Quick Summary: Yes, late ovulation is possible and occurs when ovulation happens after day 21 of your menstrual cycle. While it can result from stress, hormonal imbalances, PCOS, or thyroid issues, late ovulation doesn’t necessarily prevent pregnancy—though it may slightly reduce fertility chances and make conception timing more challenging.
The textbook menstrual cycle gets described as 28 days with ovulation happening on day 14. Neat, predictable, easy to track.
Reality? Not so simple.
Many women ovulate later than expected—sometimes significantly later. And that raises an important question: is late ovulation actually a problem, or just normal variation?
Here’s the thing though—late ovulation is incredibly common. Research analyzing 612,613 ovulatory cycles from 124,648 users found that cycle lengths vary dramatically between individuals, with ovulation timing showing substantial differences even among healthy women.
This article breaks down what late ovulation means, what causes it, how it affects fertility, and when it’s worth investigating further.
What Counts as Late Ovulation?
Before addressing whether ovulation can happen late, it helps to define what “late” actually means.
In a typical 28-day cycle, ovulation occurs around day 14—roughly in the middle of the cycle. But research from the National Institute of Environmental Health Sciences indicates that the fertile window varies significantly among women, with only approximately 30% experiencing it within days 10-17.
Most reach their fertile window earlier, and others much later.
The Medical Definition
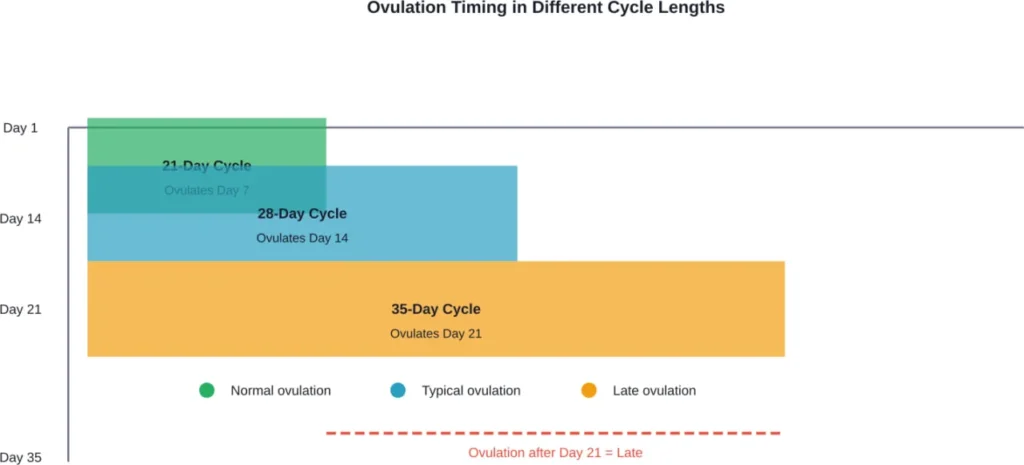
Late ovulation is generally defined as ovulation that occurs after day 21 of the menstrual cycle. This definition assumes counting starts on the first day of menstrual bleeding.
However, that definition requires some context. A woman with a 35-day cycle who ovulates on day 21 isn’t experiencing late ovulation—she’s ovulating right on schedule for her cycle length.
The more precise way to think about ovulation timing: it typically happens approximately 14 days before the next period begins. This luteal phase (the time between ovulation and menstruation) remains relatively constant at about 14 days for most women.
Normal Cycle Variation
Around 84% of women have cycles that are longer or shorter than the standard 28 days. Anything between 21 and 35 days is considered normal.
Analysis of real-world data from 124,648 users of the Natural Cycles app revealed that the mean cycle length was 29.3 days across 612,613 ovulatory cycles. The mean follicular phase length was 16.9 days (95% CI: 10–30).
This variability in the follicular phase is what creates different ovulation timing between women and between cycles for the same woman.
What Causes Late Ovulation?
Late ovulation doesn’t happen randomly. Several factors can delay the release of an egg from the ovary.
Stress and Lifestyle Factors
Physical or emotional stress can disrupt the hormonal signals that trigger ovulation. The hypothalamus—the brain region controlling reproductive hormones—is sensitive to stress.
Intense exercise, sudden weight changes, insufficient sleep, or major life stressors can all delay ovulation. The body essentially hits pause on reproduction when it perceives conditions aren’t optimal.
