Quick Summary: Popping a cold sore is harmful and should be avoided. It spreads the herpes simplex virus to other areas, increases infection risk, delays healing, and can cause scarring. Instead, use over-the-counter antiviral creams early in the outbreak and keep the area clean to speed recovery.
That tingling sensation around your lips signals trouble. A cold sore is forming, and within hours, small blisters appear. The temptation to pop them is real.
But here’s the thing—popping cold sores creates more problems than it solves. The blister fluid contains millions of viral particles just waiting to spread.
Cold sores are caused by herpes simplex virus type 1 (HSV-1), which infects a significant portion of the population. According to the CDC, HSV-1 often causes oral herpes, which can result in cold sores or fever blisters on or around the mouth. The virus remains dormant in nerve cells and reactivates during stress, illness, or sun exposure.
Understanding what happens when you pop a cold sore—and what to do instead—can save you from prolonged healing, scarring, and spreading the infection.
What Is a Cold Sore?
Cold sores are small, fluid-filled blisters that typically appear on or around the lips. They’re caused by the herpes simplex virus, primarily HSV-1, though HSV-2 can also cause oral infections.
The CDC notes that HSV-1 is typically transmitted through oral-oral contact. Once infected, the virus never leaves your body. It hides in nerve cells and can reactivate multiple times throughout life.
Common triggers include:
- Emotional or physical stress
- Fatigue and lack of sleep
- Sun exposure or wind
- Hormonal changes
- Weakened immune system
- Dental procedures or lip injury
Most people experience a tingling or burning sensation before blisters appear. This prodrome stage offers the best window for treatment.
The Cold Sore Lifecycle
Understanding how cold sores develop helps explain why popping them backfires.
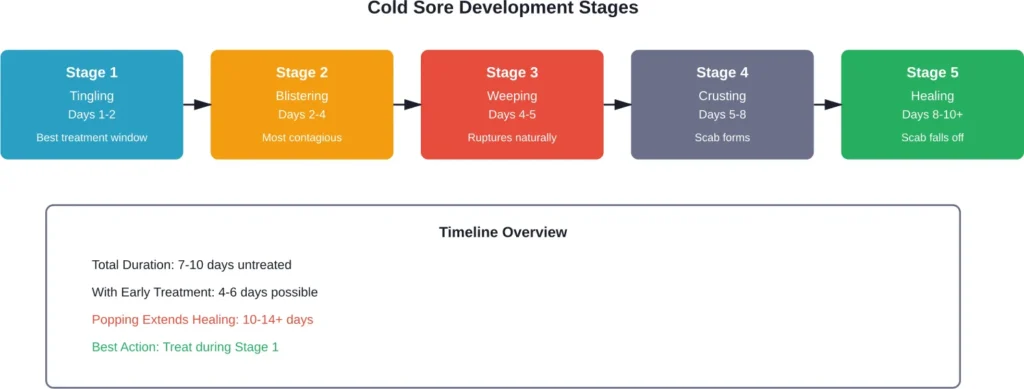
Without interference, cold sores typically heal in 7-10 days. The blisters rupture naturally during stage 3, releasing fluid before forming a protective scab.
Popping disrupts this process and introduces complications.
What Happens When You Pop a Cold Sore
Squeezing or bursting a cold sore blister releases highly infectious fluid packed with viral particles. This creates several immediate problems.
Spreads the Virus to Other Areas
The fluid inside cold sore blisters contains millions of HSV-1 particles. When you pop a blister, this fluid contacts your fingers, spreads across your skin, and can infect new areas.
Common spread zones include:
- Other parts of your lips or face
- Inside your nose
- Your eyes (HSV keratitis)
- Your fingers (herpetic whitlow)
- Genital area if touched after contact
According to the CDC, HSV can cause serious eye infections when the virus spreads to the cornea. This condition, known as HSV keratitis, can lead to scarring of the cornea or blindness when left untreated.
The CDC also notes that herpetic whitlow—HSV infection of the fingers—occurs through direct inoculation. Healthcare workers and people who touch active cold sores face higher risk.
Increases Secondary Infection Risk
Popping creates an open wound. The protective barrier your skin provides is now breached.
Bacteria, fungi, and other pathogens can enter the wound. This leads to secondary infections that require different treatment and significantly extend healing time.
Signs of bacterial infection include:
- Increased redness spreading beyond the original sore
- Yellow or green pus
- Increased pain and swelling
- Warmth around the area
- Fever or feeling unwell
Secondary infections may require antibiotic treatment on top of antiviral therapy.
Delays Healing Significantly
The natural cold sore healing process involves controlled rupture, scab formation, and tissue repair. Popping disrupts this sequence.
When you force a blister open prematurely:
- The wound is larger and deeper than natural rupture would create
- Protective cellular responses are interrupted
- Scab formation is delayed or incomplete
- The area remains vulnerable to repeated trauma
Cold sores that are popped often take 10-14 days to heal instead of the typical 7-10 days.
Creates Permanent Scarring
Forced rupture damages skin tissue more severely than natural progression. The deeper wound affects more layers of skin.
