Quick Summary: Yes, it is possible to take too much magnesium, though it’s rare from food alone. The tolerable upper intake level for supplemental magnesium is 350 mg/day for adults, with higher doses potentially causing diarrhea, nausea, and in severe cases, hypermagnesemia—a dangerous condition affecting heart rhythm and breathing. People with kidney problems face the highest risk.
Magnesium has become one of the most popular supplements on the market. Walk into any health store and you’ll find dozens of formulations promising better sleep, reduced anxiety, and improved muscle function.
But here’s the thing—just because something’s natural doesn’t mean you can take unlimited amounts. The question isn’t whether magnesium is beneficial. It absolutely is. The real question is: where’s the line between helpful and harmful?
Let’s break down what actually happens when magnesium intake goes too high.
Understanding Magnesium’s Role in Your Body
Magnesium serves as a cofactor in more than 300 enzyme systems throughout the body, according to the National Institutes of Health. These enzymes regulate everything from protein synthesis to muscle and nerve function, blood glucose control, and blood pressure regulation.
The adult human body contains about 25 grams of magnesium. Roughly 50-60% sits in your skeleton, with the remainder distributed in soft tissue and muscle. It’s the second most abundant intracellular cation after potassium.
So magnesium isn’t optional. It’s absolutely essential for survival.
That said, your body has sophisticated mechanisms for maintaining magnesium balance. Healthy kidneys can excrete excess magnesium efficiently. This is why magnesium toxicity is rare in people with normal kidney function.
The Official Upper Limit for Magnesium
In 1997, the Institute of Medicine established a tolerable upper intake level (UL) for magnesium supplementation. That limit? 350 mg per day for adults from supplemental sources only.
Notice the specification: supplemental sources. This UL doesn’t include magnesium from food.
The committee set this limit because some individuals experienced mild, reversible adverse effects—primarily diarrhea—at doses easily tolerated by others. According to research published in Advances in Nutrition, approximately 5% of men and >5% of women who used Mg supplements exceeded the UL of 350 mg/d.
Why 350 mg? That’s where gastrointestinal side effects became common enough to warrant caution. Not dangerous necessarily, but uncomfortable enough to limit further intake naturally.
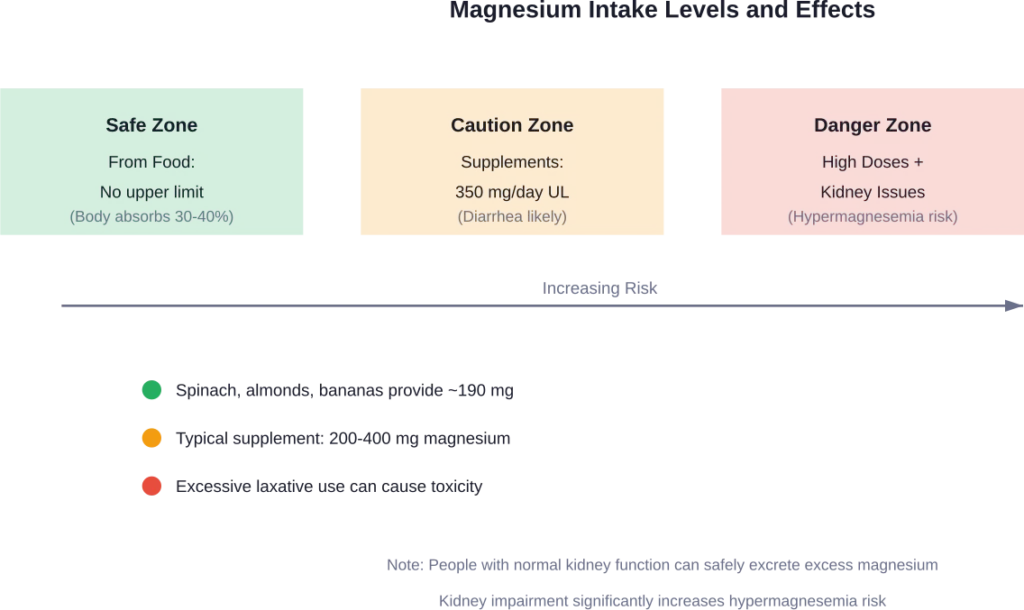
Can You Get Too Much Magnesium from Food Alone?
The short answer? It’s extremely unlikely.
Here’s why. The body typically absorbs only 30-40% of dietary magnesium from food sources. This low absorption rate acts as a natural protective mechanism.
Even magnesium-rich foods don’t pose a risk. One serving of spinach, an ounce of almonds, and a banana together provide about 190 mg of magnesium—nearly 60% of the daily recommendation for women and 45% for men. But remember, your body won’t absorb all of that.
The National Institutes of Health doesn’t set an upper limit for magnesium from food in healthy individuals. Your digestive system and kidneys work together to maintain balance.
