Quick Summary: Continuing to eat food you’re allergic to can trigger increasingly severe immune reactions, ranging from mild symptoms like hives and digestive issues to life-threatening anaphylaxis. Repeated exposure may worsen allergic responses over time and lead to chronic health complications affecting multiple organ systems. The safest approach is complete avoidance of known allergens and carrying emergency medication if prescribed.
Food allergies represent a serious public health concern, affecting over 220 million individuals worldwide, including approximately 33 million people in the United States. Among these, 5.6 million are children. But what happens when someone continues consuming foods their body has flagged as dangerous?
The answer isn’t simple. Each exposure to an allergen can trigger different reactions, and the consequences of repeated consumption range from uncomfortable to potentially fatal.
Understanding Food Allergy Reactions
When someone with a food allergy consumes the problematic food, their immune system launches an aggressive defense. The body mistakenly identifies harmless food proteins as threats and produces IgE antibodies to fight them off.
According to the CDC, symptoms of alpha-gal syndrome typically appear within 2–6 hours after exposure. However, IgE-mediated food allergies generally develop within minutes to a few hours.
The immediate effects of continuing to consume food you’re allergic to differ for each person. This variability depends on several factors: the individual’s immune response, the amount of allergen consumed, which tissue receptors are affected, and the time elapsed since previous exposure.
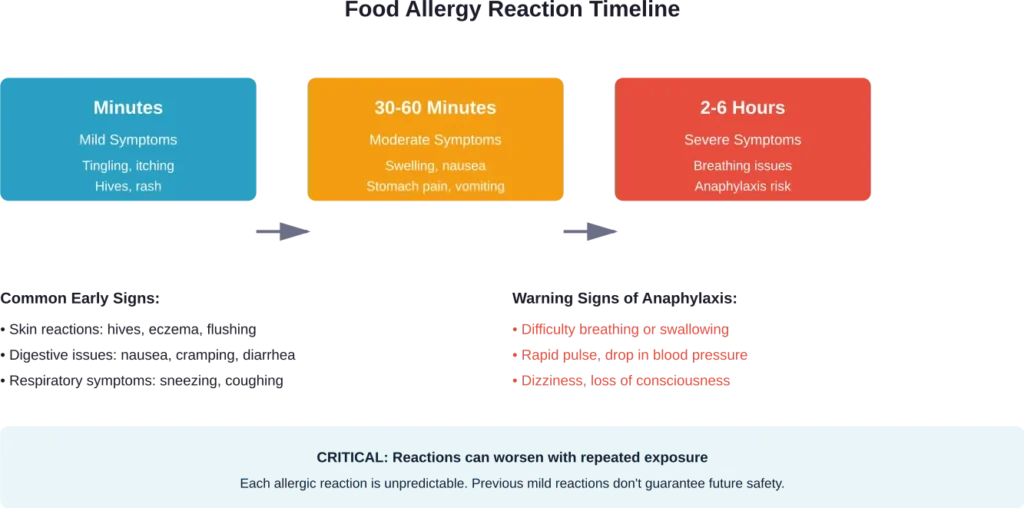
Immediate Health Risks
The most pressing danger of consuming allergenic foods is anaphylaxis—a life-threatening allergic reaction that can develop rapidly. Research shows that 51% of adults and 42% of children with a food allergy experience a severe reaction at some point.
Anaphylaxis symptoms include difficulty breathing, swollen airways, rapid pulse, dizziness, and a dangerous drop in blood pressure. Without immediate treatment with epinephrine, anaphylaxis can be fatal.
But here’s the thing: reactions aren’t always predictable. Someone might experience mild symptoms one time and severe anaphylaxis the next. The nature and severity depend on multiple variables that change from one exposure to another.
