Quick Summary: Yes, sweating blood is medically possible through a rare condition called hematidrosis or hematohidrosis, where blood exudes from intact skin without injury. This extremely rare phenomenon occurs when capillaries rupture near sweat glands, typically triggered by intense stress or anxiety. Most cases resolve with treatment including beta-blockers, psychotherapy, or anti-anxiety medications.
Throughout history, accounts of people sweating blood have appeared in religious texts, battlefield reports, and medical journals. Jesus was described as sweating blood before his crucifixion. Leonardo da Vinci documented a soldier with bloody sweat after combat.
But is sweating blood actually possible?
The answer is yes. It’s called hematidrosis—and while extremely rare, it’s a documented medical condition recognized by dermatologists and psychiatrists worldwide.
What Is Hematidrosis?
Hematidrosis (also spelled hematohidrosis or haematidrosis) is a rare clinical phenomenon where blood exudes from uninjured skin or mucous membranes. The term comes from Greek: haîma meaning blood and hidrós meaning sweat.
According to research published in the Indian Journal of Dermatology, only a handful of cases have been reported in medical literature. The condition causes blood droplets to appear on intact skin, typically on the forehead, face, or other areas where sweat glands concentrate.
Here’s what makes it particularly unusual: the bleeding occurs spontaneously, without any visible cuts, wounds, or trauma to the skin.
How Common Is This Condition?
Hematidrosis is exceptionally rare. Medical literature contains only a handful of documented cases of hematidrosis. Research published in the Indian Journal of Psychiatry noted that the legitimacy of historical cases remains questionable, as most date before the 20th century when detailed laboratory tests weren’t available to exclude other bleeding disorders.
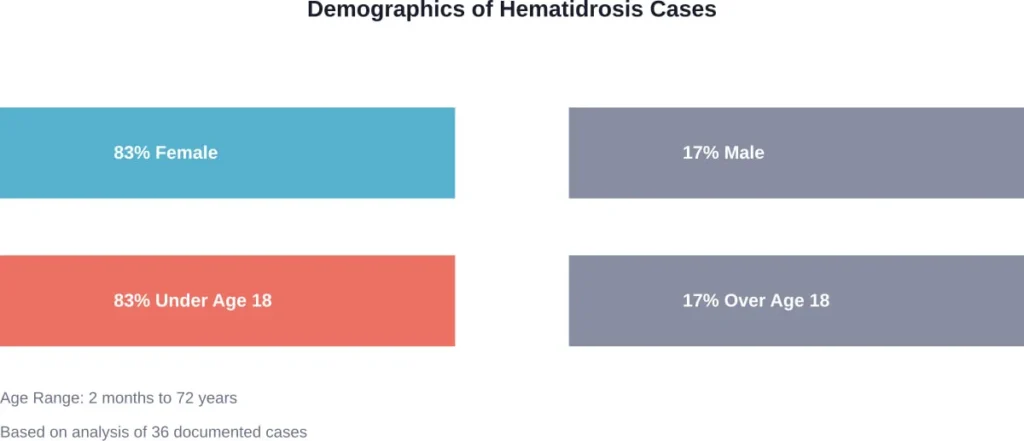
According to medical literature, the condition can occur at any age, from 2 months to 72 years of age, but rarely affects infants or the elderly. Analysis of 36 cases revealed that 83% were females, and the majority (83%) were under 18 years of age.
What Causes Sweating Blood?
The exact mechanism behind hematidrosis remains unclear, but medical researchers have identified several contributing factors.
The Stress Connection
Psychogenic causes are the most frequently identified trigger. Research published in the Indian Journal of Psychological Medicine documented a case where a young student experienced hematidrosis related to academic pressure. The child was punished for scoring 90-95% while her younger sibling scored 99%.
Another case report in Dermatology Reports described a 10-year-old Vietnamese girl who developed hematidrosis during COVID-19 quarantine due to separation anxiety disorder.
Extreme stress activates the body’s fight-or-flight response. One theory suggests this causes blood vessels surrounding sweat glands to constrict and then rupture under intense psychological pressure.
Other Potential Causes
While stress dominates case reports, researchers have suggested other possibilities:
- Component of systemic diseases
- Vicarious menstruation (bleeding from unusual sites during menstruation)
- Head injury or traumatic pressure
- Excessive physical exertion
- Blood clotting disorders (though these must be ruled out first)
According to the National Institutes of Health’s Genetic and Rare Diseases Information Center, the precise pathophysiology hasn’t been definitively proven.
Recognizing the Symptoms
Hematidrosis presents with distinctive characteristics that differentiate it from other bleeding disorders.
| Symptom | Description |
|---|---|
| Blood droplets on skin | Spontaneous appearance without injury |
| Common locations | Forehead, face, nose, palms, abdomen |
| Bleeding pattern | Episodic, typically lasting minutes |
| Associated symptoms | Headache, abdominal pain, anxiety |
| Triggering factors | Stress, fear, emotional distress |
When examined, the blood disappears as soon as it’s mopped, leaving no sign of trauma on the skin. Episodes are usually brief but can recur multiple times.
Research indicates that symptoms can persist for days to weeks before resolving, either spontaneously or with treatment.
How Doctors Diagnose Hematidrosis
Diagnosis requires ruling out other conditions that cause skin bleeding. Doctors perform comprehensive evaluations including:
Physical examination: Careful inspection of bleeding sites to confirm no visible wounds or trauma exist.
Laboratory tests: Complete blood count, coagulation studies, and platelet function tests to exclude bleeding disorders like thrombocytopenia or hemophilia.
Dermatological assessment: Skin biopsy may be performed to examine sweat glands and surrounding blood vessels.