That said, there’s a catch. If someone has compromised kidney function or takes certain medications that affect magnesium excretion, even dietary magnesium can accumulate.
What Happens When You Take Too Much Magnesium?
The Mild Stuff: Gastrointestinal Distress
The most common sign of excessive magnesium supplementation is diarrhea. This happens because unabsorbed magnesium in the intestines draws water into the bowel.
Other early symptoms include:
- Nausea and vomiting
- Abdominal cramping
- Loss of appetite
- General gastrointestinal discomfort
These symptoms are uncomfortable but reversible. Stop taking the supplement, and they typically resolve within a day or two.
Magnesium citrate and magnesium oxide are particularly likely to cause these effects because they’re less readily absorbed. That’s actually why magnesium citrate is used as a laxative.
The Serious Stuff: Hypermagnesemia
Now we’re talking about genuine magnesium toxicity. Hypermagnesemia means having excessively high magnesium levels in the blood.
This condition is rare in healthy people. But it’s potentially fatal when it occurs.
Symptoms of severe hypermagnesemia include:
- Irregular heartbeat or cardiac arrhythmias
- Dangerously low blood pressure (hypotension)
- Muscle weakness progressing to paralysis
- Slowed or difficult breathing (respiratory depression)
- Altered mental status, from drowsiness to coma
- Cardiac arrest in extreme cases
Medical literature documents fatal cases of hypermagnesemia, typically involving oral ingestion of magnesium-containing products like Epsom salts as laxatives or folk remedies. One reported case involved a 75-year-old woman who died after ingesting milk containing magnesium chloride.
Another case involved a 56-year-old man who developed bradycardia, hypotension, altered mental status, and respiratory depression requiring intubation after Epsom salt ingestion. His magnesium level was dangerously elevated.
Who’s Actually at Risk?
Certain groups face significantly higher risk of magnesium toxicity:
| Risk Group | Why They’re Vulnerable | Precautions Needed |
|---|---|---|
| People with kidney disease | Reduced ability to excrete excess magnesium | Avoid supplements unless prescribed; monitor levels |
| Elderly individuals | Often have reduced kidney function; bowel movement issues | Lower doses; medical supervision recommended |
| Those taking certain medications | Drug interactions affect magnesium absorption/excretion | Consult healthcare provider before supplementing |
| People using magnesium-containing laxatives | High magnesium doses from repeated laxative use | Follow dosing instructions; don’t exceed recommended use |
The FDA specifically warns against prolonged use of magnesium sulfate injection to stop pre-term labor in pregnant women. Administration for more than 5-7 days can lead to low calcium levels and bone problems in the developing baby, including osteopenia and fractures.
Additionally, long-term use of proton pump inhibitors (PPIs) can cause low magnesium levels—hypomagnesemia. This creates a tricky situation where people might supplement aggressively to compensate, potentially overcorrecting.
Medication Interactions with Magnesium
Magnesium doesn’t exist in isolation. It interacts with numerous medications, sometimes dangerously.
Key interactions include:
- Bisphosphonates: Magnesium can reduce absorption of these bone-strengthening drugs
- Antibiotics: Certain classes bind with magnesium, reducing effectiveness of both
- Diuretics: Some increase magnesium loss; others cause retention
- Muscle relaxants: Magnesium can enhance effects, potentially causing excessive muscle weakness
- Blood pressure medications: Combined effects may drop pressure too low
Anyone taking prescription medications should consult a healthcare provider before adding magnesium supplements.
Different Forms, Different Absorption Rates
Not all magnesium supplements are created equal. The form matters significantly.

Magnesium oxide contains about 60.3% elemental magnesium—so 1 gram provides 603 mg of actual magnesium. But absorption is only around 4%. That’s why it’s commonly used as a laxative rather than for correcting deficiency.
Magnesium glycinate and magnesium citrate offer better bioavailability with fewer gastrointestinal effects at therapeutic doses.
When reading supplement labels, look for elemental magnesium content. That’s what counts toward the 350 mg upper limit.
Signs You Should Stop Taking Magnesium Supplements
Listen to your body. These warning signs suggest you’re taking too much:
- Persistent diarrhea or loose stools
- Nausea that doesn’t resolve
- Unusual fatigue or weakness
- Confusion or difficulty concentrating
- Irregular heartbeat or palpitations
- Difficulty breathing or shortness of breath
Any cardiac or respiratory symptoms require immediate medical attention. Don’t wait to see if they resolve.
The Reality Check: How Common Is Magnesium Toxicity?
Real talk: hypermagnesemia is rare in the general population. Most reported cases involve specific circumstances—kidney disease, excessive laxative use, or medical administration errors.
Gastrointestinal distress is far more common than serious toxicity. Most people who exceed recommended doses simply experience uncomfortable digestive symptoms that prompt them to reduce intake naturally.
But rare doesn’t mean impossible. And for vulnerable populations—particularly those with kidney disease—the risks are very real.
