Quick Summary: Drinking alcohol just 2 days before surgery significantly increases risks of complications including bleeding, infection, and anesthesia interference. Medical research shows stopping alcohol 2-4 weeks prior to surgery reduces postoperative complications by up to 50%, with a minimum 48-hour abstinence required for safer outcomes.
Surgery puts the body under significant stress. Every decision made in the days leading up to a procedure can influence outcomes, recovery time, and complication rates.
Drinking alcohol within 48 hours of surgery isn’t just inadvisable—it creates measurable risks that surgical teams work hard to avoid. The interaction between alcohol and anesthesia, combined with alcohol’s effects on blood clotting and immune function, makes even moderate drinking problematic.
Here’s what actually happens when alcohol enters the equation two days before a surgical procedure.
How Alcohol Affects Anesthesia and Sedation
Alcohol and anesthesia affect the same body systems. Both suppress central nervous system function, slow breathing, and reduce heart rate. When alcohol remains in the system during surgery, predicting anesthesia response becomes significantly harder.
The problem isn’t just about alcohol still circulating in the bloodstream. Alcohol consumption within 48 hours alters how anesthesia medications work, even after the alcohol itself has been metabolized.
Anesthesiologists must carefully calibrate dosing to maintain unconsciousness and pain control while keeping vital functions stable. Alcohol disrupts this balance. Some patients may need higher doses to achieve adequate sedation, while others experience exaggerated responses.
Medical sources note that alcohol suppresses breathing, heart rate, and blood circulation—the exact functions anesthesiologists monitor most carefully. This overlap creates dangerous unpredictability during procedures.
Increased Bleeding Risk During Surgery
Alcohol interferes with platelet function and blood clotting mechanisms. Platelets are blood cells responsible for forming clots to stop bleeding. When alcohol affects their function, surgical bleeding becomes harder to control.
This risk persists even when blood tests show normal platelet counts. The cells may be present in normal numbers but function poorly due to recent alcohol consumption.
For procedures involving significant tissue manipulation or vascular work, uncontrolled bleeding can extend surgery time, require transfusions, or lead to hematoma formation during recovery. Surgeons rely on predictable clotting function—alcohol removes that predictability.
Compromised Immune Function and Infection Risk
Surgical sites are vulnerable to infection. The body’s immune response determines whether minor bacterial exposure becomes a serious postoperative infection.
Alcohol suppresses immune system function. White blood cells become less effective at identifying and eliminating pathogens. This immunosuppression continues for days after alcohol consumption stops.
Research indicates that high-risk alcohol use is a common preventable risk factor for postoperative complications, including admission to intensive care and longer hospital stays.
Two days provides insufficient time for immune function to fully recover. Surgical incisions made while the immune system operates below baseline face higher infection rates.
Medication Interactions and Drug Metabolism
Surgery involves multiple medications beyond anesthesia: antibiotics, pain relievers, anti-nausea drugs, and sometimes blood pressure medications. Alcohol affects how the liver processes all of these.
The liver uses specific enzyme systems to metabolize both alcohol and most medications. Recent alcohol consumption can either speed up or slow down drug metabolism, making standard dosing unreliable.
Some antibiotics become less effective when alcohol affects liver enzymes. Pain medications may reach toxic levels or fail to provide adequate relief. These unpredictable interactions complicate postoperative care.
Delayed Healing and Extended Recovery
Tissue repair requires optimal conditions: adequate blood flow, proper nutrition delivery, and efficient waste removal. Alcohol disrupts all three.
Blood vessels don’t function normally after recent alcohol exposure. Microcirculation in healing tissues becomes less efficient. Nutrients and oxygen reach surgical sites more slowly.
Research indicates that average weekly alcohol use decreased 50%-60% between baseline and follow-up in preoperative alcohol intervention studies, with short-term abstinence of 2 to 4 weeks prior to surgery linked to lower likelihood of complications. Even the minimum 48-hour abstinence provides measurable benefits compared to drinking up until surgery day.
Wound healing happens at the cellular level. When those cells operate in a compromised environment, recovery timelines extend.
Nausea, Vomiting, and Aspiration Risks
Postoperative nausea affects many surgical patients. Alcohol consumption before surgery significantly increases this risk.
Medical research indicates that alcohol increases the risk of nausea, vomiting, and aspiration—inhaling vomit into the lungs. Aspiration during or immediately after surgery can cause pneumonia or acute respiratory distress.
The combination of anesthesia effects, surgical stress, and residual alcohol impact creates a perfect storm for severe nausea. When patients cannot keep down oral medications or fluids, recovery becomes more complicated.
Blood Sugar Instability
Alcohol affects glucose regulation. The liver normally maintains steady blood sugar levels by releasing stored glucose when needed. Alcohol interferes with this process.
During surgery, maintaining stable blood sugar matters for multiple reasons. Too-low blood sugar affects brain function and recovery from anesthesia. Too-high blood sugar impairs immune function and wound healing.
Patients who drink within two days of surgery often show unpredictable blood sugar patterns during and after procedures. This instability requires more intensive monitoring and intervention.
