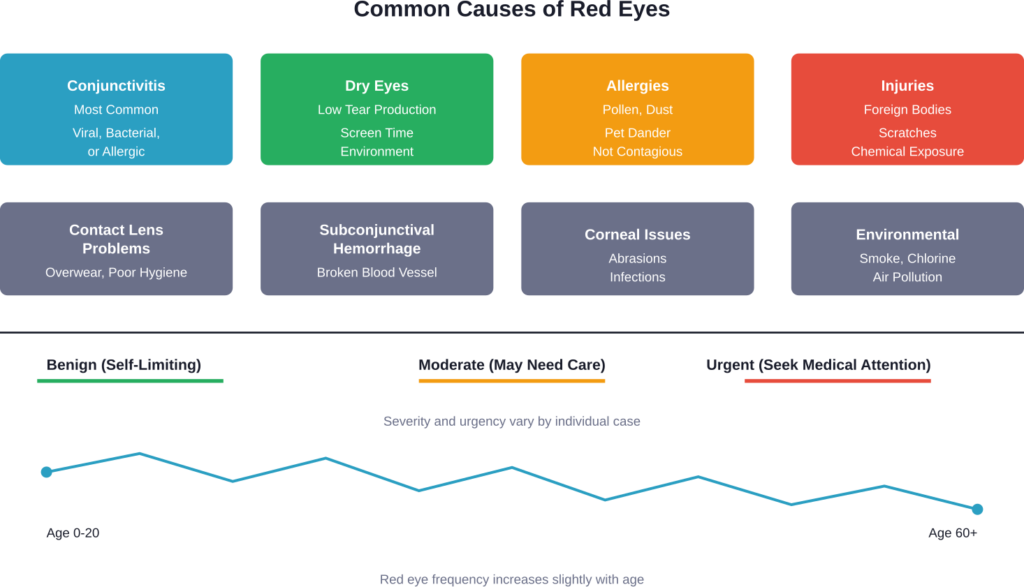
Common Causes of Red Eyes
According to the CDC, pink eye (conjunctivitis) ranks as the most common cause of eye redness. But it’s far from the only culprit.
Conjunctivitis (Pink Eye)
Pink eye causes swelling and redness inside the eyelid and the white part of the eye, according to the National Eye Institute. The condition can make eyes feel itchy and painful.
The CDC identifies three main types:
- Viral conjunctivitis: Highly contagious and often accompanies colds
- Bacterial conjunctivitis: Also very contagious, may produce thick discharge
- Allergic conjunctivitis: Not contagious, triggered by allergens
Both viral and bacterial forms spread easily through contact. Allergic conjunctivitis, however, poses no contagion risk.
Dry Eyes
Insufficient tear production or poor tear quality can cause chronic redness. Environmental factors like wind, smoke, or prolonged screen time make this worse.
Dry eyes often feel gritty or burning. The irony? Sometimes they produce excessive watering as the eye tries to compensate.
Allergies
Seasonal allergens, pet dander, or dust mites trigger histamine release. This causes blood vessels to dilate, producing red, itchy, watery eyes.
Allergic reactions typically affect both eyes simultaneously and often come with sneezing or nasal congestion.
Subconjunctival Hemorrhage
This sounds scary but it’s usually harmless. A small blood vessel breaks beneath the conjunctiva, creating a bright red patch on the white of the eye.
It can happen from coughing, sneezing, or even rubbing your eyes too hard. The blood typically absorbs within one to two weeks without treatment.
Eye Injuries and Foreign Bodies
Scratches, cuts, or objects lodged in the eye cause immediate redness. Even a loose eyelash can irritate the eye’s surface enough to trigger inflammation.
The National Eye Institute notes that small abrasions on the cornea can lead to redness and discomfort.
Contact Lens Problems
Overwearing contacts, sleeping in lenses not designed for overnight use, or poor lens hygiene can all cause red eyes. Protein deposits on lenses create friction and irritation.
Chemical Exposure and Irritants
The CDC lists chemicals, chlorine from swimming pools, smoke, and air pollution as common irritants that cause eye redness.
Even makeup, lotions, or shampoo can trigger reactions if they get into the eyes.
