Quick Summary: Sleep deprivation triggers immediate effects like impaired cognition, mood changes, and weakened immunity, while chronic sleep loss increases risks for cardiovascular disease, diabetes, obesity, and mental health disorders. According to the CDC, adults need 7-8 hours of quality sleep nightly for optimal health. The body accumulates sleep debt that can only be repaid through adequate rest, not stimulants or willpower.
Sleep isn’t optional. It’s a biological necessity as fundamental as food or water.
Yet millions of people treat sleep like a luxury they can’t afford. Late nights working, scrolling through social media, or binge-watching shows have become normalized. It is estimated that 50 to 70 million Americans chronically suffer from a disorder of sleep and wakefulness, with many more simply not prioritizing adequate rest.
But what actually happens when the body doesn’t get the sleep it needs? The consequences extend far beyond feeling groggy the next morning.
Understanding Sleep Deprivation and Deficiency
Sleep deprivation occurs when someone gets less sleep than their body requires. According to the National Heart, Lung, and Blood Institute (NHLBI), this can happen in one intense period or accumulate gradually over time.
Sleep deficiency is broader. It includes not only insufficient sleep duration but also poor-quality sleep, sleeping at the wrong times relative to your body clock, or having untreated sleep disorders that fragment rest.
Here’s the thing though—the effects aren’t always obvious at first. Many people adapt to functioning on minimal sleep without realizing the damage accumulating beneath the surface.
How Much Sleep Do Adults Actually Need?
The American Academy of Sleep Medicine and Sleep Research Society recommend that adults obtain seven or more hours of sleep per night. This isn’t arbitrary—it’s based on extensive research linking sleep duration to health outcomes.
Most adults specifically need 7 to 8 hours of quality sleep every 24 hours to function optimally, according to CDC guidelines for emergency operations workers. Children and adolescents require even more:
| Age Group | Recommended Sleep Duration |
|---|---|
| Newborns (0-3 months) | 14-17 hours |
| Infants (4-12 months) | 12-16 hours including naps |
| Toddlers (1-2 years) | 11-14 hours including naps |
| Preschool (3-5 years) | 10-13 hours including naps |
| School-age (6-12 years) | 9-12 hours |
| Teens (13-18 years) | 8-10 hours |
| Adults (18+ years) | 7-8 hours |
The CDC notes that about 6 out of 10 middle school students and a similar proportion of high school students don’t get enough sleep on school nights. National data from 2010 showed that over 50% of night shift healthcare workers reported sleeping 6 or fewer hours daily—significantly below recommendations.
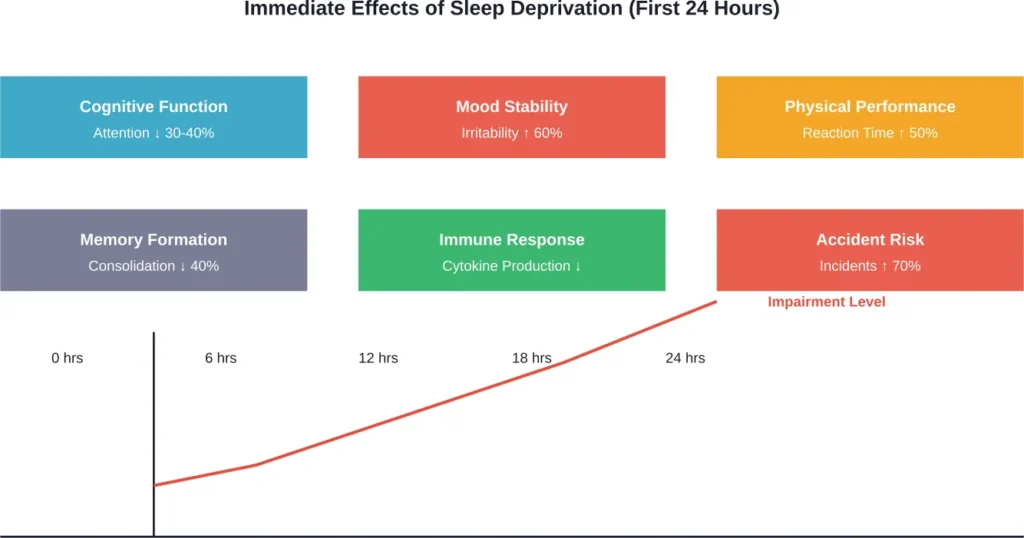
Immediate Effects: What Happens After One Night
Even a single night of inadequate sleep triggers measurable changes. The body responds almost immediately when it doesn’t get the rest it expects.
