Quick Summary: Drinking too much water can lead to water intoxication (hyponatremia), a dangerous condition where excess fluid dilutes sodium levels in the blood. Symptoms include nausea, headache, confusion, and in severe cases, seizures or brain swelling. Most healthy adults need about 8-10 cups daily, but individual needs vary based on activity level and health conditions.
Water keeps the body alive. Every cell depends on it. But here’s something most people don’t realize: drinking too much water can actually harm or even kill you.
Water intoxication—also called water toxicity or dilutional hyponatremia—happens when someone consumes so much water that their blood sodium levels drop to dangerous levels. The body thrives on balance, and flooding the system with excessive water throws off that delicate equilibrium.
While rare, this condition has led to fatal outcomes in endurance athletes, psychiatric patients with compulsive drinking behaviors, and even individuals participating in water-drinking contests. Understanding the risks and recognizing the warning signs can prevent serious health consequences.
What Is Water Intoxication?
Water intoxication occurs when excess water intake dilutes the concentration of sodium in the bloodstream. Sodium regulates fluid balance between cells and surrounding tissues. When sodium levels drop too low—a condition called hyponatremia—water moves into cells to balance the concentration gradient.
This cellular swelling becomes particularly dangerous in the brain, where the rigid skull leaves no room for expansion. Brain swelling can lead to increased intracranial pressure, causing a cascade of neurological symptoms that can progress from mild confusion to seizures, coma, and death.
According to medical research published by the National Center for Biotechnology Information, water intoxication is a life-threatening disorder accompanied by brain function impairment due to severe dilutional hyponatremia. One documented case involved an individual who drank 6 liters of water and developed prolonged hyponatremia requiring intensive medical intervention.
How the Kidneys Process Water
Healthy kidneys can process water, but only about 0.8-1.0 liters per hour. Drinking water faster than the kidneys can eliminate it creates the conditions for water intoxication.
The kidneys filter blood and remove excess fluid through urine production. When water intake overwhelms this filtering capacity, fluid accumulates in the bloodstream, diluting electrolytes and disrupting normal metabolic processes.
Symptoms of Drinking Too Much Water
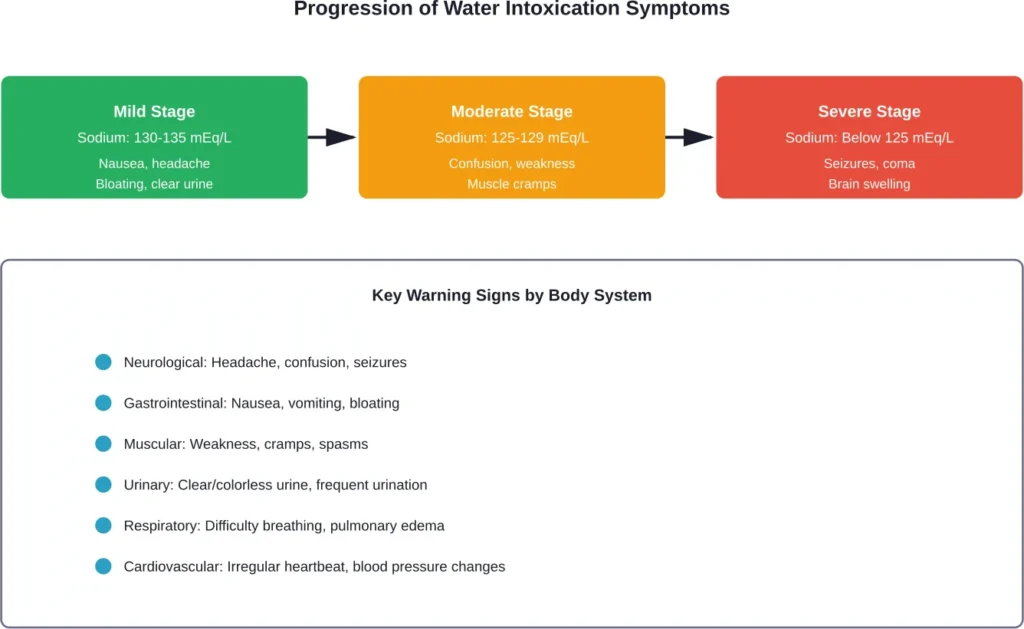
Early recognition of overhydration symptoms can prevent progression to life-threatening complications. Symptoms typically develop in stages as sodium levels decline.
