Quick Summary: Taking too much acetaminophen (Tylenol) can cause severe liver damage and even death. The FDA warns that over 600 medications contain acetaminophen, making accidental overdoses common. Symptoms develop in stages, starting with nausea and progressing to liver failure if untreated. Adults should never exceed 4,000 mg daily, and those who consume alcohol regularly face even greater risks.
Acetaminophen poisoning doesn’t always look like what people expect.
Someone takes cold medicine every few hours. Later that day, they grab Tylenol for a headache. By evening, they’ve unknowingly consumed a dangerous amount of the same drug—acetaminophen—without realizing many medications contain it.
According to the FDA, more than 600 medications contain acetaminophen, both prescription and over-the-counter. Each year in the U.S., people catch 1 billion colds and as many as 12% get the flu. Seven in ten people use nonprescription medications during these illnesses, often combining multiple products without checking ingredients.
Here’s the thing though—acetaminophen is one of the most commonly used drugs worldwide, with REMOVE – this specific statistic does not appear in source material. But it’s also the leading cause of acute liver failure in the United States, according to the National Institutes of Health.
Why Acetaminophen Overdose Happens So Easily
The danger isn’t just from taking an entire bottle at once.
Acetaminophen appears in cold medicines, flu remedies, sleep aids, allergy medications, and combination pain relievers. Product labels use different names: APAP, Acetaminoph, Acetaminop, Acetamin, or Acetam. Outside the United States, it’s called paracetamol.
Common products containing acetaminophen include Tylenol-PM, Nyquil, Vicodin, and hundreds more. When someone takes multiple medications simultaneously—say, a cold medicine, a pain reliever, and a sleep aid—they can easily exceed safe limits without intending to.
According to NIH research, a striking 50% of acetaminophen toxicity cases result from unintentional overdoses. People simply don’t realize how much they’re taking.
What Is a Dangerous Dose?
The maximum daily limit for healthy adults weighing at least 150 pounds is 4,000 mg per day, according to the FDA. But that’s not as much as it sounds.
Regular-strength Tylenol contains 325 mg per tablet. Extra-strength contains 500 mg. Taking two extra-strength tablets every six hours puts someone at 4,000 mg—right at the maximum.
| Tablet Strength | Pills Per Dose | Frequency | Daily Total |
|---|---|---|---|
| 325 mg | 1-2 tablets | Every 4-6 hours | Up to 3,900 mg |
| 500 mg | 1-2 tablets | Every 6 hours | Up to 4,000 mg |
| 650 mg ER | 1 tablet | Every 8 hours | 1,950 mg |
Research published on PubMed shows that acute toxicity typically results with ingestion of a total dose ≥ 150 mg/kg (approximately 7.5 to 10 g in adults) have caused liver damage in adults. Larger doses can be fatal.
Now, this is where it gets concerning. For most adults, serious hepatotoxicity risk begins around 12 grams in a single overdose. But individual susceptibility varies significantly.