Cognitive Impairment and Brain Function
Sleep deprivation impairs multiple aspects of brain function. Research published in medical journals shows that cognitive performance declines rapidly without adequate rest.
The brain requires sleep for memory consolidation, learning, and clearing toxic cellular molecules. During sleep, cerebrospinal fluid flows at increased levels, and the interstitial space increases by 60%, successfully clearing beta-amyloid and other waste products that accumulate during waking hours.
Without this cleaning process, mental abilities suffer. Attention span shortens. Reaction times slow. Decision-making becomes impaired.
Sound familiar? That foggy feeling after a poor night’s rest isn’t just in your head—it’s a measurable decrease in cognitive capacity.
Mood Changes and Emotional Instability
According to the CDC’s NIOSH training materials, sleep deprivation significantly impairs mood and communication skills. Sleep-deprived individuals commonly experience irritability, anxiety, and depression.
The emotional regulation centers of the brain depend on adequate rest. Without it, people tend to view situations more negatively and may avoid communicating with difficult individuals because they perceive them through a more negative lens.
Confusion, reduced vigor, and fatigue at inappropriate times also become common. These mood disruptions affect not just personal well-being but also relationships and professional interactions.
Physical Performance Decline
Motor skills deteriorate without sleep. Coordination suffers. Physical stamina drops.
Athletes know this intuitively—sleep is when the body repairs muscle tissue and consolidates motor learning. Skipping rest doesn’t just mean feeling tired during a workout; it means genuinely reduced physical capability.
The Concept of Sleep Debt
Sleep debt accumulates when someone consistently gets less sleep than needed. According to the NHLBI, if someone loses 2 hours of sleep each night, they’ll have a sleep debt of 14 hours after just one week.
This debt doesn’t disappear on its own. The only way to pay it off is through adequate sleep—not caffeine, not willpower, not weekend catch-up sessions (though those help slightly).
Sleep debt seriously impairs performance. The CDC notes that when people lose sleep, cognitive and physical abilities decline in proportion to the accumulated deficit.
Real talk: Many people operate with massive sleep debts without realizing it. They’ve adapted to feeling suboptimal and consider it normal.
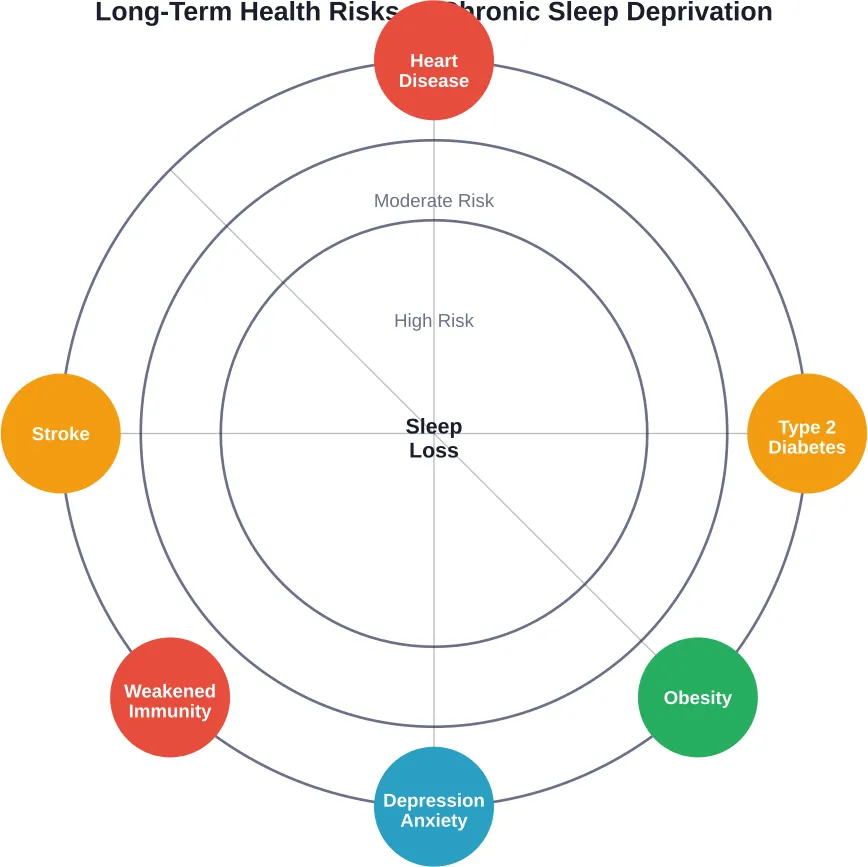
Long-Term Health Consequences of Chronic Sleep Loss
When sleep deprivation becomes chronic—lasting weeks, months, or years—the health consequences intensify dramatically.
Cardiovascular Disease and Hypertension
The NHLBI identifies strong links between insufficient sleep and cardiovascular problems. Chronic sleep deprivation increases the risk of heart disease, high blood pressure, and stroke.