Polycystic Ovary Syndrome (PCOS)
PCOS is one of the most significant contributors to irregular and late ovulation. According to the World Health Organization, PCOS affects an estimated 10–13% of reproductive-aged women (WHO data) and is the most common cause of anovulation among women globally.
Women with PCOS produce higher than normal androgen levels, which interfere with the development and release of eggs. This can result in irregular cycles, delayed ovulation, or cycles where ovulation doesn’t occur at all.
It is estimated that up to 70% of women with PCOS worldwide do not know they have this condition.
Thyroid Disorders
Both hypothyroidism (underactive thyroid) and hyperthyroidism (overactive thyroid) can disrupt ovulation timing. The thyroid produces hormones that regulate metabolism and also influence reproductive hormone production.
When thyroid function is off, it can lengthen the follicular phase and delay ovulation.
Hormonal Imbalances
The process of ovulation requires precise coordination between several hormones: follicle-stimulating hormone (FSH), luteinizing hormone (LH), estrogen, and progesterone.
Disruptions in any of these can delay ovulation. High prolactin levels, low progesterone, or insufficient LH surge can all contribute to late ovulation.
Medications and Contraceptive Transitions
Coming off hormonal birth control can temporarily cause irregular ovulation as the body readjusts to producing its own reproductive hormones. This transition period varies—some women ovulate normally within a month, others take several months to regulate.
Certain medications, including some antidepressants and antipsychotics, can also affect ovulation timing.
Perimenopause
As women approach menopause, ovulation becomes less regular. The follicular phase often lengthens, causing later ovulation or skipped ovulation altogether.
This typically begins in the late 30s or early 40s, though timing varies considerably.
| Cause | How It Affects Ovulation | Additional Notes |
|---|---|---|
| Stress | Disrupts hypothalamic signals | Can cause temporary delays |
| PCOS | Excess androgens prevent egg release | Affects 10-13% of women |
| Thyroid disorders | Alters reproductive hormone production | Both hypo- and hyperthyroidism |
| Hormonal imbalances | Disrupts FSH, LH, estrogen coordination | May affect egg development |
| Post-contraceptive | Body readjusts to natural hormone production | Usually temporary |
| Perimenopause | Declining ovarian reserve and function | Typically begins late 30s-40s |
Symptoms and Signs of Late Ovulation
How can someone tell if they’re ovulating late?
The symptoms aren’t dramatically different from normal ovulation—the timing is what changes.
Delayed Period
If ovulation happens late, the period will also arrive later than expected (assuming the luteal phase stays constant at around 14 days). A woman who typically has a 28-day cycle might suddenly have a 35-day cycle because ovulation was delayed.
Ovulation Predictor Kit Results
LH urine tests (ovulation predictor kits) can detect the LH surge that precedes ovulation by 24-36 hours. LH urine tests are approximately 97% accurate, while LH and estrogen tests (such as Clearblue digital monitors) are 95-97% accurate.
Women tracking ovulation may notice positive results appearing later in their cycle than usual—or not at all if the surge is missed.
Basal Body Temperature Pattern
Basal body temperature (BBT) rises slightly after ovulation due to increased progesterone. Women charting their temperatures will see the temperature shift occurring later in the cycle than expected.
Cervical Mucus Changes
Fertile cervical mucus—clear, stretchy, and resembling raw egg whites—appears around ovulation. This change may occur later than day 14 in women experiencing late ovulation.
Physical Symptoms
Some women experience mild cramping or twinges (mittelschmerz) during ovulation. Breast tenderness, increased libido, and bloating may also occur. The timing of these symptoms can indicate when ovulation happens.
Can You Still Get Pregnant with Late Ovulation?
This is the critical question for women trying to conceive.
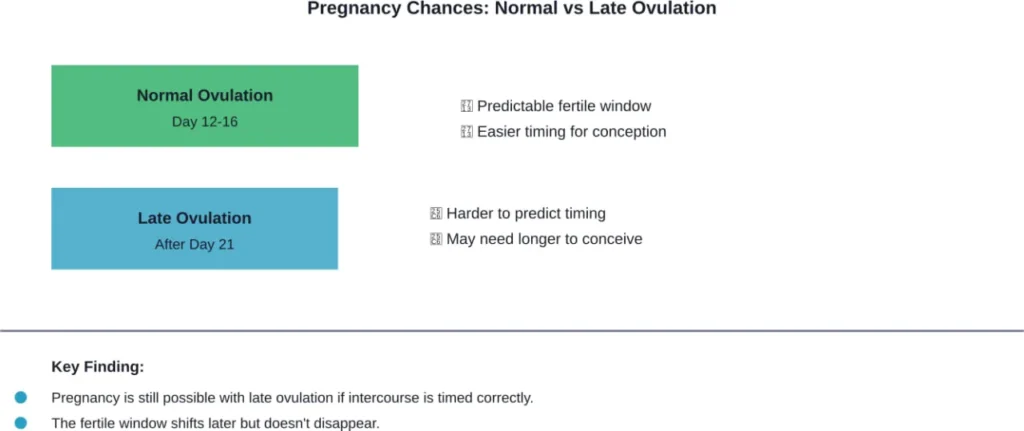
The short answer? Yes, pregnancy is still possible with late ovulation.