The Four Stages of Acetaminophen Poisoning
According to the Merck Manuals, acetaminophen overdose symptoms develop in four distinct stages:
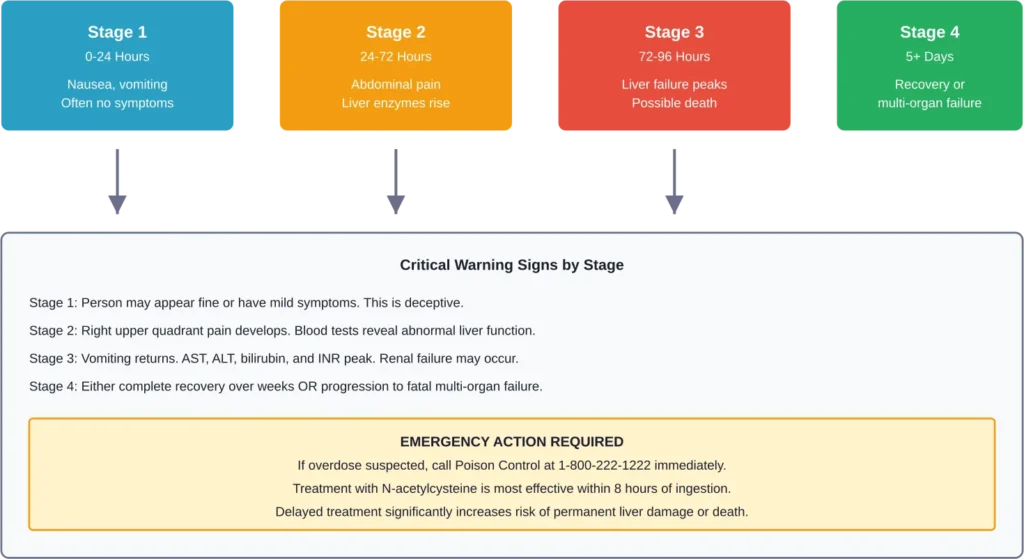
Many people have no symptoms in stage 1, which makes acetaminophen poisoning particularly dangerous. By the time obvious symptoms appear, liver damage may already be occurring.
How Acetaminophen Damages the Liver
The liver metabolizes acetaminophen through several pathways. At therapeutic doses, the process is harmless.
But when someone takes too much, the normal pathways become overwhelmed. The liver then uses an alternative pathway that produces a toxic metabolite called NAPQI (N-acetyl-p-benzoquinone imine).
Normally, glutathione—an antioxidant in the liver—neutralizes NAPQI. During overdose, glutathione stores deplete. NAPQI accumulates and directly damages liver cells, causing hepatotoxicity.
According to NIH research, acetaminophen toxicity is responsible for the majority of severe acute liver injury cases and acute liver failure cases where data is available. It’s involved in about 6% of all poisonings but causes disproportionate severe outcomes.
Who Faces Higher Risk
Not everyone has the same risk threshold.
The FDA warns that severe liver damage may occur if someone has three or more alcoholic drinks per day while using acetaminophen. Chronic alcohol consumption depletes glutathione stores and may increase NAPQI formation through enzyme changes.
Other high-risk groups include:
- People with pre-existing liver disease
- Those taking medications that affect liver enzymes
- Individuals with malnutrition or eating disorders (reduced glutathione)
- People taking multiple acetaminophen-containing products simultaneously
Chronic therapy with acetaminophen in doses of 4 grams daily has been found to lead to transient elevations in serum aminotransferase levels in a proportion of cases. Those with risk factors may experience problems at lower doses.
Treatment: Time Is Critical
The antidote for acetaminophen poisoning is N-acetylcysteine (NAC).
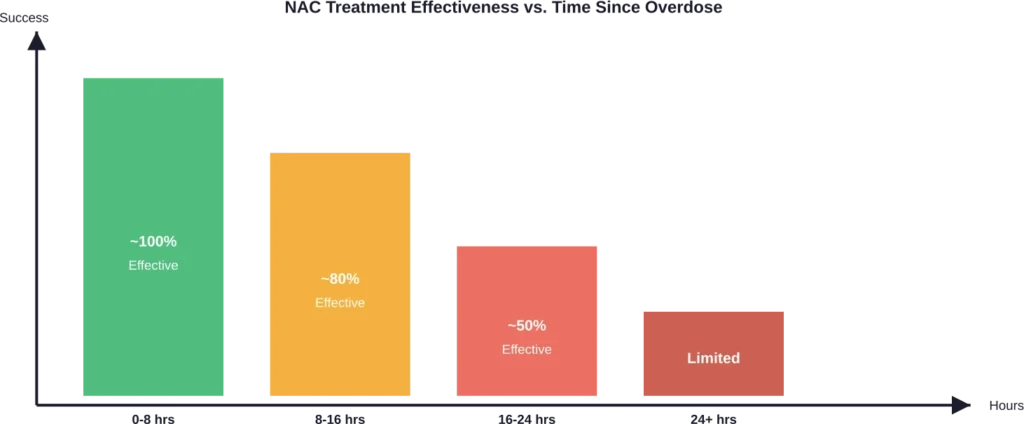
NAC works by replenishing glutathione stores, allowing the liver to neutralize toxic NAPQI. According to medical research, treatment effectiveness depends heavily on timing.