During sleep, blood pressure naturally decreases, giving the cardiovascular system a necessary break. Without adequate rest, blood pressure remains elevated for longer periods, straining the heart and blood vessels.
Research also shows that sleep disorders contribute to inflammation and changes in metabolism that damage blood vessels over time.
Metabolic Disruption and Diabetes Risk
Sleep plays a critical role in how the body processes glucose. Insufficient sleep influences the way cells use this high-energy carbohydrate for fuel.
Studies have found that sleep restriction can lead to type 2 diabetes. One short-term sleep restriction study found that healthy subjects who had their sleep cut back showed significant changes in glucose metabolism.
Sleep deficiency also disrupts hormones that regulate appetite. Ghrelin (which signals hunger) increases, while leptin (which signals fullness) decreases. This hormonal imbalance drives increased food intake and weight gain.
Immune System Weakness
The immune system depends on sleep to function effectively. During rest, the body produces infection-fighting substances like cytokines, antibodies, and immune cells.
Without adequate sleep, the immune system produces fewer of these protective substances. This makes the body more susceptible to common illnesses like colds and flu, and potentially increases the risk of chronic conditions.
The connection is measurable: people who don’t get enough sleep are more likely to get sick after being exposed to viruses compared to well-rested individuals.
Mental Health Disorders
The relationship between sleep and mental health runs both ways. Sleep problems can contribute to mental health disorders, and mental health conditions often disrupt sleep.
Chronic sleep deprivation increases the risk of depression and anxiety disorders. The CDC’s research on sleep deprivation notes that mood disturbances become progressively worse with ongoing sleep deficiency.
For individuals already living with mental health conditions, inadequate sleep typically worsens symptoms and makes treatment less effective.
Obesity and Weight Gain
Multiple mechanisms link sleep loss to weight gain. Beyond the hormonal changes affecting appetite, sleep deprivation also reduces motivation for physical activity and impairs impulse control around food choices.
Tired people tend to choose high-calorie, high-carbohydrate foods for quick energy. They also have less mental bandwidth to resist cravings or stick to health goals.
The NHLBI identifies obesity as one of the chronic health conditions associated with ongoing sleep deficiency.
Who Is Most at Risk?
Certain populations face higher risks of sleep deprivation and its consequences.
Shift workers, particularly those on night shifts and rotating schedules, experience the most difficulties with sleep. The CDC reports that these workers frequently have shorter sleep duration and poorer sleep quality compared to day workers.