Psychological evaluation: Since psychogenic factors predominate, psychiatric assessment often reveals underlying anxiety, stress disorders, or trauma.
The diagnosis is essentially one of exclusion—other causes must be ruled out before confirming hematidrosis.
Treatment Options That Work
While hematidrosis can be distressing, treatment is often effective. According to a 2021 literature review cited in Cureus, beta-blockers show remarkable success.
Treatment Effectiveness Data
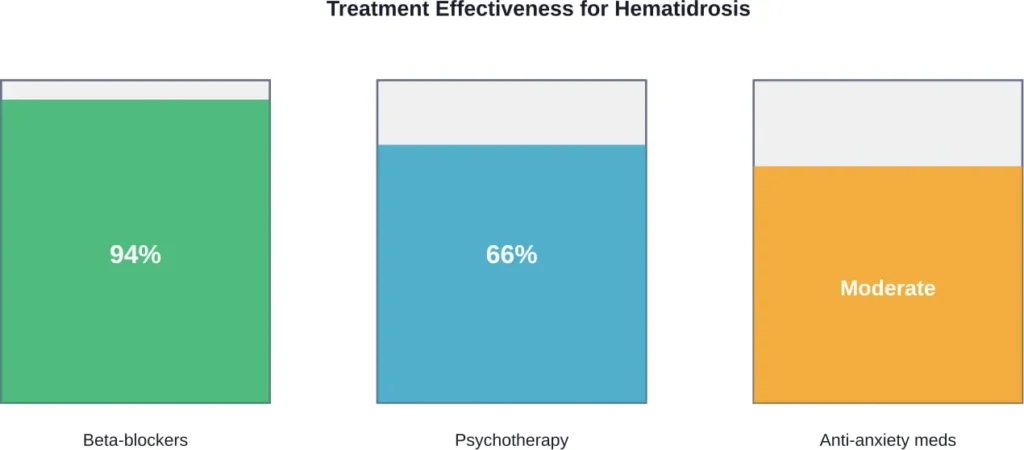
According to a 2021 literature review, treatment with beta-blockers had an effectiveness of up to 94%, while psychotherapy (including cognitive-behavioral therapy, relaxation techniques, and family education) had an effectiveness of 66%.
Common Treatment Approaches
| Treatment Type | How It Works | Success Rate |
|---|---|---|
| Beta-blockers | Regulate blood vessel response to stress | Up to 94% |
| Psychotherapy | Addresses underlying anxiety and stress | 66% |
| Anti-anxiety medications | Reduces stress response triggers | Moderate to high |
| Antidepressants | Stabilizes mood and stress hormones | Variable |
One case report published in the Indian Dermatology Online Journal described a 13-year-old boy treated with Alprazolam (0.25 mg daily for 10 days). While attempts to control sweating with aluminum hexahydrate were unsuccessful, the patient found relief through alternative medicine and breathing exercises, reporting no recurrence.
Most patients improve or achieve complete remission after treatment. The key is addressing both the physical symptoms and underlying psychological triggers.
Living With Hematidrosis
For those diagnosed with this condition, several factors matter for management and recovery.
Stress management: Learning relaxation techniques, meditation, and breathing exercises helps prevent episodes.
Medical monitoring: Regular follow-up with dermatology and psychiatry ensures comprehensive care.
Support systems: Family understanding and counseling support recovery, especially for pediatric cases.
According to the National Institutes of Health, because only about 5% of rare diseases have FDA-approved treatments, finding the right healthcare team to manage symptoms is essential. A team-based approach involving dermatologists, psychiatrists, and primary care physicians works best.
Frequently Asked Questions
No, hematidrosis isn’t considered life-threatening. While distressing and concerning, the condition doesn’t cause dangerous blood loss. Most cases resolve with appropriate treatment, and fatalities haven’t been documented in modern medical literature.
Episodes typically last several minutes, though duration varies by individual. The bleeding usually stops spontaneously or when the stress trigger is removed. Some patients experience multiple episodes over weeks before treatment achieves remission.
No. Hematidrosis involves blood exuding from intact skin without visible injury, whereas nosebleeds result from broken blood vessels inside the nose. The mechanisms and causes differ significantly.
Yes. Research shows that 83% of documented cases occur in individuals under 18 years old. Children experiencing severe academic pressure, family stress, or separation anxiety appear particularly susceptible.
No genetic or hereditary pattern has been established. Cases appear to be isolated incidents triggered by individual psychological or physiological factors rather than inherited genetic conditions.
Many patients achieve complete remission with proper treatment. However, if underlying stress triggers aren’t addressed, recurrence is possible. Ongoing stress management and psychological support reduce recurrence risk.
Careful examination reveals no cuts, scratches, or injury marks on the skin. Laboratory tests confirm normal clotting function. Psychiatric evaluation, skin biopsies, and observation during episodes help distinguish hematidrosis from self-inflicted wounds or factitious disorders.
The Bottom Line
Sweating blood isn’t just historical legend or religious metaphor—it’s a documented medical reality. Hematidrosis remains extremely rare, but for those who experience it, the condition is very real and understandably frightening.
The good news? Treatment works. With proper medical care combining medication, psychotherapy, and stress management, most patients see significant improvement or complete resolution.
If someone experiences unexplained bleeding from intact skin, especially during periods of intense stress, seeking medical evaluation is crucial. Early diagnosis and treatment lead to better outcomes and prevent the psychological distress that often accompanies this unusual condition.
Understanding that hematidrosis has recognized medical causes and effective treatments helps remove the mystery and stigma surrounding this rare phenomenon.
