Quick Summary: Missing a dose of seizure medication can lower drug levels in the body, potentially increasing seizure risk. Research shows that occasionally missing doses doesn’t always cause immediate breakthrough seizures, but consistent non-adherence raises risks significantly. If a dose is missed, the recommended action depends on timing—typically take it as soon as remembered unless the next dose is approaching.
Seizure medications—also called antisepileptic drugs or antiseizure medications (ASMs)—require consistent daily dosing to maintain therapeutic levels in the bloodstream. But life happens. Alarms get ignored, routines get disrupted, and pills get forgotten.
So what actually happens when a dose gets skipped?
The answer isn’t as straightforward as many people think. Recent research challenges some long-held assumptions about missed doses and seizure risk, while also highlighting why medication adherence remains critical for long-term seizure control.
Understanding How Seizure Medications Work
Antiseizure medications work by maintaining stable drug concentrations in the bloodstream and brain tissue. These medications suppress abnormal electrical activity that triggers seizures.
Most ASMs are taken once or twice daily. The goal is to keep blood levels within a therapeutic range—high enough to prevent seizures, but not so high that side effects become intolerable.
When a dose gets missed, drug levels begin to drop. How quickly they drop depends on the medication’s half-life, which is the time it takes for the body to eliminate half of the drug.
Medication Half-Life Matters
Some seizure medications have long half-lives, meaning they stay in the system longer. Others have short half-lives and leave the body more quickly.
For example, levetiracetam (Keppra) has a reported half-life of approximately 6-8 hours. Phenobarbital has a significantly longer half-life measured in days. Missing one dose of phenobarbital has far less immediate impact than missing one dose of levetiracetam.
This pharmacokinetic reality shapes how risky a missed dose actually is.
What Research Shows About Missing Doses
Here’s where things get interesting. While healthcare providers have long warned patients that missing even one dose could trigger a seizure, recent research paints a more nuanced picture.
Research indicates that occasionally missing ASM doses doesn’t necessarily cause immediate seizures for many patients. The researchers concluded that clinicians might reasonably reassure patients that infrequent missed doses aren’t necessarily catastrophic.
That said, this finding comes with major caveats. The keyword is occasionally. Frequent non-adherence is still a serious concern.
The Non-Adherence Problem
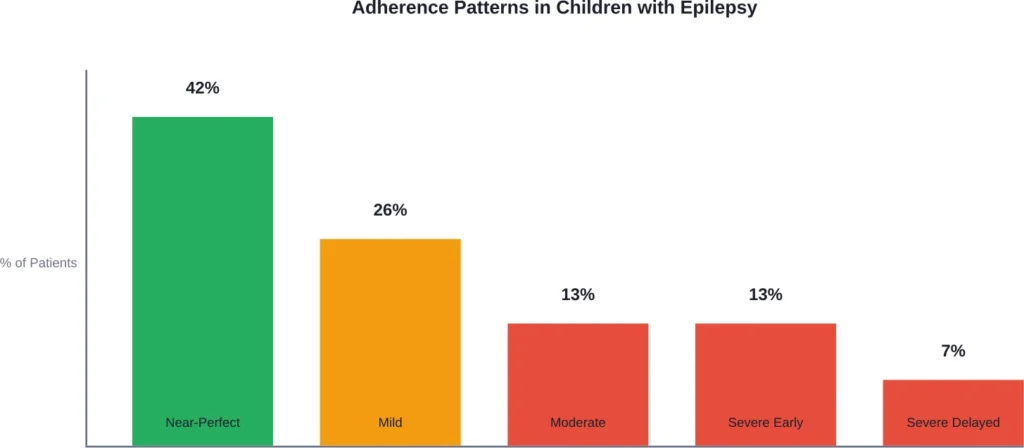
Medication non-adherence in epilepsy is surprisingly common. According to a study published in the Journal of the American Medical Association (JAMA), nearly three of every five children with newly diagnosed epilepsy do not take their antiepileptic medications as prescribed over the first six months of therapy.
The study identified different adherence patterns. Thirteen percent exhibited severe early non-adherence, 7 percent showed severe delayed non-adherence, 13 percent demonstrated moderate non-adherence, and 26 percent had mild non-adherence. Only 42 percent showed near-perfect adherence.
These patterns matter because chronic non-adherence—repeatedly missing doses over weeks and months—absolutely does increase seizure risk.
Immediate Risks of a Missed Dose
When one dose gets skipped, several things can happen—or not happen.
For many people, especially those on medications with longer half-lives, a single missed dose won’t trigger an immediate seizure. The drug concentration drops, but it may stay within or close to the therapeutic range.