Healthcare workers represent a particularly vulnerable group. National data shows that over 50% of night shift healthcare workers sleep 6 or fewer hours daily—well below the recommended minimum.
Students also struggle significantly. CDC data indicates that about 57.8% of middle school students across 9 states didn’t get enough sleep on school nights. High school students face similar challenges.
Parents of young children, individuals with untreated sleep disorders, and people managing chronic health conditions also commonly experience sleep deficiency.
Can You Catch Up on Sleep?
The short answer? Sort of, but not really.
Sleeping longer on weekends can help reduce sleep debt slightly. A longer sleep period allows some recovery of cognitive function and reduces feelings of sleepiness.
But weekend catch-up sleep doesn’t fully reverse the health consequences of chronic sleep deprivation during the week. Metabolic changes, immune system impacts, and cardiovascular strain don’t reset completely with two days of better rest.
According to the NHLBI, naps may provide a short-term boost in alertness and performance. However, naps don’t replace the need for consistent, adequate nightly sleep.
The only real solution is prioritizing sufficient sleep consistently—not just occasionally.
Recognizing the Signs of Sleep Deprivation
Many people don’t realize they’re sleep deprived. The body adapts to functioning on insufficient rest, creating a new baseline that feels normal but isn’t optimal.
Common symptoms include:
- Excessive daytime sleepiness
- Difficulty concentrating or remembering information
- Increased irritability or mood swings
- Reduced motivation or energy
- Frequent illnesses or longer recovery times
- Increased appetite, particularly for sugary or high-fat foods
- Microsleeps—brief moments of unintentional sleep during waking activities
- Dependence on caffeine to function
If someone needs an alarm clock to wake up, feels groggy throughout the day, or immediately falls asleep when lying down, they’re likely not getting enough quality sleep.
How to Improve Sleep Quality
Addressing sleep deprivation requires both increasing sleep duration and improving sleep quality.
Sleep Hygiene Basics
Sleep hygiene refers to habits and environmental factors that promote consistent, quality sleep:
- Maintain a consistent sleep schedule, even on weekends
- Create a dark, quiet, cool bedroom environment
- Limit screen exposure 1-2 hours before bedtime
- Avoid caffeine in the afternoon and evening
- Exercise regularly, but not close to bedtime
- Manage stress through relaxation techniques
- Reserve the bed for sleep only, not work or entertainment
The CDC emphasizes that good sleep hygiene, particularly for adolescents when combined with later school start times, helps improve health and academic performance.
When to Seek Medical Help
Sometimes sleep problems stem from underlying medical conditions or sleep disorders. According to research from the National Institutes of Health, About 80 to 90 percent of adults with clinically significant sleep-disordered breathing remain undiagnosed.
Warning signs that warrant medical evaluation include:
- Chronic difficulty falling or staying asleep
- Loud snoring or gasping during sleep
- Persistent daytime sleepiness despite adequate time in bed
- Uncontrollable leg movements or uncomfortable sensations that disrupt sleep
- Sleep problems lasting more than a few weeks
Healthcare providers can diagnose conditions like sleep apnea, insomnia, restless leg syndrome, and other treatable sleep disorders.
| Sleep Disorder | Key Symptoms | Treatment Approaches |
|---|---|---|
| Sleep Apnea | Loud snoring, breathing pauses, daytime fatigue | CPAP therapy, lifestyle changes, positional therapy |
| Insomnia | Difficulty falling or staying asleep, daytime impairment | Cognitive behavioral therapy, sleep hygiene, medication |
| Restless Leg Syndrome | Uncomfortable leg sensations, urge to move legs | Iron supplementation, medications, lifestyle modifications |
| Narcolepsy | Excessive daytime sleepiness, sudden sleep attacks | Stimulant medications, scheduled naps, lifestyle adjustments |
The Bottom Line on Sleep Loss
Sleep isn’t a luxury or something to sacrifice for productivity. It’s a fundamental biological requirement that affects every system in the body.