What Medical Guidelines Actually Recommend
Medical consensus is clear: 48 hours represents the absolute minimum alcohol-free period before surgery. But minimum and optimal are different standards.
Medical guidelines recommend that alcohol should be avoided for at least 48 hours before scheduled surgery to minimize the possibility of serious complications during and after the procedure.
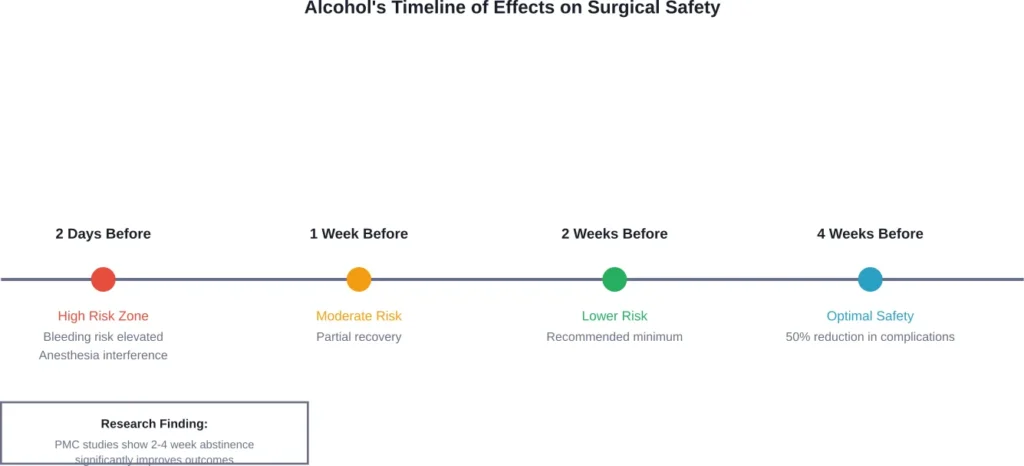
Research published in PMC journals indicates that short-term abstinence from alcohol use (2 to 4 weeks) prior to surgery is linked to a lower likelihood of postoperative complications.
| Abstinence Period | Risk Level | Clinical Notes |
|---|---|---|
| Less than 48 hours | High risk | Surgery may be postponed; significant complication risks |
| 2-7 days | Moderate risk | Some residual effects; not optimal but better than <48 hours |
| 2 weeks | Reduced risk | Standard recommendation for most elective procedures |
| 4 weeks | Optimal | 50% reduction in complications documented in research |
When Surgery Cannot Be Delayed
Emergency procedures don’t allow time for alcohol abstinence. In these cases, surgical teams adjust protocols based on known recent alcohol consumption.
Anesthesiologists may use different medication combinations. Surgical teams prepare for increased bleeding risk. Postoperative monitoring becomes more intensive.
But when surgery is elective—planned in advance—there’s no medical justification for proceeding with alcohol in the system. The risks are known, measurable, and avoidable.
Frequently Asked Questions
Many surgical centers will postpone elective procedures if patients consumed alcohol within 48 hours. Anesthesiologists assess individual risk, but most facilities enforce minimum abstinence requirements to ensure patient safety and optimal outcomes.
No. Beer, wine, and spirits all create the same physiological effects relevant to surgery. The total amount of pure alcohol consumed matters, not the beverage type. One standard drink contains similar alcohol content regardless of source.
Even moderate alcohol consumption affects anesthesia response, blood clotting, and immune function. While heavy drinking creates higher risks, light to moderate consumption still introduces measurable complications. Medical guidelines recommend complete abstinence regardless of quantity.
Alcohol typically metabolizes within 24 hours, but its effects on body systems persist longer. Platelet function, immune response, and liver enzyme activity remain altered for several days after blood alcohol returns to zero. This is why 48 hours is the minimum recommendation.
Postoperative alcohol consumption should wait until pain medications are discontinued, surgical wounds show healing progress, and medical clearance is given. Alcohol interferes with pain medication, slows healing, and can cause dangerous interactions with antibiotics and other post-surgery drugs.
Complete honesty about alcohol consumption is essential. Surgical teams need accurate information to plan appropriate anesthesia, anticipate complications, and ensure safety. Underreporting alcohol use puts patients at serious risk during procedures.
Patients can switch to alcohol-free alternatives or sparkling water in the weeks before surgery. Managing pre-surgery anxiety through meditation, light exercise, or speaking with healthcare providers about concerns provides safer stress relief than alcohol.
The Bottom Line on Pre-Surgery Drinking
Two days before surgery is too close to consume alcohol safely. The science is unambiguous: alcohol creates measurable risks for anesthesia complications, increased bleeding, infection, and delayed recovery.
Medical research demonstrates that four weeks of abstinence reduces complications by half. Even meeting the 48-hour minimum provides significantly better outcomes than drinking closer to surgery date.
Elective surgery represents an opportunity to optimize health outcomes through preparation. Abstaining from alcohol ranks among the most impactful steps patients can take to ensure successful procedures and smooth recovery.
When surgery dates are scheduled, mark the calendar and plan accordingly. The temporary sacrifice of alcohol consumption pays dividends in safety, faster healing, and fewer complications. Talk to surgical teams about specific recommendations based on individual health status and procedure type.
