Quick Summary: While IUDs are over 99% effective, pregnancy can still occur in rare cases—fewer than 1 in 100 users per year. If pregnancy happens with an IUD, there’s an increased risk of ectopic pregnancy, miscarriage, and preterm birth. Immediate medical evaluation is essential to determine if the IUD can be safely removed and to monitor for complications throughout the pregnancy.
Intrauterine devices are among the most reliable forms of birth control available. With typical use, fewer than 1 pregnancy occurs per 100 women in the first year, according to the World Health Organization. Yet despite this impressive track record, IUD failure does happen.
When pregnancy occurs with an IUD in place, it creates a unique medical situation that requires immediate attention. The presence of the device can affect where the pregnancy implants and increases certain risks that wouldn’t exist otherwise.
Here’s what actually happens when you get pregnant with an IUD—and what you need to know to protect your health.
How Do IUDs Work and Why Do They Sometimes Fail?
An intrauterine device is a small, T-shaped contraceptive placed inside the uterus to prevent pregnancy. Two main types exist: copper-bearing IUDs and levonorgestrel-releasing hormonal IUDs.
Copper IUDs work by creating an inflammatory response that’s toxic to sperm and eggs. The copper ions prevent fertilization and make the uterine lining inhospitable for implantation. These devices can prevent pregnancy for 10-12 years depending on the model.
Hormonal IUDs release levonorgestrel, which thickens cervical mucus to block sperm, thins the uterine lining, and sometimes prevents ovulation. According to the American College of Obstetricians and Gynecologists, five IUDs are currently marketed in the United States: one copper IUD and four levonorgestrel-releasing devices with varying hormone doses.
Common Reasons for IUD Failure
While rare, IUDs can fail for several reasons. Expulsion occurs when the device partially or completely comes out of the uterus—this happens in roughly 2-10% of users within the first year.
The device can also shift position over time. If an IUD moves into the cervix or becomes embedded in the uterine wall, its effectiveness decreases. Sometimes the strings become difficult to locate, which doesn’t always mean the IUD has moved but warrants investigation.
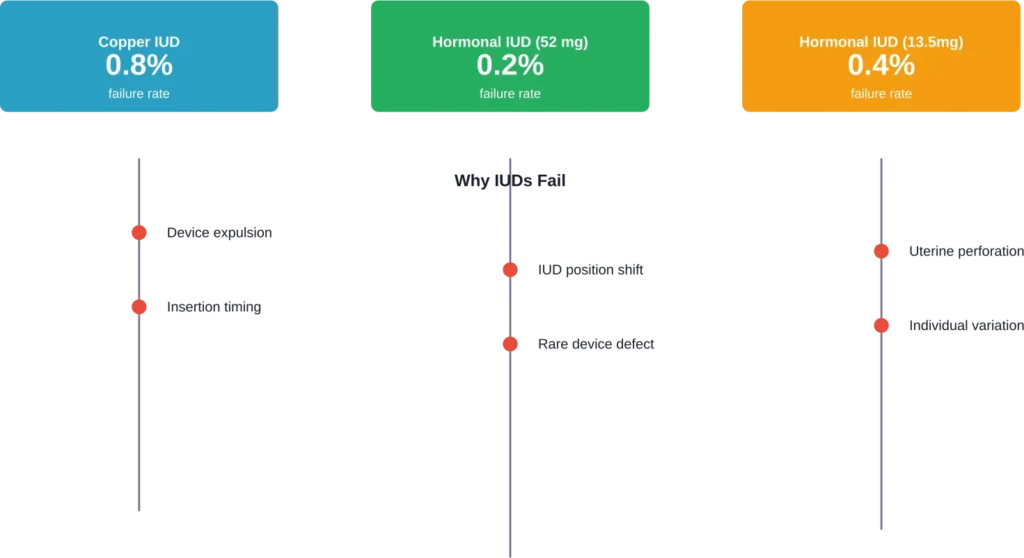
Research published in medical journals shows that pregnancy can occur even with a properly positioned IUD. The failure rate varies slightly between types, with hormonal IUDs generally showing higher effectiveness than copper devices.