The CDC and other health authorities consistently emphasize that sleep is as essential as food for life and health. Skimp on it, and the consequences compound—from immediate cognitive impairment to serious chronic diseases.
According to the American Academy of Sleep Medicine, adults need seven or more hours of sleep per night to avoid health risks. This recommendation is based on substantial evidence linking adequate sleep to better physical health, mental well-being, and quality of life.
Most adults specifically need 7 to 8 hours of good-quality sleep every 24 hours. Children and adolescents need even more to support growth and development.
The good news? Sleep problems are often treatable. Whether through improved sleep hygiene, lifestyle changes, or medical intervention for sleep disorders, most people can improve their sleep with the right approach.
Prioritizing sleep isn’t selfish—it’s essential self-care that enables better performance, healthier relationships, and longer, healthier life.
Frequently Asked Questions
After 24 hours without sleep, cognitive function declines significantly, with impairments in attention, reaction time, and decision-making. Mood becomes unstable, with increased irritability and anxiety. The immune system begins producing fewer infection-fighting substances. Accident risk increases dramatically as microsleeps—brief, uncontrollable moments of sleep—start occurring involuntarily.
Recovery time depends on the severity and duration of sleep debt. After a few nights of poor sleep, one or two nights of adequate rest can restore much of the cognitive function. However, chronic sleep deprivation lasting weeks or months may require consistent good sleep for several weeks to fully recover. Some metabolic and immune system changes may take even longer to normalize completely.
While most effects of sleep deprivation reverse with adequate rest, chronic severe sleep loss may contribute to permanent health conditions. Long-term sleep deficiency increases the risk of developing cardiovascular disease, diabetes, and other chronic conditions that don’t fully reverse once established. Additionally, chronic sleep loss during critical developmental periods in children and adolescents may have lasting impacts on growth and brain development.
Lack of sleep weakens the immune system by reducing production of protective cytokines and other infection-fighting substances. This makes the body more vulnerable to viruses and bacteria. Sleep deprivation also triggers inflammatory responses and stress hormone release, which can cause symptoms like headaches, body aches, and general malaise that resemble illness.
For most adults, 6 hours of sleep is insufficient. The American Academy of Sleep Medicine and CDC recommend 7 or more hours for optimal health. National data shows that over 50% of night shift healthcare workers sleeping 6 or fewer hours daily experience significant health and performance impacts. While some rare individuals may function adequately on 6 hours, they represent exceptions rather than the norm.
Both are severely detrimental, but research suggests that getting 2 hours of sleep is marginally better than none at all. Even brief sleep allows some degree of brain waste clearance and minimal physical restoration. However, 2 hours falls far short of what the body needs and will still result in severe cognitive impairment, mood disturbances, and safety risks. Neither option is sustainable or safe.
Yes, substantially. According to CDC research, sleep deprivation significantly impairs mood and can cause irritability, anxiety, and depression. The relationship is bidirectional—sleep problems contribute to mental health disorders, and mental health conditions disrupt sleep. Chronic sleep deficiency increases the risk of developing clinical anxiety and depression, and worsens symptoms in those already diagnosed with these conditions.
Take Action for Better Sleep
Understanding what happens when sleep gets neglected is the first step. Taking action is the next.
Start by honestly assessing current sleep habits. Track sleep duration and quality for a week. Note how rested or tired you feel each day. Identify patterns and obstacles preventing adequate rest.
Then implement one or two sleep hygiene improvements at a time. Set a consistent bedtime. Reduce evening screen time. Create a darker, cooler bedroom environment.
If sleep problems persist despite lifestyle changes, consult a healthcare provider. Undiagnosed sleep disorders affect millions and remain treatable when properly identified.
Sleep is an investment in health, productivity, and quality of life. The body can’t function optimally without it—no matter how much willpower or caffeine someone has.
Make sleep a priority. The benefits extend to every aspect of life.