The Fertility Window
Research from the National Institute of Environmental Health Sciences (Wilcox et al., BMJ 2000) found that the fertile window timing varies significantly among women.
A man’s sperm can survive inside a woman’s body for about 3 days (and sometimes up to 5 days) after sexual intercourse. A woman’s egg only lives for about 12-24 hours after ovulation. This creates a six-day fertile window each cycle.
Late ovulation doesn’t eliminate this window—it just shifts it later in the cycle. If a woman correctly identifies when late ovulation is occurring and times intercourse accordingly, conception remains possible.
Potential Challenges
That said, late ovulation can present some fertility challenges.
Research from Boston University School of Public Health found that women with cycles of 26 days or fewer had reduced chances of becoming pregnant, with an average cycle length among participants of 29 days.
The study didn’t specify exact reduction percentages, but the association suggests that irregular ovulation timing may slightly decrease fertility odds.
Egg Quality Considerations
There’s some debate about whether late ovulation affects egg quality. The concern is that eggs taking longer to mature might not be as viable.
However, most research suggests that occasional late ovulation doesn’t significantly impact egg quality. Chronic issues causing consistently late ovulation (like PCOS or thyroid disorders) may have broader effects on fertility, but the timing itself isn’t the primary problem.
Luteal Phase Concerns
A short luteal phase (fewer than 10 days) can prevent successful implantation even if fertilization occurs. Some women with late ovulation also have shortened luteal phases, which can reduce pregnancy chances.
But this isn’t universal—many women with late ovulation maintain a normal 14-day luteal phase.
How to Track Late Ovulation
Identifying late ovulation requires more careful tracking than assuming ovulation happens on day 14.
Ovulation Predictor Kits
OPKs detect the LH surge that precedes ovulation. For women with irregular cycles, testing should start earlier and continue longer than standard kit instructions suggest.
Tests combining LH and estrogen detection show 95-97% accuracy in identifying the fertile window.
Basal Body Temperature Charting
Daily temperature tracking reveals ovulation after it occurs (when the temperature rises). While this doesn’t help with timing intercourse for the current cycle, it establishes patterns for future cycles.
Consistency is crucial—temperatures must be taken at the same time each morning before getting out of bed.
Cervical Mucus Monitoring
Checking cervical mucus changes throughout the cycle helps identify the fertile window in real time. Fertile-quality mucus appears in the days leading up to ovulation.
Fertility Tracking Apps
Apps that incorporate multiple data points (temperature, cervical mucus, OPK results) provide more accurate predictions than apps relying solely on calendar calculations.
Analysis of data from app users revealed significant variation in cycle characteristics, demonstrating that personalized tracking beats standardized predictions.
Does Late Ovulation Affect Your Period?
Yes, but not in the way many women expect.
Late ovulation delays the period—it doesn’t typically make the period itself abnormal. Since the luteal phase remains relatively constant at 14 days, a period will arrive approximately two weeks after ovulation occurs, regardless of when ovulation happens.
A woman who ovulates on day 24 will likely get her period around day 38, resulting in a longer overall cycle.
Distinguishing Late Ovulation from Pregnancy
A delayed period raises the question: late ovulation or pregnancy?
If ovulation was late, the period will eventually arrive (assuming fertilization didn’t occur). If conception happened, the period won’t come at all.
Pregnancy tests become accurate about 10-14 days after ovulation—roughly around the time a period would be expected. Testing too early can produce false negatives.
Treatment Options for Late Ovulation
Whether late ovulation needs treatment depends on the underlying cause and whether someone is trying to conceive.
Lifestyle Modifications
For stress-related ovulation delays, addressing the stressor can restore normal timing. Adequate sleep, stress management techniques, moderate exercise, and maintaining stable body weight all support regular ovulation.