Types of Pregnancy That Can Occur With an IUD
Not all IUD pregnancies are the same. Where the embryo implants determines the risks involved and the treatment approach.
Intrauterine Pregnancy
This is when the embryo implants normally inside the uterus despite the IUD being present. It’s the most common type of IUD pregnancy, though still rare overall.
The IUD sits alongside the developing pregnancy. Depending on its position, the device may be removable in early pregnancy or may need to remain in place if the strings aren’t accessible.
Ectopic Pregnancy
Here’s the concerning part: when pregnancy does occur with an IUD, there’s a higher-than-normal chance it will be ectopic. This means the embryo implants outside the uterus, most commonly in the fallopian tube.
According to CDC surveillance data, ectopic pregnancies represented 1.5% of total pregnancies in the general population. But when pregnancy occurs with an IUD in place, the proportion of ectopic cases increases significantly.
Ectopic pregnancy is a medical emergency. The pregnancy cannot survive, and without treatment, it can cause life-threatening internal bleeding. Research shows that while IUDs prevent both intrauterine and ectopic pregnancies overall, they’re more effective at preventing intrauterine pregnancies—so if contraception fails, the relative risk of ectopic pregnancy is higher.
| Pregnancy Type | Implantation Location | Can Continue? | Urgency Level |
|---|---|---|---|
| Intrauterine | Inside uterus | Possibly | Urgent evaluation needed |
| Ectopic (tubal) | Fallopian tube | No | Medical emergency |
| Ectopic (other) | Cervix, ovary, abdomen | No | Medical emergency |
Signs and Symptoms of Pregnancy With an IUD
Recognizing pregnancy symptoms early makes a huge difference in outcomes. The signs are similar to any pregnancy, but some warrant immediate attention when you have an IUD.
Common early pregnancy symptoms include a missed period, breast tenderness, nausea, and fatigue. Many women also experience light spotting or cramping during implantation.
But watch for red flags. Severe one-sided pelvic pain, especially with vaginal bleeding, could indicate ectopic pregnancy. Sharp, stabbing abdominal pain or shoulder pain can signal internal bleeding from a ruptured ectopic pregnancy.
Dizziness, lightheadedness, or fainting combined with abdominal pain requires emergency evaluation. According to medical case reports, ruptured ectopic pregnancy remains a leading cause of first-trimester maternal mortality.
Some women feel their IUD strings differently or notice the device has shifted. Others can’t locate the strings at all. Any of these changes should prompt a medical visit.
Immediate Risks of IUD Pregnancy
Pregnancy with an IUD in place carries specific complications that don’t affect other pregnancies to the same degree.
Miscarriage
The risk of miscarriage increases substantially when an IUD remains in place. The device can interfere with the pregnancy’s attachment to the uterine wall or trigger contractions.
Research evaluating pregnancy outcomes shows that removing an accessible IUD typically reduces miscarriage risk, though some risk elevation persists compared to pregnancies without prior IUD use.
Preterm Birth
Studies published in medical journals demonstrate significantly higher rates of preterm delivery in IUD pregnancies. One retrospective study of copper IUD pregnancies found preterm birth rates of 23.0% compared to 6.8% in controls without IUDs. The same study reported preterm premature rupture of membranes in 37.8% of IUD pregnancies versus much lower rates in the general population.
Premature rupture of membranes also occurs more frequently in IUD pregnancies.
| Complication | IUD Removed Early | IUD Retained | No IUD |
|---|---|---|---|
| Preterm delivery | 14.3% | 14.1% | 6.8% |
| Miscarriage | Reduced risk | Higher risk | Baseline risk |
| Infection | Reduced risk | Elevated risk | Baseline risk |
Infection
The IUD provides a pathway for bacteria to enter the uterus during pregnancy. Infections can affect the pregnancy, the uterus, and surrounding organs.
