Quick Summary: Yes, it’s possible to skip a period safely using hormonal birth control methods like pills, patches, or rings. According to ACOG, skipping periods is medically safe and healthy—monthly bleeding during birth control isn’t necessary for health. Whether missing a period naturally or intentionally suppressing it, understanding the causes and methods helps individuals make informed decisions about menstrual management.
The idea of skipping periods sounds too good to be true for many people. But here’s the thing—it’s not only possible, it’s completely safe when done correctly.
Whether periods interfere with athletic performance, travel plans, or simply cause unwanted symptoms, the medical community has clear guidance on menstrual suppression. And the science behind it might surprise anyone who’s been told monthly bleeding is “necessary.”
Understanding Period Suppression: The Medical Perspective
According to the NIH’s StatPearls medical database, menstruation occurs in approximately 26% of the world’s population. Medication-induced secondary amenorrhea—the medical term for intentionally stopping periods—uses hormonal contraceptives or other medications to decrease menses or achieve complete amenorrhea.
The key insight? Withdrawal bleeding that occurs during typical hormonal contraceptive use isn’t required for health. This bleeding differs entirely from a natural menstrual period.
ACOG confirms that using birth control to have fewer periods is normal and healthy, regardless of the reason. The monthly bleed during birth control placebo weeks was originally included to mimic natural cycles and gain social acceptance—not for medical necessity.
How Birth Control Enables Period Skipping
Hormonal birth control methods provide the most reliable way to skip periods intentionally. These methods work by maintaining consistent hormone levels that prevent the endometrial lining from building up and shedding.
Birth Control Pills and Vaginal Rings
According to the CDC’s 2024 contraceptive guidelines, combined hormonal contraceptives (CHCs) contain both estrogen and progestin. These include combined oral contraceptives, transdermal patches, and combined vaginal rings.
To skip periods with these methods, individuals simply continue taking active pills or keep the ring in place continuously, skipping the placebo week entirely. This maintains steady hormone levels without the drop that triggers withdrawal bleeding.
Progestin-only pills work differently. The CDC notes that three formulations are currently available in the United States: norethindrone, norgestrel, and drospirenone.
Long-Acting Methods
Intrauterine devices offer another option. ACOG reports that five IUDs are currently marketed in the United States—one copper-containing IUD and four levonorgestrel-releasing intrauterine devices (LNG-IUDs).
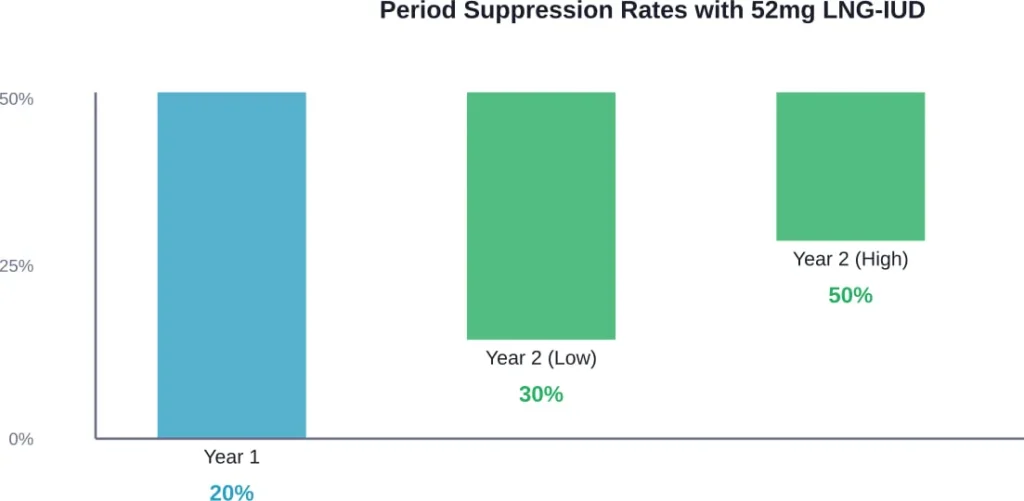
The higher-dose LNG-IUD containing 52 mg of levonorgestrel shows particularly strong results for period suppression. After one year of use, 20% of users report having no periods. After two years, 30% to 50% of users report having no periods.
Natural Causes of Missed Periods
Not all skipped periods result from intentional suppression. Several natural factors can cause periods to disappear temporarily when pregnancy isn’t the cause.
Stress and Lifestyle Changes
Intense stress affects the hormones that regulate menstruation. Major life changes, excessive exercise, or significant weight fluctuations can all disrupt normal cycles.
Athletes in particular may experience amenorrhea when training intensity increases dramatically or body fat percentage drops below certain thresholds.
Age-Related Changes
During the later stage of perimenopause, periods may not occur for more than 60 days. The later stages of perimenopause frequently involve irregular cycles and skipped periods.
On the other end of the age spectrum, irregular periods are completely normal when menstruation first begins. Cycles typically take time to regulate during adolescence.
Primary Ovarian Insufficiency
UCLA Health reports that Primary Ovarian Insufficiency (POI), also known as premature ovary failure, affects about 1% of females. This condition causes estrogen levels to drop and ovaries to stop working before age 40.
Medical Conditions
Certain health conditions directly impact menstruation. Polycystic ovary syndrome (PCOS), thyroid disorders, and bleeding disorders all commonly cause irregular or absent periods.
