Quick Summary: Popping a stye is strongly discouraged as it can spread bacteria, worsen the infection, and lead to serious complications like periorbital cellulitis. According to the NIH, styes typically drain naturally within 5-7 days with warm compresses, though some may take up to two weeks, and manual popping can push infection deeper into surrounding tissues, potentially requiring medical intervention.
That red, painful bump on your eyelid is frustrating. It’s tender, noticeable, and the temptation to squeeze it can feel overwhelming. But before reaching for the mirror and your fingers, here’s what you need to know about the risks of popping a stye.
The short answer? Don’t do it. What seems like a quick fix can actually make things significantly worse.
Understanding What a Stye Actually Is
A stye, medically termed hordeolum, is an acute bacterial infection affecting the oil glands along your eyelid margin. According to the National Institutes of Health, these infections arise when bacteria—typically Staphylococcus aureus—invade and block the small glands at the base of your eyelashes.
Styes appear as small, red, tender bumps that can develop either externally along the eyelid edge or internally underneath the lid. The CDC notes that about 30% of people carry Staph bacteria in their noses, making cross-contamination to the eyes relatively common through touching.
The gland becomes plugged with oil, dead skin cells, and debris. Bacteria multiply within this blocked environment, creating the characteristic painful, pus-filled bump. Most styes develop quickly and hurt more than they actually harm—but only if left alone to heal properly.
The Immediate Dangers of Popping a Stye
When you squeeze or pop a stye, several problematic things happen simultaneously. None of them help.
Bacterial Spread and Deeper Infection
Squeezing forces bacteria deeper into surrounding tissues rather than expelling it outward. According to NIH research on hordeolum complications, manual manipulation can push the infection past the orbital septum—a thin fibrous membrane that normally acts as a protective barrier.
This creates risk for periorbital cellulitis, a more serious infection of the eyelid and surrounding soft tissues. The American Academy of Ophthalmology warns that in rare cases, infection can progress to orbital cellulitis, which affects deeper eye structures and requires urgent medical intervention.
Tissue Damage and Scarring
The eyelid contains delicate skin and sensitive structures. Aggressive squeezing damages healthy tissue surrounding the infected gland. This trauma can lead to:
- Permanent scarring along the eyelid margin
- Damage to nearby oil glands, increasing future stye risk
- Disruption of eyelash follicles
- Prolonged inflammation and swelling
The pressure applied during popping also ruptures small blood vessels, causing additional bruising and extending your recovery time.
Contamination to Other Areas
Staphylococcus aureus is highly contagious. When pus from a popped stye contacts your fingers, it easily transfers to:
- Your other eye
- Different areas of the same eyelid
- Other people through shared towels or pillowcases
- Your nose or mouth if you touch your face
According to CDC infection control guidance, Staph bacteria can survive on surfaces and cause secondary infections elsewhere on your body.
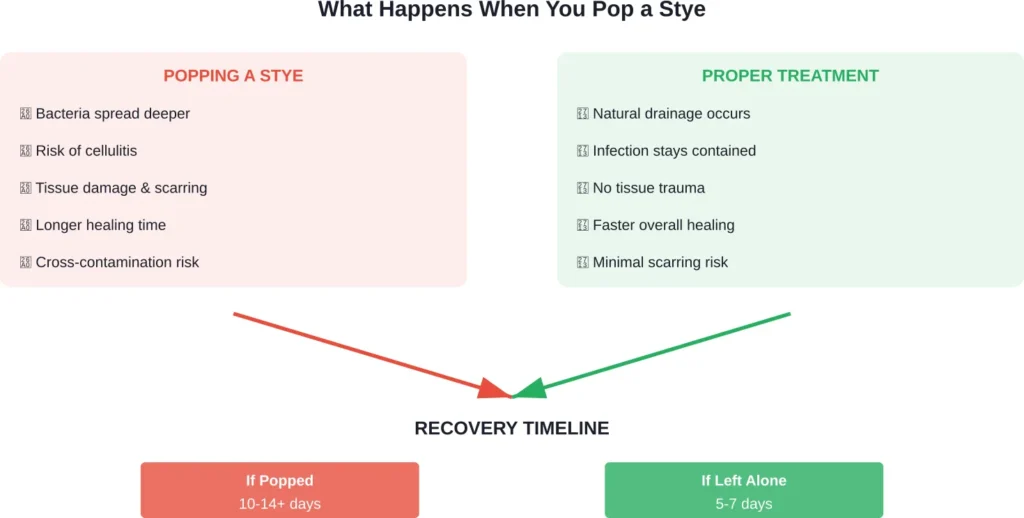
When a Stye Pops on Its Own
Sometimes styes drain spontaneously without any squeezing. This natural drainage is fundamentally different from forced popping.