Bacterial infections during pregnancy increase the risk of preterm labor, premature rupture of membranes, and postpartum complications.
What Doctors Do When You Get Pregnant With an IUD
Medical management depends on several factors: where the pregnancy is located, whether the IUD strings are visible, and how far along the pregnancy is.
Initial Evaluation
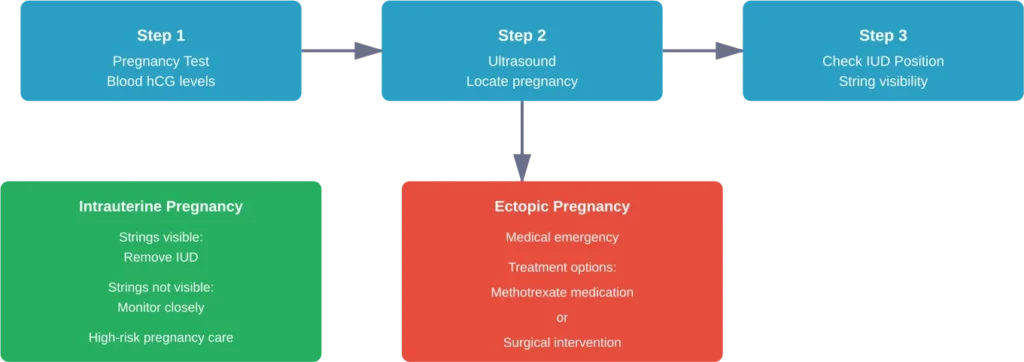
First, your doctor confirms the pregnancy with blood tests measuring hCG (human chorionic gonadotropin). Rising hCG levels confirm pregnancy, while the rate of increase helps distinguish between normal intrauterine pregnancy and ectopic pregnancy.
An ultrasound examination shows where the pregnancy has implanted and where the IUD is positioned. Early ultrasounds may not definitively locate a very early pregnancy, requiring follow-up scans.
IUD Removal Decision
If the IUD strings are visible through the cervix, removal is generally recommended. According to the American College of Obstetricians and Gynecologists, removing an accessible IUD typically improves pregnancy outcomes by reducing miscarriage and infection risks.
The removal itself carries a small risk of causing miscarriage, but leaving the device in place poses greater risks overall. Removal is usually performed early in the first trimester.
When strings aren’t visible and the IUD sits high in the uterus beyond reach, removal becomes more complicated. Attempting to retrieve an inaccessible IUD can cause more harm than leaving it in place. In these cases, doctors monitor the pregnancy closely for complications.
Ectopic Pregnancy Treatment
Ectopic pregnancies require prompt intervention since they cannot result in a viable birth and pose serious health risks. Treatment options include medication (methotrexate) for early ectopic pregnancies or surgery for more advanced cases or ruptured ectopic pregnancy.
Continuing Pregnancy With an IUD
Some women choose to continue their pregnancy even with an IUD that cannot be removed. This requires specialized prenatal care and close monitoring.
Regular ultrasounds track the pregnancy’s development and the IUD’s position. Healthcare providers watch for signs of preterm labor, infection, or other complications that occur more frequently in these pregnancies.
The IUD typically doesn’t cause birth defects. Research shows no significant difference in congenital malformation rates between pregnancies with copper IUDs in situ and those without IUDs.
However, the elevated risks of preterm birth and membrane rupture persist throughout pregnancy. Women carrying pregnancies with retained IUDs should be aware of preterm labor symptoms and maintain close communication with their healthcare team.
Long-Term Implications and Future Fertility
Having a pregnancy with an IUD doesn’t typically affect future fertility once the situation is resolved. After miscarriage, ectopic pregnancy treatment, or delivery, most women can conceive again normally.
