Quick Summary: Yes, it is possible to have two uteruses—a rare congenital condition called uterus didelphys that occurs in approximately 0.3% of women. This condition develops when the Müllerian ducts fail to fuse completely during fetal development, resulting in two separate uterine cavities, and often two cervixes and vaginal canals.
The human body sometimes develops in unexpected ways. And one of the most fascinating reproductive anomalies is having two complete uteruses—a condition that sounds like science fiction but is very real.
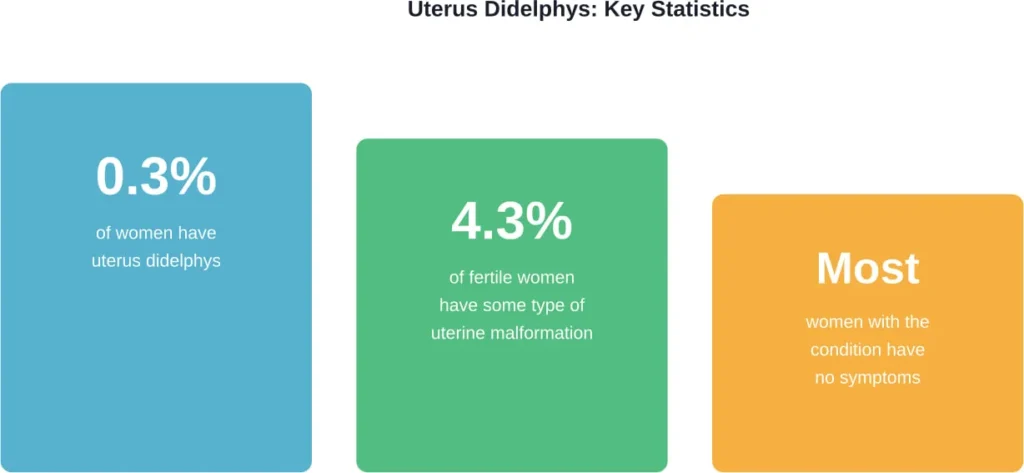
This rare congenital abnormality affects roughly 0.3 percent of women worldwide. Most people with this condition don’t even know they have it until they undergo imaging for unrelated reasons or experience pregnancy complications.
So what exactly causes someone to develop two uteruses instead of one? And what does this mean for menstruation, fertility, and pregnancy? Here’s everything you need to know.
What Is Uterus Didelphys?
Uterus didelphys—also called double uterus—is a congenital condition where a person is born with two separate uterine cavities instead of one. Instead of the typical pear-shaped uterus, each uterus resembles a banana shape.
This condition belongs to a category of birth defects called Müllerian duct anomalies (MDAs). According to research published in the International Journal of Environmental Research and Public Health (2022), reproductive organ malformations occur in approximately 4.3% of fertile women and approximately 3.5% in infertile women.
But uterus didelphys is among the rarest of these anomalies. While septate uterus is the most common uterine malformation, uterus didelphys occurs in just 0.3% of the general population.
What Makes It Different From Other Uterine Anomalies
Not all double uteruses are created equal. Several types of Müllerian duct anomalies can affect the uterine structure:
- Uterus didelphys: Two completely separate uterine cavities, often with two cervixes and sometimes two vaginal canals
- Bicornuate uterus: The uterus has two horns at the top but joins into a single cavity and cervix at the bottom
- Septate uterus: A single uterus divided by a wall (septum) of tissue
- Unicornuate uterus: A single, smaller uterus with only one functioning side
The key distinction? With uterus didelphys, you’ve got two completely independent uterine systems. Each uterus typically has its own fallopian tube and ovary connection.
How Does Someone Develop Two Uteruses?
The development happens long before birth—during fetal life between 6 and 22 weeks of gestation. Here’s how it works.
