Quick Summary: Keeping weight off after stopping Ozempic is possible but challenging, as studies show most people regain some weight when they discontinue GLP-1 medications. Research from Vanderbilt University found that patients who transitioned to older, generic weight-loss medications after stopping GLP-1 drugs maintained significant weight loss, while other studies show reduced-frequency dosing can preserve results. Success requires a comprehensive approach including regular physical activity (200-250 minutes weekly), strength training, dietary changes, and sometimes transitioning to alternative medications rather than stopping treatment entirely.
The explosion of GLP-1 receptor agonist medications like Ozempic has transformed obesity treatment. Millions of people have achieved significant weight loss with these drugs. But here’s the reality check most patients face: a new study surveying more than 120,000 people found that the majority stop taking these medications after just two years.
So what happens when treatment stops? And more importantly, is it actually possible to maintain that hard-won weight loss?
The short answer is yes, but it requires intentional effort. Recent research shows several pathways to maintaining weight after discontinuing GLP-1 medications, though weight regain remains common. Understanding what works—and what doesn’t—can make the difference between long-term success and frustration.
Why People Stop Taking Ozempic
Before diving into maintenance strategies, it’s worth understanding why so many people discontinue these medications in the first place.
Cost stands as the primary barrier. The high expense of novel GLP-1 receptor agonist class agents often limits access and creates barriers to care, according to research published in Obesity. Even with insurance, copays can reach hundreds of dollars monthly.
Side effects drive others away. Nausea, vomiting, and gastrointestinal discomfort affect many users. Some experience these effects throughout treatment, not just in the initial weeks.
Then there’s the psychological factor. Many patients reach their goal weight and wonder whether they really need to continue medication indefinitely. The idea of lifelong pharmaceutical dependence doesn’t sit well with everyone.
Supply shortages have also forced discontinuation for some patients, particularly during 2023 and 2024 when demand outstripped manufacturing capacity.
What Happens When You Stop Taking Ozempic
Understanding the physiological changes that occur after stopping helps explain why weight maintenance proves challenging.
Appetite Returns With a Vengeance
GLP-1 medications work partly by suppressing appetite and slowing gastric emptying. These effects typically wear off within days to weeks after the final dose.
Patients report feeling hungrier than before they started treatment. The medication essentially turns down the volume on hunger signals—when it’s gone, those signals come roaring back. Many describe this as one of the most difficult adjustments.
Metabolic Adaptations Work Against You
Weight loss from any method—not just medications—triggers metabolic adaptations. The body becomes more efficient at storing energy and less enthusiastic about burning it.
This metabolic slowdown means maintenance requires fewer calories than someone of the same weight who never lost weight in the first place. It’s an unfair biological reality, but one that must be addressed.
Blood Sugar Control Changes
For patients with type 2 diabetes, stopping Ozempic or similar medications means losing the glucose-lowering effects. Blood sugar levels often climb after discontinuation.
According to research cited in NCBI resources, metformin remains the preferred first-line therapy for treating type 2 diabetes according to the American Diabetes Association. Patients stopping GLP-1 medications may need to transition to or intensify other diabetes treatments.
Weight Regain Is Common But Not Universal
Studies suggest patients taking these medications can lose 15% to 20% of their body weight on average while actively using them. But what happens after stopping?
Real talk: weight regain after stopping is the norm, not the exception. Some evidence suggests that certain cardiometabolic benefits may persist but only modestly after discontinuation.
However—and this is crucial—weight regain is not inevitable. The degree of regain varies tremendously based on what patients do after stopping.
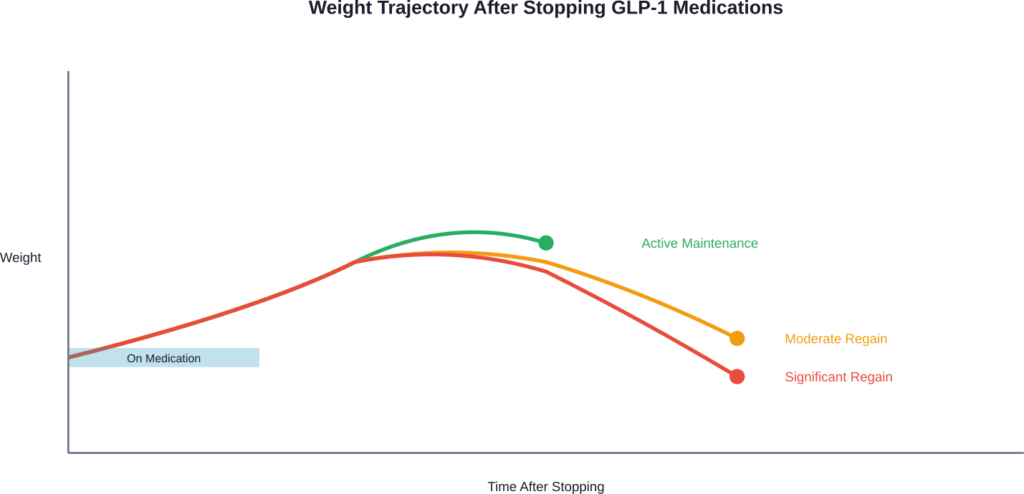
Research-Backed Strategies That Actually Work
Now for the practical part. What does the evidence say about maintaining weight loss after stopping Ozempic and similar drugs?