But that’s not guaranteed. Some people are more sensitive to fluctuations in medication levels. Factors that influence risk include:
- Type and severity of epilepsy
- Specific medication and its half-life
- Current drug levels (were they already on the lower end of therapeutic range?)
- Other seizure triggers present (stress, sleep deprivation, alcohol use)
- How long since the last seizure occurred
The FDA has issued warnings about specific antiseizure medications. For instance, levetiracetam (Keppra, Keppra XR, Elepsia XR, Spritam) and clobazam (Onfi, Sympazan) can cause rare but serious reactions called Drug Reaction with Eosinophilia and Systemic Symptoms. While this isn’t directly about missed doses, it highlights that these medications require careful management.
Breakthrough Seizures
A breakthrough seizure is one that occurs despite being on medication. Missing doses is one potential trigger, though not the only one.
Research on remedial dosing published in Neurology emphasizes that delayed or missed ASM doses are common during long-term treatment. The study developed model-informed approaches to provide individualized remedial regimens for 11 commonly used ASMs.
The takeaway? Medical professionals recognize that missed doses happen, and there are evidence-based strategies to minimize harm when they do.
What to Do If You Miss a Dose
The standard advice depends on timing.
If it’s been just a few hours since the missed dose and the next scheduled dose is still far off, take the missed dose as soon as remembered. Most healthcare providers recommend this approach when less than half the dosing interval has passed.
But if it’s almost time for the next dose—say, within a few hours—skip the missed dose entirely. Never double up on doses to make up for one that was skipped. Taking two doses too close together raises the risk of side effects and potential toxicity.
Medication-Specific Guidance
Different medications may have slightly different recommendations. Here’s what matters for commonly prescribed ASMs:
| Medication | Half-Life | If Missed Dose Remembered Soon | If Near Next Dose |
|---|---|---|---|
| Levetiracetam (Keppra) | 6-8 hours | Take as soon as remembered | Skip and resume schedule |
| Lamotrigine (Lamictal) | 24-35 hours | Take as soon as remembered | Skip and resume schedule |
| Carbamazepine (Tegretol) | 12-17 hours | Take as soon as remembered | Skip and resume schedule |
| Valproic Acid (Depakote) | 9-16 hours | Take as soon as remembered | Skip and resume schedule |
| Phenytoin (Dilantin) | 22 hours | Take as soon as remembered | Skip and resume schedule |
Always consult the specific prescribing information or ask a pharmacist if unsure.
Special Situations
What if the dose was vomited shortly after taking it? If vomiting occurs within 30 minutes of taking seizure medication, it may not have been fully absorbed. Contact a doctor or pharmacist before taking another dose. Don’t automatically retake the medication without guidance.
What about extended-release formulations? These require even more caution. Extended-release medications are designed to release slowly over many hours. The dosing schedule is built around this. Missing a dose or doubling up can disrupt the intended steady release.
Long-Term Consequences of Non-Adherence
While one missed dose might not be catastrophic, patterns of non-adherence create serious problems.
Chronic non-adherence increases seizure frequency. It also makes it harder for neurologists to determine whether a medication is actually working. If seizures continue despite treatment, the doctor needs to know whether it’s because the medication isn’t effective or because it’s not being taken consistently.
Quality of Life Impact
Research published in PubMed examined whether adjusting treatment in well-managed epilepsy patients improves quality of life. The study found that despite possible seizure recurrence risk, adjusting drug treatment in patients who report considerable medication-related complaints does improve quality of life.
This highlights a delicate balance. Medication side effects—which antiseizure medications including levetiracetam, lamotrigine, carbamazepine, and oxcarbazepine—can be so burdensome that they affect adherence.
A study from the Human Epilepsy Project found that Levetiracetam was associated with >3-fold risk of psychiatric adverse effects compared to lamotrigine. Levetiracetam had the highest proportion of discontinuations because of adverse effects alone, while lamotrigine had the lowest.
When side effects are intolerable, people are more likely to skip doses or stop taking medications altogether.