Treating Underlying Conditions
PCOS management often includes medications like metformin or letrozole to promote regular ovulation. There is currently no cure for PCOS, but lifestyle changes, medications and fertility treatments can reduce symptoms, increase fertility rates and protect longer-term health.
Thyroid disorders require hormone replacement or suppression therapy to normalize thyroid levels, which typically restores regular ovulation.
Ovulation-Inducing Medications
Clomiphene citrate (Clomid) and letrozole are commonly prescribed to stimulate ovulation in women who ovulate irregularly or not at all. These medications increase FSH production, encouraging follicle development and egg release.
Fertility Treatments
For women struggling to conceive due to late or absent ovulation, assisted reproductive technologies may be recommended. These range from timed intercourse with ovulation induction to intrauterine insemination (IUI) or in vitro fertilization (IVF).
Supplements
Some evidence suggests inositol supplements may help regulate ovulation in women with PCOS. Vitamin D, omega-3 fatty acids, and CoQ10 have also been studied for fertility support, though research results vary.
| Treatment Type | Best For | Considerations |
|---|---|---|
| Lifestyle changes | Stress-related delays | First-line approach; no side effects |
| Thyroid medication | Thyroid disorders | Requires ongoing monitoring |
| Metformin | PCOS-related issues | Improves insulin sensitivity |
| Clomid/Letrozole | Ovulation induction | Prescription required; monitoring needed |
| Supplements | Supportive therapy | Evidence varies; discuss with provider |
| Assisted reproduction | Multiple failed cycles | More intensive; higher cost |
When to See a Doctor About Late Ovulation
Not every instance of late ovulation warrants medical attention. Occasional variations are normal.
But certain situations do call for consultation with a healthcare provider.
Consistently Irregular Cycles
If cycles regularly vary by more than seven days, or if they’re consistently longer than 35 days or shorter than 21 days, evaluation is appropriate.
Difficulty Conceiving
Standard guidance suggests seeking fertility evaluation after 12 months of trying to conceive for women under 35, or after six months for women over 35.
However, if late or absent ovulation is suspected, earlier consultation makes sense.
Other Symptoms Present
Late ovulation accompanied by excessive hair growth, severe acne, significant weight changes, fatigue, or other concerning symptoms may indicate PCOS, thyroid disorders, or other conditions requiring treatment.
After Discontinuing Birth Control
If regular cycles don’t return within three to six months after stopping hormonal contraceptives, medical evaluation can determine whether intervention is needed.
Understanding the Bigger Picture
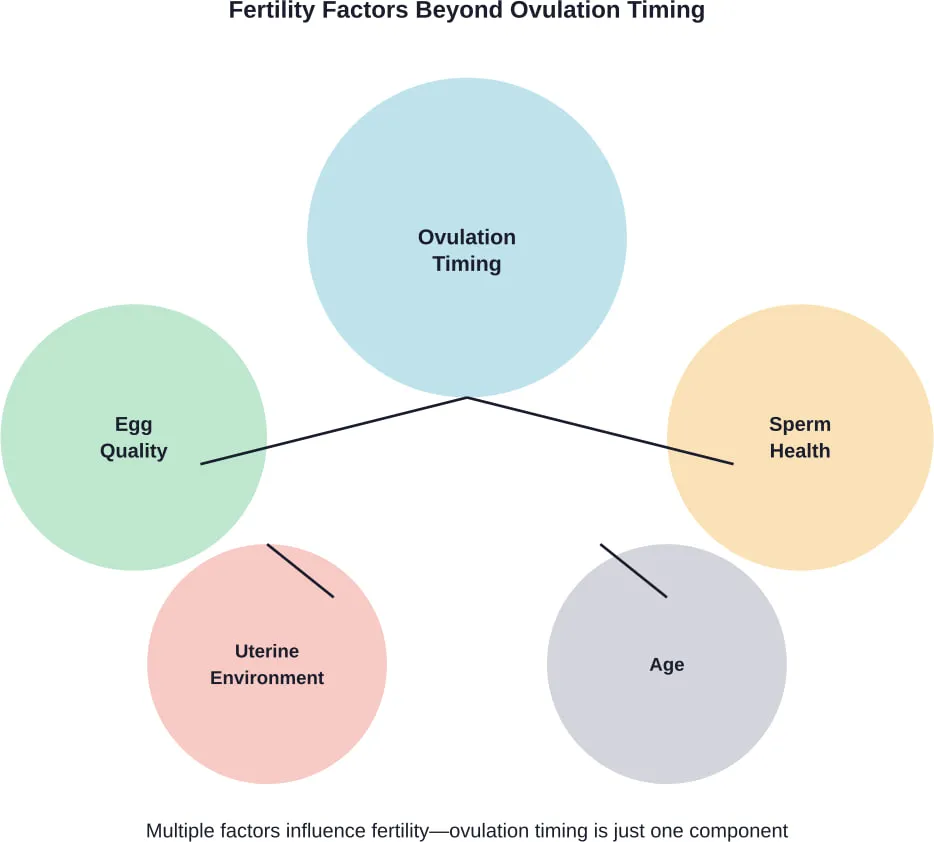
Late ovulation is one piece of a larger fertility puzzle.