Transition to Alternative Medications
Here’s where it gets interesting. Research from Vanderbilt University Medical Center published in 2024 offers a promising path forward.
A research study examined patients who transitioned from expensive GLP-1 medications to generic, older-generation antiobesity medications after their initial weight loss. At 12 months, patients in the study showed an average of 18.3% body weight loss from baseline, with a mean BMI of 27.9 kg/m².
At 18 months, weight maintenance was noted with a mean BMI of 27.9 kg/m². Research suggests patients treated with GLP-1 receptor agonists may maintain weight loss using generic older-generation antiobesity medications, suggesting potential cost savings and new policy implications.
This approach essentially bridges from one medication class to another rather than stopping pharmaceutical support entirely.
Reduced-Frequency Dosing
Another study examined whether patients could step down to less frequent dosing rather than stopping completely.
The research found that in patients with prior weight loss and metabolic improvement on GLP-1 therapy, reduced-frequency maintenance dosing preserved outcomes. These findings support structured de-escalation as a promising strategy to reduce treatment burden without sacrificing efficacy.
Think of it as a middle ground—not full discontinuation, but less frequent injections at potentially lower cost and with fewer side effects.
Intensive Physical Activity Programs
Movement matters more than most people realize when it comes to weight maintenance.
The recommendation is specific: engage in at least 200 to 250 minutes of moderate-intensity physical activity each week. That exercise should include regular strength training exercises to maintain muscle mass.
Why so much? Because loss of muscle during weight loss is a major reason weight comes back as fat. Strength training helps preserve lean tissue, which keeps metabolic rate higher.
One structured program showed results within 10 weeks: 69 percent of inactive members became active or healthy active, members completed an average of 4.5 guided sessions per week, and sedentary time dropped by more than [amount not specified in source]. Additionally, 91 percent of members reported feeling moderately or much better.
| Maintenance Strategy | Evidence Level | Weight Maintenance Rate | Key Considerations |
|---|---|---|---|
| Transition to generic medications | Clinical study | 18.3% loss maintained at 12 months | Requires prescription, ongoing cost |
| Reduced-frequency GLP-1 dosing | Clinical research | Outcomes preserved | Lower cost than full dose, continued medication |
| Intensive exercise (200-250 min/week) | Established guidelines | Varies widely | Requires significant time commitment |
| Dietary modifications alone | Historical data | Modest success | Difficult without other support |
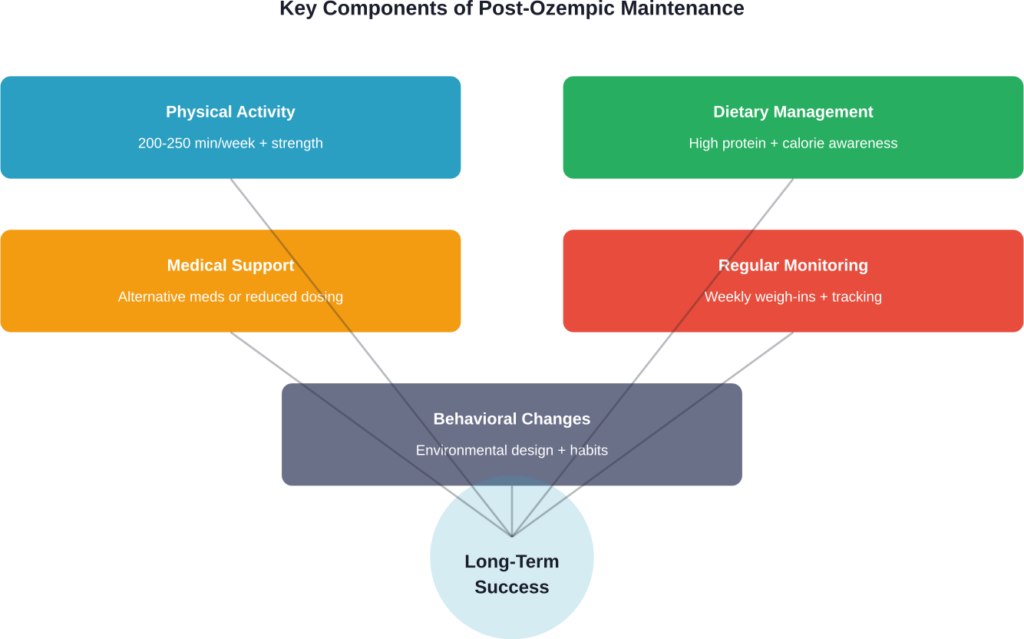
Building a Sustainable Maintenance Plan
Success rarely comes from a single intervention. The most effective approach combines multiple strategies tailored to individual circumstances.