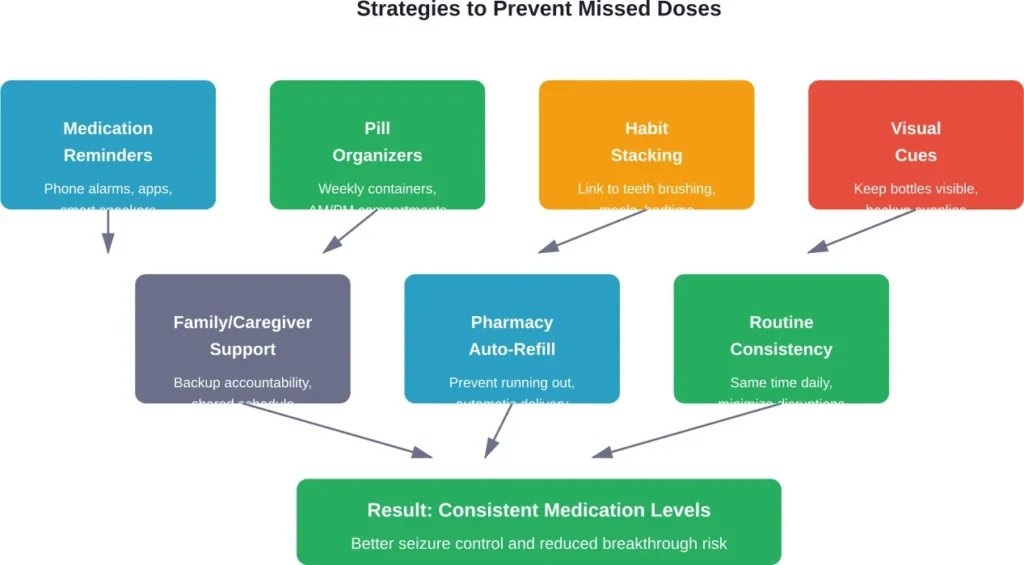
Strategies to Prevent Missed Doses
Preventing missed doses is far better than managing them after the fact. Here are evidence-based strategies that work.
Use Medication Reminders
Set daily alarms on a phone. Use multiple alarms if taking medication more than once daily. Smart speakers and health apps can also send reminders.
Some people with epilepsy have memory problems related to their condition, making external reminders essential.
Pill Organizers
Weekly pill organizers with compartments for each day help track whether doses have been taken. Some organizers have separate compartments for morning and evening doses.
Loading the organizer once a week creates a routine and makes it immediately visible if a dose was skipped.
Link to Daily Habits
Take medication at the same time each day, linked to an existing habit. Common anchors include:
- Brushing teeth in the morning and evening
- Eating breakfast or dinner
- Arriving at or leaving work
- Bedtime routine
Habit stacking makes medication-taking more automatic.
Keep Medication Visible
Store medication bottles somewhere visible, not tucked away in a cabinet. The visual cue serves as a reminder.
For those who travel frequently, keep a backup supply in a work bag, purse, or car. Just ensure medications aren’t exposed to extreme temperatures.
Involve Family or Caregivers
For children with epilepsy or adults who need additional support, involving family members or caregivers helps maintain consistency. Having someone else who knows the medication schedule provides a backup system.
When to Contact a Healthcare Provider
Certain situations require immediate medical consultation.
Contact a doctor or pharmacist if:
- Multiple doses have been missed in a short period
- A seizure occurs after missing a dose
- Unsure about when to take a missed dose
- Side effects are making it difficult to take medication consistently
- Running out of medication and unable to get a refill immediately
- Considering stopping or changing medication
Never abruptly stop taking seizure medication without medical supervision. Rapid withdrawal can trigger seizures, even in people whose epilepsy has been well-controlled.
Medication Withdrawal and Seizure Risk
Research on antiepileptic drug withdrawal shows that premature withdrawal doesn’t necessarily result in uncontrollable seizures for everyone. Studies of children who were seizure-free for two years found that withdrawal can be beneficial for most patients.
However, this is done under careful medical supervision with gradual tapering. It’s completely different from suddenly stopping medication because doses were missed or pills ran out.
The Role of Medication Monitoring
Some people benefit from therapeutic drug monitoring, where blood tests measure drug levels. This is particularly useful for medications with narrow therapeutic ranges, like phenytoin and carbamazepine.
Monitoring helps doctors determine whether drug levels are within the target range. If levels are consistently low, it might indicate non-adherence—or it might mean the dose needs adjustment due to individual metabolism differences.
For newer medications like levetiracetam and lamotrigine, routine monitoring is less common because these drugs have wider therapeutic ranges. But it can still be useful in specific situations, such as pregnancy or when adherence is a concern.
Understanding Individual Risk Factors
Not everyone faces the same risk from a missed dose. Several factors influence individual vulnerability.
Epilepsy Type and Severity
People with well-controlled epilepsy who haven’t had a seizure in years may tolerate an occasional missed dose better than someone whose seizures are frequent or difficult to control.
Certain epilepsy types are more sensitive to medication fluctuations than others.