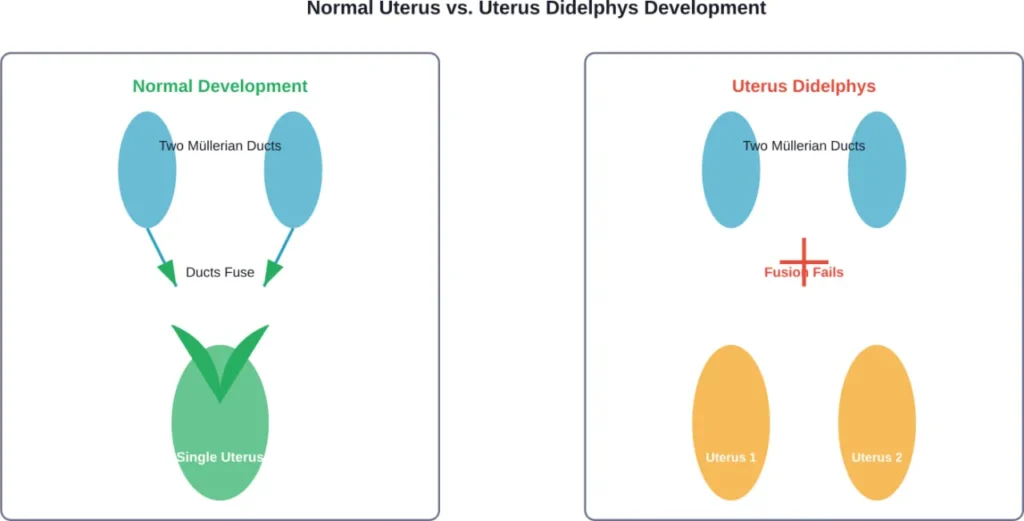
In a female fetus, the reproductive system starts as two small tubes called Müllerian ducts (also known as paramesonephric ducts). As the fetus develops, these tubes normally migrate toward each other and fuse together, creating one hollow organ: the uterus.
When this fusion process fails completely, both ducts develop independently. The result? Two separate uteruses, each with its own cavity.
According to research from Case Reports in Obstetrics and Gynecology, these abnormalities can include failure of development, fusion, canalization, or resorption during the critical developmental window. Most sources estimate the incidence of these abnormalities to range from 0.5 to 5.0% in the general population.
Why Does This Happen?
The exact cause remains unclear. There’s no known genetic pattern, and it doesn’t run in families in a predictable way. It simply happens during fetal development—likely due to a combination of genetic and environmental factors that researchers don’t fully understand yet.
What’s certain is that nobody did anything wrong. This isn’t caused by anything the mother did or didn’t do during pregnancy.
Symptoms and How It’s Diagnosed
Here’s the thing: many women with uterus didelphys have zero symptoms. They might go their entire lives without knowing they have two uteruses.
But some people do experience signs, particularly during adolescence or pregnancy.
Common Symptoms Include
- Painful menstrual periods (dysmenorrhea)
- Abnormal vaginal bleeding or spotting
- Painful intercourse (dyspareunia)
- Recurrent pregnancy loss
- Preterm labor and delivery
- Unusual pelvic pain
If there’s a longitudinal vaginal septum (a wall dividing the vagina into two canals), some people experience discomfort with tampon use or during pelvic exams.
How Doctors Diagnose Double Uterus
Most cases are discovered incidentally during imaging for other reasons—or when complications arise during pregnancy.
Diagnostic methods include:
- Pelvic ultrasound: Often the first imaging test performed
- MRI (Magnetic Resonance Imaging): Provides the most detailed view of uterine structure
- Hysterosalpingography: An X-ray procedure using contrast dye to visualize the uterine cavities
- Sonohysterography: Ultrasound with saline infusion for better cavity visualization
According to research on double cervix diagnosis, careful evaluation of the uterine fundus is required for correct diagnosis, as septate uterus can present similarly to uterus didelphys in women with a double cervix.
Can You Get Pregnant With Two Uteruses?
Absolutely. Most women with uterus didelphys can get pregnant and carry healthy babies to term.
But there’s a catch—pregnancy with this condition does carry higher risks. Research published in the International Journal of Environmental Research and Public Health indicates that uterus didelphys can impact fertility and pregnancy outcomes.