When Red Eyes Signal Something Serious
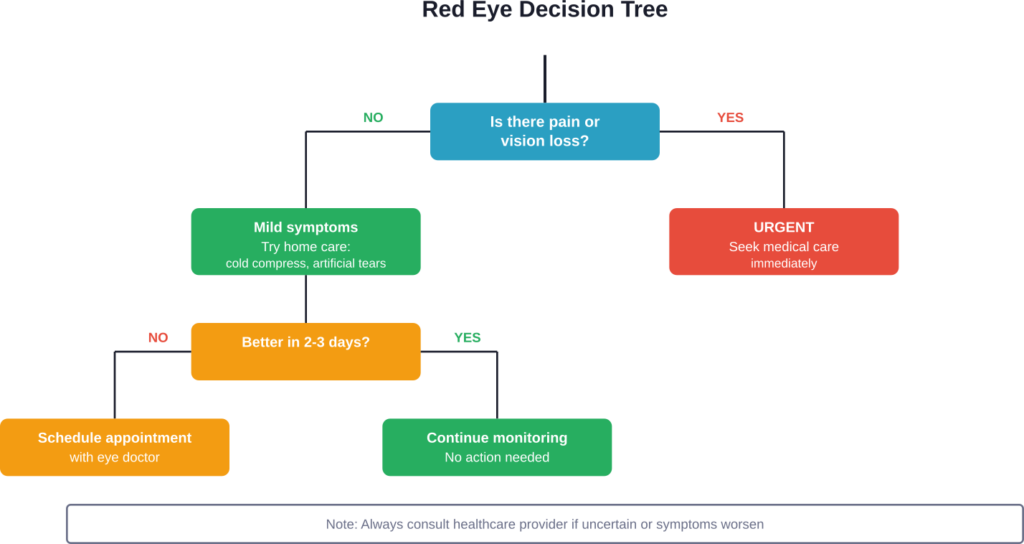
Most cases of red eyes aren’t emergencies. But certain symptoms demand immediate medical attention.
Medical research indicates that if vision changes or eye pain accompany redness, more serious conditions may be present.
Warning Signs That Need Immediate Care
Seek urgent medical attention if red eyes occur with:
- Sudden vision loss or blurry vision
- Severe eye pain
- Sensitivity to light (photophobia)
- Halos around lights
- Headache or nausea
- Eye injury or chemical exposure
- Discharge that’s thick, green, or yellow
- Redness that doesn’t improve after 2-3 days
According to the National Eye Institute, corneal conditions can present with eye pain, blurry vision, red or watery eyes, sensitivity to light, and eye pain.
Vision-Threatening Conditions
Certain serious conditions present with eye redness:
Acute angle-closure glaucoma: A medical emergency where pressure inside the eye rises rapidly. Symptoms include severe pain, nausea, and seeing halos around lights.
Uveitis: Inflammation of the middle layer of the eye. Can cause permanent vision damage if untreated.
Keratitis: Corneal infection that can result from bacteria, viruses, or fungi. Often seen in contact lens wearers.
Scleritis: Deep inflammation of the white part of the eye. Associated with autoimmune diseases and causes severe pain.
An estimated 400,000 Americans have had some form of ocular herpes. Previous studies show that once people develop ocular herpes, they have up to a 50 percent chance of having a recurrence.
Treatment Options for Red Eyes
Treatment depends entirely on the underlying cause. There’s no one-size-fits-all solution.
Home Remedies and Self-Care
The CDC and National Eye Institute recommend these approaches for mild cases:
Cold compresses: Apply a cold washcloth or gentle ice pack to eyes for relief, using for no longer than 10 minutes at a time to reduce swelling.
Artificial tears: Over-the-counter eye drops can relieve dryness. The National Eye Institute specifically recommends this type of eye drop for symptom relief.
Avoid irritants: Remove contact lenses, stay away from smoke, and reduce screen time.
Don’t rub: Rubbing inflamed eyes makes redness worse and can spread infection.
According to the National Eye Institute, most cases of pink eye will go away on their own without medical intervention.
Medical Treatments
When home care isn’t enough, medical interventions include:
Antibiotic eye drops or ointment: For bacterial conjunctivitis or infections.
Antiviral medications: The National Eye Institute reports that acyclovir, taken by mouth, reduced by 41 percent the probability that any form of herpes of the eye would return in patients who had the infection in the previous year.
Antihistamine drops: For allergic conjunctivitis.
Steroid eye drops: For severe inflammation (used cautiously due to potential side effects).
