Quick Summary: Drinking alcohol while taking most antibiotics won’t reduce their effectiveness, but it can worsen side effects like nausea and stomach upset. However, certain antibiotics like metronidazole and tinidazole cause severe reactions with alcohol. It’s generally best to avoid alcohol during antibiotic treatment to support healing and minimize health risks.
That warning label on antibiotic bottles about avoiding alcohol isn’t just cautious advice. The interaction between antibiotics and alcohol ranges from mildly uncomfortable to genuinely dangerous, depending on which medication is prescribed.
According to the National Institute on Alcohol Abuse and Alcoholism, by one estimate, 40% of adults took a medication in the past year that could interact harmfully with alcohol. Understanding these interactions matters for anyone undergoing antibiotic treatment.
Does Alcohol Make Antibiotics Less Effective?
Here’s what surprises most people: alcohol doesn’t typically reduce antibiotic effectiveness. The common belief that drinking “cancels out” antibiotics is largely a myth.
According to research published in Antimicrobial Agents and Chemotherapy, alcohol did not impact the pharmacokinetics of ceftriaxone in rat pneumonia models. Similar findings exist for many commonly prescribed antibiotics.
But that doesn’t mean mixing them is harmless. The real concern lies elsewhere—in how alcohol and antibiotics together affect the body and amplify side effects.
The Real Risks: Side Effects and Safety Concerns
Both alcohol and antibiotics place demands on the liver and digestive system. When combined, they can intensify uncomfortable and potentially dangerous side effects.
Common Side Effects When Mixing Alcohol and Antibiotics
The most frequently reported issues include:
- Nausea and vomiting
- Stomach pain and cramping
- Headaches and dizziness
- Drowsiness and fatigue
- Rapid heart rate
- Flushing or skin redness
According to the CDC, drinking alcohol while using other drugs can be dangerous. The effects may be stronger and more deadly than using either one alone.
The NHS advises that it’s a good idea to avoid drinking alcohol when taking medicine or feeling unwell, as alcohol can reduce immune function when the body needs to fight infection.
How Alcohol Interferes With Healing
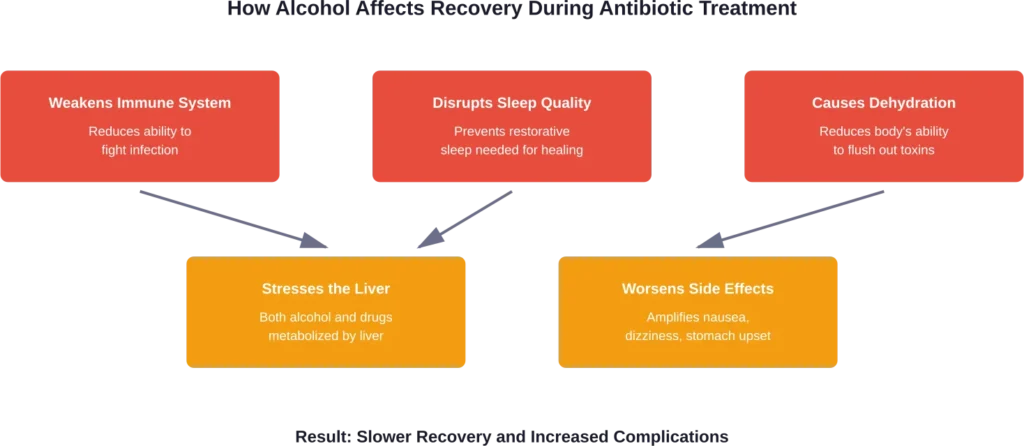
Beyond direct interactions, alcohol consumption during illness creates additional problems. It can disrupt sleep quality, dehydrate the body, and weaken immune response—all factors that slow recovery from bacterial infections.
Dangerous Combinations: Which Antibiotics React Severely With Alcohol
While most antibiotics simply increase side effect risk when mixed with alcohol, certain medications cause severe, potentially life-threatening reactions.
Metronidazole and Tinidazole: The Most Dangerous Interaction
These two antibiotics create what’s called a disulfiram-like reaction when combined with alcohol. The combination can trigger symptoms within 30 minutes to several hours after drinking.
Symptoms include:
- Severe nausea and vomiting
- Rapid heart rate (tachycardia)
- Sudden drop in blood pressure
- Intense facial flushing
- Severe headache
- Chest pain
According to research analyzing real-world drug interactions, metronidazole showed particularly strong associations with alcohol intolerance. In the broader drug-alcohol intolerance analysis, outcomes included hospitalization (16%), disability (6.4%), and death (1.7%) across reported cases.
Other High-Risk Antibiotics
Several other antibiotics warrant extreme caution when alcohol is involved:
| Antibiotic | Brand Names | Reaction Type |
|---|---|---|
| Metronidazole | Flagyl | Severe disulfiram-like reaction |
| Tinidazole | Tindamax | Severe disulfiram-like reaction |
| Cefoperazone | Cefobid | Strong alcohol intolerance |
| Sulfamethoxazole/Trimethoprim | Bactrim, Septra | Increased side effects, liver stress |
| Linezolid | Zyvox | Dangerous blood pressure changes |
| Isoniazid | Various | Increased liver toxicity risk |
Research published in Hospital Pharmacy identified cefoperazone, spiramycin, metronidazole, and dupilumab as having particularly strong associations with alcohol intolerance through Volcano plot analysis.