Start Planning Before You Stop
The worst time to figure out maintenance is the day after the final dose. Begin planning weeks or months in advance.
This includes establishing exercise habits while still on medication, when appetite suppression makes dietary compliance easier. It also means building a support system and potentially consulting with specialists about transition medications.
Prioritize Protein and Resistance Training
Muscle loss during weight loss is inevitable to some degree. But minimizing it is crucial for long-term maintenance.
Higher protein intake combined with resistance training provides the best defense against muscle loss. This preserves metabolic rate and makes weight maintenance more forgiving.
Stock the fridge with easily accessible high-protein snacks. Make strength training non-negotiable, not optional.
Create Environmental Supports
Willpower is overrated. Environmental design is underrated.
Simple changes make a difference: keeping tempting foods out of the house, preparing healthy snacks in advance like carrot sticks and fresh fruit, and structuring daily routines to include movement.
When healthy choices become the default rather than requiring constant decision-making, maintenance becomes significantly easier.
Monitor Weight Regularly
Weekly weigh-ins provide early warning signals. A 3-5 pound gain is much easier to address than a 20-pound regain.
This isn’t about obsession—it’s about data. Catching small increases early allows for minor adjustments before problems compound.
When Stopping Might Not Be the Right Choice
Here’s an uncomfortable truth: for some people, continuing medication long-term may be the most practical solution.
Obesity is a chronic condition. The Endocrine Society and other medical organizations increasingly recognize it as a disease requiring ongoing management, not a temporary problem solved with short-term intervention.
GLP-1 medications offer benefits beyond weight loss. Research shows these drugs may lower the risk of acute pancreatitis recurrence. When the GLP-1 group was compared with patients taking SGLT2 inhibitors, the GLP-1 group showed a lower risk of acute pancreatitis recurrence (15.2%) compared with 24% in the SGLT2i group.
Cardiovascular benefits also emerge in studies. For patients with both obesity and heart disease risk factors, the medication’s protective effects might justify continued use regardless of weight stability.
The decision to stop or continue should involve thorough discussion with healthcare providers, weighing costs, benefits, side effects, and individual health priorities.
Common Mistakes That Undermine Maintenance
Understanding what doesn’t work is as important as knowing what does.
Assuming Results Will Maintain Themselves
The biggest mistake? Treating Ozempic like a permanent fix rather than a temporary tool.
Weight loss creates new health, but maintaining that health requires ongoing effort. Patients who assume the weight will stay off without active maintenance almost universally experience regain.
Stopping Abruptly Without a Plan
Cold-turkey discontinuation without preparation sets people up for failure.
Better approach: gradually build maintenance habits while still on medication, then transition slowly rather than stopping overnight.
Focusing Only on Diet
Diet matters, absolutely. But exercise—particularly resistance training—may matter more for long-term maintenance.
The metabolic benefits of muscle mass can’t be replaced by dietary restriction alone. Skipping exercise severely compromises maintenance odds.
Ignoring Small Regains
Five pounds becomes ten becomes twenty faster than most people expect.
Early intervention when weight starts creeping up prevents the need for major interventions later. This means acting on 3-5 pound gains, not waiting until clothes don’t fit.
The Role of Medical Support
Going it alone makes everything harder. Professional support significantly improves maintenance odds.
Endocrinologists can help navigate medication transitions. Registered dietitians provide personalized nutrition strategies that account for metabolic changes. Exercise physiologists design programs that preserve muscle mass.
Behavioral health professionals address the psychological aspects—the emotional eating patterns, stress responses, and mindset challenges that often derail maintenance efforts.
Research indicates an interprofessional team of nurses, primary care clinicians, pharmacists, and endocrinologists is important for care of patients prescribed this class of medications.
This multidisciplinary approach addresses obesity as the complex, multifaceted condition it is rather than reducing it to simple willpower.
What the Latest Research Tells Us
As we move through 2026, understanding of GLP-1 medications continues evolving.
Recent research explores how these medications transform eating control and hunger at a neurobiological level. According to a review published in Endocrinology, researchers are now exploring how GLP-1 receptor agonists can further transform obesity care and offer new possibilities for long-term weight management.