Scarring becomes more likely when:
- The wound is picked at repeatedly
- Secondary infection develops
- Scabs are removed before full healing
- The same area experiences repeated trauma
Facial scarring from cold sores can be permanent, appearing as small pits, discolored patches, or textural changes.
Transmits to Others More Easily
According to the CDC, HSV spreads through kissing even without visible symptoms—a phenomenon called asymptomatic shedding. But active sores dramatically increase transmission risk.
When you pop a cold sore, viral particles spread to surfaces, objects, and other people through:
- Direct contact (kissing, touching)
- Shared items (cups, utensils, lip balm)
- Towels and washcloths
- Your hands touching others
The CDC emphasizes that oral herpes can cause genital infections through oral-genital contact, making transmission prevention important during outbreaks.
Why the Temptation to Pop Is So Strong
Understanding the psychological factors helps resist the urge.
Cold sores are visible, often appearing right before important events. The desire to make them disappear quickly is powerful. The fluid-filled appearance makes them seem “ready” to pop, similar to a pimple.
But here’s the difference: pimples contain sebum and dead skin cells. Cold sores contain active virus.
The physical discomfort—tightness, tingling, and pressure—makes people think releasing the fluid will provide relief. In reality, it increases pain by exposing raw tissue and nerve endings.
What to Do Instead of Popping
Effective cold sore management focuses on antiviral action, symptom relief, and preventing spread.
Start Antiviral Treatment Immediately
Over-the-counter topical treatments containing aciclovir or penciclovir work best when applied during the tingling stage, before blisters fully form.
These medications slow viral replication, reducing blister size and healing time. Apply them every 2-3 hours during waking hours for maximum effectiveness.
For frequent outbreaks, prescription oral antivirals provide stronger results. Options include acyclovir, famciclovir, and valacyclovir. These medications can reduce outbreak duration and, when taken daily, prevent recurrences.
Apply Cold Compresses
The American Academy of Dermatology recommends applying a cold, wet, clean towel to cold sores for 5-10 minutes several times daily. This reduces redness, swelling, and discomfort without damaging tissue.
The cooling effect provides temporary pain relief and helps dry out blisters naturally.
Keep the Area Clean and Dry
Gentle cleansing prevents secondary infection without irritating the sore. Wash your hands thoroughly before and after any contact with the area.
Pat dry with a clean towel—never rub. Keeping the area dry between treatments helps scabs form properly.
Avoid Touching or Picking
This sounds obvious, but it’s critical. Every time you touch a cold sore, you risk spreading the virus.
Keep your hands away from your face. If you must apply medication, wash hands immediately afterward. Never share towels, utensils, or personal items during an outbreak.
Protect Your Lips
Sun exposure triggers cold sore outbreaks. Use lip balm with SPF 30 or higher daily, even when you don’t have active sores.
During an outbreak, petroleum jelly can keep scabs from cracking, though it doesn’t speed healing. Apply with a clean cotton swab, never your finger.
Pain Management
Over-the-counter pain relievers like ibuprofen or acetaminophen reduce discomfort and inflammation. Topical numbing agents containing benzocaine provide temporary relief but don’t affect healing.

How Long Does a Cold Sore Take to Heal?
Healing time depends on when treatment starts and whether the sore is disturbed.
| Scenario | Typical Healing Time | Key Factors |
|---|---|---|
| Early antiviral treatment (during tingling stage) | 4-6 days | Virus replication limited before blisters fully form |
| Treatment after blisters appear | 7-10 days | Antivirals still help but less dramatically |
| No treatment, left alone | 10-14 days | Natural immune response handles virus |
| Popped or repeatedly touched | 14+ days | Secondary infection risk, delayed scab formation |
Research indicates that vesicles contain the highest virus concentration within the first 24-48 hours after appearance, which can show high positivity on viral culture testing. This window represents peak contagiousness and optimal treatment timing.
Preventing Future Outbreaks
While you can’t eliminate HSV-1 from your body, you can reduce outbreak frequency.
Identify Your Triggers
Track when outbreaks occur. Common patterns include:
- Stressful periods at work or home
- Lack of sleep or irregular sleep schedule
- Prolonged sun exposure
- Illness or weakened immunity
- Menstrual cycle changes
- Dental work or facial trauma
Once you know your triggers, you can take preventive action.
Daily Suppressive Therapy
For people with frequent outbreaks, daily antiviral medication can reduce recurrence. Valacyclovir and acyclovir taken daily may decrease outbreak frequency.
This approach also reduces asymptomatic shedding, lowering transmission risk to partners.
Lifestyle Modifications
Stress management, adequate sleep, and a balanced diet support immune function. While these don’t guarantee prevention, they reduce outbreak likelihood.
Sun protection is particularly important. Apply SPF lip balm before outdoor activities, skiing, or beach trips.