Pregnancy Risks Associated With Double Uterus
| Complication | Risk Level | Description |
|---|---|---|
| Preterm delivery | Increased | Babies may arrive earlier than 37 weeks |
| Breech presentation | Higher than normal | Baby positioned feet-first instead of head-down |
| Cesarean delivery | More common | Often required due to breech position or other factors |
| Fetal growth restriction | Moderate risk | Limited space in each uterine cavity may restrict growth |
| Miscarriage | Slightly increased | Higher rate in first trimester compared to general population |
That said, many women with uterus didelphys have completely normal pregnancies. According to a case report published in Cureus in 2024, full-term pregnancies are achievable with proper monitoring and care.
The Extraordinary Case of Twin Pregnancies
Now this is where it gets really interesting.
In extremely rare cases, a woman with uterus didelphys can become pregnant in both uteruses simultaneously—what’s called a dicavitary twin pregnancy.
The University of Alabama at Birmingham documented one such case in December 2023. Kelsey Hatcher, who has uterus didelphys, became pregnant with a baby in each uterus. She delivered two healthy baby girls—born 10 hours apart on separate days, each with their own birthday.
According to UAB’s report, uterus didelphys occurs in 0.3 percent of women, and dicavitary twin pregnancy (a baby in each uterus) is extraordinarily rare.
According to BMC Pregnancy and Childbirth research published in 2025, there’s even been a documented case of asynchronous twin delivery with a 12-week interval between births.
Treatment Options and Management
Most people with uterus didelphys don’t need treatment. The condition itself isn’t dangerous—it’s just an anatomical variation.
Treatment becomes relevant only when complications arise.
When Surgery Might Be Considered
Surgery isn’t typically recommended for uterus didelphys itself. However, surgical intervention might be appropriate for:
- Removing a vaginal septum that causes pain or difficulty with intercourse
- Addressing recurrent pregnancy loss due to cervical insufficiency
- Managing obstructive symptoms if one uterine horn isn’t functioning properly
According to American College of Obstetricians and Gynecologists (ACOG) guidance on obstructive uterovaginal anomalies, these conditions are not surgical emergencies, and the complexities are best managed by subspecialists with expertise in reproductive tract anomalies.
Managing Pregnancy With Double Uterus
If you’re pregnant with uterus didelphys, expect closer monitoring. Your healthcare provider will likely recommend:
- More frequent ultrasounds to monitor fetal growth
- Cervical length assessments to screen for preterm labor risk
- Discussion about delivery planning (vaginal vs. cesarean)
- Monitoring for signs of preterm contractions
The good news? With proper prenatal care, outcomes are generally positive.
Living With Two Uteruses
So what’s daily life like with this condition?
For most people—completely normal. The condition doesn’t affect hormone levels, menstrual cycles, or sexual function in most cases.
What About Periods?
Here’s a common question: do you get two periods?
Not exactly. While you have two uteruses, your menstrual cycle is still controlled by the same hormones. Both uteruses typically respond to these hormonal signals simultaneously, so menstruation happens at the same time from both cavities.
That said, some people report heavier or more painful periods due to menstrual flow from both uterine cavities.
Fertility Considerations
Most women with uterus didelphys have normal fertility. Ovulation occurs normally, and either uterus can support a pregnancy.
According to research published in the International Journal of Environmental Research and Public Health (2022), reproductive organ malformations occur in approximately 4.3% of fertile women and approximately 3.5% in infertile women—suggesting the condition itself doesn’t necessarily cause infertility.
That said, if you’re experiencing recurrent pregnancy loss or difficulty conceiving, consultation with a reproductive endocrinologist or maternal-fetal medicine specialist is worthwhile.
Related Conditions and Variations
Uterus didelphys isn’t the only Müllerian duct anomaly worth knowing about.
Bicornuate Uterus
A bicornuate uterus forms when the two Müllerian ducts partially fuse. The result? Two horns at the upper part of the uterus, while the lower part fuses into a single uterine cavity and cervix.