Early Warning Signs
The initial symptoms of water intoxication often resemble other common conditions, making early detection challenging:
- Nausea and vomiting
- Headache that worsens with physical activity
- Bloating and abdominal discomfort
- Clear or colorless urine (healthy urine should be pale yellow)
- Frequent urination beyond normal patterns
These early signs indicate the body is struggling to maintain electrolyte balance. Stopping water intake at this stage typically allows the body to self-correct without medical intervention.
Severe Symptoms Requiring Immediate Medical Attention
As hyponatremia worsens, neurological symptoms emerge:
- Confusion and disorientation
- Severe muscle weakness or cramps
- Seizures or convulsions
- Altered mental status or agitation
- Loss of consciousness
- Difficulty breathing or pulmonary edema
Research from the National Center for Biotechnology Information documents cases where severe hyponatremia developed rapidly in hospitalized patients engaging in surreptitious water drinking. In one case, symptoms only resolved after bathroom water access was restricted.
Who Is at Risk for Water Intoxication?
While anyone can develop water intoxication if they drink enough water rapidly, certain groups face elevated risk.
Endurance Athletes
Marathon runners, triathletes, and ultra-distance competitors commonly develop exercise-associated hyponatremia. According to research on endurance athletes, individuals participating in ultra-distance events face particular risk, with cases reported in competitors who gained weight during races—indicating excessive water retention.
Documented cases involve athletes who gained weight during ultra-distance events and developed symptomatic hyponatremia requiring medical intervention. Athletes with water intoxication required elimination of excess fluid during recovery.
Athletes often drink aggressively to prevent dehydration but fail to replace sodium lost through sweat. Sports drinks containing electrolytes provide some protection, but research indicates that electrolyte-containing beverages alone are not likely to prevent water intoxication if consumption remains excessive.
Individuals with Psychiatric Conditions
Psychogenic polydipsia—compulsive water drinking—occurs in patients with schizophrenia, anorexia nervosa, and other psychiatric disorders. Medical literature documents fatal cases of water intoxication in psychiatric patients who consumed excessive quantities of water as part of their illness.
One published case detailed a patient with anorexia nervosa and body dysmorphic disorder who required treatment with olanzapine and fluoxetine to manage both the psychiatric disturbances and prevent recurrent hyponatremia episodes.
Infants and Young Children
Infants have immature kidney function and lower body mass, making them particularly vulnerable to water intoxication. Cases have been reported where excessive water intake was used as a form of abuse.
Medical research documented a pediatric case where a child developed severe hyponatremia due to excessive water intake. Infants should receive breast milk or formula, not plain water, during infancy.
People Taking Certain Medications
Some medications impair the kidneys’ ability to excrete water, including:
- Selective serotonin reuptake inhibitors (SSRIs)
- Nonsteroidal anti-inflammatory drugs (NSAIDs)
- Opiate pain medications
- Certain diabetes medications
These drugs can cause syndrome of inappropriate antidiuretic hormone secretion (SIADH), where the body retains excessive water. One medical case report described prolonged hyponatremia caused by excessive water drinking combined with secondary SIADH.
How Much Water Is Too Much?
The kidneys of a healthy adult can process roughly 0.8-1.0 liters of water per hour. According to guidance from the University of Illinois Division of Research Safety, individuals should drink no more than 48 fluid ounces (approximately 1.4 liters) per hour during strenuous activity.
The same source recommends drinking 1 cup of water every 15-20 minutes during activity, totaling about 24-32 fluid ounces per hour. Exceeding these rates increases the risk of water intoxication.