Research from the National Institute of Environmental Health Sciences (Wilcox et al., BMJ 2000) found that the fertile window timing varies significantly among women.
This variability is normal—not pathological.
The key is understanding individual patterns rather than comparing to textbook averages. What matters isn’t whether ovulation happens on day 14, but whether it happens consistently enough to create opportunities for conception.
Age and Ovarian Reserve
Age affects fertility independently of ovulation timing. Research from UC San Francisco and Chan Zuckerberg Biohub San Francisco shows that the surrounding cells and tissues of the ovary play a crucial role in how eggs mature and how quickly fertility wanes.
From age 25 to 40, a woman’s chance of conceiving each month decreases drastically, and by age 50, after menopause, ovarian function ceases.
Male Fertility Factors
Conception requires both partners. Approximately half of fertility challenges involve male factors such as sperm count, motility, or morphology.
Focusing solely on ovulation timing without considering male fertility provides an incomplete picture.
Frequently Asked Questions
No, women don’t ovulate twice in the same cycle. However, both ovaries can release an egg during the same ovulation event (within 24 hours), which can result in fraternal twins. Once ovulation occurs, hormonal changes prevent another egg from being released until the next cycle.
Not necessarily. Late ovulation delays the progesterone surge, but doesn’t automatically mean progesterone levels are inadequate. However, some conditions causing late ovulation (like PCOS) can also involve low progesterone. Testing can determine actual hormone levels.
Absolutely. A single stressful event or period of high stress can delay ovulation for that cycle. Once stress resolves, ovulation typically returns to its normal pattern. Chronic stress tends to cause more persistent ovulation irregularities.
Wait approximately 14 days after confirmed or suspected ovulation. Testing earlier often produces false negatives because implantation takes 6-12 days after ovulation, and pregnancy hormones need time to reach detectable levels. If ovulation was on day 24, test around day 38.
Current research doesn’t show a direct link between late ovulation and increased miscarriage risk. However, conditions causing late ovulation (like thyroid disorders or PCOS) may independently affect pregnancy outcomes. Proper management of underlying conditions helps minimize risks.
Yes, several scenarios can cause this. The LH surge might be brief and missed between testing times. Some women have lower LH levels that don’t trigger positive results on standard tests. Testing at the wrong time of day or insufficient urine concentration can also produce false negatives.
It can be slightly more challenging, primarily because timing is less predictable. The fertile window still exists—it just shifts later. Women who accurately identify late ovulation and time intercourse accordingly can still conceive successfully. The underlying cause of late ovulation may have more impact on fertility than the timing itself.
Moving Forward with Late Ovulation
So, is it possible to ovulate late?
Not only is it possible—it’s relatively common.
Late ovulation represents normal biological variation for many women. For others, it signals an underlying condition that benefits from treatment. The distinction matters.
Understanding personal ovulation patterns provides valuable information whether someone is trying to conceive, avoid pregnancy, or simply monitor reproductive health.
The American College of Obstetricians and Gynecologists emphasizes that the menstrual cycle should be considered a vital sign—an important indicator of overall health status.
Tracking cycles, noting changes, and recognizing patterns helps women advocate effectively for their health. Late ovulation doesn’t necessarily mean something is wrong, but it does warrant attention and, in some cases, medical evaluation.
Most importantly, late ovulation doesn’t eliminate pregnancy possibilities. It changes the timeline and may require more careful tracking, but conception remains achievable for most women experiencing delayed ovulation.
If late ovulation is affecting fertility attempts or causing concern, consulting with a healthcare provider or reproductive endocrinologist can provide personalized guidance based on individual circumstances, health history, and fertility goals.
The takeaway? Late ovulation happens. Understanding why, recognizing when it requires intervention, and learning how to work with individual cycle patterns empowers women to make informed decisions about their reproductive health.