According to research, bicornuate uteri can increase pregnancy risks—particularly risks of premature delivery, cesarean delivery, and fetal growth restriction.
Septate Uterus
A septate uterus appears normal from the outside but has an internal wall (septum) dividing the cavity. According to research, septate uterus can present similarly to uterus didelphys in women with a double cervix, requiring careful diagnostic evaluation.
Comparison of Uterine Anomalies
| Condition | External Shape | Internal Structure | Cervix Count |
|---|---|---|---|
| Normal uterus | Single pear shape | Single cavity | One |
| Uterus didelphys | Two separate organs | Two complete cavities | Two (usually) |
| Bicornuate uterus | Heart-shaped with indent | Two horns joining lower | One |
| Septate uterus | Normal appearing | Internal wall dividing cavity | One |
| Unicornuate uterus | Smaller, banana-shaped | Single smaller cavity | One |
When to See a Doctor
Most people with uterus didelphys discover their condition by accident. But you should definitely consult a healthcare provider if you experience:
- Unusually painful periods that don’t respond to standard pain management
- Persistent pelvic pain
- Pain during intercourse
- Difficulty inserting tampons
- Recurrent pregnancy loss
- Abnormal vaginal bleeding patterns
And if you know you have uterus didelphys and you’re planning pregnancy, talk with your healthcare provider before conceiving. They can help you understand your specific risks and create a monitoring plan.
Frequently Asked Questions
Yes, both uteruses typically menstruate simultaneously because they respond to the same hormonal signals from your ovaries. Some women report heavier or longer periods due to menstrual flow from both uterine cavities, though many experience completely normal menstrual cycles.
Uterus didelphys is not typically hereditary and doesn’t follow a predictable genetic pattern. The condition develops during fetal life between 6 and 22 weeks of gestation when the Müllerian ducts fail to fuse properly. The exact cause remains unclear and likely involves multiple factors.
Yes, though it’s extremely rare. This is called dicavitary twin pregnancy, where a baby develops in each uterus simultaneously. The University of Alabama at Birmingham documented such a case in 2023, where a woman delivered healthy babies from each uterus 10 hours apart on separate days.
Not necessarily. While cesarean delivery is more common with uterus didelphys—often due to breech presentation or other complications—vaginal delivery is possible in many cases. Your delivery method depends on various factors including baby’s position, your obstetric history, and your healthcare provider’s assessment.
Most women with uterus didelphys have normal fertility and can conceive naturally. Research shows reproductive organ malformations occur in approximately 4.3% of fertile women versus 3.5% in infertile women, suggesting the condition doesn’t necessarily cause infertility. However, pregnancy may carry higher risks of preterm delivery and other complications.
Most people don’t need surgery for uterus didelphys itself. Surgery might be considered only if you have a vaginal septum causing pain or sexual difficulties, or if you experience recurrent pregnancy complications. According to ACOG guidance, these are not surgical emergencies and should be managed by specialists.
Yes, but it requires proper imaging. MRI provides the most detailed visualization, while ultrasound and hysterosalpingography can also identify the condition. The key diagnostic feature is complete duplication of the uterine cavities with two separate cervixes, distinguishing it from septate or bicornuate uterus.
The Bottom Line on Having Two Uteruses
So yes—it is absolutely possible to have two uteruses. Uterus didelphys is a rare congenital condition affecting approximately 0.3% of women, where complete duplication of the uterine cavities occurs due to failed fusion of the Müllerian ducts during fetal development.
Most people with this condition live completely normal lives without ever knowing they have it. When symptoms do occur, they’re manageable with proper medical care.
And while pregnancy with uterus didelphys does carry some increased risks, the vast majority of women with this condition can conceive naturally and deliver healthy babies with appropriate monitoring.
If you suspect you might have this condition—or you’ve been diagnosed and have concerns—don’t hesitate to consult with a gynecologist or reproductive specialist. They can provide personalized guidance based on your specific anatomy and reproductive goals.
Living with two uteruses doesn’t mean living with limitations. With knowledge and proper healthcare support, you can navigate this anatomical variation successfully.