When a stye opens naturally, it typically happens gradually as the infection matures and the body’s immune response creates a controlled exit point. The drainage is usually minimal, and the surrounding tissue experiences less trauma.
If your stye has popped on its own, the following steps are recommended after natural stye drainage:
- Gently clean the area with warm water and a clean cloth
- Avoid touching or rubbing your eye
- Continue warm compresses to encourage complete drainage
- Monitor for signs of worsening infection
- Keep the area clean and avoid makeup for several days
Anecdotal reports from patients indicate that many people experience relief once natural drainage occurs. However, persistent pain, increased swelling, or vision changes after 48 hours warrant professional evaluation.
Safe and Effective Stye Treatment Methods
The NIH recommends conservative home treatment for most uncomplicated styes. These methods work with your body’s natural healing processes rather than against them.
Warm Compress Therapy
This remains the gold standard for stye treatment. Heat promotes blood flow, helps liquefy blocked oil, and encourages natural drainage.
Proper technique matters:
- Soak a clean washcloth in warm (not hot) water
- Wring out excess water
- Apply to the closed eyelid for 5-10 minutes
- Repeat 3-6 times daily
- Use a fresh, clean cloth each time
Warm compress therapy should be applied for 5-10 minutes at a time, repeated 3-6 times daily.
Proper Eyelid Hygiene
Keeping the eyelid clean prevents secondary infection and supports healing. Gently wash the eyelid margin with diluted baby shampoo or specialized eyelid cleansers once daily.
Avoid eye makeup, contact lenses, and shared towels until the stye completely resolves. These all introduce additional bacteria or irritation.
Over-the-Counter Options
Non-prescription antibiotic ointments designed for eye use may help prevent bacterial spread. However, these treat surface bacteria and won’t penetrate to drain the blocked gland.
Pain relievers like ibuprofen can reduce discomfort and inflammation, but they don’t speed healing.
When Medical Intervention Becomes Necessary
Most styes resolve within one week with home care. But certain situations require professional evaluation.
See an eye doctor if:
- Pain and swelling worsen after 48 hours of home treatment
- The stye doesn’t improve within one week
- Vision becomes blurry or impaired
- Swelling spreads beyond the immediate bump area
- You develop fever or feel systemically unwell
- Multiple styes develop simultaneously
- Styes recur frequently
According to NIH research, recurrent styes often link to underlying conditions like blepharitis, rosacea, or diabetes. Persistent problems warrant evaluation for these contributing factors.
Professional Treatment Options
When home treatment fails, ophthalmologists can provide more aggressive interventions. These include prescription antibiotic ointments or oral antibiotics for spreading infection.
For particularly stubborn styes, doctors may perform incision and drainage in a sterile clinical setting. This controlled procedure differs dramatically from home popping—it’s done with proper instruments, under sterile conditions, with local anesthesia.
The key difference? Professional drainage removes the entire infected material while minimizing tissue damage and contamination risk.