When administered within 8 hours of overdose, NAC prevents nearly all serious liver injury. After 24 hours, effectiveness drops significantly, though treatment should still be attempted.
Emergency departments use a nomogram—a graph plotting serum acetaminophen concentration against time since ingestion—to determine who needs treatment. Patients whose levels fall above the treatment line require NAC.
Real talk: don’t wait to see if symptoms develop. By the time stage 2 or 3 symptoms appear, liver damage is already occurring.
Prevention: Read Every Label
The FDA’s Division of Drug Information emphasizes checking every medication label before use.
Look for these ingredient names:
- Acetaminophen
- APAP
- Paracetamol
- Any abbreviation: Acetaminoph, Acetaminop, Acetamin, Acetam
Never combine multiple products without confirming they don’t contain the same active ingredient. When treating cold or flu symptoms, pick one multi-symptom medication rather than stacking individual remedies.
For those with liver disease, the FDA recommends consulting a healthcare professional before using any acetaminophen product—even at normal doses.
Frequently Asked Questions
For adults, the maximum single dose is 1,000 mg (two 500mg extra-strength tablets). Taking more than 4,000 mg total in 24 hours increases liver damage risk. Acute overdoses of 7 grams or more can cause hepatotoxicity according to medical research.
Initial symptoms include nausea, vomiting, loss of appetite, and sweating, usually appearing within 24 hours. However, many people have no symptoms in the first stage, making overdose particularly dangerous. Right upper abdominal pain developing after 24-72 hours indicates liver involvement.
Recovery depends on severity and treatment timing. With prompt NAC treatment, most patients recover completely. Severe cases may progress to stage 4, which has two outcomes: complete recovery over several weeks, or irreversible multi-organ failure requiring liver transplant.
Yes. The FDA specifically warns that severe liver damage may occur when consuming three or more alcoholic drinks daily while using acetaminophen. Alcohol depletes glutathione stores needed to neutralize toxic metabolites and may increase formation of harmful NAPQI.
Call Poison Control immediately at 1-800-222-1222 or use the webPOISONCONTROL online tool. Both options provide free, confidential expert guidance 24/7. Don’t wait for symptoms—treatment effectiveness drops significantly after 8 hours. If someone collapses, has seizures, or trouble breathing, call 911.
Children face overdose risk when caregivers misunderstand concentration or dosing. The poison control organization notes that confusion about formulations has led to accidental overdoses. Always use the measuring device that comes with children’s medication and verify dosing based on weight, not age.
Acetaminophen has a half-life of about 2-3 hours in healthy adults. It’s mostly eliminated within 24 hours. However, toxic metabolites can continue damaging the liver for days after ingestion if glutathione stores are depleted, which is why symptoms often worsen 24-72 hours post-overdose.
The Bottom Line
Acetaminophen is genuinely safe when used correctly. It’s effective, widely available, and has helped billions of people manage pain and fever.
But the difference between safe and dangerous is smaller than most people realize. Two extra-strength tablets every six hours puts someone at the daily maximum. Adding a nighttime cold medicine or second pain reliever can push them into dangerous territory.
According to authoritative medical sources, acetaminophen poisoning causes more acute liver failure cases than any other drug in the United States. Yet half of these cases are completely unintentional.
Check every medication label. Count total daily acetaminophen from all sources. When in doubt, call a pharmacist or healthcare provider.
And if overdose is suspected—don’t wait. Contact Poison Control at 1-800-222-1222 immediately. Those first eight hours make the difference between complete recovery and permanent liver damage.