According to ACOG, bleeding disorders are found in approximately 20% of adolescent girls who present for evaluation of heavy menstrual bleeding, compared to 1-2% frequency in the general population.
| Cause Category | Common Examples | Typical Duration |
|---|---|---|
| Lifestyle Factors | Stress, excessive exercise, weight changes | Temporary, resolves with lifestyle adjustment |
| Age-Related | Perimenopause, early adolescence | Months to years during transition periods |
| Hormonal Conditions | PCOS, thyroid disorders, POI | Ongoing without treatment |
| Intentional Suppression | Hormonal birth control use | Continues as long as method is used |
Safety and Long-Term Considerations
The most common question about period suppression concerns safety. Research provides clear answers.
Manipulating the menstrual cycle through hormonal contraception is widely recognized as safe. The NIH confirms that withdrawal bleeding periods during hormonal contraceptive use are not required for health.
What about fertility? Continuous use of birth control pills or rings doesn’t make it harder to get pregnant later. Fertility returns to baseline levels after stopping hormonal contraception, regardless of whether it was used continuously or cyclically.
Some individuals experience breakthrough bleeding when first starting continuous hormonal contraception. According to the CDC’s 2024 guidelines on managing bleeding irregularities, this typically decreases over time as the body adjusts.
Methods for Skipping Periods
Different birth control methods offer varying levels of control over menstrual timing.
Continuous-Use Birth Control
With continuous-use birth control, active hormonal pills are taken every day without any placebo breaks. Some products are specifically formulated for continuous use, while standard monthly packs can be used continuously by skipping placebo weeks.
Vaginal rings work similarly—instead of removing the ring after three weeks, a new ring is inserted immediately.
Extended-Use Protocols
Extended-use differs slightly from continuous-use. Instead of having periods monthly, they occur every few months—typically quarterly. This reduces annual periods from 12-13 down to just four.
Some birth control pills are pre-packaged for extended use, with 84 active pills followed by seven placebo pills.
Injectable and Implant Options
Hormonal injections and implants frequently result in reduced bleeding or complete amenorrhea, though this varies by individual. These methods don’t require daily attention, making them convenient for long-term period management.

When to Consult a Healthcare Provider
While skipping periods intentionally with birth control is safe, unexplained missed periods warrant medical attention in certain situations.
Consult a doctor if periods stop suddenly without using hormonal contraception, especially when accompanied by other symptoms like severe pain, unusual discharge, or dramatic weight changes.
According to Stanford Medicine, adolescents experiencing very heavy or prolonged periods lasting eight to nine days should seek medical evaluation. Coming home exhausted from school due to heavy bleeding isn’t normal and may indicate an underlying condition requiring treatment.
Anyone considering period suppression for medical reasons—such as bleeding disorders, disabilities, or conditions that make menstruation particularly difficult—should discuss options with their healthcare provider. ACOG provides specific guidance for menstrual suppression in various populations, including transgender and gender-diverse patients, and those with physical or cognitive disabilities.
Common Misconceptions About Skipping Periods
Several myths persist about period suppression despite clear medical evidence.
The biggest misconception? That monthly bleeding “cleanses” the body or is necessary for health. This isn’t true. The withdrawal bleed during birth control differs entirely from a natural menstrual period and serves no physiological purpose.
Another common worry suggests that skipping periods causes blood or tissue to “build up” inside the body. But hormonal contraception prevents the endometrial lining from thickening in the first place—there’s nothing to build up or shed.
Some believe continuous birth control use damages fertility. Research shows otherwise. Fertility returns to baseline after stopping hormonal contraception, whether used continuously or cyclically.
Frequently Asked Questions
Yes, continuous use of hormonal birth control to skip periods every month is medically safe. ACOG confirms that monthly bleeding during birth control use isn’t necessary for health, and individuals can skip periods as often as desired when using hormonal contraception properly.
No, continuous use of birth control doesn’t affect future fertility. Fertility returns to baseline levels after stopping hormonal contraception, regardless of whether it was used continuously or with monthly breaks.
Breakthrough bleeding commonly occurs when first starting continuous hormonal contraception as the body adjusts to constant hormone levels. According to CDC guidelines, this typically decreases over time. If bleeding persists or becomes bothersome, consulting a healthcare provider about adjusting the method or dosage can help.
Period suppression with IUDs develops gradually. With the 52mg levonorgestrel IUD, about 20% of users report no periods after one year, increasing to 30-50% after two years. Results vary by individual.
Occasional missed periods can be normal, especially due to stress, significant weight changes, or excessive exercise. However, if periods stop for several months without an obvious cause, or if accompanied by concerning symptoms, medical evaluation is recommended to rule out underlying conditions.
Yes, birth control pills and vaginal rings offer the flexibility to schedule periods around important events. By continuing active pills or keeping the ring in place, periods can be delayed. Taking a break from active hormones triggers withdrawal bleeding within a few days, allowing scheduled timing.
No, skipping periods through hormonal contraception doesn’t increase health risks compared to cyclic use. The health risks associated with hormonal contraception remain the same whether used continuously or cyclically—the bleeding pattern itself doesn’t affect safety.
Making an Informed Decision
Period suppression represents a personal choice supported by medical evidence. Whether seeking relief from menstrual symptoms, managing medical conditions, or simply preferring fewer periods, safe and effective options exist.
The key is understanding which method aligns best with individual needs, lifestyle, and health considerations. Birth control pills and rings offer maximum flexibility and control. IUDs provide long-term suppression without daily management. Injectable methods reduce maintenance but offer less control over timing.
Talk with a healthcare provider about goals for period management. They can recommend the most appropriate method based on medical history, lifestyle factors, and personal preferences. And remember—choosing to have fewer periods or no periods is a medically sound decision that doesn’t compromise health or future fertility.
Ready to take control of menstrual timing? Schedule a consultation with an obstetrician-gynecologist or reproductive health specialist to explore which period suppression method works best for your situation.