Should You Worry About Combining Food and Supplement Sources?
Generally speaking, eating magnesium-rich foods while taking supplements within recommended doses poses minimal risk for healthy individuals.
Here’s why. That 350 mg upper limit applies specifically to supplemental magnesium. Dietary magnesium from food doesn’t count toward this threshold in people with normal kidney function.
However, always follow dosing instructions. Don’t assume that because food sources are safe, you can double or triple your supplement dose.
Treatment for Magnesium Overdose
For mild cases with just gastrointestinal symptoms, treatment is straightforward: stop taking magnesium supplements. Symptoms typically resolve within 24-48 hours.
Severe hypermagnesemia requires medical intervention:
- Intravenous calcium gluconate to counteract magnesium’s effects on the heart and muscles
- Intravenous fluids to support kidney function and dilute magnesium concentration
- Diuretics to increase magnesium excretion
- Dialysis in cases of kidney failure or life-threatening toxicity
According to medical research, in approximately one-quarter of cases involving PPI-induced hypomagnesemia, magnesium supplementation alone didn’t improve low levels. The PPI had to be discontinued.
Smart Supplementation Guidelines
If you’re going to supplement with magnesium, do it intelligently:
- Stay at or below 350 mg daily from supplements
- Take magnesium with food to minimize gastrointestinal effects
- Choose highly bioavailable forms like glycinate or citrate for general use
- Space doses throughout the day rather than taking one large dose
- Inform your doctor about all supplements you’re taking
- Get blood levels checked if you have kidney disease or take medications affecting magnesium
- Start with lower doses and increase gradually
For disease prevention and general health, a balanced diet that includes magnesium-rich foods often provides adequate amounts without supplementation.
Frequently Asked Questions
Magnesium supplements don’t typically cause kidney damage in healthy individuals. However, people with existing kidney disease can’t excrete excess magnesium properly, leading to dangerous accumulation. If you have kidney problems, consult a healthcare provider before supplementing.
The Recommended Dietary Allowance (RDA) is the average daily intake sufficient to meet nutrient requirements—about 400-420 mg for adult men and 310-320 mg for adult women from all sources. The tolerable upper limit (UL) of 350 mg applies only to supplemental magnesium and represents the threshold where adverse effects become more likely.
There’s no evidence that the body develops tolerance to magnesium requiring progressively higher doses. If supplements seem less effective over time, it may indicate an underlying condition affecting magnesium absorption or utilization. Consult a healthcare provider rather than increasing dosage.
Gastrointestinal symptoms like diarrhea typically appear within a few hours of taking excessive magnesium. More serious symptoms of hypermagnesemia develop over hours to days, depending on the dose and individual kidney function. Anyone experiencing cardiac or respiratory symptoms should seek immediate medical care.
Topical magnesium applications like sprays or lotions generally pose lower risk of systemic toxicity because absorption through skin is limited and variable. However, research on transdermal magnesium absorption remains limited. These products likely won’t provide therapeutic magnesium levels but also won’t cause toxicity in typical use.
Children can take magnesium supplements, but dosing differs significantly from adults. The upper limit varies by age, ranging from 65 mg for children 1-3 years to 350 mg for those 9 and older. Always consult a pediatrician before giving magnesium supplements to children, as their needs and tolerances differ from adults.
If you’ve taken significantly more than recommended and feel fine, stop taking magnesium and stay hydrated. If you experience diarrhea, nausea, or weakness, these typically resolve within a day. However, if you develop irregular heartbeat, difficulty breathing, extreme weakness, or confusion, seek emergency medical attention immediately as these could indicate dangerous hypermagnesemia.
The Bottom Line on Magnesium Safety
So, is it possible to take too much magnesium? Absolutely.
But context matters enormously. For healthy adults with normal kidney function eating a balanced diet and taking moderate supplements, the risk remains low. The body’s regulatory mechanisms—particularly kidney excretion—provide substantial protection.
The 350 mg supplemental upper limit exists for good reason. It’s not arbitrary. Exceeding it regularly increases the likelihood of uncomfortable gastrointestinal effects at minimum.
For people with kidney disease, elderly individuals, or those taking medications affecting magnesium metabolism, the stakes are considerably higher. Medical supervision isn’t optional—it’s essential.
The smartest approach? Get most of your magnesium from whole foods. Leafy greens, nuts, seeds, whole grains, and legumes provide magnesium alongside other beneficial nutrients and fiber. Supplement strategically and conservatively if blood tests reveal deficiency or your healthcare provider recommends it.
Don’t fall into the trap of thinking more is better. With magnesium, as with most nutrients, there’s a sweet spot. Stay within it, and you’ll get the benefits without the risks.
Need personalized guidance on magnesium supplementation? Consult with a healthcare provider or registered dietitian who can assess your individual needs, current health status, and medication regimen. They can help determine whether supplementation is appropriate and what dose makes sense for your specific situation.