Preventing Future Styes
Some people experience recurrent styes despite treatment. Prevention strategies target the underlying causes.
| Prevention Method | How It Helps | Frequency |
|---|---|---|
| Daily eyelid cleaning | Removes oil and debris that block glands | Once or twice daily |
| Proper makeup removal | Prevents product buildup in glands | Every night |
| Replace eye cosmetics | Eliminates bacterial contamination | Every 3-6 months |
| Avoid touching eyes | Reduces bacterial transfer | Continuous habit |
| Manage blepharitis | Treats chronic eyelid inflammation | As prescribed |
| Control rosacea | Reduces oil gland dysfunction | Ongoing with dermatologist |
For people with chronic blepharitis, the American Academy of Ophthalmology recommends regular warm compresses and eyelid scrubs as maintenance therapy, not just treatment during active infection.
Managing underlying conditions like diabetes also reduces stye frequency, as better blood sugar control improves immune function and bacterial resistance.
Distinguishing Styes from Other Eyelid Bumps
Not every eyelid bump is a stye. Chalazia, while similar in appearance, follow different courses and need different approaches.
A chalazion forms when an oil gland becomes blocked without acute bacterial infection. These bumps tend to develop more slowly, hurt less, and persist longer than styes. According to medical literature, chalazia account for 13.4% of all benign eyelid lesions.
While styes are typically red, tender, and located right at the eyelid margin near lashes, chalazia often appear as painless lumps set back slightly from the edge. They may require steroid injections or surgical removal if they don’t resolve spontaneously.
Other conditions that mimic styes include milia, xanthelasma, and rarely, eyelid tumors. Persistent lumps that don’t follow typical stye patterns need professional evaluation to rule out more serious conditions.
Frequently Asked Questions
While rare, severe complications from popping a stye can theoretically affect vision. If infection spreads to orbital structures behind the eye, it can cause orbital cellulitis—a serious condition requiring urgent treatment. However, permanent blindness from a routine stye is extremely uncommon when appropriate medical care is sought.
According to NIH sources, most styes resolve within 5-7 days with proper warm compress treatment. Some may take up to two weeks. Styes that persist beyond two weeks despite home care should be evaluated by an eye doctor.
No. Contact lenses can harbor bacteria, potentially worsening the infection or spreading it across the eye surface. Switch to glasses until the stye completely heals and symptoms resolve for at least 24 hours.
Only use antibiotic ointments specifically formulated for ophthalmic use. Regular skin antibiotics can irritate eye tissues. Even ophthalmic antibiotics primarily prevent spread rather than cure styes, which need to drain naturally. Consult a doctor before applying any medication near your eyes.
Recurrent styes often indicate underlying conditions. The NIH identifies blepharitis, acne rosacea, and diabetes as common culprits. Poor eyelid hygiene, contaminated cosmetics, and chronic eye rubbing also contribute. If you experience frequent styes, see an ophthalmologist to identify and address root causes.
Many styes do drain spontaneously as they mature. This natural drainage typically happens gradually and causes less tissue damage than forced popping. However, some styes reabsorb without ever coming to a head, particularly smaller ones caught early with aggressive warm compress treatment.
The bacteria causing styes can transfer to your other eye through contaminated fingers, towels, or pillowcases. This is why careful hand hygiene and using separate, clean cloths for each eye during treatment is crucial. The infection itself doesn’t “jump” between eyes, but cross-contamination is definitely possible.
The Bottom Line on Stye Popping
The temptation to pop that painful eyelid bump is understandable. It looks like a pimple, it feels like a pimple, so why not treat it like one?
Because it’s not a pimple. It’s an active bacterial infection in one of the most delicate, vascular areas of your body. The risks of spreading infection, damaging tissue, and prolonging your recovery far outweigh any temporary satisfaction from squeezing.
Warm compresses work. They’re boring, they require patience, but they align with how your body naturally fights and resolves these infections. Give them the full week before concluding they’ve failed.
If home treatment isn’t working or you’re experiencing concerning symptoms, see an eye care professional. They have the tools and expertise to safely resolve stubborn styes without the complications that come from DIY approaches.
Your eyes are worth the patience. Keep your hands off that stye.