Daily Water Needs Vary
The classic advice to drink eight glasses of water daily originated from military research on soldiers carrying heavy packs in hot conditions. Harvard Health Publishing notes this estimate included water from all sources—including food—and applied specifically to active soldiers under stress.
For most people, thirst serves as an adequate guide. But thirst isn’t always reliable during intense exercise or in extreme heat, which is why monitoring urine color provides a better indicator.
| Urine Color | Hydration Status | Action Needed |
|---|---|---|
| Pale yellow (lemonade color) | Well hydrated | Maintain current intake |
| Dark yellow or amber | Mild dehydration | Increase fluid intake gradually |
| Clear or colorless | Possible overhydration | Reduce water intake |
| Brown or tea-colored | Severe dehydration or medical issue | Seek medical attention |
Treatment for Water Intoxication
Treatment depends on severity. Mild cases often resolve simply by stopping water intake and allowing the kidneys to restore balance naturally.
Medical Interventions for Severe Cases
Severe hyponatremia requires immediate medical care. Treatment typically includes:
- Fluid restriction to allow sodium levels to normalize
- Intravenous administration of hypertonic saline solution
- Diuretics to promote water excretion
- Continuous monitoring of electrolyte levels
- Treatment of underlying causes (SIADH, psychiatric conditions)
Rapid correction of sodium levels carries its own risks, including osmotic demyelination syndrome, a condition that damages the protective covering of nerve cells. Medical providers must carefully calculate the rate of sodium replacement.
Research on severe cases indicates that some patients required prolonged hospitalization. In one documented case, symptoms only improved after removing access to water sources, highlighting the importance of identifying and addressing compulsive drinking behaviors.
How to Prevent Overhydration
Prevention is straightforward once the risks are understood.
Listen to Your Body
Drink when thirsty. Stop when satisfied. This simple approach works for most people in normal conditions.
But recognize that certain situations—intense exercise, extreme heat, illness—alter fluid needs. In these cases, monitoring urine color and body weight changes provides better guidance than thirst alone.
Adjust for Activity Level
According to the University of Illinois Division of Research Safety, individuals should start hydrating at least a day before strenuous activity and replenish fluids at regular intervals during activity—but never exceed 48 fluid ounces per hour.
For exercise lasting less than 75 minutes at moderate intensity, water typically suffices. Longer or more intense activities benefit from beverages containing electrolytes.
Replace Electrolytes During Extended Exercise
Sweat contains sodium, potassium, and other electrolytes. During prolonged exercise, especially in heat, replacing these minerals prevents dangerous imbalances.
Sports drinks, coconut water, or electrolyte tablets help maintain proper sodium levels. But moderation matters here too—the American Heart Association notes that electrolyte drinks should be consumed appropriately, not excessively.

Monitor Weight During Long Events
Weight gain during exercise indicates water retention, not proper hydration. Athletes should weigh themselves before and after long training sessions or competitions.
Any weight gain suggests excessive fluid intake. Weight loss of 2-3% of body weight indicates appropriate fluid balance for most endurance activities.
Common Myths About Hydration
Several persistent myths encourage overconsumption of water.
Myth: Everyone Needs Eight Glasses Daily
The eight-glasses rule oversimplifies hydration needs. Individual requirements depend on body size, activity level, climate, diet, and health status.
Someone who eats water-rich foods (fruits, vegetables, soups) needs less drinking water than someone consuming a dry, processed diet. A 120-pound sedentary office worker needs far less water than a 200-pound construction worker in summer heat.
Myth: Clear Urine Means Perfect Hydration
Clear urine actually signals overhydration. Pale yellow urine indicates optimal hydration status. Persistently clear urine suggests excessive water intake.
Myth: More Water Flushes Out Toxins Better
The kidneys and liver handle toxin removal efficiently at normal hydration levels. Drinking excessive water doesn’t enhance this process and can actually impair kidney function by forcing these organs to work harder removing excess fluid.