Polypharmacy Considerations
Many people take multiple antiseizure medications. Missing a dose of one medication while continuing others may have less impact than missing the only medication being taken.
But this also creates complexity. Remembering multiple medications with different dosing schedules increases the chance that something gets missed.
Other Health Conditions
Kidney or liver problems can affect how medications are processed and eliminated. This can make drug levels more unpredictable when doses are missed.
Other medications can also interact with antiseizure drugs, affecting their levels and effectiveness.
Practical Tips for Traveling
Travel disrupts routines, making missed doses more likely. Plan ahead to maintain consistency.
Pack more medication than needed for the trip duration. Keep medication in carry-on luggage, not checked bags that could get lost.
Set phone alarms that account for time zone changes. If traveling across time zones, consult a pharmacist about how to adjust dosing times gradually.
Bring a copy of the prescription and a letter from the doctor explaining the medical necessity, especially when traveling internationally.
Addressing Side Effects to Improve Adherence
One major reason people miss doses—intentionally or not—is side effects. Research consistently shows that adverse events affect adherence.
Common side effects of antiseizure medications include:
- Drowsiness and fatigue
- Dizziness and unsteadiness
- Cognitive effects (memory problems, difficulty concentrating)
- Mood changes (depression, irritability, aggression)
- Weight changes
- Gastrointestinal issues
According to research from the Human Epilepsy Project, patients with comorbid depression and anxiety report significantly worse side effect profiles, regardless of which medication they’re taking.
If side effects are burdensome, talk to a healthcare provider. Sometimes adjusting the dose, changing the timing, or switching to a different medication can reduce side effects while maintaining seizure control.
Frequently Asked Questions
There’s no fixed timeline. Some people may never have a seizure from one missed dose, while others might experience one within hours. It depends on the medication’s half-life, individual drug metabolism, seizure threshold, and other factors. Medications with shorter half-lives create more immediate risk as drug levels drop faster.
No. Never double up on doses. Taking two doses close together increases the risk of side effects and potential toxicity without providing better seizure control. If a dose is missed and it’s almost time for the next one, skip the missed dose and return to the regular schedule.
Frequent missed doses significantly increase seizure risk and make it harder to assess medication effectiveness. Talk to a healthcare provider about strategies to improve adherence, potential side effects that might be interfering, or whether a different medication or dosing schedule might work better. Don’t wait until seizures worsen to address the issue.
No. Missing a single dose is very different from abruptly stopping medication entirely. Stopping suddenly, especially after taking medication regularly for a long time, can cause withdrawal effects and greatly increase seizure risk. One missed dose is a temporary dip in drug levels; stopping completely eliminates the medication from the system entirely.
Yes. Medications with shorter half-lives (like levetiracetam at 6-8 hours) create more immediate concerns when missed compared to those with longer half-lives (like phenobarbital at 2-6 days). Extended-release formulations are also designed for specific steady release patterns, making missed doses potentially more problematic. Ask a pharmacist about the specific medication being taken.
If unsure whether a dose was taken and it’s still early in the dosing interval, it’s generally safer to skip it rather than risk taking a double dose. Use a pill organizer to prevent this uncertainty—if the compartment is empty, the dose was taken. If full, it wasn’t. Some smart pill bottles also track when they’re opened.
Don’t change dosing schedules without consulting a healthcare provider. Some medications require specific timing intervals for optimal effectiveness. A doctor or pharmacist can advise whether schedule adjustments are safe and might even suggest switching to a once-daily formulation if one is available and appropriate.
Conclusion
Missing a dose of seizure medication isn’t ideal, but it’s also not necessarily an immediate catastrophe. Research shows that occasionally missing doses doesn’t always trigger breakthrough seizures, especially for medications with longer half-lives.
That said, consistent adherence remains critically important. Chronic non-adherence—repeatedly missing doses over time—absolutely does increase seizure frequency and reduces medication effectiveness.
If a dose gets missed, the general rule is simple: take it as soon as remembered unless it’s almost time for the next dose. Never double up. And if doses are being missed frequently, that’s a signal to talk with a healthcare provider about strategies to improve adherence or address side effects that might be interfering.
The best approach is prevention. Use reminders, pill organizers, habit stacking, and support systems to maintain consistent medication-taking. When seizure control is stable and medication is taken as prescribed, quality of life improves dramatically.
If you’re struggling with medication adherence, don’t wait until seizures become a problem again. Reach out to your neurologist or epilepsy care team. There are evidence-based solutions—from medication adjustments to behavioral strategies—that can help. Taking control of medication management is one of the most powerful steps toward better seizure control and a fuller life.