When to See a Doctor
Most cold sores heal without medical intervention. However, certain situations require professional care:
- Cold sore lasts longer than two weeks
- Sores are severe, extremely painful, or widespread
- You experience eye irritation, redness, or vision changes
- Signs of bacterial infection develop (pus, increasing redness, fever)
- You have a weakened immune system (HIV, cancer treatment, organ transplant)
- Outbreaks occur frequently (six or more times yearly)
- You develop cold sores in unusual locations
According to NIH research, erythema multiforme—a hypersensitivity reaction—is precipitated by herpes infection in up to 70% of cases. This condition causes distinctive target-like lesions and requires specific treatment.
The CDC notes that HSV infections in infants can be severe, requiring immediate medical attention. Parents with active cold sores should take careful precautions around newborns.
Common Myths About Cold Sores
Misinformation about cold sores is widespread. Let’s clear up some confusion.
Myth: Popping Helps Them Heal Faster
False. Popping extends healing time, increases infection risk, and spreads the virus. The fluid inside blisters contains millions of viral particles that contaminate surrounding skin.
Myth: Toothpaste Dries Out Cold Sores
There’s no scientific evidence supporting this home remedy. Toothpaste ingredients can irritate broken skin and don’t have antiviral properties. Stick to proven treatments.
Myth: Cold Sores Only Spread During Outbreaks
According to the CDC, HSV spreads through asymptomatic shedding even without visible sores. Active outbreaks increase transmission risk dramatically, but the virus can spread anytime.
Myth: Only HSV-2 Causes Genital Herpes
The CDC notes that an increasing proportion of anogenital herpes infections are attributed to HSV-1, which is especially prominent among young women and MSM. Oral-genital contact can transmit HSV-1 to the anogenital area.
Myth: You Can’t Get Cold Sores If You’re Healthy
HSV-1 infection is extremely common regardless of health status. The virus affects people of all ages, backgrounds, and health levels. Stress and other triggers can activate the virus even in otherwise healthy individuals.
The Bottom Line on Popping Cold Sores
Resist the urge. Popping cold sores creates more problems than it solves.
The blister fluid spreads active virus to new areas of skin. Open wounds invite bacterial infections that complicate healing. The damaged tissue takes longer to repair and may scar permanently.
Effective cold sore management starts early—ideally at the first tingle. Antiviral creams applied during the prodrome stage shorten outbreaks significantly. Cold compresses reduce discomfort without damaging tissue. Keeping the area clean and avoiding contact prevents spread.
For frequent outbreaks, prescription antivirals offer stronger prevention and treatment. Daily suppressive therapy can significantly reduce recurrence for people with six or more outbreaks yearly.
Most importantly, leave cold sores alone. The natural healing process works best without interference. Your patience will be rewarded with faster healing, less scarring, and lower transmission risk.
Take action at the first sign of tingling, apply proven treatments consistently, and let your body’s healing mechanisms do their work. That’s the fastest path from outbreak to recovery.
Frequently Asked Questions
Yes, but results are modest compared to early intervention. Apply over-the-counter antiviral cream (aciclovir or penciclovir) every 2-3 hours during waking hours. Cold compresses reduce swelling and discomfort. Keep the area clean and dry. Prescription oral antivirals like valacyclovir work faster than topical treatments but require a doctor’s visit. Even with treatment after blisters form, expect 7-10 days for complete healing.
Wash your hands immediately with soap and water. Clean the area gently with mild soap and water, then pat dry with a clean towel. Apply antiviral cream if you have it. Avoid touching the sore again. Watch for signs of bacterial infection like increased redness, pus, or fever. If these develop, consult a doctor—you may need antibiotics. The sore will now take longer to heal, possibly 14+ days.
Yes, though less contagious than during the blister stage. The virus can still be present until the scab falls off completely and the skin underneath has fully healed. The CDC notes that HSV spreads through asymptomatic shedding even without visible sores, so transmission is possible anytime. Avoid kissing, sharing utensils, and oral contact until the cold sore has completely healed and disappeared.
Wait until the blister has dried and crusted over before applying makeup. Use a clean cotton swab or disposable applicator to apply concealer—never use fingers or reusable brushes directly on the sore. Apply antiviral medication first, let it absorb, then carefully apply makeup. Throw away any applicators that touched the sore. Remove makeup gently and thoroughly before bed. Never apply makeup to open, weeping sores.
HSV-1 establishes latency in specific nerve ganglia near the original infection site. When the virus reactivates, it travels down the same nerve pathways to the same skin area. This is completely normal. The virus “remembers” its pathway, causing outbreaks in predictable locations. Frequent outbreaks in the same spot indicate you might benefit from daily suppressive antiviral therapy to reduce recurrence.
Yes, but take precautions. Avoid activities that involve facial contact or sharing equipment (contact sports, shared gym mats). Don’t touch your face during workouts. Bring your own towel and water bottle. Wash hands thoroughly before and after exercise. Intense exercise that causes extreme fatigue might temporarily suppress immunity and prolong healing, so moderate intensity is better during outbreaks.
Absolutely. The fluid inside cold sore blisters contains millions of viral particles. When you pop a blister, this fluid gets on your fingers, surfaces, and anything you touch. You can then transfer the virus to other people through direct contact, shared objects, or contaminated surfaces. This is one of the primary ways cold sores spread. Always wash hands thoroughly if you touch an active cold sore.