Common Immediate Symptoms
| Body System | Mild to Moderate Symptoms | Severe Symptoms |
|---|---|---|
| Skin | Hives, itching, eczema, flushing | Widespread swelling, severe rash |
| Digestive | Nausea, stomach pain, diarrhea | Severe vomiting, abdominal cramping |
| Respiratory | Runny nose, sneezing, mild cough | Wheezing, throat tightness, difficulty breathing |
| Cardiovascular | Mild increase in heart rate | Rapid pulse, drop in blood pressure, shock |
| Neurological | Mild anxiety, tingling | Dizziness, confusion, loss of consciousness |
Long-Term Consequences of Continued Exposure
Repeated consumption of allergens doesn’t just cause immediate reactions. According to CDC research on chronic sequelae of foodborne disease, chronic complications may occur in 2% to 3% of foodborne disease cases, with potential long-term consequences to human health.
Chronic allergic inflammation is on the rise in the United States and other developed countries. When the immune system remains in a constant state of alert, it can lead to several complications.
Chronic Inflammatory Conditions
Ongoing exposure to food allergens can contribute to persistent inflammatory states. The body’s continuous production of IgE antibodies and inflammatory mediators like histamine keeps tissue in a stressed condition.
This chronic inflammation may manifest in conditions affecting multiple systems: rheumatoid disease, autoimmune thyroid disease, inflammatory bowel disease, and renal disease have all been associated with chronic foodborne exposure in medical literature.
The link between chronic allergy signaling and mitochondrial stress represents an emerging area of research. Stressed mitochondria in cells affected by ongoing allergic responses may contribute to broader systemic health issues.
Worsening Allergic Sensitivity
Contrary to what some might hope, continuing to eat allergenic foods doesn’t typically lead to tolerance. In most cases, repeated exposure can actually sensitize the immune system further.
Each encounter with the allergen reinforces the immune system’s response pattern. The body produces more IgE antibodies, more mast cells become primed to react, and the threshold for triggering a reaction may lower.
That said, controlled medical interventions like oral immunotherapy represent a different scenario. Under strict medical supervision, gradually increasing doses of allergens can sometimes retrain the immune system—but this is fundamentally different from uncontrolled, repeated exposure.
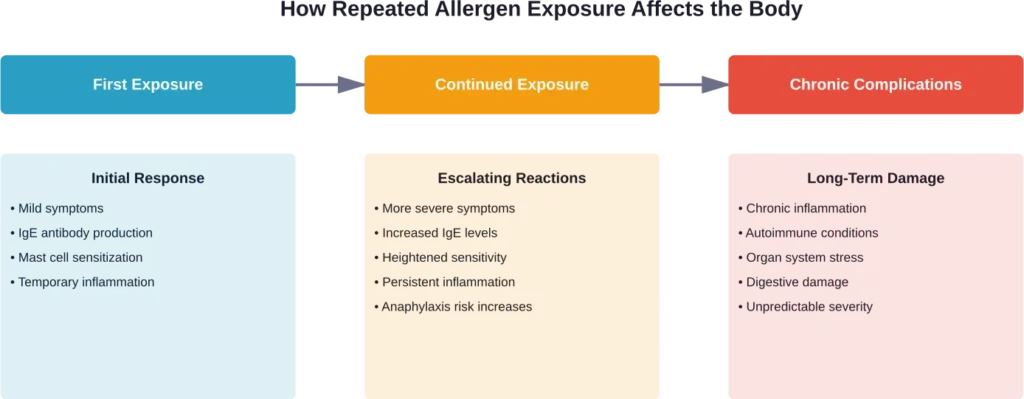
Food Allergy vs. Food Intolerance
Not all adverse food reactions involve the immune system. Food intolerance affects the digestive system and occurs when the body has trouble digesting certain foods or ingredients.
Some research suggests that approximately 20% of people report a food intolerance. Unlike allergies, intolerances typically cause uncomfortable but not life-threatening symptoms: nausea, heartburn, bloating, upset stomach, and gas.
The distinction matters. Someone with lactose intolerance might experience digestive discomfort from dairy but faces no risk of anaphylaxis. Someone with a milk allergy, however, could develop a severe and potentially fatal reaction.