When to Seek Medical Attention
Seek immediate medical care if experiencing:
- Severe confusion or disorientation
- Seizures or convulsions
- Loss of consciousness
- Persistent vomiting that prevents keeping fluids down
- Extreme weakness or inability to stand
- Irregular heartbeat or chest pain
These symptoms indicate potentially life-threatening hyponatremia requiring emergency intervention.
For milder symptoms—nausea, headache, bloating—that don’t improve after stopping water intake for several hours, consult a healthcare provider. Blood tests can measure sodium levels and guide appropriate treatment.
Frequently Asked Questions
Yes, though deaths from water intoxication are rare. Severe hyponatremia causes brain swelling that can lead to seizures, coma, respiratory failure, and death. Medical literature documents fatal cases in psychiatric patients with psychogenic polydipsia and endurance athletes who consumed excessive water during competitions. Prompt medical treatment is critical when severe symptoms develop.
This varies by individual factors, but generally drinking more than 0.8-1.0 liters per hour overwhelms kidney processing capacity. Research documents cases developing from as little as 6 liters consumed over several hours. The rate of consumption matters more than total volume—drinking several liters rapidly poses greater risk than the same amount spread throughout a day. Healthy kidneys can handle up to about 1 liter per hour.
Early warning signs include nausea, headache, bloating, and clear or colorless urine. These symptoms indicate the body is struggling to maintain electrolyte balance. Other initial signs include frequent urination beyond normal patterns and a feeling of fullness or discomfort in the stomach. Stopping water intake when these symptoms appear usually allows the body to restore balance without medical intervention.
Sports drinks containing electrolytes provide some protection by replacing sodium lost through sweat, but research indicates they’re not likely to prevent water intoxication if consumption remains excessive. The key is moderating total fluid intake to no more than 48 fluid ounces per hour during activity, regardless of beverage type. Electrolyte drinks work best for activities lasting more than 75 minutes or high-intensity exercise where significant sweat loss occurs.
Mild cases typically resolve within a few hours once water intake stops and the kidneys restore electrolyte balance. Severe cases requiring hospitalization may take several days to weeks for complete recovery, depending on how low sodium levels dropped. Medical research documents cases with prolonged hyponatremia requiring extended treatment. The recovery rate must be carefully controlled because correcting sodium levels too rapidly can cause additional neurological damage.
Yes, infants and young children are more vulnerable to water intoxication due to smaller body mass and immature kidney function. Infants should receive only breast milk or formula, not plain water. Young children need smaller fluid volumes adjusted for their body weight. Parents should never force children to drink water and should monitor for signs of overhydration, which can develop more rapidly in small children than adults.
The kidneys and liver efficiently remove metabolic waste products at normal hydration levels. Drinking adequate water supports these organs, but excessive water doesn’t enhance detoxification. In fact, overhydration can stress the kidneys by forcing them to process and eliminate unnecessary fluid. Proper hydration means drinking enough to maintain pale yellow urine—not clear, which indicates excess.
Conclusion
Water sustains life, but like anything essential, balance matters. Water intoxication remains rare, but the consequences can be severe or fatal when it occurs.
The body sends clear signals about hydration needs. Thirst, urine color, and how the body feels during activity provide reliable guidance for most people. Drinking when thirsty and stopping when satisfied works well for everyday situations.
During intense exercise, extreme heat, or other challenging conditions, monitoring becomes more important. Keep fluid intake below 48 ounces per hour, replace electrolytes during prolonged activity, and watch for early warning signs like nausea or headache.
Clear or colorless urine isn’t a badge of health—it’s a warning sign to reduce intake. Pale yellow indicates optimal hydration. Stop drinking if experiencing bloating, headache, or discomfort.
Understanding these principles protects against a preventable but dangerous condition. Stay informed, listen to the body’s signals, and remember that more isn’t always better when it comes to water consumption.