Specialized treatments: Procedures like laser surgery, corneal transplant, or artificial cornea may be necessary for certain corneal conditions, according to the National Eye Institute.
| Condition | Primary Treatment | Recovery Time |
|---|---|---|
| Viral Conjunctivitis | Supportive care, cold compresses | 1-2 weeks (can take up to 3 weeks or more) |
| Bacterial Conjunctivitis | Antibiotic drops | Usually clears in 2 to 5 days with treatment |
| Allergic Conjunctivitis | Antihistamine drops, avoid allergens | Varies, often chronic |
| Dry Eyes | Artificial tears, lifestyle changes | Ongoing management |
| Subconjunctival Hemorrhage | None needed | 1-2 weeks |
Preventing Red Eyes
Many cases of eye redness are preventable with simple precautions.
Hand hygiene: The CDC emphasizes that washing hands frequently prevents spreading viral and bacterial conjunctivitis.
Proper contact lens care: Follow wearing schedules, clean lenses properly, and replace them as directed.
Protect your eyes: Wear safety glasses during activities that could cause injury. Use swim goggles in chlorinated pools.
Manage allergies: Keep windows closed during high pollen days. Use air purifiers and wash bedding regularly.
Screen breaks: Follow the 20-20-20 rule: every 20 minutes, look at something 20 feet away for 20 seconds.
Don’t share: Never share eye makeup, towels, or contact lenses.
Red Eyes in Special Populations
Newborns and Infants
Pink eye in newborns requires special attention. According to the National Eye Institute, newborns who develop pink eye typically show symptoms 1 day to 2 weeks after birth.
Pink eye can cause serious health problems for newborn babies. Call a doctor now if your baby has unusual fluid (discharge) coming from the eye or puffy red eyelids.
Contact Lens Wearers
Contact lens users face higher risks for certain types of red eye, particularly keratitis. Sleeping in contacts not designed for overnight wear dramatically increases infection risk.
Proper hygiene—washing hands before handling lenses, using fresh solution daily, and replacing lenses on schedule—prevents most complications.
Frequently Asked Questions
Indirectly, yes. Stress often leads to behaviors that cause red eyes—like rubbing them, reduced sleep, or eye strain from prolonged screen time. Stress can also trigger or worsen dry eye symptoms.
Duration varies by cause. Subconjunctival hemorrhages resolve in 1-2 weeks. Viral conjunctivitis clears within 1-2 weeks. Bacterial conjunctivitis improves within 2-5 days with antibiotic treatment. Chronic conditions like dry eyes may require ongoing management.
These drops, usually containing decongestants, temporarily constrict blood vessels to reduce redness. But ophthalmologists generally recommend using them sparingly. Overuse can cause rebound redness—making eyes even redder when the drops wear off.
Subconjunctival hemorrhages (broken blood vessels in the eye) can occasionally occur with sudden blood pressure spikes, though they’re usually not directly caused by chronic hypertension. If concerned about cardiovascular health, consult a physician for proper blood pressure monitoring.
It depends on the cause. With infectious conjunctivitis, avoid eye makeup entirely—it can harbor bacteria and prolong infection. With non-infectious causes like allergies or dry eyes, makeup is generally safe, though it may cause additional irritation. Never share eye makeup, as this spreads infection.
Not at all. While infections like bacterial or viral conjunctivitis cause redness, many non-infectious factors do too: allergies, dry eyes, irritants, broken blood vessels, or simply fatigue. The presence of other symptoms helps determine the cause.
The CDC advises that children with viral or bacterial conjunctivitis should stay home until symptoms improve or a doctor clears them. These types are highly contagious. Red eyes from allergies or non-contagious causes don’t require staying home, though checking with the school nurse is advisable.
The Bottom Line on Red Eyes
Red eyes are absolutely possible—and incredibly common. Most cases stem from minor issues that resolve with simple home care.
But distinguishing between harmless redness and serious conditions matters. Pain, vision changes, light sensitivity, or persistent symptoms warrant professional evaluation.
The good news? According to medical research, conjunctivitis and most common causes of red eye are not associated with disturbance of vision or significant pain. When these warning signs appear, that’s when urgent care becomes necessary.
Listen to your symptoms. Most red eyes clear up within days. When they don’t—or when something feels seriously wrong—trust that instinct and seek medical attention.
Your vision is too valuable to risk on uncertainty. If in doubt, get it checked out.