What About Common Antibiotics Like Amoxicillin?
Amoxicillin, one of the most frequently prescribed antibiotics, doesn’t have a severe interaction with alcohol. According to the NHS, amoxicillin works by killing bacteria that cause infection, and moderate alcohol consumption doesn’t interfere with this mechanism.
That said, alcohol can still worsen common antibiotic side effects like stomach upset and dizziness. The NHS notes it’s generally a good idea to avoid drinking alcohol when taking medicine or feeling unwell.

How Long After Taking Antibiotics Can You Drink Alcohol?
Timing matters. Even after finishing an antibiotic course, traces remain in the system.
For most antibiotics, waiting 48-72 hours after the final dose provides adequate clearance time. But certain medications require longer waiting periods.
For metronidazole, it is best to completely avoid alcohol while taking it and continue to avoid alcohol for a period after finishing, with healthcare providers often recommending waiting 48-72 hours or longer after the last dose.
The medication label and patient information leaflet provide specific guidance for each antibiotic. When in doubt, ask the prescribing doctor or pharmacist for precise timing recommendations.
Alcohol and Medication Interactions Beyond Antibiotics
The concerns about mixing alcohol with antibiotics extend to many other medications. According to the National Institute on Alcohol Abuse and Alcoholism, combining alcohol with certain medications—particularly those with sedative effects—can increase the risk of adverse events, including falls, driving accidents, and fatal overdoses.
The NIAAA notes that alcohol can alter the metabolism and pharmacological effects of many common medications, and conversely, many medications can alter the effects of alcohol. This bidirectional interaction creates compound risks.
Some medicines even contain alcohol themselves. According to the NIAAA’s Harmful Interactions guide, certain medicines contain up to 10 percent alcohol. Cough syrup and laxatives may have some of the highest alcohol concentrations.
What Healthcare Professionals Recommend
The consensus among medical professionals is clear: abstaining from alcohol during antibiotic treatment is the safest approach.
The CDC advises that to keep yourself safe and healthy, you should not drink alcohol when using other drugs. This guidance applies to prescription medications, over-the-counter drugs, and supplements.
Healthcare providers emphasize several key points:
- Always read medication labels carefully
- Ask the prescribing doctor about specific alcohol restrictions
- Consult pharmacists when picking up prescriptions
- Report any unusual symptoms immediately
- Complete the full antibiotic course regardless of feeling better
The NHS recommends that when taking antibiotics, patients should tell their doctor if they do not start feeling better after 3 to 5 days of treatment, as the antibiotic may not be working properly.
When to Seek Medical Help
Certain symptoms require immediate medical attention, especially after combining alcohol and antibiotics:
- Severe vomiting that won’t stop
- Rapid or irregular heartbeat
- Difficulty breathing
- Extreme dizziness or fainting
- Chest pain or pressure
- Severe skin reactions or rash
- Signs of liver problems (yellowing skin or eyes, dark urine)
These symptoms may indicate a serious drug interaction requiring emergency care.
Frequently Asked Questions
For most antibiotics, one beer likely won’t cause severe harm, but it can worsen side effects like nausea and dizziness. However, with metronidazole or tinidazole, even small amounts of alcohol can trigger dangerous reactions. The safest approach is avoiding alcohol entirely during treatment.
No, alcohol doesn’t typically prevent antibiotics from killing bacteria. Research shows most antibiotics maintain their effectiveness when alcohol is consumed. The primary concerns are increased side effects and slowed healing, not reduced antibiotic efficacy.
Most antibiotics are eliminated within 48-72 hours after the final dose, but this varies by medication. Metronidazole requires waiting 48-72 hours, while some antibiotics clear faster. Always check the specific medication’s guidance or ask a healthcare provider.
Combining metronidazole with alcohol can cause severe reactions including violent vomiting, rapid heartbeat, flushing, chest pain, and dangerous drops in blood pressure. Symptoms typically appear within 30 minutes to several hours. Seek medical attention immediately if this occurs.
While no antibiotic is officially “completely safe” with alcohol, some like amoxicillin and azithromycin don’t have severe interactions. That said, alcohol can still worsen common side effects and slow recovery. Medical professionals recommend avoiding alcohol during any antibiotic treatment.
For most antibiotics, 24 hours isn’t long enough. Healthcare providers typically recommend waiting 48-72 hours after the final dose before consuming alcohol. This allows the medication to clear your system and reduces interaction risk.
Alcohol doesn’t directly worsen bacterial infections, but it weakens immune function, disrupts sleep, and causes dehydration—all factors that can slow recovery and make it harder for the body to fight infection effectively.
Conclusion: The Bottom Line on Antibiotics and Alcohol
The relationship between alcohol and antibiotics is nuanced. While moderate drinking won’t render most antibiotics ineffective, it creates unnecessary risks through amplified side effects, liver stress, and compromised healing.
Certain antibiotics like metronidazole and tinidazole pose serious dangers when combined with any amount of alcohol. Even with lower-risk antibiotics, alcohol consumption during illness hinders recovery.
The smartest approach? Skip the drinks until treatment is complete and the body has fully cleared the medication—typically 48-72 hours after the final dose. When health is on the line, temporary abstinence is a small price for safe, effective recovery.
Always consult healthcare providers with questions about specific medications and follow the guidance on prescription labels. When in doubt, choosing caution over convenience protects long-term health.