The Alpha-Gal Syndrome Example
Alpha-gal syndrome demonstrates how unique food allergies can be. This condition, often triggered by tick bites, causes reactions to red meat and dairy products.
What makes it unusual? Symptoms typically appear 2–6 hours after consuming products containing alpha-gal—much later than typical food allergies. According to the CDC, reactions can range from mild to severe and life-threatening, and they can be different from person to person.
This delayed reaction pattern means someone might not immediately connect their symptoms to food consumed hours earlier, potentially leading to repeated exposures before diagnosis.
Why Complete Avoidance Matters
Medical consensus is clear: the standard of care for food allergies consists of food-allergen avoidance and carrying emergency medication like epinephrine auto-injectors.
Complete avoidance means vigilant label reading, asking about ingredients at restaurants, and understanding cross-contamination risks. The FDA enforces regulations requiring companies to list major food allergens on packaged foods.
Sesame is included among allergens that must be clearly labeled on food products, alongside milk, eggs, fish, shellfish, tree nuts, peanuts, wheat, and soybeans.
Even trace amounts can trigger reactions in highly sensitive individuals. Cross-contamination during food processing or preparation presents real risks that can’t be dismissed.
Frequently Asked Questions
No. Continued exposure to food allergens typically doesn’t lead to tolerance and can actually worsen allergic sensitivity. Each exposure reinforces the immune response and may increase the severity of future reactions. Controlled oral immunotherapy under medical supervision is a different scenario that involves carefully calibrated doses.
Most IgE-mediated food allergy symptoms develop within minutes to a few hours after eating the allergenic food. Reactions typically occur within this timeframe, though some allergies like alpha-gal syndrome can cause delayed reactions appearing several hours later.
Food allergies involve the immune system producing IgE antibodies and can cause life-threatening reactions. Food intolerances affect only the digestive system, causing uncomfortable but not dangerous symptoms like bloating, gas, and nausea. Food allergy affects an estimated 8% of children under age 5 and up to 4% of adults.
Yes. Allergic reactions are unpredictable. Someone who previously experienced only mild symptoms can suddenly develop severe anaphylaxis upon subsequent exposure. Research shows that 51% of adults and 42% of children with food allergies experience severe reactions at some point, regardless of previous mild symptoms.
According to CDC research on chronic sequelae of foodborne disease, chronic complications may occur in 2-3% of foodborne disease cases. Long-term complications can include chronic inflammatory conditions, autoimmune disorders, inflammatory bowel disease, and damage to multiple organ systems. Ongoing immune system activation from repeated exposure keeps the body in a stressed state.
Yes. Medical professionals recommend that anyone with diagnosed food allergies carry epinephrine, regardless of past reaction severity. Since reactions are unpredictable and can escalate quickly, having emergency medication available can be lifesaving. Discuss an emergency action plan with your healthcare provider.
Food allergy testing—including skin prick tests and blood tests measuring specific IgE antibodies—provides useful diagnostic information but isn’t perfect. False positives and false negatives can occur. Diagnosis typically combines test results with clinical history and, in some cases, medically supervised food challenges to confirm allergies.
The Bottom Line
Continuing to eat foods you’re allergic to poses serious and escalating health risks. Each exposure can trigger unpredictable reactions ranging from uncomfortable symptoms to life-threatening anaphylaxis.
Beyond immediate dangers, repeated allergen consumption may lead to chronic inflammatory conditions and progressive immune system sensitization. The body doesn’t adapt—it intensifies its defensive response.
If you suspect a food allergy, seek proper medical evaluation. Allergists can perform diagnostic testing and develop management plans tailored to your specific situation. With accurate diagnosis and strict avoidance strategies, people with food allergies can live full, healthy lives while minimizing risks.
Don’t gamble with allergen exposure. The temporary convenience of eating a problem food isn’t worth the potential consequences to your health and wellbeing.