If you want to continue using an IUD after pregnancy, you can have a new device placed postpartum. According to CDC guidelines, IUD insertion is safe immediately after delivery or Cesarean section, though expulsion rates are higher with immediate postpartum placement compared to placement at 4-6 weeks postpartum.
For those who’ve experienced ectopic pregnancy, there’s a slightly increased risk of another ectopic pregnancy in future conceptions, regardless of contraceptive method. This elevated risk relates to the underlying factors that caused the first ectopic pregnancy rather than the IUD itself.
Frequently Asked Questions
The likelihood is very low. With typical use, fewer than 1 pregnancy occurs per 100 women in the first year. Hormonal IUDs with 52 mg levonorgestrel show failure rates around 0.2%, while copper IUDs have failure rates near 0.8%. Despite these low rates, pregnancies can and do occur.
Yes, pregnancy tests work normally with an IUD. The device doesn’t interfere with pregnancy test accuracy. If you suspect pregnancy, take a home test or visit your doctor for blood testing. The IUD presence doesn’t affect hCG hormone production that pregnancy tests detect.
No, IUDs don’t cause false negative results. However, testing too early before hCG levels rise sufficiently can produce false negatives regardless of whether you have an IUD. Wait until your expected period or at least 10-14 days after potential conception for accurate results.
While IUDs reduce the overall risk of ectopic pregnancy compared to using no contraception, if pregnancy does occur with an IUD, the proportion that are ectopic is higher than in the general population. The increased relative risk occurs because IUDs are more effective at preventing intrauterine pregnancy than ectopic pregnancy.
Absolutely. If you’re planning pregnancy, have your IUD removed before trying to conceive. Fertility typically returns immediately after removal—you can become pregnant in the first cycle. Intentionally conceiving with an IUD in place would expose a pregnancy to unnecessary risks.
Sometimes, but not always. You might notice longer or shorter IUD strings, or you might feel the hard plastic of the IUD itself through your cervix. Some women experience increased cramping, unusual bleeding, or spotting when an IUD shifts. However, many position changes occur without symptoms, which is why regular checkups matter.
If miscarriage occurs with an IUD in place, your healthcare provider will typically remove the IUD during or after the miscarriage. Management depends on whether the miscarriage is complete or requires medical intervention. The IUD is usually removed to reduce infection risk and allow the uterus to return to normal.
When to Seek Immediate Medical Care
Certain symptoms require emergency evaluation rather than waiting for a scheduled appointment. Severe one-sided pelvic or abdominal pain, especially with vaginal bleeding, needs immediate attention.
Shoulder pain combined with abdominal pain can indicate internal bleeding from a ruptured ectopic pregnancy. Dizziness, fainting, or feeling lightheaded with abdominal pain also suggests internal bleeding.
Heavy vaginal bleeding that soaks through a pad in an hour or less requires urgent care. Fever above 100.4°F with abdominal pain could indicate infection.
If you can’t reach your regular doctor and experience these symptoms, go to an emergency department. According to medical case reports, ruptured ectopic pregnancy requires immediate surgical intervention to prevent life-threatening blood loss.
Bottom Line: What You Should Do
Getting pregnant with an IUD is uncommon but possible. The key is recognizing it early and getting proper medical evaluation.
If you suspect pregnancy with an IUD, take a pregnancy test and contact your healthcare provider immediately—don’t wait for your next scheduled appointment. Early detection allows doctors to determine whether the pregnancy is intrauterine or ectopic and whether the IUD can be safely removed.
The outcome depends significantly on where the pregnancy implanted and how quickly appropriate care begins. Intrauterine pregnancies can sometimes continue successfully, especially if the IUD is removed early. Ectopic pregnancies require prompt treatment to protect your health and future fertility.
Most importantly, trust your body. If something feels wrong or you experience symptoms that concern you, seek medical attention. IUD pregnancies carry specific risks that benefit from early intervention and specialized prenatal care.