The focus is shifting from just achieving weight loss to understanding sustainable maintenance. Real-world studies comparing different management strategies provide increasingly practical guidance.
One thing becomes clearer with each study: there’s no single “right” answer. Individual responses vary tremendously based on genetics, lifestyle factors, support systems, and underlying metabolic health.
Setting Realistic Expectations
Managing expectations matters as much as managing weight.
Perfect maintenance—keeping off every single pound—is rare. Some regain is normal and doesn’t represent failure. Maintaining 70-80% of weight lost represents success, not disappointment.
The goal isn’t perfection. It’s meaningful, sustained improvement in health markers, quality of life, and metabolic function.
Someone who loses 50 pounds and keeps off 40 has achieved something remarkable, even if that final 10 pounds creeps back. That’s still life-changing weight loss with significant health benefits.
| Maintenance Outcome | Percentage Kept Off | Realistic Assessment |
|---|---|---|
| Excellent | 90-100% | Rare but possible with comprehensive support |
| Good | 70-89% | Achievable goal for many with consistent effort |
| Fair | 50-69% | Still clinically meaningful, better than no intervention |
| Poor | Less than 50% | Suggests need for resumed or alternative treatment |
Frequently Asked Questions
Weight regain timing varies considerably among individuals. Some people notice appetite increases within days of their final dose, with weight starting to climb within weeks. Others maintain stable weight for months before regaining. The rate and extent of regain depends heavily on what maintenance strategies are implemented after stopping.
Yes, maintaining weight without medication is possible, though challenging. Research shows it requires a comprehensive approach including 200-250 minutes of weekly exercise with strength training, dietary modifications, environmental changes, and regular monitoring. Success rates improve when multiple strategies are combined rather than relying on any single approach.
Appetite typically returns within days to weeks after stopping GLP-1 medications. Many patients report feeling hungrier than before they started treatment. The medication suppresses hunger signals, and when it’s discontinued, those signals return at full strength. This appetite increase is one of the primary drivers of weight regain after stopping.
Yes. Research from Vanderbilt University found that patients who transitioned to generic, older-generation antiobesity medications after stopping GLP-1 drugs maintained an average of 18.3% body weight loss at 12 months. This approach offers a more affordable option for continued pharmaceutical support, though it still requires prescription and medical supervision.
Guidelines recommend at least 200 to 250 minutes of moderate-intensity physical activity each week, along with regular strength training to maintain muscle mass. This amount is higher than general health recommendations because it addresses the metabolic adaptations that occur after weight loss, which make the body more efficient at regaining weight.
For patients with type 2 diabetes, blood sugar levels often increase after stopping GLP-1 medications because these drugs have glucose-lowering effects beyond their impact on weight. Patients may need to transition to or intensify other diabetes medications. According to research cited in NCBI resources, metformin remains the preferred first-line therapy for treating type 2 diabetes according to the American Diabetes Association, and patients stopping GLP-1 drugs should work with their healthcare provider to adjust their diabetes management plan.
Research suggests that reduced-frequency maintenance dosing can preserve weight loss outcomes while reducing treatment burden and cost. Studies found that structured de-escalation—spacing out doses rather than stopping completely—represents a promising strategy. This approach may be preferable to complete discontinuation for patients who can afford reduced dosing and want to maintain pharmaceutical support.
The Bottom Line on Weight Maintenance
So is it possible to keep weight off after Ozempic? Yes, but it requires realistic expectations and sustained effort.
The most successful approaches combine multiple strategies: transitioning to alternative medications or reduced dosing, implementing intensive exercise programs with strength training, making dietary modifications, and building environmental supports that make healthy choices easier.
Weight regain after stopping GLP-1 medications is common but not inevitable. The degree of regain varies tremendously based on what patients do after discontinuation.
For some people, continuing medication long-term—either at full strength or reduced frequency—may be the most practical and health-promoting choice. Obesity is a chronic condition, and there’s no shame in using pharmaceutical tools for ongoing management.
The key is approaching maintenance as seriously as the initial weight loss phase. That means planning ahead, building new habits while still on medication, enlisting professional support, and acting quickly when weight starts creeping back.
Research continues evolving. Studies on medication transitions, reduced-frequency dosing, and maintenance strategies provide increasingly practical guidance. What worked in 2023 may be refined by new evidence in 2026 and beyond.
But the fundamentals remain constant: sustainable weight maintenance requires addressing the biological, behavioral, and environmental factors that influence weight. Single interventions rarely succeed long-term. Comprehensive, multifaceted approaches offer the best odds of lasting success.
If you’re considering stopping Ozempic or similar medications, start the conversation with your healthcare provider early. Develop a detailed maintenance plan before your final dose. Success is possible—but it won’t happen by accident.
